Upper system:
nose, nasal cavity, pharynx, and associated structures
Lower system:
larynx, trachea, bronchi, and lungs
Conducting zone:
conduits for air to REACH the sites of gas exchange
** includes all other respiratory structures (i.e. nose, nasal cavity, pharynx, trachea)
Respiratory zone:
where gas exchange OCCURS
** respiratory bronchioles, alveolar ducts, alveolar sacs, and alveoli
What is the functional unit of the respiratory system?
alveoli
Nose is divided into 2 sections:
1. external nose: including the root, bridge, dorsum nasi, and apex
2. internal nasal cavity
What is the name of the shallow vertical groove inferior to the apex?
philtrum
Functions of the nasal mucosa and conchae:
1. during inhalation: they filter (coarse hairs), heat, and moisten air
2. during exhalation: they reclaim heat and moisture, minimize heat and moisture loss
Paranasal sinuses:
sinuses in bones that surround the nasal cavity
**sinuses lighten the skull and help to warm and moisten the air
***contributes to how our voice sounds!
Pharynx?
funnel-shapes tube of skeletal muscle that connects to the:
a) nasal cavity and mouth superiorly
b) larynx and esophagus inferiorly
Space behind the nose is called?
Nasopharynx (strictly an air passageway)
** lined with pseudostratified columnar epithelium (GOBLET CELLS!!)
What is the area called that links the oral and nasal cavities?
Oropharynx (food and air passage)
What is the structure that extends to the larynx, where the respiratory and digestive pathways diverge?
Laryngopharynx (food and air passage)
How far does the pharynx extend?
from the base of the skull to the level of the sixth cervical vertebra
What is the voice box called?
Larynx
What are the functions of the larynx?
1. provides a patent airway
2. acts as a switching mechanism to route air and food into the proper channels
3. voice production
Where does the larynx attach to?
attaches to the hyoid bone and opens into the laryngopharynx superiorly
What is the laryngeal cartilage that gives you the "Adam's apple"?
thyroid cartilage
What is the laryngeal cartilage that closes the larynx during swallowing?
epiglottis
What is the laryngeal cartilage that is used for the emergency air-opening procedure (tracheotomy?
cricoid
Laryngeal cartilages picture
Thyroid (2 fused), epiglottis, cricoid, arytenoid (paired), corniculate (paired), cuneiform (paired)
Voice production:
1. ventricular/false vocal cords(cuneiform)
2. vocal/true vocal cords (corniculate)
Ventricular folds (false vocal cords)
has the ability to close during coughing, sneezing, and Valsalva's maneuver
What is Valsalva's maneuver?
causes intra-abdominal pressure to rise when abdominal muscles contract,
**helps to empty the rectum,
***acts as a splint to stabilize the trunk when lifting heavy loads (think of the ridiculous faces weight-lifters make)
What is the space that allows the vocal cords to open and close called?
rima glottidis
What happens during whispering?
everything is closed except the posterior rima glottidis, the vocal folds do not vibrate (no pitch)
What is the flexible and mobile tube extending from the larynx into the mediastinum?
trachea
Conducting zone: bronchi
...
What is the trachea called before it splits into the primary bronchi?
"ca-ry-na?" lol i forgot (look this up later)
What do the alveolar walls secrete?
**What do the type II cells secrete?
Alveolar walls secrete angiotensin convering enzyme (ACE)
** type II cells secrete surfactant
How do alveolar walls permit gas exchange?
by simple diffusion
What are alveolar walls made up of?
type I epithelial cells
How many alveoli are in the respiratory zone?
approximately 300 million
Type 1 = ACE
Type 2 = Surfactant
Macrophages have to clean up the batches of messy alveolar when someone smokes.. sometimes they get exhausted by cleaning up all the tar that they will slow down. The alveoli will collapse, and is damaged forever. -->COPD
Picture: an alveolar exposed to cigarette smoke
**alveoli don't regenerate
Lung Anatomy
MUST KNOW: number of lobes per side, fissures and location-apex,middle,base
right side has 3 lobes, left side has 2 lobes
What are the two main circulations that supply blood to the lungs?
pulmonary and bronchial
What is the name of the thin, double-layered serosa that covers the external lung surface?
pleura
**visceral or pulmonary on external, parietal covers the thoracic wall and superior face of the diaphragm
What is another name for breathing?
pulmonary ventilation
Respiratory pressure is always described relative to:
atmospheric pressure (Patm)
Pressure within the alveoli is called:
intrapulmonary pressure (Ppul)
Pressure within the pleural cavity:
intrapleural pressure (Pip)
Pressure that keeps the airways open:
transpulmonary pressure (Ppul minus Pip)
When pressure is negative, you breathe in, when it is positive - you breathe out
Air flows into the lungs, down its pressure gradient, until intrapleural pressure = atmospheric pressure
**if intrapleural pressure is lower than alveolar, it is negative - because inhalation will occur
What is the major nonelastic source of resistance to airflow?
friction
(friction = change in pressure over resistance)
As airway resistance rises, breathing movements become more strenuous
severely constricted or obstructed bronchioles: can prevent life-sustaining ventilation
can occur during acute asthma attacks which stops ventilation
What does epinephrine do to the respiratory structures?
it dilated bronchioles and reduces air resistance
Define: surface tension
this happens when there's a decrease in surfactin;
** the attraction of liquid molecules to one another at a liquid-gas interface
Define: surfactant
a detergent-like complex that reduces surface tension and helps keep the alveoli from collapsing
Define: lung compliance
how much it allows you to expand/relax, contributed by the amount of pressure it is subjected to
Lung compliance is determined by two main factors:
1. distensibility of the lung tissue
2. surface tension of the alveoli
factors that diminish lung compliance:
1. scar tissue/fibrosis
2. blockage of smaller respiratory passages w/ mucus or fluid
3. reduced production of surfactant
4. decreased flexibility of thoracic cage/decreased ability to expand
Respiratory Volumes:

Tidal volume (TV): air that movies into and out of the lungs with each breath
Inspiratory volume (IV): air that can be inspired forcibly beyond tidal volume
Expiratory volume (EV): air that can be evacuated from the lungs after a tidal expiration
Residual volume (RIV): air left in the lungs after strenuous expiration
Respiratory Capacities:
Inspiratory capacity (IC): total amount of air that can be inspirated after a tidal expiration
Functional residual capacity (FRC): amount of air remaining in lungs after a tidal expiration
Vital capacity (VC): the total amount of exchangeable air
Total lung capacity (TLC): sum of all lung volumes **approximately 6000ml in males**
Anatomical dead space:
volume of the conducting respiratory passages (150ml)
Alveolar dead space:
alveoli that cease to act in gas exchange due to collapse of obstruction
Total dead space:
sum of alveolar and anatomical dead spaces
Pulmonary Function Tests:
Total ventilation: total amount of gas flow into and out of the respiratory tract in one minute
Forced vital capacity (FRC: gas forcibly expelled after taking a deep breath
Forced expiratory volume (FEV): the amount of gas expelled during specific time intervals of the FVC
What is the instrument that consists of a hollow bell inverted over water, used to evaluate respiratory function?
Spirometer
Obstructive pulmonary disease:
increased airway resistance (asthma)
Restrictive disorders:
reduction in total lung capacity from structural of funtional lung changes (1800s corsets)
What is the name for the amount of gas reaching the alveoli?
ventilation
What is the amount of blood flow reaching the alveoli?
perfusion

Ventilation-Perfusion coupling
...
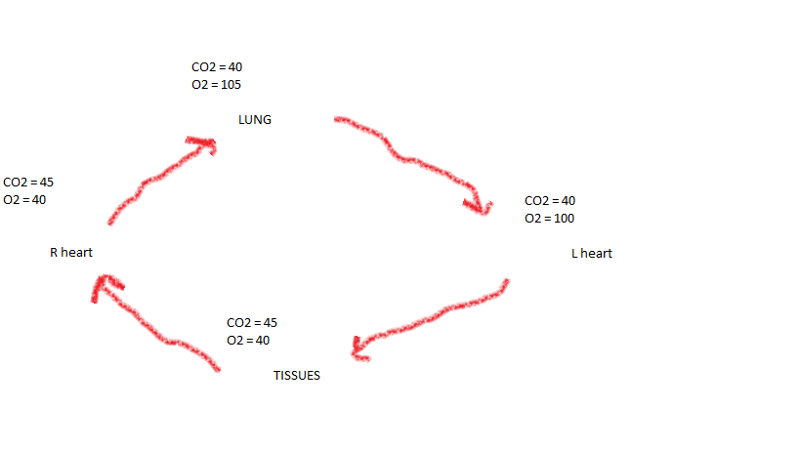
Internal respiration:
The partial pressures and diffusion gradients are reversed..
**PO2 in tissue is always lower than in systemic arterial blood
**PO2 of venous blood draining tissues is 40 mm Hg and PCO2 is 45 mm Hg (huh what)
Hemoglobin-oxygen is called:
oxyhemoglobin (HbO2)
Hemoglobin that has released oxygen is called:
reduced hemoglobin (HHb)
Henry's law:
the amount of gas that will dissolve in a liquid also depends upon its solubility
**CO2 is most soluble
**O2 is 1/20th as soluble as CO2
**nitrogen is practically insoluble in plasma
Carbon monoxide:
hemoglobin has greater affinity for carbon monoxide than for oxygen, prevents oxygen from binding to hemoglobin
poisoning = snow white appearance... skin is very pale while areas closer to bone (i.e. cheekbones) are red
Transport and exchange of carbon dioxide
(look at direction of arrows, if it is fast or slow, and chloride shift)
(IN LUNGS, THESE PROCESSES ARE REVERSED)
(DRG)dorsal respiratory group, or inspiratory center:
appears to be pacesetting respiratory center, becomes dormant during expiration
(VRG) ventral respiratory group:
involved in FORCED inspiration and expiration
Medullary Respiratory groups
...
Inflation reflex (Hering-Breuer)
stretch receptors in the lungs are stimulated by lung inflation
**when you hold your breath too long, your brain will override and force you to exhale
COPD is exemplified by:
chronic bronchitis (barrel chested, crackly) and obstructive emphysema (short, rapid breaths and cute pink cheeks)
COPD patients have a history of:
smoking (or 2nd hand smoke), dyspnea, coughing, and frequent pulmonary infections
*DRAWINGS FROM CLASS*