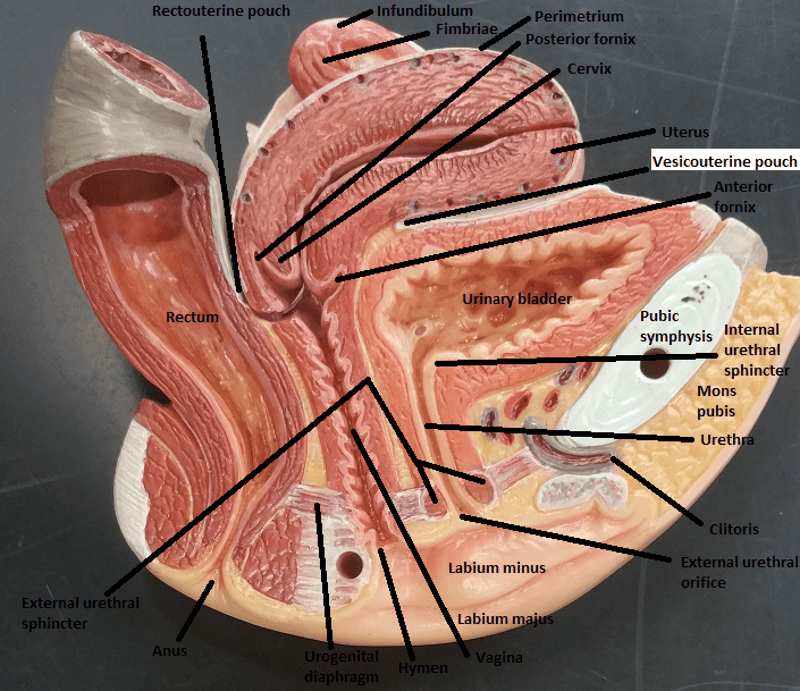
Metabolism of nutrients by the body produces what 3 wastes that must be eliminated from the body?
1. Carbon dioxide
2. Nitrogenous wastes
3. Ammonia
The urinary system is primarily responsible for the removal of what type of wastes?
Nitrogenous wastes
In addition to the removal of nitrogenous wastes, the kidney of the urinary system also has what 3 important functions? (Hint: Think ions, acid-base, and fluid..)
1. Electrolyte balance
2. Acid-base balance
3. Fluid balances of the blood
The kidneys also produce what fluid?
Urine
Is the kidney a major homeostatic organ of the body?
Yes
To perform all its functions, the kidney first acts as what type of filter and then as what type of processor?
It first acts as a blood filter and then as a filtrate processor.
The kidney allows what 3 substances to leave the body in the urine while simultaneously doing what?
1. Toxins
2. Metabolic wastes
3. Excess ions
...while simultaneously retaining needed substances and returning them to the blood
Malfunction of the urinary system, especially of the kidneys, leads to a failure in homeostasis, which uncorrected, is fatal. T/F?
True
The urinary system consists of what 4 structures?
1. Kidneys (paired)
2. Ureters (paired)
3. Urinary bladder
4. Urethra
Of the urinary system, the ureters, urinary bladder, and urethra provide what 2 functions?
1. Provide temporary storage reservoirs
2. Act as transportation channels
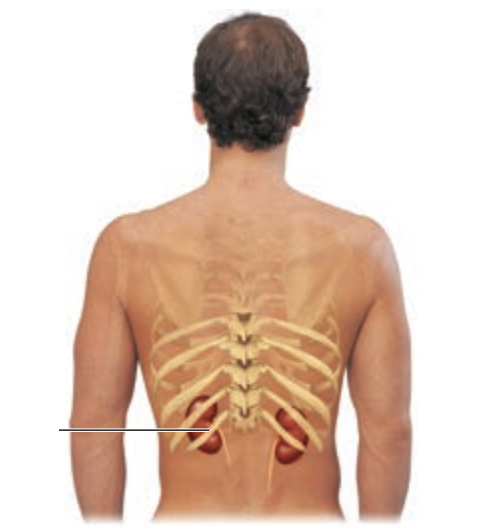
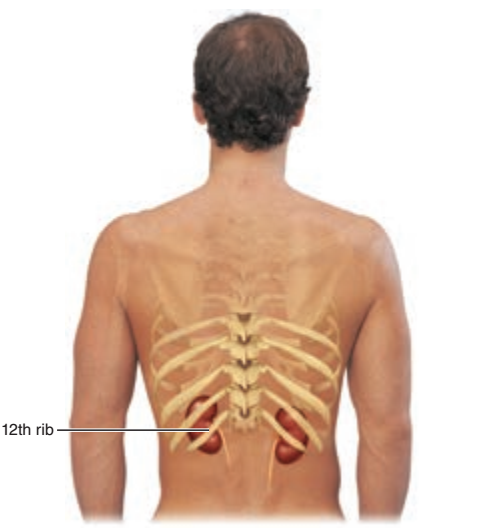
Why is the right kidney slightly lower than the left kidney?
It is crowded by the liver
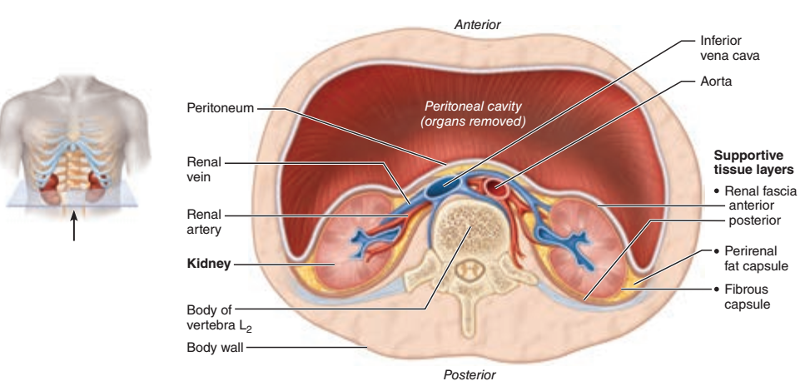
How many layers of support tissue surround each kidney (from the innermost layer to the outermost layer)? What are they?
1. Fibrous capsule
2. Perirenal fat capslue
3. Renal fascia
Describe the texture of the renal fascia?
Fibrous
What is the function of the fibrous renal fascia?
Holds the kidneys in place in a retroperitoneal position
In cases of rapid weight loss or in very thin individuals, what may happen to the fat capsule?
It may be reduced in amount
1. When the fat capsule of the kidneys is reduced with rapid weight loss or in very thin individuals, what is the consequence?
2. What is the condition above called?
1. The kidneys are less anchored and may drop to a more inferior position in the abdominal cavity
2. Ptosis
The renal arteries diverge from what major artery and plunge into what area of the kidney?
Diverge from the descending aorta and plunge into the renal hilum
What blood vessels drain the kidneys?
Renal veins
What is the function of the two ureters?
Carry urine from the kidneys to the bladder
How do the two ureters move the urine from the kidneys?
By peristalsis
Is the bladder involved in temporary storage?
Yes
Which part of the urinary system drains the urinary bladder?
The urethra
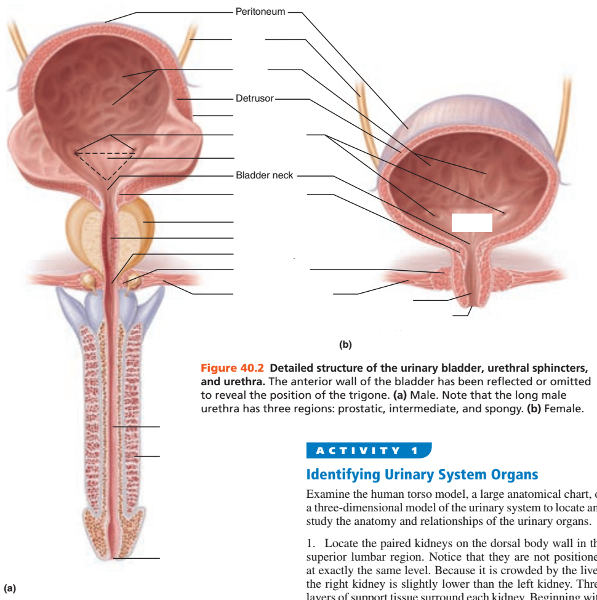
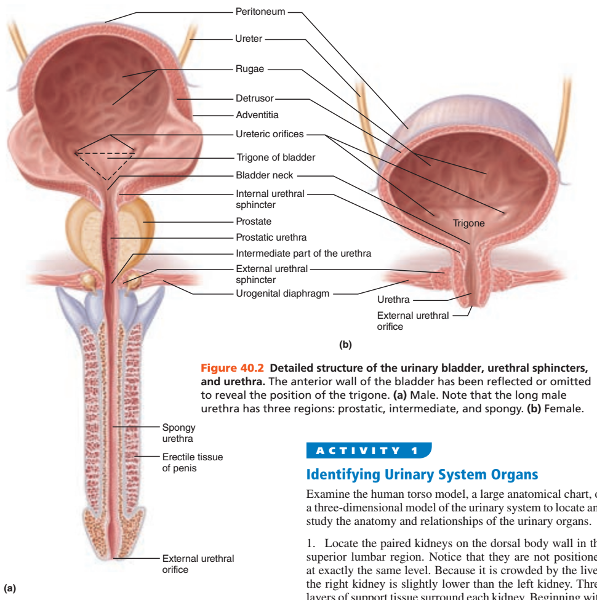
The triangular region of the bladder that lies above the opening of the urethra and is delineated by the openings of the ureters is referred to as what?
The trigone
The urethra travels the length of what organ in males?
The penis
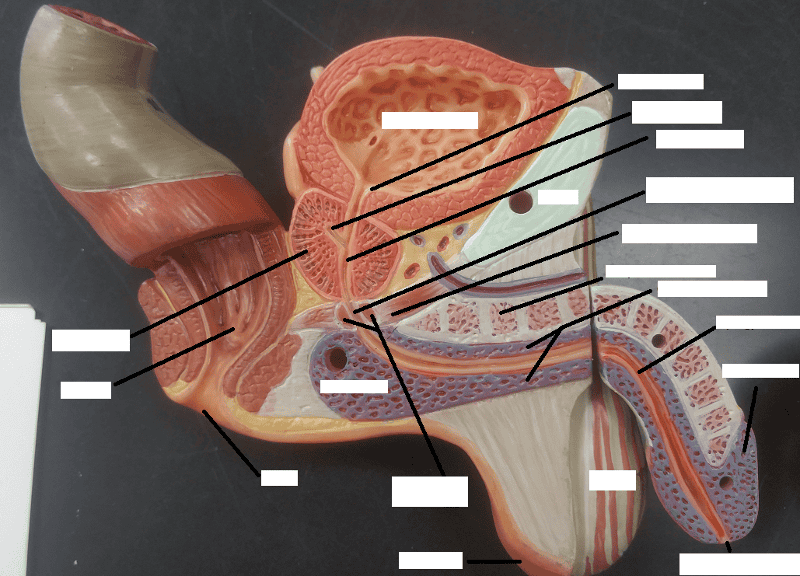
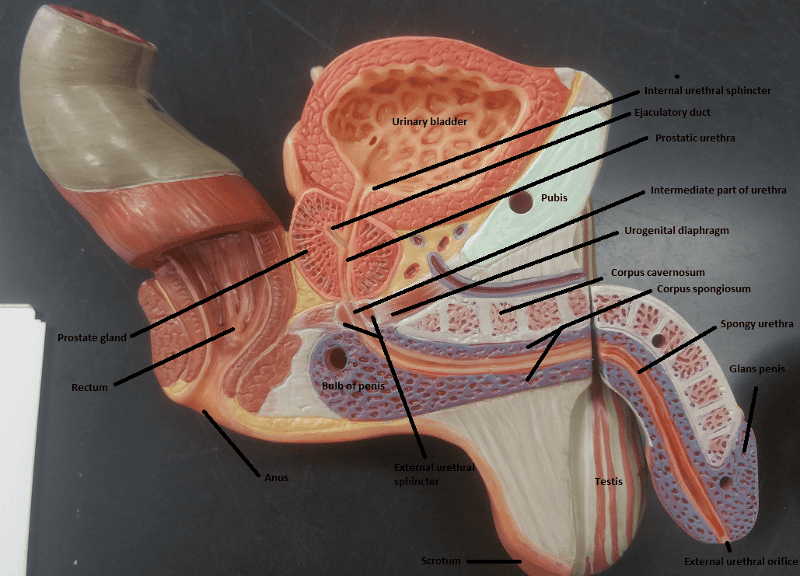
The urethra in males is made up of what 3 regions?
1. Prostatic urethra
2. Intermediate part of the urethra aka membranous urethra
3. Spongy urethra
1. The male urethra has how many functions?
2. About how long is the male urethra?
1. Two
2. About 20 cm or 8inches long
What are the 2 functions of the male urethra?
1. Carries urine to the body exterior
2. Provides a passageway for semen ejaculation
In males, the urethra is part of what 2 systems?
1. Urinary system
2. Reproductive system
1. Compared to the male urethra, are there any reproductive pathways in the female urethra?
2. About how long is the female urethra?
1. No
2. About 4 cm or 1.5 inches long
What is the sole function of the female urethra?
Serves to transport urine to the body exterior
What is the external opening of the male and female urethra?
The external urethral orifice
How does the fibrous capsule adhere to the kidney and to which aspect? (Hint: think external or internal.)
Adheres tightly to the external aspect of the kidney
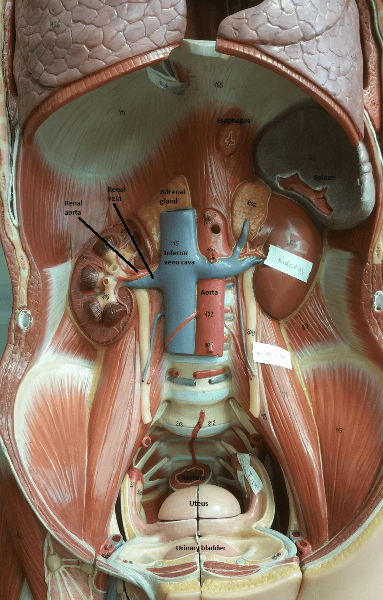
What 3 structures enter the renal hilum?
1. Ureter
2. Renal vein
3. Renal artery
Of the ureter, renal vein, and renal artery, which one has the thinnest wall and will be collapsed?
Renal vein
Of the ureter, renal vein, and renal artery, which one has the thickest wall?
Ureter
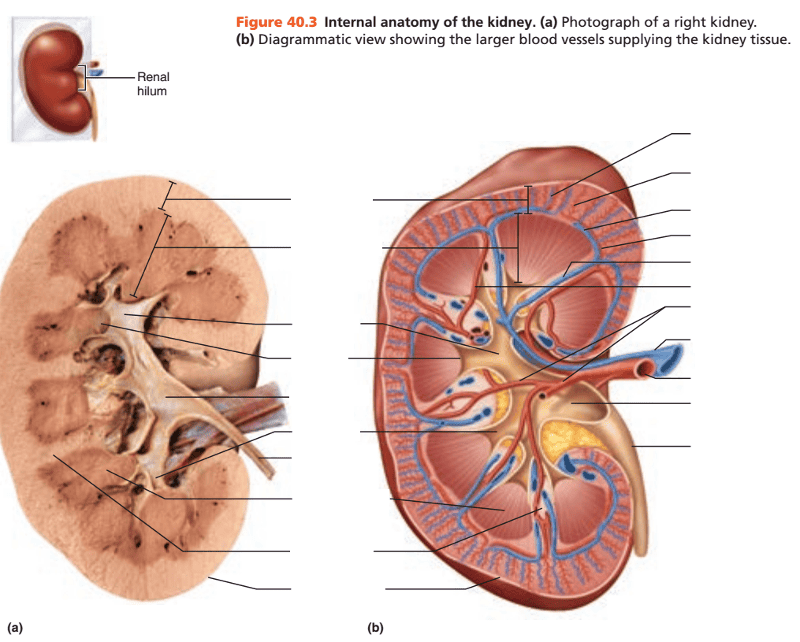
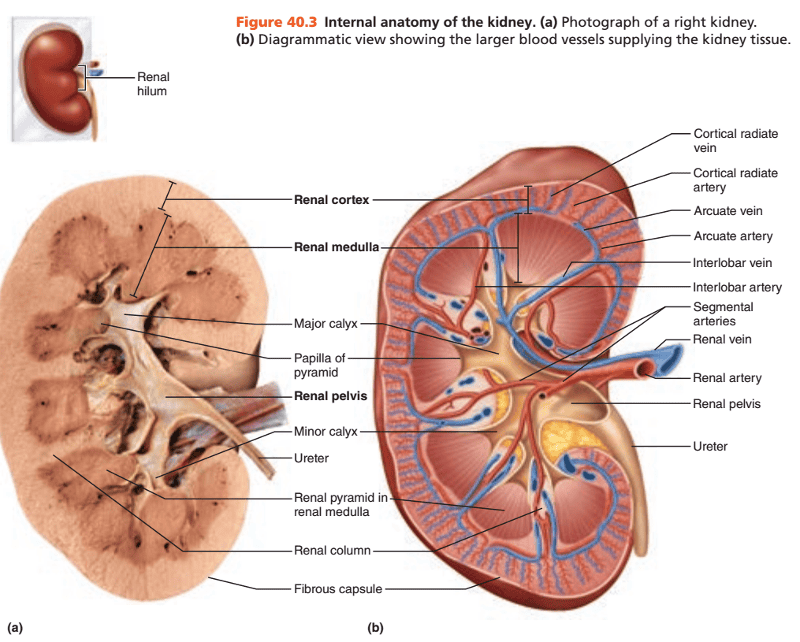
Where is the renal cortex located?
Superficial kidney region or outermost region
The renal cortex is rich in what type of supply?
Vascular supply
In the medullary region, the medulla is separated into what regions?
Renal pyramids
How do the renal pyramids appear? (Hint: striped or non-striped?)
They are striped
The base of each pyramid faces toward what region of the kidney?
Toward the cortex of the kidney
The part of the renal pyramids that points to the innermost kidney region is called what?
Papilla or apex
The renal columns are similar in appearance to what region of the kidney?
The renal cortex
What is the function of the renal columns?
Separate the renal pyramids
Extending inward from the hilum is what basin-like cavity that is continuous with the ureter?
The renal pelvis
The ureter exits from what region of the kidney?
The hilum region
What is the larger or primary extension of the renal pelvis called?
Major calyx
A smaller subdivision of the major calyx is called what?
Minor calyx
A minor calyx terminates in cup-like areas that enclose what?
The apexes or papilla of the renal pyramids
What is the function of a minor calyx?
To collect urine draining from the apexes or papilla of the renal pyramids and transfer it to the renal pelvis
What fraction of the total blood flow of the body is delivered to the kidneys each minute?
1/4
What vessels deliver blood to the kidneys?
Renal arteries
As a renal artery approaches the kidney, it breaks up into what arteries?
Segmental arteries
1. The segmental arteries enter what region of the kidneys?
2.The segmental arteries further break up into what arteries?
1. Renal hilum
2. Interlobar arteries
The interlobar arteries extend outward toward what region of the kidneys?
Renal cortex
Approaching the base of the renal pyramids, the interlobar arteries further branch into what arteries?
Arcuate arteries
The arcuate arteries curve over which part of the renal pyramids?
Base of the renal pyramids
The arcuate arteries further branch into what arteries and extend into what region of the kidneys?
Further branch into cortical radiate arteries that ascend into the cortex
In the cortical region of the kidneys, the cortical radiate arteries further branch off into what blood vessels?
Afferent arterioles
Afferent arterioles enter which specific structure of the kidney? (Hint: part of the nephron)
The glomerulus
The glomerulus is a ball of what blood vessel?
A ball of capillaries
What blood vessels drain the glomerulus?
Efferent arterioles
The efferent arterioles that drain the glomerulus feed into one of what 2 capillary beds?
1. Peritubular capillaries
2. Vasa recta
Blood draining from the peritubular capillaries or vasa recta then enter what blood vessels?
The cortical radiate veins
The cortical radiate veins then drain into what blood vessels?
Arcuate veins
The arcuate veins then drain into what blood vessels?
Interlobar veins
The interlobar veins then drain into what blood vessel?
The renal vein
The renal veins then drain into what major blood vessel?
The inferior vena cava
Trace a drop of blood from the renal artery to the renal vein. (Hint: 13 steps)
1. Renal artery
2. Segmental arteries
3. Interlobar arteries
4. Arcuate arteries
5. Cortical radiate arteries
6. Afferent arterioles
7. Glomerulus
8. Efferent arterioles
9. Vasa recta or peritubular capillaries
10. Cortical radiate veins
11. Arcuate veins
12. Interlobar veins
13. Renal vein
Each kidney contains over a million what?
Nephrons
What are the structural and functional units of the kidneys?
Nephrons
What are the 2 functions of the nephrons?
1. Filtering the blood
2. Forming urine
Each nephron consists of what 2 major structures?
1. Renal corpuscle
2. Renal tubule
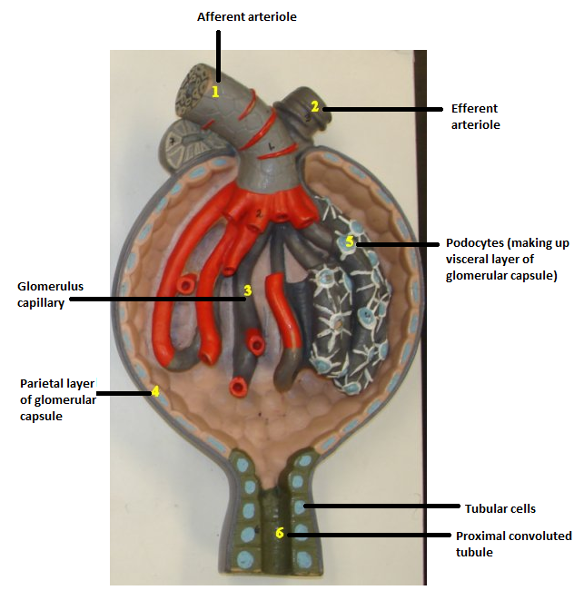
What are the 3 structures within the renal corpuscle? (Hint: Think capillaries and 2 other layers)
1. Glomerulus
2. Visceral layer of the glomerular capsule
3. Parietal layer of the glomerular capsule
The glomerulus is made up of what epithelium?
Fenestrated endothelium or simple squamous epithelium
What is the function of the glomerulus?
Forms part of the filtration membrane
The visceral layer of the glomerular capsule is composed of what type of cells?
Podocytes
The visceral layer of the glomerular capsule is composed of what type of epithelium?
Simple squamous epithelium
What is the function of the podocytes of the visceral layer of the glomerular capsule?
Forms part of the filtration membrane
The spaces between the podocytes form what type of slits?
Filtration slits
The parietal layer of the glomerular capsule is composed of what type of epithelium?
Simple squamous epithelium
What is the function of the parietal layer of the glomerular capsule?
Forms the outside of the glomerular capsule
Does the parietal layer of the glomerular capsule play any role in filtration?
No
What are the 6 structures within the renal tubule (following the glomerular capsule)?
1. Proximal convoluted tubule (PCT)
2. Descending limb of the nephron loop
3. Descending thin limb of the nephron loop
4. Thick ascending limb of the nephron loop
5. Distal convoluted tubule (DCT)
6. Collecting duct
What is the epithelium of the proximal convoluted tubule?
Simple cuboidal
1. Does the proximal convoluted tubule contain many mitochondria?
2. Does the proximal convoluted tubule contain many microvilli?
1. Yes
2. Yes
1. What is the main function of the proximal convoluted tubule?
2. Does some secretion also occur?
1. Primary site of tubular reabsorption of water and solutes
2. Yes
What is the epithelium of the descending limb of the nephron loop?
Simple cuboidal epithelium
What is the microvilli concentration like in the descending limb of the nephron loop?
Some microvilli, decreased in number compared to the concentration seen in the PCT
What are the 2 functions of the descending limb of the nephron loop?
1. Tubular reabsorption
2. Tubular secretion
What is the epithelium of the descending thin limb of the nephron loop?
Simple squamous epithelium
What is the concentration of aquaporins like in the descending thin limb of the nephron loop?
Many aquaporins
1. What is the main function of the descending thin limb of the nephron loop? (Hint: think water)
2. Is the descending thin limb of the nephron permeable to water?
1. Water is reabsorbed, but no solutes are reabsorbed.
2. Yes
What are the 2 epitheliums of the thick ascending limb of the nephron loop?
1. Cuboidal epithelium
2. Low columnar epithelium
What is the concentration of aquaporins like in the thick ascending limb of the nephron loop?
Very few aquaporins
1. What is the main function of the thick ascending limb of the nephron loop?
2. Is the thick ascending limb of the nephron loop permeable to water?
1. Passive and active reabsorption of solutes
2. Not permeable to water
What is the epithelum of the distal convoluted tubule?
Simple cuboidal
1. What is the microvilli concentration in the distal convoluted tubule?
2. What is the mitochondria concentration in the distal convoluted tubule?
1. Few microvilli
2. Many mitochondria
What are the 2 main functions of the distal convoluted tubule?
1. Some reabsorption of water and solutes
2. Some secretion
The collecting duct receives filtrate from what structure within the renal tubule?
Receives filtrate form the distal collecting tubule of many nephrons
What is the epithelium of the collecting duct?
Simple cuboidal
What 2 specialized cells are also found in the collecting duct?
1. Principal cells
2. Intercalated cells
1. What is the function of principal cells?
2. What is the function of intercalated cells?
1. Electrolyte homeostasis
2. Maintain acid-base homeostasis
What are the 4 functions of the collecting duct?
1. Some reabsorption of body fluids
2. Some secretion of body fluids
3. Maintain blood pH
4. Regulate solute concentrations
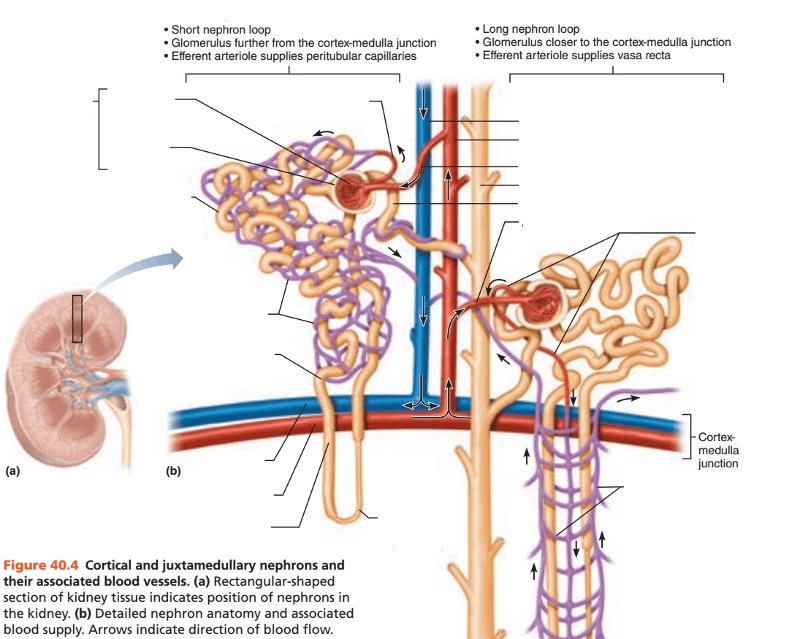
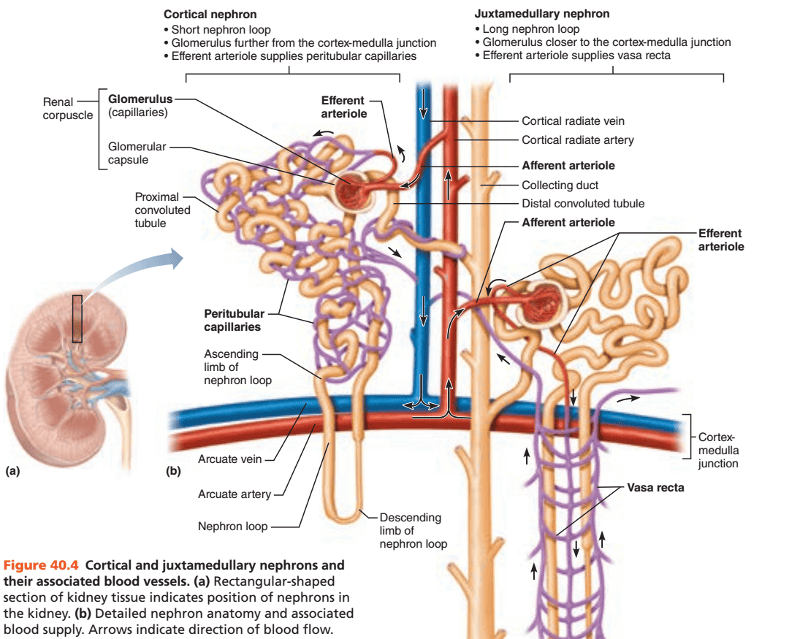
What are the 2 kinds of nephrons?
1. Cortical nephrons
2. Juxtamedullary nephrons
What are the most numerous type of nephrons, and they comprise what percentage of all the body's nephrons?
Cortical nephrons are the most numerous ones, and they make up about 85% of all nephrons
Cortical nephrons are located almost entirely within what region of the kidney?
The renal cortex
Although cortical nephrons are almost entirely located within the renal cortex, small parts of their loops do dip into what area of the kidney?
The renal medulla
How are the renal corpuscles of juxtamedullary nephrons different from the renal corpuscles of cortical nephrons (in regards to location in the renal cortex)?
The renal corpuscles of juxtamedullary nephrons are located deep in the renal cortex at the border with the renal medulla
How are the long nephron loops of juxtamedullary nephrons different from the nephron loops of cortical nephrons (in regards to location in the renal medulla)?
Their long nephron loops penetrate deeply into the medulla
Which group of nephrons play an important role in concentrating urine?
Juxtamedullary nephrons
The function of the nephron depends on what 3 features of renal circulation?
1. Glomerular filtration
2. Tubular resorption
3. Tubular secretion
What are the 3 capillary vascular supply of nephrons?
1. Glomerulus
2. Pertitubular capillary bed
3. Vasa recta
Of the 3 capillary beds, glomerulus, peritubular capillary bed, and vasa recta, which one is first encountered in the nephron?
Glomerulus
Vessels leading to and from the glomerulus are what type of arterioles?
Glomerular arterioles
Which arteriole feeds the glomerulus and which arteriole drains it?
The afferent arteriole feeds the glomerulus, and the efferent arterole drains it.
Why is the glomerular capillary bed unique in the body? (Hint: think pressure)
It is a high-pressure bed
The glomerular capillary bed is a high-pressure bed because of what reason?
The afferent feeder arteriole is larger in diameter than the efferent arteriole draining it
How are fluid and blood components smaller than proteins forced out of the glomerulus into the glomerular capsule?
The afferent and efferent arterioles create high hydrostatic pressure to force fluid and blood components out of the glomerulus into the glomerular capsule
Fluid and blood components forced out of the glomerulus into the glomerular capsule (through the high hydrostatic pressure created by afferent and efferent arterioles) form what, and what is it processed by?
The filtrate is formed, which is processed by the nephron tubule
Efferent arterioles that supply cortical nephrons and drain the glomerulus tend to form what specific type of capillary bed?
The peritubular capillary bed
How does this set of capillaries cling to the renal tubule?
They cling very closely to the renal tubule
Describe the peritubular capillary bed in regards to pressure and porosity?
Low-pressure, high porosity
The peritubular capillary bed is mainly adapted for what function? (Hint: absorption or filtration?)
Absorption
Since the peritubular capillary bed is mainly adapted for absorption rather than filtration, what 2 substances does it take up from the filtrate?
1. Solutes
2. Water
Which cells process and resorb the solutes and water of the filtrate, two substances that are eventually absorbed again by the peritubular capillary bed?
Tubule cells
Efferent arterioles that supply juxtaglomerular nephrons tend not to form peritubular capillaries, and instead, form what specific capillary bed?
The vasa recta
Differentiate the structure of the peritubular capillary bed and the vasa recta in regards to structure and how the run to their nephron loops.
The peritubular capillary bed clings intimately to its renal tubule and is very coiled. The vasa recta runs parallel to its renal tubule and also clings close, but it is not coiled.
The vasa recta is essential for what to happen?
The concentration of urine
Each nephron also has what complex?
A juxtaglomerular complex
Where is the juxtaglomerular complex located? (Hint: think of the nephron loop and the afferent arteriole)
Located where the most distal portion of the ascending limb of the nephron loop touches the afferent arteriole
What 2 cell types form the juxtaglomerular complex?
1. Granular cells or juxtaglomerular cells
2. Macula densa cells
1. The granular cells or juxtaglomerular cells are located where?
2. What is their function?
1. Located in the arteriole walls of the afferent arteriole
2. Sense blood pressure in the afferent arteriole
1. The macula densa cells are located where?
2. What is their function?
1. Located in the most distal portion of the ascending limb of the nephron loop
2. Monitors sodium chloride concentration in the filtrate
What are the 2 functions of the juxtaglomerular complex?
1. Regulate the rate of filtration based on the salt concentration
2. Regulate systemic blood pressure
Urine forms as a result of what 3 processes?
1. Glomerular filtration
2. Tubular resorption
3. Tubular secretion
Glomerular filtration is accomplished by feature of the nephron?
The glomerulus
Is glomerular filtration passive or active?
Passive
Describe glomerular filtration.
A portion of the blood passes from the glomerular capillary into the glomerular capsule
What happens during tubular resorption? (Hint: Filtrate components move through what cells and return to what?)
Filtrate components move through the tubule cells and return to the blood in the peritubular capillaries
1. Is tubular resorption passive or active, or both?
2. If both, describe what is passively resorbed (by what process) and what is actively resorbed?
1. Both
2. Water is passively resorbed by osmosis, but most substances are actively resorbed.
What are 3 substances that are almost entirely resorbed from the filtrate?
1. Water
2. Glucose
3. Amino acids
Of water, glucose, and amino acids, what is passively resorbed, and what 2 are actively resorbed?
Water is passively resorbed, while glucose and amino acids are actively resorbed.
Is active resorption highly selective?
Yes
Various ions are selectively resorbed or allowed to go out into the urine based on what 2 conditions?
1. What is required to maintain appropriate blood pH
2. What is required to maintain appropriate electrolyte composition
What 4 substances are resorbed to a lesser degree or not resorbed at all?
1. Urea
2. Creatinine
3. Uric acid
4. Drug metabolites
Most of tubular resorption occurs in what part of the nephron tubule? (Hint: Give the percentage of tubular resorption for the associated part of the tubule)
Most (about 75-85%) of tubular resorption occurs in the proximal convoluted tubule
Tubular secretion is the reverse process of what of the 3 process that form urine: glomerular filtration, tubular resorption, and tubular secretion?
Tubular resorption
1. What 3 substances move from the blood of the peritubular capillaries through the tubular cells into the filtrate to be disposed of in urine?
2. Describe the process of tubular secretion from the blood in the peritubular capillaries to urine. (Hint: 4 steps)
1. Hydrogen
2. Potassium ions
3. Creatinine
____________________
1. Peritubular capillaries
2. Tubular cells
3. Filtrate
4. Urine
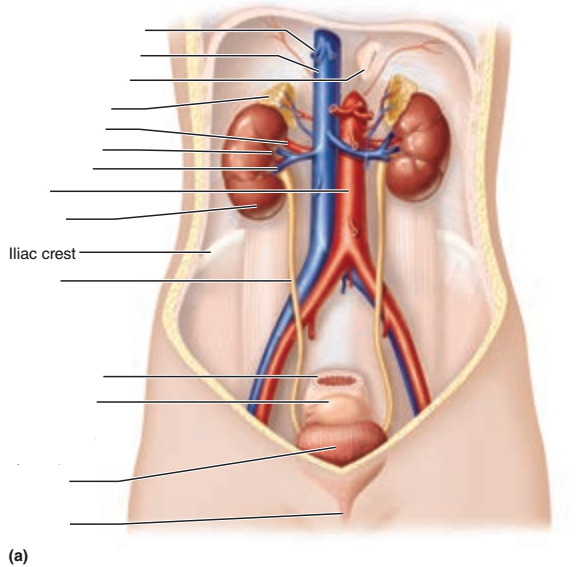
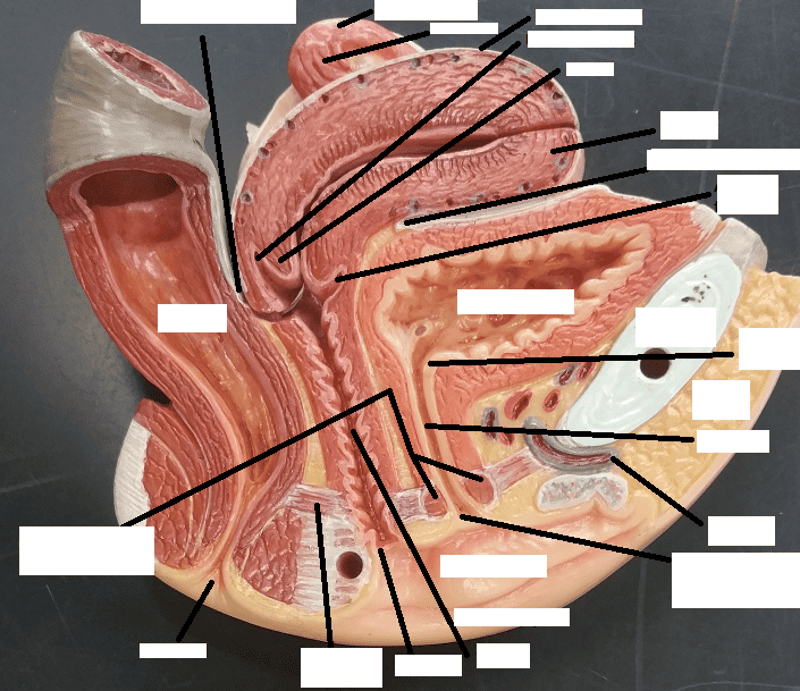
Identify the blanks.
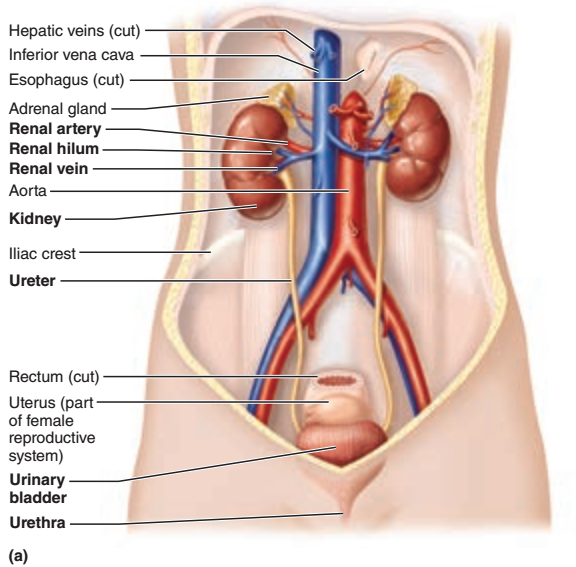
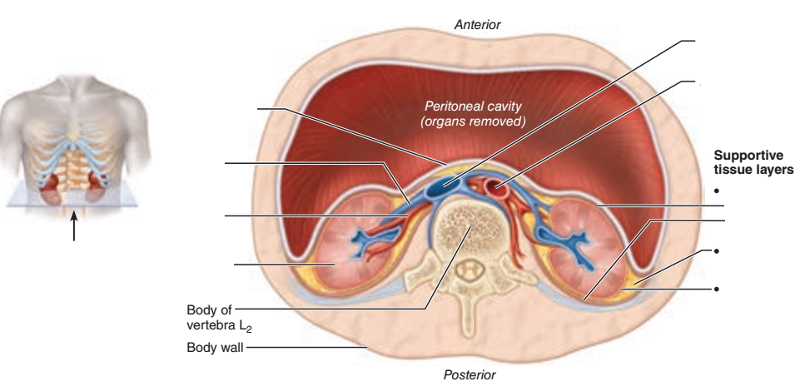
Identify the blanks.
Identify the blanks.
Identify the blanks.
Identify the blanks.
Identify the blanks.
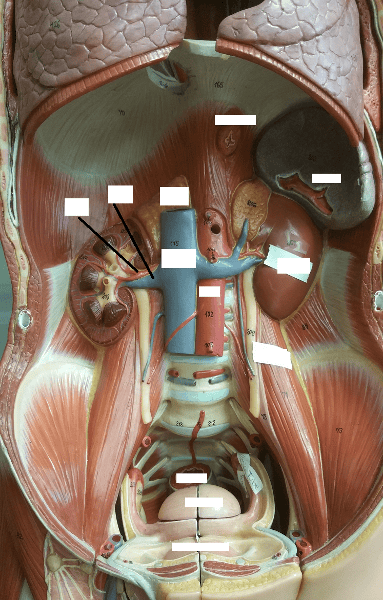
Identify the blanks.
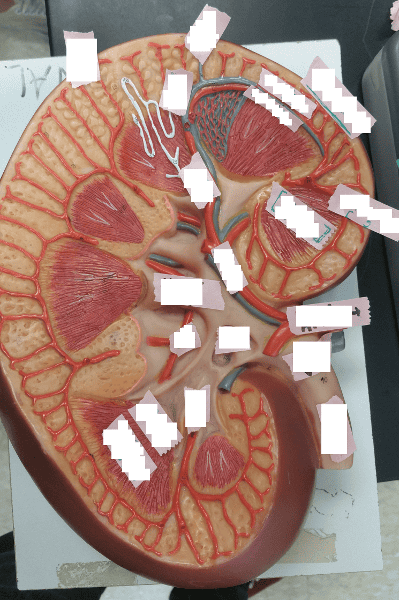
Identify the blanks.
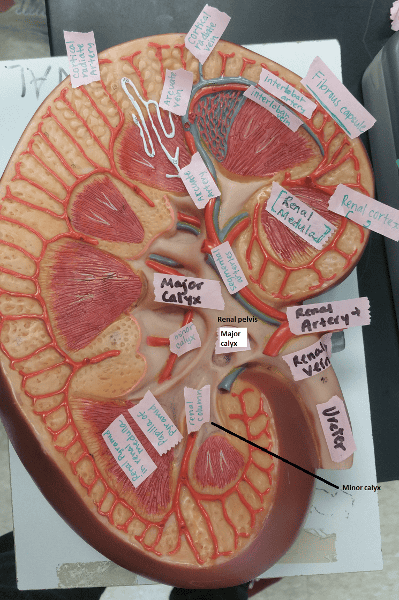

Identify the blanks.
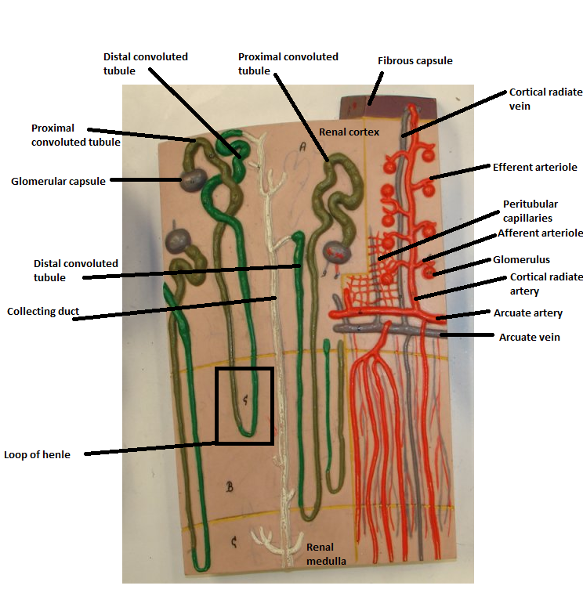

Identify the blanks.