
Complete Breech

Frank Breech
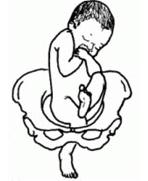
Footling Breech
When is the embryonic period?
6-12 weeks
When is the 1st trimester?
0 - 13 weeks
When is the Fetal Phase?
12 + weeks
When is the 2nd trimester?
14 - 26 weeks
Dissecting vrs concealed?
in a marginal abruption the hemorrhage dissects beneath the placental
membrane & is associated with little detachment
in a retro-placental abruption if the blood remains
retro-placental the patient has no visible bleeding
How many days is a normal pregnancy?
280 days
What makes an OB scan difficult?
patient habitus
What is the purpose of a full bladder during an OB scan?
to measure the cervix
The bladder needs to be full to measure the
cervix, after that a full bladder is not required
What is the normal measurement of the cervix?
3 cm
What are the measurements for an OB scan?
BPD
HC
AC
Femur Length
HC/AC
CI
CIterna Magna
Ventricular Atria
Amniotic fluid (AFI)
Cerebellum
What images need to be included?
Face
Neck & Spine
4 chamber heart
diaphragm
stomach
kidneys
bladder
cord - 3 vessels
cord insertion
extremities
placenta
fetal lie
genitalia
What is a cephalic position?
generic term for head down
What are the different fetal positions?
longitudinal lie
transverse lie
oblique lie
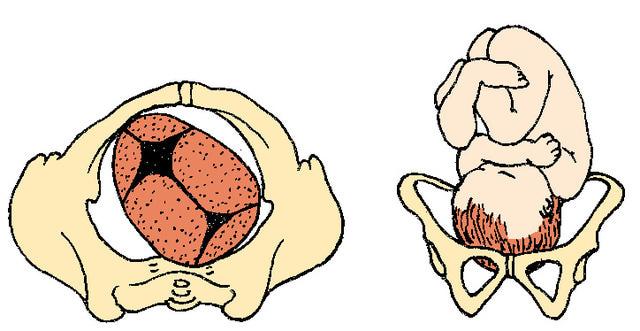
Left Occiput Posterior
LOP
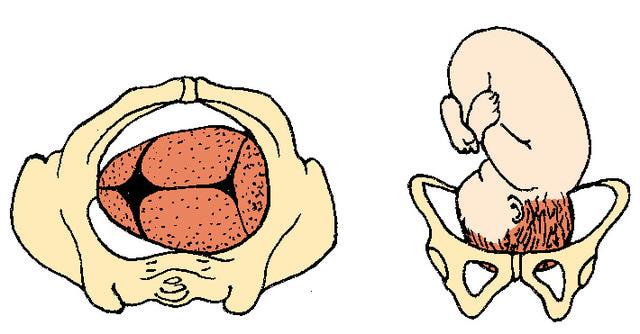
Left Occiput Transverse
LOT
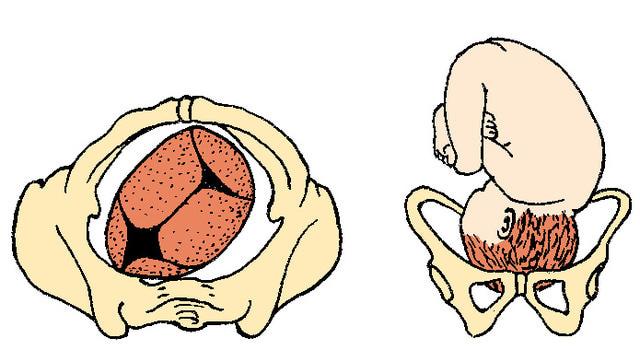
Left Occiput Anterior
LOA
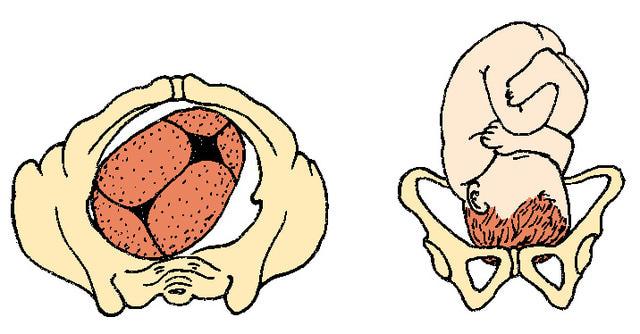
Right Occiput Posterior
ROP
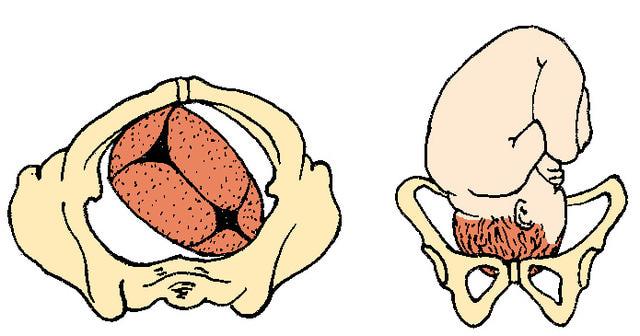
Right Occiput Anterior
ROA
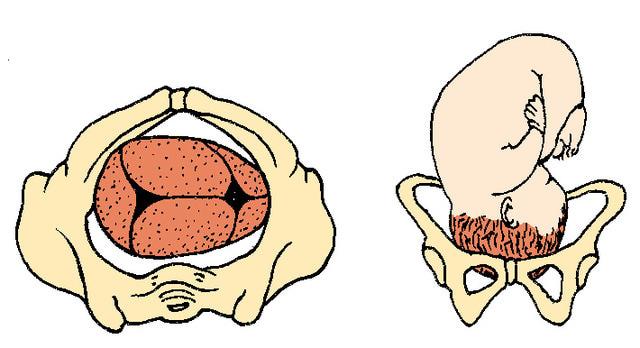
Right Occiput Transverse
ROT
What are the two footling breech positions?
single footling
double footling
What is an ECV?
external cephalic version
What must be done before an ECV can be performed?
OR must be booked in case of an emergency birth.
What can a shoulder presentation lead to?
Shoulder Dystocia
What is shoulder dystocia?
obstructed labour whereby after the delivery of the head, the
anterior shoulder of the infant cannot pass below, or requires
significant manipulation to pass below, the pubic symphysis. It is
diagnosed when the shoulders fail to deliver shortly after the fetal head.
What is the vertex presentation?
anterior and posterior fontanel presenting
How many babies are cephalic after 34 weeks?
90%
How many babies are breech at term?
3% to 4%
What is the incidence of abnormalities in breech babies?
6.3%
What is the incidence of abnormalities in vertex babies?
2.4%
What plane are brain anatomy and measurements taken in?
transverse
What should you do if the head is round rather than oval?
slide inferior
What can free a low head from the pelvis?
drinking water (filling bladder)
trendelenburg
What images are taken of the fetal head?
Faux cerebri (IHF)
Choroid Plexus
cavum septum pellucidum
Thalami
Cerebral peduncles
cerbellum & cisterna magna
Nuchal fold
orbits
profile
coronal facial views
What does the presence of the faux cerebri imply?
separation of the cerebrum has occured
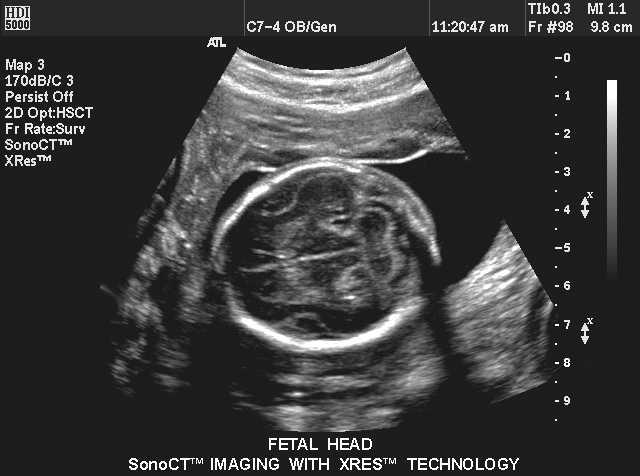
Faux cerebri
What is the function of the choroid plexus?
produce cerebrospinal fluid
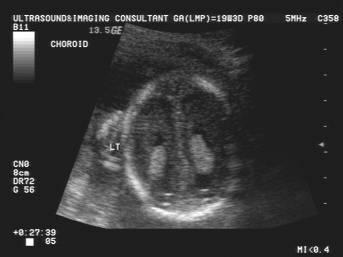
Choroid Plexus
What is the size of the choroid plexus at 20 week scan?
10 mm or less
Why is the choroid plexus image taken?
to exclude ventricular megaly
What is a dangling choroid plexus caused by?
ventricular megaly
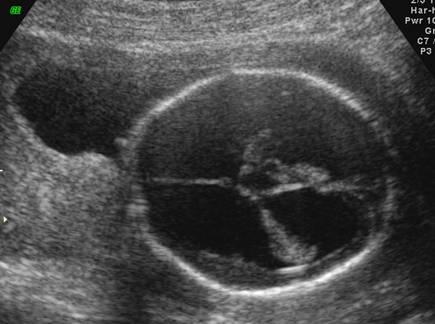
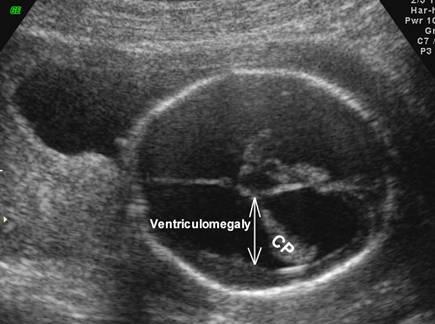
dangling choroid plexus
What is the significance of choroid plexus cysts?
none baby can become brain surgeon or
increase the risk of T18
WHAT IS TRISOMY 18?
Trisomy 18, also known as Edwards syndrome, is a condition which is
caused by an error in cell division, known as meiotic
disjunction. When
this happens, instead of the normal pair, an
extra chromosome 18
results (a triple) in the developing baby
and disrupts the normal
pattern of development in significant
ways that can be
life-threatening, even before birth. A Trisomy
18 error occurs in
about 1 out of every 2500 pregnancies in the
United States, about in
about 1 in 6000 live births. The
numbers of total births is much
higher because it includes
significant numbers of stillbirths that
occur in the 2nd and
3rd trimesters of pregnancy.
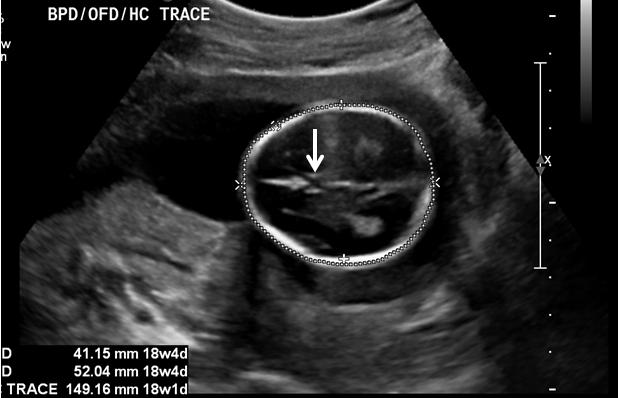
Cavum Septum Pellucidum
What is the cavum septum pellucidum?
arched band of nervous tissue that connects left & right cerebrum
What does the visualization of the cavum septum pellucidum imply?
excludes agenesis of corpus callosum
At what level is the BPD and HC taken?
the level of the thalami
What is the function of the thalami?
receive sensory impulses and transmits them to the cerebrum
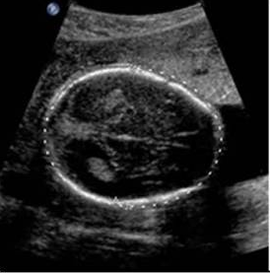
thalami view
What is the function of the cerebral peduncles?
receive impulses from brain stem and transmit them to cerebrum
2-way path
How do you find the cerebral peduncles?
first find the thalami and the peduncles with pop out
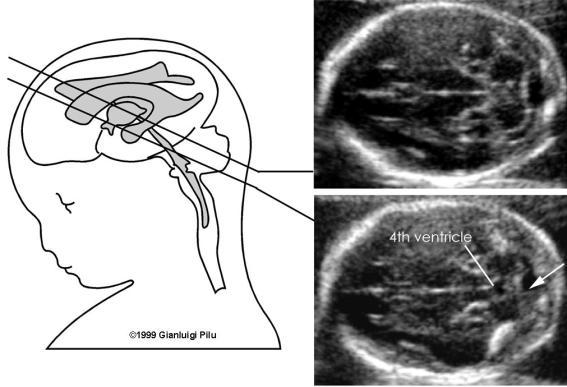
cerebral peduncles
What is the function of the cerebellum?
equilibrium
What is the measurement of the cisterna magna at 20 weeks?
10 mm or less
What is the nuchal fold?
skin behind the neck
What is the normal measurement of the nuchal fold?
5 mm of less
What does the nuchal fold measurement determine?
rules out trisomy 21
production of abnormal amounts of collagen
Down-syndrome
What is anophthalmia?
No eyes
What is hypotelorism?
close eyes
What is hypertelorism?
far eyes
What is the purpose of taking an image of the orbits?
to rule out
hypotelorism
hypertelorism
anophthalmia
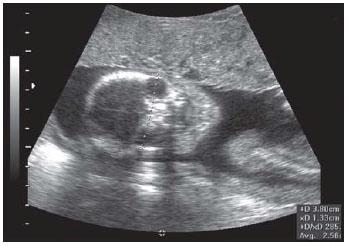
orbits
What is the purpose of the profile image?
exclude
anterior cephalocele - unicorn bony defect
frontal bossing
What is anterior cephalocele?
unicorn bony defect
What is frontal bossing?
protuding forehead
What is the significance of fetal tongue out?
Bad news -
aniplody
downs syndrome
tripody 21
Beckwith-Wiedemann syndrome
What is Beckwith-Wiedemann syndrome?
an overgrowth syndrome, which means that affected infants are
considerably larger than normal (macrosomia) and tend to be taller
than their peers during childhood.
What is micrognathia?
no chin
What is the purpose of coronal facial views?
exclude cleft lip
evaluate the integrity of nasal
How many cervical vertebra are there?
7
What happens to the cervical vertebra at the base of the skull?
widens
How many thoracic vertebra?
12
How many lumbar vertebra?
5
How many sacral vertebra?
5
How many coccyx vertebra?
4
What happens to the spine at the sacrum?
tapers
What is the most important when evaluating the spine?
follow skin covering
2 orientations
How do the lungs appear in the 1st & 2nd trimester?
isoechoic to the liver
How do the lungs appear in the 3rd trimester?
hyperechoic to the liver
What is situ?
positioning
What should happen if call made of omphalocele in 1st trimester?
Rescan at 14 to 15 weeks to rule out rotation of mid gut
How is situ evaluated?
apex of heart points to left
stomach - left
liver right
GB on right
How many heart anomalies can be excluded with the 4 chamber view?
65%
How many heart anomalies can be excluded with the 5 chamber view?
85%
What age can a pediatric echo be done to examine the heart?
18 weeks gestation
Symetry in the heart
...
What is the function of the foramen ovale?
shunting of blood from right to left
How much blood is shunted through the foramen ovale?
60%
What skirts blood through the foramen ovale?
eustation valve
Why must the heart septum be evaluated?
exclude wall defects
How is the 5 chamber best viewed?
baby lieing on back
How do you get the 5 chamber / aorta image?
angle up from 4 chamber view
How do you get the 5 chamber / pulmonary artery image?
angle up from aorta
What is evaluated to rule out diaphragmatic hernia?
heart superior to diaphragm
stomach inferior to diaphragm
Where do diaphragm abnormalities usually occur?
left side
Why is a diaphragmatic hernia dangerous?
stomach can move to the thoracic
What is esophagus atresia?
no stomach
esophagus ends in bind end tube
When is the stomach apparent?
11 wks
When must the stomach be seen?
16 wks
Why are the small intestines evaluated?
rule out meconium spillage
cystic fibrosis
Why are the large intestines evaluated?
to rule out anal atresia
What is the sonographic appearance of anal atresia?
dilated loops of bowel
When are the kidneys seen?
15 weeks
Where are the kidneys located?
retroperitoneal
how much of the abdominal circumference do the kidneys take up?
1/3
What is the normal measurement of the renal pelvis in the 2nd trimester?
5 mm or less
What is the normal measurement of the renal pelvis in the 3rd trimester?
7 mm or less
If the measurement of the renal pelvis is greater than 10 mm?
BAD
Where are the adrenals located?
superior to the kidneys
When can the adrenals be seen?
20 weeks
What is one of the problems scanning the adrenals?
can mimic kidneys
especially when kidneys are missing
What is the size of the adrenals?
50% the size of the kidneys
When can swallowing be seen?
8 - 11 weeks
What is the significance of the bladder being seen?
at least one kidney exists
At what age are the kidneys fully functioning?
16 weeks
What is the function of the kidneys before birth?
produce amniotic fluid
How often does a fetus void?
30 to 45 minutes
When does AFL peak?
34 weeks
When is XY genitalia best determined?
20 weeks
possible at 14 weeks
What is gender linked disorder?
hemophilia
When is XX genitalia best determined?
20 weeks
possible at 14 weeks
Why is it important to evaluate long bones?
determine fetal age
detection of skeletal dysplasia
detection of limb malformation
What is skeletal dysplasia?
dwarfism
When is the proximal humerus epiphyssis apparent?
39 weeks
What does the distal femoral epiphyssis indicate?
gestational age between 33 - 35 weeks
What do you evaluate with the extremities?
3 bones visible
What do you evaluate with the hands?
open good
closed fist - BAD BAD BAD
When the feet have a sandal gap what is indicated?
downs syndrome
what is a sandal gap?
gap between big toe and 2nd toe
What is the function of amniotic fluid?
movement
temperature control
shock absorber
normal lung development
What is AFI?
amniotic fluid index?
What contributes to amniotic fluid?
kidneys, lungs, cord & skin
When does fetal urine account for almost all amniotic fluid?
20 weeks
What is the sonographic appearance of amniotic fluid?
anechoic
floating vernix caseosa
When is AFI measured routinely?
after 24 weeks
What is oligohydraminos?
too little fluid
What is oligohydraminos?
...
What is pulmonary hyperplasia?
bad lung formation
What can oligohydraminos cause?
pulmonary hyperplasia
joint defect from restriction
What is a BPP?
evaluation of fetal well being
What is evaluated during a BPP?
NST
fetal tone
fetal breathing
fetal movement
What is NST?
Neonatal stress test
presence of 2 or more fetal heart rate
accelerations of at least 15 bpm in amplitude & of at least 15
seconds in duration associated with fetal movement in a 20 minute period
How is fetal tone evaluated?
extension & flexion
How is fetal breathing evaluated?
30 seconds worth
How is fetal movement evaluated?
trunk movement
How is AFI evaluated?
2 cm puddle
What is conceptual age?
fetal age
restricted to pregnancies in which the actual
date of conception is known
- in vitro fertilization
- artificial insemination
conceptual age + 14 days =
menstrual age
What is nagele's rule?
used my
LMP - 3 months + 7 days
What is menstrual age?
gestational age
What is gestational age based on?
first day of LMP
What is gestational age used for?
scedule invasive procedures
alpha-feto-protein screening
plan date of delivery
evaluate fetal growth
What is the most accurate sonographic technique for establishing
gestational age?
3 CRL
Crown rump length
What is the accuracy of the CRL?
+/- 5 days
95%
Why is s the CRL and excellent correlation of length and age?
pathological conditions minimally affect growth in the first trimester
What is the formula for gestational age in weeks?
(CRL)cm +6
When does the CRL become inaccurate?
after 12 weeks
Why is the CRL inaccurate after 12 weeks?
due to movement including extension and flexion
What is BPD?
Biparietal diameter
What is the accuracy of a BPD between 17 - 26 weeks?
+/- 11 days
What is the accuracy of a BPD after 26 weeks?
+/- 3 weeks
How is the BPD measurement taken?
outer to inner
What landmarks should bee visualized at the area of a BPD measurement?
Falx cerebri
cavum septum pellucidum
thalami
What is the ambiguous stage of the fetus?
13 - 14 weeks
Why is 13 - 14 weeks considered the ambiguous stage?
fetus is too big for CRL yet the landmarks for a BPD are not seen yet.
Use choroid plexus and head shape as the landmark
What is the formula for HC?
(BPD + OFD)(Pie)/2
How is the HC measurement taken?
outer to outer
Why is the HC a valuable measurement?
less affected by head compression
What should the shape of the head be in a fetus?
ovid
What does brachycephaly refer to?
a round head
How are the BPD measurements inaccurate with brachycephaly?
overestimate
What does Dolichocephaly refer to?
elongated head
How are the BPD measurements inaccurate with dolichocephaly?
underestimate
What is the cephalic index?
devised to determine the normality of the fetal head shape
What is the formula for C.I,?
BPD / OFD x 100
If the C.I. is <75% what is indicated?
dolichocephaly
If the C.I. is >85% what is indicated?
brachycephaly
If the C.I. is between 75% - 85% what is indicated?
Normal
What is AC?
abdominal circumference
Where is the AC taken?
level of the liver where the umbilical vein branches in the left
portal vein
The the AC should be taken in what plane?
transverse
What is the AC formula?
(D1 +D2)(pie) /2
What are the landmarks of the AC measurement?
stomach
3 ossification centers of the spine
portal vein
What is the importance of the AC?
Useful in predicting fetal weight
useful in monitoring normal fetal growth
AC size is a direct indicator of the size of the liver
useful in detecting fetal growth disturbances
such as IUGR
How accurate is femur length when determining GA?
about as accurate as BPD
When would you use femur length fo determine GA?
fetal head can not be measured due to position or anomaly
fetal death
Where is the femur measured?
from greater trochanter to the distal femoral condyle
What should happen if there is a > 2 week difference with other
biometric parameters?
measure all fetal bone
targeted exam should be done to rule out pathology
trisomy
dwarfism
What is a short femur a marker for?
trisomy
dwarfism
What are the normal gram measurement of the orbits?
ocular distance (OD)
binocular distance (BD)
interocular distance (IOD)
What is inter-ocular distance (IOD)?
between eyes
What is the binocular distance (BD)?
distance from outer orbit to contra-lateral outer orbit
What is the ocular distance (OD)?
distance of the orbit
What is the best measure of GA with the orbital measurements?
BD binocular distance
How are the orbital measurements taken?
outer to outer
When is a orbital measurement used to determine GA?
when ventriculomegaly or skeletal dysplasia exists making BPD
measurements inaccurate.
What are the orbital measurements useful in excluding?
Hypotelorism
hypertelorism
anophthalmus
microphthalmos
What is Hypotelorism?
close eyes
What is hypertelorism?
wide eyes
What is anophthalmus?
no eyes
What is microphthalmos?
small eyes
What are the parts of the cerebellum?
vermis and 2 lobes
Why is the cerebellum measured?
good correlation with GA
excluding Arnold Chiari seen in spina bifida
Dandy Walker syndrome
What is Arnold Chiari?
downward displacement of the cerebellum through the foramen magnum
banana shaped cerebellum
What is Dandy Walker?
hypoplasia of the vermis and cephalad rotation of the vermian
remnant cystic dilatation of the fourth ventricle extending
posteriorly
The placenta is composed of two components, what are they?
tissue from both mother and fetus
What is the fetal part of the placenta called?
Chorionic plate
chorion frondosum
What is the maternal part of the placenta called?
Decidua basalis
endometrial surface
What is the Decidua?
uterine lining (endometrium) during a pregnancy, which forms the
maternal part of the placenta.
What causes decidualize?
influence of hormones
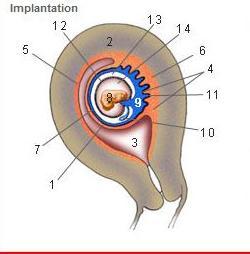
Where is the Desidua Capsularis?
1
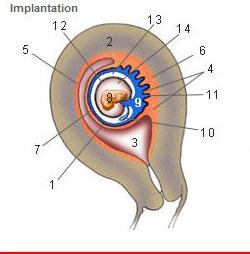
Where is the Desidua basalis?
6
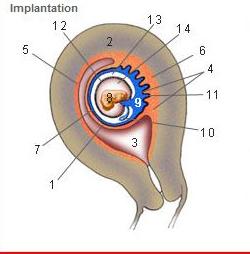
Where is the Desidua parietalis?
5
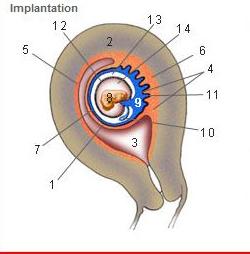
Where is the chorion frondosum?
11
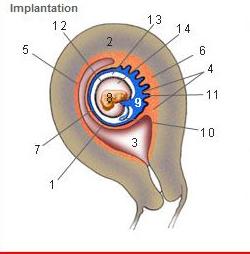
Where is the amnion?
12

Where is the chorionic cavity?
13
What is the chorionic villi?
functioning unit of the placenta
finger-like structures containing one fetal blood
capillary per villi
Where are the chorionic villi located?
intervillious space
What is the chorionic villi responsible for?
exchange of:
nutrients
waste
oxygen
carbon dioxide
Blood flow in the placenta is ______impedance.
low
Explain the blood flow from the uterus to the placenta and back.
uterine arteries
intervillous spaces
villous capillaries
umbilical vein
umbilical artery
villous capillaries
intervillous space
basilar vein
What is the function of the placenta?
Nutrition
respiration
excretion
protection
storage
hormone production (chorionic villi)
Explain the placenta evaluation.
position
echotexture / grade
size
What is changes in the maturing placenta referred to?
grading
Placenta maturation does not occur at the same rate in women
...
What can affect the maturation process?
Rh disease
diabetes
What is placenta grade 0?
smooth edges
homogeneous
1st - early 2nd
What is placenta grade 1?
small intraplacental calcifications
as early as 14 weeks
common until 34 weeks
What is placenta grade 2?
calcifications at basilar plate
greater than 30 weeks
What is placenta grade 3?
calcified indentions of placenta
35 weeks +
1/3 of term placenta
What are some causes of delayed placental maturation?
maternal diabetes
Rh sensitivity
What are some causes of advanced placental maturation?
maternal HTN
IUGR
smoking
What are some causes of a small placenta?
placental infarct
primary placental growth retardation
interuterine infection
chromosomal anomalies
What are some causes of a large placenta?
maternal diabetes
maternal anemia
non-immune Hydrops
interuterine infection
chromosomal anomalies
What is the normal size of the placenta?
less than 4 cm
1 mm thick for every week gestation
What is Placental Accreta?
attaches to myometrium
What is Placental Increta?
invades myometrium
What is Placental Percreta?
penetrates through uterus
(myometrium and serosa)
What are the risk factors of Placental Accreta?
placental previa
Hx of C-section
uterine surgeries
advanced maternal age
How is Placental Accreta detected?
elevated maternal serum AFT
MRI
Sonography
What is the sonographic appearance of Placental Accreta?
absent or thin myometrium under placenta
multiple lakes
increased vascularity
(Percreta) extrauterine mass
swiss cheese
Uterine wall should be thick!
...
What is a pregnancy loss of 19 week and under called?
miscarriage
What is a pregnancy loss after 20 week called?
Fetal Death
What is a placental abruption?
premature separation of the implanted placenta between 20 weeks and birth
What is a placental abruption associated with?
preterm labor / delivery
fetal death
How is placental abruption diagnosed?
history
physical findings:
-back pain
-bleeding
What are the signs and symptoms of placental abruption?
vaginal bleeding
pelvic pain
shock
asymptomatic
What are the risk factors of placental abruption?
hx of abruption
trauma
fibroids
placental previa
What is a Retroplacental abruption?
rupture of the spiral artery
separation of basal plate from the uterine wall
high pressure bleeds
What is Retroplacental abruption associated with?
HTN
vascular disease
What is the sonographic appearance of Retroplacental abruption?
anechoic subchorionic area between placenta and uterus
thickened uterus
collection greater than 2 cm
What is a subchorionic (marginal) abruption?
tears in the marginal vein
separates the chorion from decidua
low pressure bleed
What is associated with subchorionic (marginal) abruption?
maternal cig smoking
What is the sonographic appearance of subchorionic (marginal) abruption?
anechoic subchorionic area between placenta and uterus
Dissecting vrs concealed?
in a marginal abruption the hemorrhage dissects beneath the placental
membrane & is associated with little detachment
in a retro-placental abruption if the blood remains
retro-placental the patient has not visible bleeding
How far from the cervix is a low-lying placenta on a trans-abdominal exam?
less than 5 cm
How far from the cervix is a low-lying placenta on a trans-abdominal exam?
less than 2.5
What is the #1 cause of painless 2nd & 3rd tri bleeding?
placental previa
What are the risk factors for placenta previa?
multigravida
hx of c-sec
hx of therapeutic abortion
advanced maternal age
abnormal presentation
maternal anemia
closely spaced pregnancies
how many women have placenta previa after 24 weeks?
1: (150 =- 305)
What are the different types of placenta previa?
partial
complete
marginal
low
What is the difference between marginal and partial placental previa?
marginal just touches the cervix and partial covers some of the cervix
How many pregnancy are normal?
96%
What is wrong with the term placental migration?
Do not use around radiologists
What are the placental masses and lesions?
chorioangioma
teratoma
hemangioma
hematoma
thrombosis
placenta extrachorialis
placental cysts
membranous cord insertion
battledore placenta
What is a placental lake?
subchorionic fibrin depositions
NO CLINICAL SIGNIFICANCE
What is a placental chorioangioma?
vascular malformation, Similiar to a hemangioma
most common placental tumor can lead to fetal hydrops
What is the sonographic appearance of chorioangioma?
well-circumscribed mass; usually lobulated
hypoechoic
located within placental tissue
may contain calcifications
What is the cause of chorioangioma?
failure in development of the chorion villi persists
What is placenta membranacea?
rare
placenta develpos as a thin membrane along the
periphery of the chorion along the entire gestational sac
What is placenta membranacea associated with?
increase risk of
placenta accreta
placenta increta
placenta percreta
How many pregnancy have placenta extrachorialis?
1% to 2%
What are the two types of placenta extrachorialis?
circummarginate
circumvallate
What is circumvallate placenta extrachorialis?
chorionic plate is surrounded by a thick ring
What is associated with circumvallate placenta extrachorialis?
PROM
premature labor
placental abruption
hemorrhage
What is circummarginate placenta extrachorialis?
chorionic plate is surrounded by a thin ring
no clinical significance
How many pregnancies show placental cysts?
less than 20%
Where are placental cysts usually located?
subchorionic
placental cysts are difficult to separate from ______ ______.
intervillous thrombosis
What is velamentous (membranous) cord insertion?
cord inserts at placental margin into corion laeve
not protected my wharton's jelly
How often does a velamentous (membranous) cord insertion occur?
1% of pregnancies
What is velamentous (membranous) cord insertion associated with?
IUGR
What is IUGR?
Interuterine growth regressor
What is battledore placenta?
Cord inserts at placental margin.
Not clinically significant
looks like baddmitten
How often does battledore placenta occur?
7% of pregnancies
What is succenturiate placenta?
presence of one or more accessory lobes connected to the body of the
placenta by blood vessels
What is another name for succenturiate placenta?
bilobate placenta
What is the main problem with succenturiate placenta?
can rupture during labor
it can be left behind
What is the umbilical cord?
connection between the placenta and the fetus
What is the function of the umbilical cord?
essential link for oxygen and nutrients
What does the umbilical cord consist of?
2 umbilical arteries
1 umbilical vein
When is the umbilical cord usually seen?
week 9
What is wharton's Jelly?
surrounds the vessels within the umbilical cord to protect them
What is a short umbilical cord associated with?
abdominal wall defect
What is a long umbilical cord associated with?
prolapse
nuchal cord
true knots
What is another name of the umbilical arteries?
hypogastric arteries
What is umbilical cord prolapse?
cord gets caught in the endocervical canal
What is an umbilical nuchal cord?
cord wraps around neck
What is an umbilical true knots
knots
How many pregnancies is is an SUA found?
1%
What is an SUA?
single umbilical artery
What is the most common umbilical cord anomaly?
single umbilical artery
What is an SUA associated with?
congenital anomalies (25 - 50 %)
perinatal death
premature delivery
IUGR
chromosomal anomalies
What should happen when a 2 vessel cord is found?
very aggressive at 20 week exam lookig for anomalies
How to confirm two umbilical arteries.
follow cord from insertion to IIV
What does the umbilical arteries become after birth?
hypogastric ligaments
What is the normal A/B ratio in 3rd trimester?
less than 4:1
What is the RI after 26 weeks?
.45 - .58
End diastolic flow ______ with gestational age.
increases
What is absent or reverse EDF associated with?
fetal morbidity and mortality
What is the sonographic appearance of umbilical artery Doppler?
normal pulsatile pattern
forward flow
What happens if there is not end-diastolic flow in the umbilical artery?
be ready to go to OR but not emergency at this time...IN RED
What happens if there is reverse flow in the umbilical artery?
Emergency ....OR
What are the umbilical cord masses?
allatoic duct cysts
omphalomesenteric duct cysts
hemagioma
hematoma
mucoid degeneration of wharton's jelly
omphalocele
umbilical hernia
What is an Allantoic Duct cysts?
Allantoic cysts of the umbilical cord are extremely rare anomalies.
What are possible causes of a patient measuring Large for date?
gestational diabetes
palpating fibroids
What are possible causes of a patient with Increased Serum HCG?
gestational trophoblastic disease
What are some possible causes of a patient with Increased AFP?
twins
open neural tube defect
What are the increased risks of twins?
fetal death
premature delivery
fetal anomalies
maternal bleeding
vas previa
What is vasa previa
placenta over cervix
A condition in which blood vessels within the placenta or
theumbilical cord are trapped between the fetus and the opening to the
birth canal, a situation that carries a high risk the fetus may die
from hemorrhagedue to a blood vessel tearing at the time the fetal
membranes rupture or during labor and delivery
What is a fertilized egg called?
zygote
What is a fertilized egg that splits causing twins called?
monozygotic
What are two fertilized eggs causing twins called?
Dizygotic
How are multiple pregnancies classified?
# of chorion
# of amniotic sacs
What does the amount of separation depend on?
time of cell division
If a monozygotic divides 1-3 days post conception what is the result?
Dichorionic Diamniotic
If a monozygotic divides 4-8 days post conception what is the result?
Monochorionic Diamniotic
If a monozygotic divides 8-13 days post conception what is the result?
Monochorionic Monoamniotic
If a monozygotic divides 13+ days post conception what is the result?
conjoined twins
What is the most common form of conjoined twins?
thoracopagus
What is thoracopagus
joined at the thorax
What percent of conjoined twins are born alive?
60%
How many conjoined twins are fused on the ventral wall?
56%
polydramnios is commonly present in what type of twin?
conjoined
How many monozygotic twins are classified DCDA?
Dichorionic Diamniotic
25%
How many fetal deaths occur due to DCDA?
10%
How many monozygotic twins are classified MCDA?
Monochorionic Diamniotic
73%
How many fetal deaths occur due to MCDA?
10%
ow many monozygotic twins are classified MCMA?
Monochorionic Monoamniotic
2%
How many fetal deaths occur due to MCMA?
25%
How many twin pregnancy ends in a singleton birth?
70%
What is vanishing twin?
a small cystic collection appearing adjacent to gestational sac, that
appears to be a second gestational sac gets smaller and smaller.
Usually disappearing by the second trimester
What is papyraceous?
fetus passes around 14 weeks
fluid is reabsorbed
lost twin is wrapped in amniotic membrane
pushed to the side by developing fetus
persists as a soft tissue mass
When one twin dies the other may live depending on?
chorionicity
amnionicity
uterine response
What are problems of MCMA twins?
twin to twin transfusion
entangles umbilical cord
What are problems of MCDA twins?
twin to twin transfusion
stuck twin
What form of twins are in danger of twin to twin transfusion?
Monozygotic twins
MCMA
MCDA
What is twin to twin transfusion?
A/V shunt within the placenta
arterial blood of one twin is pumped into venous system of
the other twin
What happens to the donor with twin to twin transfusion?
anemic
IUGR
oligohydramnios
What happens to the recipient with twin to twin transfusion?
LGA = large for gestational age
polyhydramnios
Too much glucose and urinates to try to rid of it
eventually leads to CHF and possible death
What is the term used for abnormal growth when one twin is much
larger than the other?
Discordant growth
What is the term used for normal growth of twins?
concordant
When is evaluation of the number of chorions and amnions done?
best done in 1st trimeter
What are the signs of DCDA twins?
lambda sign
thick separating membrane
What are the signs of MCDA twins?
T sign
thin separating membrane
What is for sure when twins are of different genders?
dizygotic
DCDA
If cords insert into placenta at different locations?
DCDA
What is discordant growth?
differences of estimated weight between monochorionic twins is
greater than 20%
What is concordant growth?
differences of estimated weight between monochorionic twins is less
than 20%
During singleton pregnancy when is growth a cause for concern?
10th & 90th percentile
Real world
5th & 95th
What is dolichocephaly?
skiny head
common in twins
Why is dolichocephaly a pitfall?
underestimates BPD
What is Fetal Hydrops?
AKA Hydrops fatalis. Two sites of fluid accumulation or one site of
fluid collection and fetal ascites.
What is another name for fetal hydrops?
Hydrops fatalis
What are the types of fetal hydrops?
Immune Hydrops: results of Rh sensitivity
Nonimmune Hydrops: any hydrops in the absence of Rh sensitivity
What is Immune hydrops?
results of Rh sensitivity
What is Nonimmune Hydrops?
any hydrops in the absence of Rh sensitivity
What is the sonographic appearance of Fetal Hydrops?
Fluid collection
Fetal Ascites
Scalp Edema
Skin edema
Pleural Effusion
Pericardial effusion
Polyhydramnios
Large thick placenta
Enlarged fetal liver and spleen
Congestive heart failure
What is Rh sensitivity?
Rh- mother & Rh+ father = Rh+ baby
On second baby mothers antebodies cross the placenta and
cause hemolysis of eurthrocytes
baby tries to increase erythrocytes production
causing:
FCHF
Anemia
Edema
How is Rh sensitivity treated?
Rhogam shots at
28 weeks
3 days before delivery
anytime a procedure is done
What is Rh+ immunoglobin?
Rogram
anti-D
How is Immune Hydrops diagnosed?
ABO -Rh blood typing
antibody screening
Spectrophotometric evaluation of amniocentesis fro bilirubin
at 26 - 28 weeks
What is unlikely if antibody titer of < 1:16
interuterine fetal death
What is what i if antibody titer of < 1:16
interuterine fetal death
What is the sonographic appearance of Immune Hydrops?
Fluid collection
Fetal Ascites
Scalp Edema
Skin edema
Pleural Effusion
Pericardial effusion
Polyhydramnios
Large thick placenta
Enlarged fetal liver and spleen
Congestive heart failure
How is Immune Hydrops diagnosed?
Amniocentesis - Old method
Cordocentesis -
What can be checked with Cordocentesis?
fetal hemoglobin
test for bilirubin
if elevated excessive destruction of red blood cells
What does low hemoglobin mean during a Cordocentesis?
baby is anemic
transfusion can be done during Cordocentesis.
What is Low Zone immune Hydrops?
mildly affected
deliverable at term
What is Mid Zone immune Hydrops?
Fetus is affected but not an emergency
early delivery of intrauterine transfusion may be indicated
What is High Zone immune Hydrops?
Emergency
immediate treatment
What is Alloimmune Thrombocytopenia?
mother develops an immune response to fetal platelets
antibodes are produced
Baby has deficiency of cells for blood clotting
baby suffers from hemolysis
What is the treatment for Alloimmune Thrombocytopenia?
via cordocentisis
What is NIH?
Nonimmune Hydrops
Not a result of Rh- sensistivity
What are the causes of NIH?
Cardiovascular
Chromosomal
Twin to twin transfer
Urinary respiratory
G.I problems
Liver problems
Infectious problems
Placenta and umbilical cord problems
Parvo
What is Parvo?
dangerous to pregnant women before 20 weeks
What does parvo cause?
Hydrops
What is 5th disease?
Parvo
What is slap cheek syndrome?
parvo
What is done to determine the cause of non immune hydrops?
ultrasound
What is the sonographic appearance of NIH?
edema
* especially scalp edema
fetal ascites
pleural effusion
pericardial effusion
polyhydramnios
large thick placenta
fetal hepatomegaly
fetal spleenomegaly
What is Insulin Diabetes Mellitis?
Type I
pancreas does not produce enough insulin
Why is Type 1 Diabetes dangerous during pregnancy?
Elevated glucose fires up fetal growth (FAT babies)
fetuses are frequently macrosomic
shoulder dystokia
Increased difficult labor
increased fetal death
incidence of neural tube defect increases 10 fold
What is macrosomic?
Big ass baby
8 lbs 13 oz
4000 grams
What is done for diabetic pregnancy?
frequent U/S
What are the sonographic findings more common to diabetic mothers?
fetal macrosomia
polydramnios
increased fetal adipose tissue
caudal regression syndrome
congenital heart defects
Neural tube defects
What should be considered if polyhydramnios with a baby that is macrosomia?
Gestational Diabetes
Insulin diabetic who have diabetes under control reduce the risk of
structural anomalies
...
What are the sonographic appearance of Hypertension?
small placenta
Growth retardation
oligohydraminos
placenta abruption
What is Eclampsia?
Pregnancy induced hypertension prior to 20 weeks
What are possible problems of patients with pre-eclampsia?
maternal proteinuria
edema
possible seizures
What are possible problems of patients with sever pre-eclampsia?
baby must be delivered immediately
What are possible problems of patients with Eclampsia?
seizures and/or coma
What are some causes of Maternal Vomiting?
Hyperenemis graviarum
gallstones
peptic ulcers
trophoblastic disease
Twins = Higher hcg
What can excessive vomiting cause?
dehydration
admitted for IV therapy
How many preg patients will have bacteria?
4-6%
25% of 4-6 will have UTI
Why is mild hydronephrosis normal in pregnancy?
progesterone dilates the ureteric smooth muscle
uterine compression of the ureters
*Sever hydronephrosis is ABNORMAL
What is a Dysgerminoma?
germ cell tumor female counterpart of seminoma. Corpus Luteum of
pregnancy does not resolve
What is the Sonographic Appearance of Dysgerminoma?
Cyst on ovary
8 – 10 cm
Why are fibroids problematic with pregnancy?
grow in response to estrogen. Can rapidly grow and undergo necrosis.
They can become large and interfere with pregnancy.
compression effects on baby
Causing pain and preterm labor
How to tell the difference between fibroids and uternine contractions?
contractions resolve within 30 minutes
different blood flow patterns
What is fetal demise?
absence of fetal tone after 20 weeks
1/2 of fetal deaths can have determining factors
infection
congenital anomalies
pre-eclampsia
placenta abruption
diabetes growth retardation
Rh sensitivity
How many miscarriages happen in the 1st trimester?
15/20 : 100
What are signs of viability?
TV heartbeat at 5.5 weeks
Lack of fetal Doppler after 12 weeks or fetal movement after 16 weeks prompts?
Ultrasound
What are the signs of long term fetal death?
overlapping cranium (spaulding sign)
liquefaction of brain material
skin thickening / scalp edema
dependency
gas shadowing - Roberts sign
What is spaulding sign?
overlapping cranium
What is robert's sign in abdomen?
gas shadowing within fetus
What is Premature labor?
Onset of labor prior to 37 weeks gestation
What are possible causes of premature labor?
PROM
Intrauterine infection
Bleeding
Fetal abnormalities
Polyhydramnios
Multiples
IUGR
Maternal diabetes/hypertension
What are increased risks to the fetus With premature labor?
RDS
Intracranial hemorrhage
GI Immaturity
Eating problems but
At what a week he is a fetus viable In Born early?
22 weeks
What is EFW?
Estimated fetal weight
What is the EFW of a viable fetus?
Greater than 500 g
*22 weeks
What is PROM management?
Watching for signs of fetal distress
Infection
Monitor and olighydramnios
meconium and in fluid
What is external cephalic version?
Looking the baby
How many babies are breach at term?
4%
Why would an external cephalic version be performed?
Tried to reduce the number of Breech Babies
Breech babies are more likely to have a C-section
The section increases risk, Length of stay and length of recovery
Breech babies have low APGAR scores
What are breach babies increased risk for?
Cord prolapse
Prolonged labor - Increased risk of death
Complications - higher risk of chromosomal abnormalities
Wind is an external cephalic version most successful?
between 37 - 38 weeks
What should happen if call made of omphalocele in 1st trimester?
Re scan at 14 to 15 weeks to rule out rotation of mid gut
What is gastroschisis?
A wall defects tends to occur in boys on the right side
What is the sonographic appearance of gastroschisis?
Free floating loops of bowel in the amniotic fluid
What is Omphalocele?
the intestines, liver, and occasionally other organs remain outside
of the abdomen in a sac
35 – 60% caused by chromosomal abnormaities (bowel)
What is the sonographic appearance of Omphalocele?
intestines appear outside abdomen in pouch
At what week is head identified?
What is the dominant feature?
7 weeks
choroid plexus is the dominant feature
When is cranial anatomy best viewed?
12 - 14 weeks
What is the difference between omphalocele and gastroschisis?
omphalocele has a surrounding membrane
gastroschisis is in direct contact with amniotic fluid
What is Anacephaly?
Failure of closure of neurotube at cephalic end, brain is in direct
contact with amniotic fluid and dissolves.
What is the sonographic appearance of Anecephaly?
Frog apearance
no parenchymal tissue is seen above the orbits
What is Hydrancephaly?
brain necrosis results from obstruction of ICA – lack of nutrients
What is the sonographic appearance of Hydrancephaly?
Cystic mass in place of brain parenchyma
What is Turner syndrome?
congenital endocrine disorder
ovaries do not respond to FSH & LH
What is Cystic Hygroma?
Sign of Turner syndrome. Bad insertion of lymphatics into IJV.
Associated with Trisomy 12, 18, 21
What is the sonographic appearance of Cystic Hygroma?
Cystic mass in cervical region
septated
What is a umbilical cord cyst?
benign
Wharton's Jelly cysts
ophalomesentery duct cyst
Monitor for changes (can be caused by other abnormalities)
What is a placental hematoma?
collection of blood from detached placenta
Prognosis – size dependent
What is a Corpus Luteum Cyst?
secretes progesterone to support pregnancy until placenta takes over.
Less than 5 cm – normal
Greater than 5cm – intervention needed
Sonographic Appearance:
Septations
What is the most common location of an ectopic pregnancy?
ampulla - 80%
fimbrae - 0.5%
isthmus - 15%
Cervix - 0.1%
How many maternal deaths are ectopic pregnancy?
10%
What is the most dangerous area for ectopic?
interstitial AKA Cornial
rarest and most dangerous
very vascular
What are the associated risks factors of an ectopic?
PID
IUCD
fallopian tube surgery
inferitlity treatment
previous
What is the presentation of an ectopic?
Pain 97%
Vag bleeding 75%
palpable adnexal mass 50%
What do the beta hCG levels need to be to see an IUP?
500 IU/L trans vag
1800 IU/L trans abdominal
What will the Beta hCG levels be with ectopic?
lower than IUP
BhCG levels double every ____________?
2 days 1st 6 weeks
3 days 6+ weeks
What is a ring of fire?
Doppler
ectopic - trophoblastic tissue lights up
corpus luteum cyst - lights up also
What is a heterotopic pregnancy?
simutaneous intrauterine and ectrauterine pregnancy
Very rare
1:6000 / 8000 pregnancy
What is the cornual pregnancy ?
Ectopic pregnancy at cornual
Life threatening condition due to increased area vascularity and
possible rupture of tissue
SURGERY
RARE
How are ovarian ectopic pregnancies identify?
But complex mass on the ovary
Differential diagnosis hemorrhagic corpus luteum cyst
RARE 0.5%
What percent of pregnancies are abnormal?
4%
What day should a live embryo be seen?
46
6 weeks
What is a blighted ovum?
a fertilized ovum that does not result in a embryo.
something goes wrong after implantation.
normal signs of pregnancy will occur
What are the signs of a blighted ovum?
Large gestation all sac without inter gestation all anatomy
irregular shaped or abnormally shaped gestation all sac
What should the fetal heart rate be in first trimester?
90 to 170 bpm
Less than 90 bpm is very pour prognosis
Oligiohydramnios in 1st trimester
Poor prognosis
Associated with babies that are starving baby that are starving do
not urinate
What is the sonographic appearance of a complete miscarriage?
Empty uterus
No free fluid
No adnexal mass
hCG should be declining
What is the sonographic appearance of a incomplete miscarriage?
gestational sac may be normal with embryo w/ no fetal heart rate
misshappen gestational sac
RPOC?
retained products of conseption
What is a threatened abortion?
vaginal bleeding with a closed cervical OS in a preganancy of less
than 20 weeks.
What are the three forms of tropoblastic disease?
hydatiform mole - growth that forms inside the womb (uterus) at the
beginning of a pregnancy. Partial (2-1) complete (1-0)
invasive mole - chorioadenoma destruens grows
into the muscular wall of the uterus
choriocarcinoma -
What is the sonographic appearance of Gestational tropoblastic disease?
snowstorm late 1st
sac of grapes in 2nd
What are the two types of IUGR?
symmetrical
asymmetrical
10th (5th) percentile
What are the risk factors for IUGR?
previous
maternal hypertension
tobacco
uterine anomolies
placental hemorrhage
What are the problems associated with IUGR?
increased risk of antepartum death
perinatal asphyxia
Neonatal morbidity
later development problems
What usually causes symmetric IUGR?
1st trimester insult
hypertension
diabetes
What type of IUGR is most common?
asymmetric
usually caused by placental insufficiency
What is suggestive of Head sparring IUGR?
BPD & HC normal
AC small
What is suggestive of femur sparring IUGR?
FL 90th percentile
AC below 5th
What is the best indicator of IUGR?
AC
liver is severely affected by IUGR
What is the best indicator for predicting a symmetrical IUGR?
HC/AC ratio
EFW decreasing
ratio increases with increasing gestational age with IUGR
What is indicative of oligohydramnios?
polyhydramnios?
oligo< 5cm
poly >22 cm
What are the placental markers that indicate IUGR?
decreased placental thickness < 1.5 cm
grade 3 before 36 weeks
NOT good method!
What is the chance of fetal loss with CVS?
1% - 3%
missing limbs risk too
What are the advantages of CVS?
early (10-12 weeks)
results in 1 week
more options if early
What are the benefits of amniocentesis?
when is it done?
disgnose spina bifida
chromosomal abnormalities
15 - 20 weeks
Why would amnio be performed?
advanced maternal age
children with chromosomal abnormalities
AFT
U/S detected problems
What are physical features suggesting chromosomal abnormalities?
clenched hands
5th middle phalanx hypoplasia
choroid plexus cysts
ventriularmegaly
thickened nuchal fold
cardiac anomalies
omphalocele
spina bifida
foot anomalies
What is PUBS?
Percutaneous umbilical cord sampling
difficult
done on patients when CVS and amnio inconclusive
What is FISH?
experimental
florescent chromosomal markers into amniotic fluid
early detection of Trisomy 13 18 21
amniocentesis must be done after
Where is AFP found?
fetal spine
GI tract
liver
kidneys
transported to mother placenta
What are the causes of elevated AFP?
ectopia corditis
anterior abdominal wall defect
bowel obstruction
amniotic band syndrome
twins
renal disorders
placental lesions
fetal heart disease - hydrops / ascites
Cystic hygroma
maternal & fetal liver disease
oligohydramnios
heredity
blood contaminated anmiocentesis
virus / infection
high blood pressure
What are the causes of decreased AFP?
Trisomy 13, 18, 21
fetus younger than expected
fetal death
hydatidiform mole
spontaneous abortion
When do fetal AFP levels peak?
15 - 18 weeks.
Trisomy 18
Edwards not good usually fatal
Trisomy 21
downs
Trisomy 13
Patau's syndrom