Instructions for Side by Side Printing
- Print the notecards
- Fold each page in half along the solid vertical line
- Cut out the notecards by cutting along each horizontal dotted line
- Optional: Glue, tape or staple the ends of each notecard together
OB 1
front 1  | back 1 Complete Breech |
front 2  | back 2 Frank Breech |
front 3 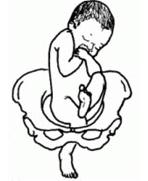 | back 3 Footling Breech |
front 4 When is the embryonic period? | back 4 6-12 weeks |
front 5 When is the 1st trimester? | back 5 0 - 13 weeks |
front 6 When is the Fetal Phase? | back 6 12 + weeks |
front 7 When is the 2nd trimester? | back 7 14 - 26 weeks |
front 8 Dissecting vrs concealed? | back 8 in a marginal abruption the hemorrhage dissects beneath the placental
|
front 9 How many days is a normal pregnancy? | back 9 280 days |
front 10 What makes an OB scan difficult? | back 10 patient habitus |
front 11 What is the purpose of a full bladder during an OB scan? | back 11 to measure the cervix
|
front 12 What is the normal measurement of the cervix? | back 12 3 cm |
front 13 What are the measurements for an OB scan? | back 13 BPD
|
front 14 What images need to be included? | back 14 Face
|
front 15 What is a cephalic position? | back 15 generic term for head down |
front 16 What are the different fetal positions? | back 16 longitudinal lie
|
front 17 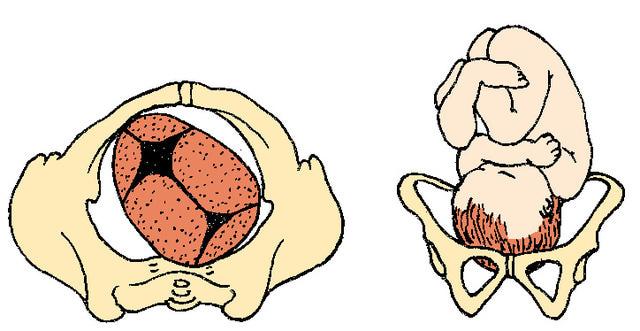 | back 17 Left Occiput Posterior
|
front 18 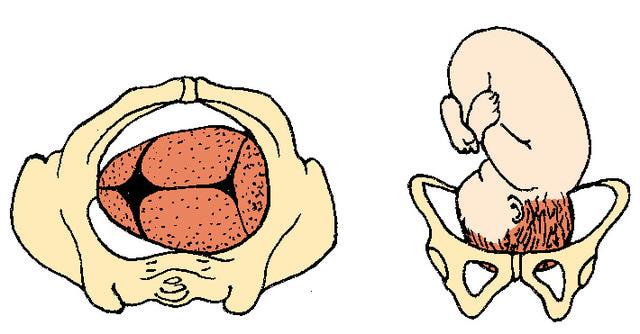 | back 18 Left Occiput Transverse
|
front 19 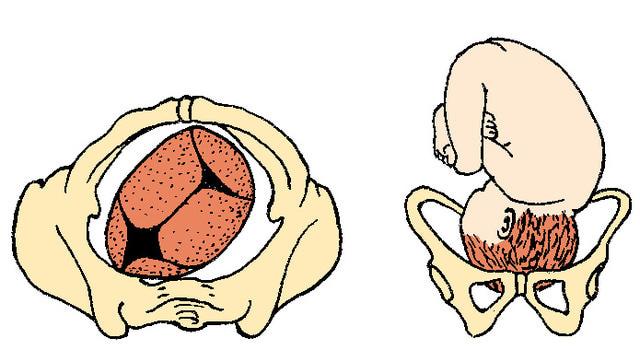 | back 19 Left Occiput Anterior
|
front 20 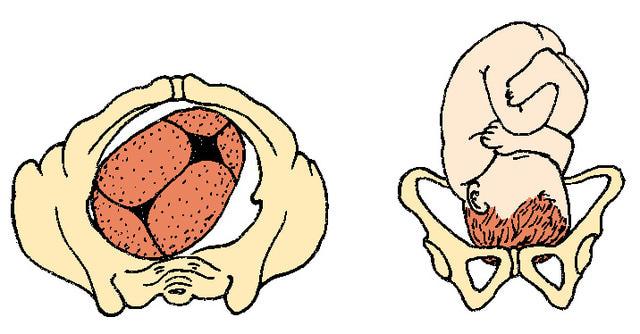 | back 20 Right Occiput Posterior
|
front 21 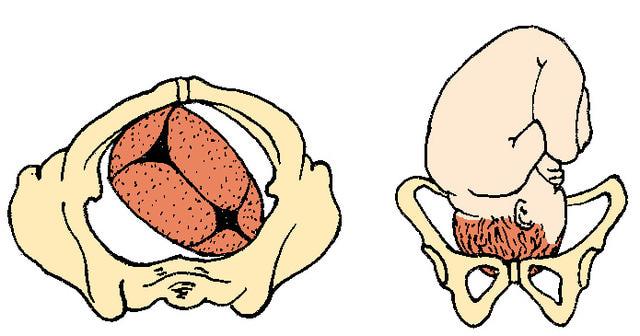 | back 21 Right Occiput Anterior
|
front 22 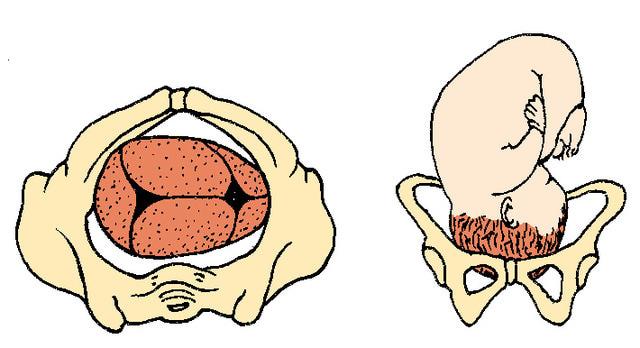 | back 22 Right Occiput Transverse
|
front 23 What are the two footling breech positions? | back 23 single footling
|
front 24 What is an ECV? | back 24 external cephalic version |
front 25 What must be done before an ECV can be performed? | back 25 OR must be booked in case of an emergency birth. |
front 26 What can a shoulder presentation lead to? | back 26 Shoulder Dystocia |
front 27 What is shoulder dystocia? | back 27 obstructed labour whereby after the delivery of the head, the
|
front 28 What is the vertex presentation? | back 28 anterior and posterior fontanel presenting |
front 29 How many babies are cephalic after 34 weeks? | back 29 90% |
front 30 How many babies are breech at term? | back 30 3% to 4% |
front 31 What is the incidence of abnormalities in breech babies? | back 31 6.3% |
front 32 What is the incidence of abnormalities in vertex babies? | back 32 2.4% |
front 33 What plane are brain anatomy and measurements taken in? | back 33 transverse |
front 34 What should you do if the head is round rather than oval? | back 34 slide inferior |
front 35 What can free a low head from the pelvis? | back 35 drinking water (filling bladder)
|
front 36 What images are taken of the fetal head? | back 36 Faux cerebri (IHF)
|
front 37 What does the presence of the faux cerebri imply? | back 37 separation of the cerebrum has occured |
front 38 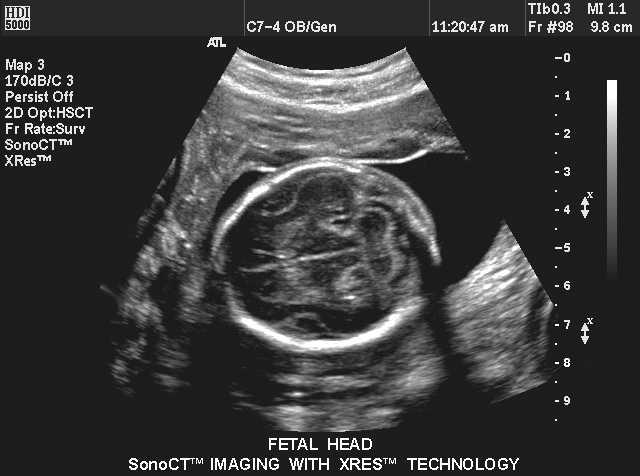 | back 38 Faux cerebri |
front 39 What is the function of the choroid plexus? | back 39 produce cerebrospinal fluid |
front 40 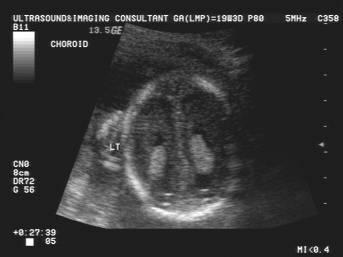 | back 40 Choroid Plexus |
front 41 What is the size of the choroid plexus at 20 week scan? | back 41 10 mm or less |
front 42 Why is the choroid plexus image taken? | back 42 to exclude ventricular megaly |
front 43 What is a dangling choroid plexus caused by? | back 43 ventricular megaly |
front 44 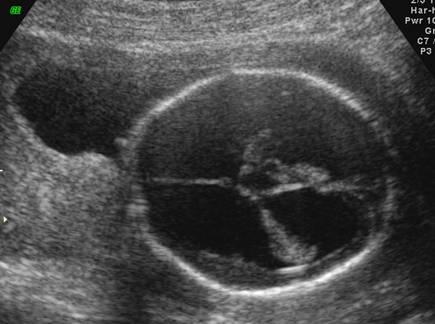 | back 44 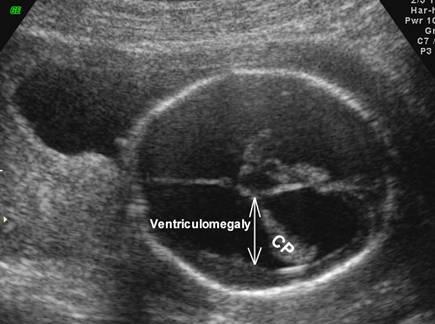 dangling choroid plexus |
front 45 What is the significance of choroid plexus cysts? | back 45 none baby can become brain surgeon or
|
front 46 WHAT IS TRISOMY 18? | back 46 Trisomy 18, also known as Edwards syndrome, is a condition which is
|
front 47 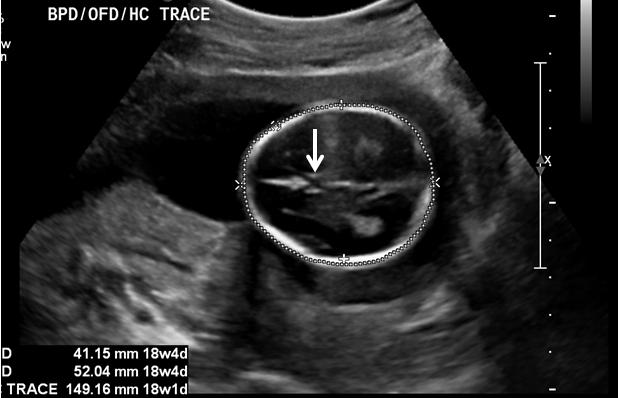 | back 47 Cavum Septum Pellucidum |
front 48 What is the cavum septum pellucidum? | back 48 arched band of nervous tissue that connects left & right cerebrum |
front 49 What does the visualization of the cavum septum pellucidum imply? | back 49 excludes agenesis of corpus callosum |
front 50 At what level is the BPD and HC taken? | back 50 the level of the thalami |
front 51 What is the function of the thalami? | back 51 receive sensory impulses and transmits them to the cerebrum |
front 52 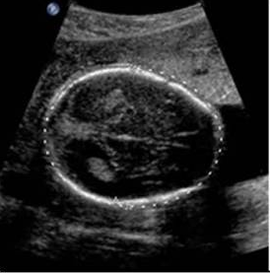 | back 52 thalami view |
front 53 What is the function of the cerebral peduncles? | back 53 receive impulses from brain stem and transmit them to cerebrum
|
front 54 How do you find the cerebral peduncles? | back 54 first find the thalami and the peduncles with pop out |
front 55 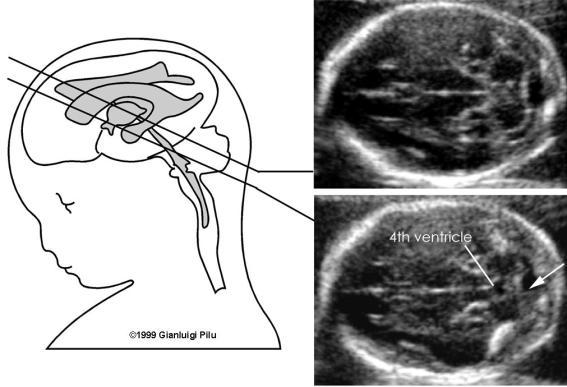 | back 55 cerebral peduncles |
front 56 What is the function of the cerebellum? | back 56 equilibrium |
front 57 What is the measurement of the cisterna magna at 20 weeks? | back 57 10 mm or less |
front 58 What is the nuchal fold? | back 58 skin behind the neck |
front 59 What is the normal measurement of the nuchal fold? | back 59 5 mm of less |
front 60 What does the nuchal fold measurement determine? | back 60 rules out trisomy 21
|
front 61 What is anophthalmia? | back 61 No eyes |
front 62 What is hypotelorism? | back 62 close eyes |
front 63 What is hypertelorism? | back 63 far eyes |
front 64 What is the purpose of taking an image of the orbits? | back 64 to rule out
|
front 65 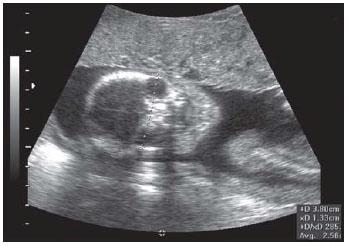 | back 65 orbits |
front 66 What is the purpose of the profile image? | back 66 exclude
|
front 67 What is anterior cephalocele? | back 67 unicorn bony defect |
front 68 What is frontal bossing? | back 68 protuding forehead |
front 69 What is the significance of fetal tongue out? | back 69 Bad news -
|
front 70 What is Beckwith-Wiedemann syndrome? | back 70 an overgrowth syndrome, which means that affected infants are
|
front 71 What is micrognathia? | back 71 no chin |
front 72 What is the purpose of coronal facial views? | back 72 exclude cleft lip
|
front 73 How many cervical vertebra are there? | back 73 7 |
front 74 What happens to the cervical vertebra at the base of the skull? | back 74 widens |
front 75 How many thoracic vertebra? | back 75 12 |
front 76 How many lumbar vertebra? | back 76 5 |
front 77 How many sacral vertebra? | back 77 5 |
front 78 How many coccyx vertebra? | back 78 4 |
front 79 What happens to the spine at the sacrum? | back 79 tapers |
front 80 What is the most important when evaluating the spine? | back 80 follow skin covering
|
front 81 How do the lungs appear in the 1st & 2nd trimester? | back 81 isoechoic to the liver |
front 82 How do the lungs appear in the 3rd trimester? | back 82 hyperechoic to the liver |
front 83 What is situ? | back 83 positioning |
front 84 What should happen if call made of omphalocele in 1st trimester? | back 84 Rescan at 14 to 15 weeks to rule out rotation of mid gut |
front 85 How is situ evaluated? | back 85 apex of heart points to left
|
front 86 How many heart anomalies can be excluded with the 4 chamber view? | back 86 65% |
front 87 How many heart anomalies can be excluded with the 5 chamber view? | back 87 85% |
front 88 What age can a pediatric echo be done to examine the heart? | back 88 18 weeks gestation |
front 89 Symetry in the heart | back 89 no data |
front 90 What is the function of the foramen ovale? | back 90 shunting of blood from right to left |
front 91 How much blood is shunted through the foramen ovale? | back 91 60% |
front 92 What skirts blood through the foramen ovale? | back 92 eustation valve |
front 93 Why must the heart septum be evaluated? | back 93 exclude wall defects |
front 94 How is the 5 chamber best viewed? | back 94 baby lieing on back |
front 95 How do you get the 5 chamber / aorta image? | back 95 angle up from 4 chamber view |
front 96 How do you get the 5 chamber / pulmonary artery image? | back 96 angle up from aorta |
front 97 What is evaluated to rule out diaphragmatic hernia? | back 97 heart superior to diaphragm
|
front 98 Where do diaphragm abnormalities usually occur? | back 98 left side |
front 99 Why is a diaphragmatic hernia dangerous? | back 99 stomach can move to the thoracic |
front 100 What is esophagus atresia? | back 100 no stomach
|
front 101 When is the stomach apparent? | back 101 11 wks |
front 102 When must the stomach be seen? | back 102 16 wks |
front 103 Why are the small intestines evaluated? | back 103 rule out meconium spillage
|
front 104 Why are the large intestines evaluated? | back 104 to rule out anal atresia |
front 105 What is the sonographic appearance of anal atresia? | back 105 dilated loops of bowel |
front 106 When are the kidneys seen? | back 106 15 weeks |
front 107 Where are the kidneys located? | back 107 retroperitoneal |
front 108 how much of the abdominal circumference do the kidneys take up? | back 108 1/3 |
front 109 What is the normal measurement of the renal pelvis in the 2nd trimester? | back 109 5 mm or less |
front 110 What is the normal measurement of the renal pelvis in the 3rd trimester? | back 110 7 mm or less |
front 111 If the measurement of the renal pelvis is greater than 10 mm? | back 111 BAD |
front 112 Where are the adrenals located? | back 112 superior to the kidneys |
front 113 When can the adrenals be seen? | back 113 20 weeks |
front 114 What is one of the problems scanning the adrenals? | back 114 can mimic kidneys
|
front 115 What is the size of the adrenals? | back 115 50% the size of the kidneys |
front 116 When can swallowing be seen? | back 116 8 - 11 weeks |
front 117 What is the significance of the bladder being seen? | back 117 at least one kidney exists |
front 118 At what age are the kidneys fully functioning? | back 118 16 weeks |
front 119 What is the function of the kidneys before birth? | back 119 produce amniotic fluid |
front 120 How often does a fetus void? | back 120 30 to 45 minutes |
front 121 When does AFL peak? | back 121 34 weeks |
front 122 When is XY genitalia best determined? | back 122 20 weeks
|
front 123 What is gender linked disorder? | back 123 hemophilia |
front 124 When is XX genitalia best determined? | back 124 20 weeks
|
front 125 Why is it important to evaluate long bones? | back 125 determine fetal age
|
front 126 What is skeletal dysplasia? | back 126 dwarfism |
front 127 When is the proximal humerus epiphyssis apparent? | back 127 39 weeks |
front 128 What does the distal femoral epiphyssis indicate? | back 128 gestational age between 33 - 35 weeks |
front 129 What do you evaluate with the extremities? | back 129 3 bones visible |
front 130 What do you evaluate with the hands? | back 130 open good
|
front 131 When the feet have a sandal gap what is indicated? | back 131 downs syndrome |
front 132 what is a sandal gap? | back 132 gap between big toe and 2nd toe |
front 133 What is the function of amniotic fluid? | back 133 movement
|
front 134 What is AFI? | back 134 amniotic fluid index? |
front 135 What contributes to amniotic fluid? | back 135 kidneys, lungs, cord & skin |
front 136 When does fetal urine account for almost all amniotic fluid? | back 136 20 weeks |
front 137 What is the sonographic appearance of amniotic fluid? | back 137 anechoic
|
front 138 When is AFI measured routinely? | back 138 after 24 weeks |
front 139 What is oligohydraminos? | back 139 too little fluid |
front 140 What is oligohydraminos? | back 140 no data |
front 141 What is pulmonary hyperplasia? | back 141 bad lung formation |
front 142 What can oligohydraminos cause? | back 142 pulmonary hyperplasia
|
front 143 What is a BPP? | back 143 evaluation of fetal well being |
front 144 What is evaluated during a BPP? | back 144 NST
|
front 145 What is NST? | back 145 Neonatal stress test
|
front 146 How is fetal tone evaluated? | back 146 extension & flexion |
front 147 How is fetal breathing evaluated? | back 147 30 seconds worth |
front 148 How is fetal movement evaluated? | back 148 trunk movement |
front 149 How is AFI evaluated? | back 149 2 cm puddle |
front 150 What is conceptual age? | back 150 fetal age
|
front 151 conceptual age + 14 days = | back 151 menstrual age |
front 152 What is nagele's rule? | back 152 used my
|
front 153 What is menstrual age? | back 153 gestational age |
front 154 What is gestational age based on? | back 154 first day of LMP |
front 155 What is gestational age used for? | back 155 scedule invasive procedures
|
front 156 What is the most accurate sonographic technique for establishing
| back 156 3 CRL
|
front 157 What is the accuracy of the CRL? | back 157 +/- 5 days
|
front 158 Why is s the CRL and excellent correlation of length and age? | back 158 pathological conditions minimally affect growth in the first trimester |
front 159 What is the formula for gestational age in weeks? | back 159 (CRL)cm +6 |
front 160 When does the CRL become inaccurate? | back 160 after 12 weeks |
front 161 Why is the CRL inaccurate after 12 weeks? | back 161 due to movement including extension and flexion |
front 162 What is BPD? | back 162 Biparietal diameter |
front 163 What is the accuracy of a BPD between 17 - 26 weeks? | back 163 +/- 11 days |
front 164 What is the accuracy of a BPD after 26 weeks? | back 164 +/- 3 weeks |
front 165 How is the BPD measurement taken? | back 165 outer to inner |
front 166 What landmarks should bee visualized at the area of a BPD measurement? | back 166 Falx cerebri
|
front 167 What is the ambiguous stage of the fetus? | back 167 13 - 14 weeks |
front 168 Why is 13 - 14 weeks considered the ambiguous stage? | back 168 fetus is too big for CRL yet the landmarks for a BPD are not seen yet.
|
front 169 What is the formula for HC? | back 169 (BPD + OFD)(Pie)/2 |
front 170 How is the HC measurement taken? | back 170 outer to outer |
front 171 Why is the HC a valuable measurement? | back 171 less affected by head compression |
front 172 What should the shape of the head be in a fetus? | back 172 ovid |
front 173 What does brachycephaly refer to? | back 173 a round head |
front 174 How are the BPD measurements inaccurate with brachycephaly? | back 174 overestimate |
front 175 What does Dolichocephaly refer to? | back 175 elongated head |
front 176 How are the BPD measurements inaccurate with dolichocephaly? | back 176 underestimate |
front 177 What is the cephalic index? | back 177 devised to determine the normality of the fetal head shape |
front 178 What is the formula for C.I,? | back 178 BPD / OFD x 100 |
front 179 If the C.I. is <75% what is indicated? | back 179 dolichocephaly |
front 180 If the C.I. is >85% what is indicated? | back 180 brachycephaly |
front 181 If the C.I. is between 75% - 85% what is indicated? | back 181 Normal |
front 182 What is AC? | back 182 abdominal circumference |
front 183 Where is the AC taken? | back 183 level of the liver where the umbilical vein branches in the left
|
front 184 The the AC should be taken in what plane? | back 184 transverse |
front 185 What is the AC formula? | back 185 (D1 +D2)(pie) /2 |
front 186 What are the landmarks of the AC measurement? | back 186 stomach
|
front 187 What is the importance of the AC? | back 187 Useful in predicting fetal weight
|
front 188 How accurate is femur length when determining GA? | back 188 about as accurate as BPD |
front 189 When would you use femur length fo determine GA? | back 189 fetal head can not be measured due to position or anomaly
|
front 190 Where is the femur measured? | back 190 from greater trochanter to the distal femoral condyle |
front 191 What should happen if there is a > 2 week difference with other
| back 191 measure all fetal bone
|
front 192 What is a short femur a marker for? | back 192 trisomy
|
front 193 What are the normal gram measurement of the orbits? | back 193 ocular distance (OD)
|
front 194 What is inter-ocular distance (IOD)? | back 194 between eyes |
front 195 What is the binocular distance (BD)? | back 195 distance from outer orbit to contra-lateral outer orbit |
front 196 What is the ocular distance (OD)? | back 196 distance of the orbit |
front 197 What is the best measure of GA with the orbital measurements? | back 197 BD binocular distance |
front 198 How are the orbital measurements taken? | back 198 outer to outer |
front 199 When is a orbital measurement used to determine GA? | back 199 when ventriculomegaly or skeletal dysplasia exists making BPD
|
front 200 What are the orbital measurements useful in excluding? | back 200 Hypotelorism
|
front 201 What is Hypotelorism? | back 201 close eyes |
front 202 What is hypertelorism? | back 202 wide eyes |
front 203 What is anophthalmus? | back 203 no eyes |
front 204 What is microphthalmos? | back 204 small eyes |
front 205 What are the parts of the cerebellum? | back 205 vermis and 2 lobes |
front 206 Why is the cerebellum measured? | back 206 good correlation with GA
|
front 207 What is Arnold Chiari? | back 207 downward displacement of the cerebellum through the foramen magnum
|
front 208 What is Dandy Walker? | back 208 hypoplasia of the vermis and cephalad rotation of the vermian
|
front 209 The placenta is composed of two components, what are they? | back 209 tissue from both mother and fetus |
front 210 What is the fetal part of the placenta called? | back 210 Chorionic plate
|
front 211 What is the maternal part of the placenta called? | back 211 Decidua basalis
|
front 212 What is the Decidua? | back 212 uterine lining (endometrium) during a pregnancy, which forms the
|
front 213 What causes decidualize? | back 213 influence of hormones |
front 214 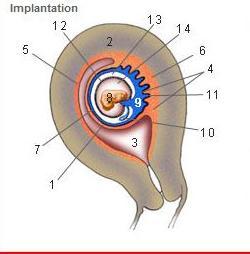 Where is the Desidua Capsularis? | back 214 1 |
front 215 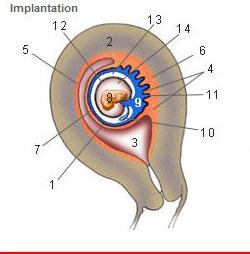 Where is the Desidua basalis? | back 215 6 |
front 216 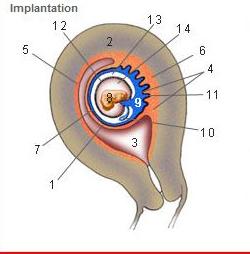 Where is the Desidua parietalis? | back 216 5 |
front 217 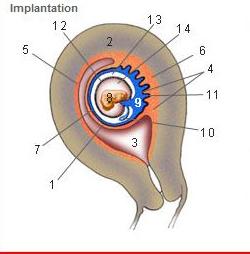 Where is the chorion frondosum? | back 217 11 |
front 218 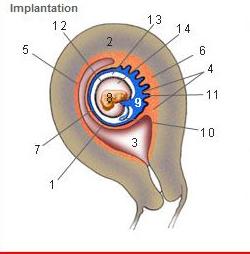 Where is the amnion? | back 218 12 |
front 219  Where is the chorionic cavity? | back 219 13 |
front 220 What is the chorionic villi? | back 220 functioning unit of the placenta
|
front 221 Where are the chorionic villi located? | back 221 intervillious space |
front 222 What is the chorionic villi responsible for? | back 222 exchange of:
|
front 223 Blood flow in the placenta is ______impedance. | back 223 low |
front 224 Explain the blood flow from the uterus to the placenta and back. | back 224 uterine arteries
|
front 225 What is the function of the placenta? | back 225 Nutrition
|
front 226 Explain the placenta evaluation. | back 226 position
|
front 227 What is changes in the maturing placenta referred to? | back 227 grading |
front 228 Placenta maturation does not occur at the same rate in women | back 228 no data |
front 229 What can affect the maturation process? | back 229 Rh disease
|
front 230 What is placenta grade 0? | back 230 smooth edges
|
front 231 What is placenta grade 1? | back 231 small intraplacental calcifications
|
front 232 What is placenta grade 2? | back 232 calcifications at basilar plate
|
front 233 What is placenta grade 3? | back 233 calcified indentions of placenta
|
front 234 What are some causes of delayed placental maturation? | back 234 maternal diabetes
|
front 235 What are some causes of advanced placental maturation? | back 235 maternal HTN
|
front 236 What are some causes of a small placenta? | back 236 placental infarct
|
front 237 What are some causes of a large placenta? | back 237 maternal diabetes
|
front 238 What is the normal size of the placenta? | back 238 less than 4 cm
|
front 239 What is Placental Accreta? | back 239 attaches to myometrium |
front 240 What is Placental Increta? | back 240 invades myometrium |
front 241 What is Placental Percreta? | back 241 penetrates through uterus
|
front 242 What are the risk factors of Placental Accreta? | back 242 placental previa
|
front 243 How is Placental Accreta detected? | back 243 elevated maternal serum AFT
|
front 244 What is the sonographic appearance of Placental Accreta? | back 244 absent or thin myometrium under placenta
|
front 245 Uterine wall should be thick! | back 245 no data |
front 246 What is a pregnancy loss of 19 week and under called? | back 246 miscarriage |
front 247 What is a pregnancy loss after 20 week called? | back 247 Fetal Death |
front 248 What is a placental abruption? | back 248 premature separation of the implanted placenta between 20 weeks and birth |
front 249 What is a placental abruption associated with? | back 249 preterm labor / delivery
|
front 250 How is placental abruption diagnosed? | back 250 history
|
front 251 What are the signs and symptoms of placental abruption? | back 251 vaginal bleeding
|
front 252 What are the risk factors of placental abruption? | back 252 hx of abruption
|
front 253 What is a Retroplacental abruption? | back 253 rupture of the spiral artery
|
front 254 What is Retroplacental abruption associated with? | back 254 HTN
|
front 255 What is the sonographic appearance of Retroplacental abruption? | back 255 anechoic subchorionic area between placenta and uterus
|
front 256 What is a subchorionic (marginal) abruption? | back 256 tears in the marginal vein
|
front 257 What is associated with subchorionic (marginal) abruption? | back 257 maternal cig smoking |
front 258 What is the sonographic appearance of subchorionic (marginal) abruption? | back 258 anechoic subchorionic area between placenta and uterus |
front 259 Dissecting vrs concealed? | back 259 in a marginal abruption the hemorrhage dissects beneath the placental
|
front 260 How far from the cervix is a low-lying placenta on a trans-abdominal exam? | back 260 less than 5 cm |
front 261 How far from the cervix is a low-lying placenta on a trans-abdominal exam? | back 261 less than 2.5 |
front 262 What is the #1 cause of painless 2nd & 3rd tri bleeding? | back 262 placental previa |
front 263 What are the risk factors for placenta previa? | back 263 multigravida
|
front 264 how many women have placenta previa after 24 weeks? | back 264 1: (150 =- 305) |
front 265 What are the different types of placenta previa? | back 265 partial
|
front 266 What is the difference between marginal and partial placental previa? | back 266 marginal just touches the cervix and partial covers some of the cervix |
front 267 How many pregnancy are normal? | back 267 96% |
front 268 What is wrong with the term placental migration? | back 268 Do not use around radiologists |
front 269 What are the placental masses and lesions? | back 269 chorioangioma
|
front 270 What is a placental lake? | back 270 subchorionic fibrin depositions
|
front 271 What is a placental chorioangioma? | back 271 vascular malformation, Similiar to a hemangioma
|
front 272 What is the sonographic appearance of chorioangioma? | back 272 well-circumscribed mass; usually lobulated
|
front 273 What is the cause of chorioangioma? | back 273 failure in development of the chorion villi persists |
front 274 What is placenta membranacea? | back 274 rare
|
front 275 What is placenta membranacea associated with? | back 275 increase risk of
|
front 276 How many pregnancy have placenta extrachorialis? | back 276 1% to 2% |
front 277 What are the two types of placenta extrachorialis? | back 277 circummarginate
|
front 278 What is circumvallate placenta extrachorialis? | back 278 chorionic plate is surrounded by a thick ring |
front 279 What is associated with circumvallate placenta extrachorialis? | back 279 PROM
|
front 280 What is circummarginate placenta extrachorialis? | back 280 chorionic plate is surrounded by a thin ring
|
front 281 How many pregnancies show placental cysts? | back 281 less than 20% |
front 282 Where are placental cysts usually located? | back 282 subchorionic |
front 283 placental cysts are difficult to separate from ______ ______. | back 283 intervillous thrombosis |
front 284 What is velamentous (membranous) cord insertion? | back 284 cord inserts at placental margin into corion laeve
|
front 285 How often does a velamentous (membranous) cord insertion occur? | back 285 1% of pregnancies |
front 286 What is velamentous (membranous) cord insertion associated with? | back 286 IUGR |
front 287 What is IUGR? | back 287 Interuterine growth regressor |
front 288 What is battledore placenta? | back 288 Cord inserts at placental margin.
|
front 289 How often does battledore placenta occur? | back 289 7% of pregnancies |
front 290 What is succenturiate placenta? | back 290 presence of one or more accessory lobes connected to the body of the
|
front 291 What is another name for succenturiate placenta? | back 291 bilobate placenta |
front 292 What is the main problem with succenturiate placenta? | back 292 can rupture during labor
|
front 293 What is the umbilical cord? | back 293 connection between the placenta and the fetus |
front 294 What is the function of the umbilical cord? | back 294 essential link for oxygen and nutrients |
front 295 What does the umbilical cord consist of? | back 295 2 umbilical arteries
|
front 296 When is the umbilical cord usually seen? | back 296 week 9 |
front 297 What is wharton's Jelly? | back 297 surrounds the vessels within the umbilical cord to protect them |
front 298 What is a short umbilical cord associated with? | back 298 abdominal wall defect |
front 299 What is a long umbilical cord associated with? | back 299 prolapse |
front 300 What is another name of the umbilical arteries? | back 300 hypogastric arteries |
front 301 What is umbilical cord prolapse? | back 301 cord gets caught in the endocervical canal |
front 302 What is an umbilical nuchal cord? | back 302 cord wraps around neck |
front 303 What is an umbilical true knots | back 303 knots |
front 304 How many pregnancies is is an SUA found? | back 304 1% |
front 305 What is an SUA? | back 305 single umbilical artery |
front 306 What is the most common umbilical cord anomaly? | back 306 single umbilical artery |
front 307 What is an SUA associated with? | back 307 congenital anomalies (25 - 50 %)
|
front 308 What should happen when a 2 vessel cord is found? | back 308 very aggressive at 20 week exam lookig for anomalies |
front 309 How to confirm two umbilical arteries. | back 309 follow cord from insertion to IIV |
front 310 What does the umbilical arteries become after birth? | back 310 hypogastric ligaments |
front 311 What is the normal A/B ratio in 3rd trimester? | back 311 less than 4:1 |
front 312 What is the RI after 26 weeks? | back 312 .45 - .58 |
front 313 End diastolic flow ______ with gestational age. | back 313 increases |
front 314 What is absent or reverse EDF associated with? | back 314 fetal morbidity and mortality |
front 315 What is the sonographic appearance of umbilical artery Doppler? | back 315 normal pulsatile pattern
|
front 316 What happens if there is not end-diastolic flow in the umbilical artery? | back 316 be ready to go to OR but not emergency at this time...IN RED |
front 317 What happens if there is reverse flow in the umbilical artery? | back 317 Emergency ....OR |
front 318 What are the umbilical cord masses? | back 318 allatoic duct cysts
|
front 319 What is an Allantoic Duct cysts? | back 319 Allantoic cysts of the umbilical cord are extremely rare anomalies. |
front 320 What are possible causes of a patient measuring Large for date? | back 320 gestational diabetes
|
front 321 What are possible causes of a patient with Increased Serum HCG? | back 321 gestational trophoblastic disease |
front 322 What are some possible causes of a patient with Increased AFP? | back 322 twins
|
front 323 What are the increased risks of twins? | back 323 fetal death
|
front 324 What is vasa previa | back 324 placenta over cervix
|
front 325 What is a fertilized egg called? | back 325 zygote |
front 326 What is a fertilized egg that splits causing twins called? | back 326 monozygotic |
front 327 What are two fertilized eggs causing twins called? | back 327 Dizygotic |
front 328 How are multiple pregnancies classified? | back 328 # of chorion
|
front 329 What does the amount of separation depend on? | back 329 time of cell division |
front 330 If a monozygotic divides 1-3 days post conception what is the result? | back 330 Dichorionic Diamniotic |
front 331 If a monozygotic divides 4-8 days post conception what is the result? | back 331 Monochorionic Diamniotic |
front 332 If a monozygotic divides 8-13 days post conception what is the result? | back 332 Monochorionic Monoamniotic |
front 333 If a monozygotic divides 13+ days post conception what is the result? | back 333 conjoined twins |
front 334 What is the most common form of conjoined twins? | back 334 thoracopagus |
front 335 What is thoracopagus | back 335 joined at the thorax |
front 336 What percent of conjoined twins are born alive? | back 336 60% |
front 337 How many conjoined twins are fused on the ventral wall? | back 337 56% |
front 338 polydramnios is commonly present in what type of twin? | back 338 conjoined |
front 339 How many monozygotic twins are classified DCDA? | back 339 Dichorionic Diamniotic
|
front 340 How many fetal deaths occur due to DCDA? | back 340 10% |
front 341 How many monozygotic twins are classified MCDA? | back 341 Monochorionic Diamniotic
|
front 342 How many fetal deaths occur due to MCDA? | back 342 10% |
front 343 ow many monozygotic twins are classified MCMA? | back 343 Monochorionic Monoamniotic
|
front 344 How many fetal deaths occur due to MCMA? | back 344 25% |
front 345 How many twin pregnancy ends in a singleton birth? | back 345 70% |
front 346 What is vanishing twin? | back 346 a small cystic collection appearing adjacent to gestational sac, that
|
front 347 What is papyraceous? | back 347 fetus passes around 14 weeks
|
front 348 When one twin dies the other may live depending on? | back 348 chorionicity
|
front 349 What are problems of MCMA twins? | back 349 twin to twin transfusion
|
front 350 What are problems of MCDA twins? | back 350 twin to twin transfusion
|
front 351 What form of twins are in danger of twin to twin transfusion? | back 351 Monozygotic twins
|
front 352 What is twin to twin transfusion? | back 352 A/V shunt within the placenta
|
front 353 What happens to the donor with twin to twin transfusion? | back 353 anemic
|
front 354 What happens to the recipient with twin to twin transfusion? | back 354 LGA = large for gestational age
|
front 355 What is the term used for abnormal growth when one twin is much
| back 355 Discordant growth |
front 356 What is the term used for normal growth of twins? | back 356 concordant |
front 357 When is evaluation of the number of chorions and amnions done? | back 357 best done in 1st trimeter |
front 358 What are the signs of DCDA twins? | back 358 lambda sign
|
front 359 What are the signs of MCDA twins? | back 359 T sign
|
front 360 What is for sure when twins are of different genders? | back 360 dizygotic
|
front 361 If cords insert into placenta at different locations? | back 361 DCDA |
front 362 What is discordant growth? | back 362 differences of estimated weight between monochorionic twins is
|
front 363 What is concordant growth? | back 363 differences of estimated weight between monochorionic twins is less
|
front 364 During singleton pregnancy when is growth a cause for concern? | back 364 10th & 90th percentile
|
front 365 What is dolichocephaly? | back 365 skiny head
|
front 366 Why is dolichocephaly a pitfall? | back 366 underestimates BPD |
front 367 What is Fetal Hydrops? | back 367 AKA Hydrops fatalis. Two sites of fluid accumulation or one site of
|
front 368 What is another name for fetal hydrops? | back 368 Hydrops fatalis |
front 369 What are the types of fetal hydrops? | back 369 Immune Hydrops: results of Rh sensitivity
|
front 370 What is Immune hydrops? | back 370 results of Rh sensitivity |
front 371 What is Nonimmune Hydrops? | back 371 any hydrops in the absence of Rh sensitivity |
front 372 What is the sonographic appearance of Fetal Hydrops? | back 372 Fluid collection
|
front 373 What is Rh sensitivity? | back 373 Rh- mother & Rh+ father = Rh+ baby
|
front 374 How is Rh sensitivity treated? | back 374 Rhogam shots at
|
front 375 What is Rh+ immunoglobin? | back 375 Rogram
|
front 376 How is Immune Hydrops diagnosed? | back 376 ABO -Rh blood typing
|
front 377 What is unlikely if antibody titer of < 1:16 | back 377 interuterine fetal death |
front 378 What is what i if antibody titer of < 1:16 | back 378 interuterine fetal death |
front 379 What is the sonographic appearance of Immune Hydrops? | back 379 Fluid collection
|
front 380 How is Immune Hydrops diagnosed? | back 380 Amniocentesis - Old method
|
front 381 What can be checked with Cordocentesis? | back 381 fetal hemoglobin
|
front 382 What does low hemoglobin mean during a Cordocentesis? | back 382 baby is anemic
|
front 383 What is Low Zone immune Hydrops? | back 383 mildly affected
|
front 384 What is Mid Zone immune Hydrops? | back 384 Fetus is affected but not an emergency
|
front 385 What is High Zone immune Hydrops? | back 385 Emergency
|
front 386 What is Alloimmune Thrombocytopenia? | back 386 mother develops an immune response to fetal platelets
|
front 387 What is the treatment for Alloimmune Thrombocytopenia? | back 387 via cordocentisis |
front 388 What is NIH? | back 388 Nonimmune Hydrops
|
front 389 What are the causes of NIH? | back 389 Cardiovascular
|
front 390 What is Parvo? | back 390 dangerous to pregnant women before 20 weeks |
front 391 What does parvo cause? | back 391 Hydrops |
front 392 What is 5th disease? | back 392 Parvo |
front 393 What is slap cheek syndrome? | back 393 parvo |
front 394 What is done to determine the cause of non immune hydrops? | back 394 ultrasound |
front 395 What is the sonographic appearance of NIH? | back 395 edema
|
front 396 What is Insulin Diabetes Mellitis? | back 396 Type I
|
front 397 Why is Type 1 Diabetes dangerous during pregnancy? | back 397 Elevated glucose fires up fetal growth (FAT babies)
|
front 398 What is macrosomic? | back 398 Big ass baby
|
front 399 What is done for diabetic pregnancy? | back 399 frequent U/S |
front 400 What are the sonographic findings more common to diabetic mothers? | back 400 fetal macrosomia
|
front 401 What should be considered if polyhydramnios with a baby that is macrosomia? | back 401 Gestational Diabetes |
front 402 Insulin diabetic who have diabetes under control reduce the risk of
| back 402 no data |
front 403 What are the sonographic appearance of Hypertension? | back 403 small placenta
|
front 404 What is Eclampsia? | back 404 Pregnancy induced hypertension prior to 20 weeks |
front 405 What are possible problems of patients with pre-eclampsia? | back 405 maternal proteinuria
|
front 406 What are possible problems of patients with sever pre-eclampsia? | back 406 baby must be delivered immediately |
front 407 What are possible problems of patients with Eclampsia? | back 407 seizures and/or coma |
front 408 What are some causes of Maternal Vomiting? | back 408 Hyperenemis graviarum
|
front 409 What can excessive vomiting cause? | back 409 dehydration
|
front 410 How many preg patients will have bacteria? | back 410 4-6%
|
front 411 Why is mild hydronephrosis normal in pregnancy? | back 411 progesterone dilates the ureteric smooth muscle
|
front 412 What is a Dysgerminoma? | back 412 germ cell tumor female counterpart of seminoma. Corpus Luteum of
|
front 413 What is the Sonographic Appearance of Dysgerminoma? | back 413 Cyst on ovary
|
front 414 Why are fibroids problematic with pregnancy? | back 414 grow in response to estrogen. Can rapidly grow and undergo necrosis.
|
front 415 How to tell the difference between fibroids and uternine contractions? | back 415 contractions resolve within 30 minutes
|
front 416 What is fetal demise? | back 416 absence of fetal tone after 20 weeks |
front 417 1/2 of fetal deaths can have determining factors | back 417 infection |
front 418 How many miscarriages happen in the 1st trimester? | back 418 15/20 : 100 |
front 419 What are signs of viability? | back 419 TV heartbeat at 5.5 weeks |
front 420 Lack of fetal Doppler after 12 weeks or fetal movement after 16 weeks prompts? | back 420 Ultrasound |
front 421 What are the signs of long term fetal death? | back 421 overlapping cranium (spaulding sign)
|
front 422 What is spaulding sign? | back 422 overlapping cranium |
front 423 What is robert's sign in abdomen? | back 423 gas shadowing within fetus |
front 424 What is Premature labor? | back 424 Onset of labor prior to 37 weeks gestation |
front 425 What are possible causes of premature labor? | back 425 PROM
|
front 426 What are increased risks to the fetus With premature labor? | back 426 RDS
|
front 427 At what a week he is a fetus viable In Born early? | back 427 22 weeks |
front 428 What is EFW? | back 428 Estimated fetal weight |
front 429 What is the EFW of a viable fetus? | back 429 Greater than 500 g
|
front 430 What is PROM management? | back 430 Watching for signs of fetal distress
|
front 431 What is external cephalic version? | back 431 Looking the baby |
front 432 How many babies are breach at term? | back 432 4% |
front 433 Why would an external cephalic version be performed? | back 433 Tried to reduce the number of Breech Babies
|
front 434 What are breach babies increased risk for? | back 434 Cord prolapse
|
front 435 Wind is an external cephalic version most successful? | back 435 between 37 - 38 weeks |
front 436 What should happen if call made of omphalocele in 1st trimester? | back 436 Re scan at 14 to 15 weeks to rule out rotation of mid gut |
front 437 What is gastroschisis? | back 437 A wall defects tends to occur in boys on the right side |
front 438 What is the sonographic appearance of gastroschisis? | back 438 Free floating loops of bowel in the amniotic fluid |
front 439 What is Omphalocele? | back 439 the intestines, liver, and occasionally other organs remain outside
|
front 440 What is the sonographic appearance of Omphalocele? | back 440 intestines appear outside abdomen in pouch |
front 441 At what week is head identified?
| back 441 7 weeks
|
front 442 When is cranial anatomy best viewed? | back 442 12 - 14 weeks |
front 443 What is the difference between omphalocele and gastroschisis? | back 443 omphalocele has a surrounding membrane
|
front 444 What is Anacephaly? | back 444 Failure of closure of neurotube at cephalic end, brain is in direct
|
front 445 What is the sonographic appearance of Anecephaly? | back 445 Frog apearance
|
front 446 What is Hydrancephaly? | back 446 brain necrosis results from obstruction of ICA – lack of nutrients |
front 447 What is the sonographic appearance of Hydrancephaly? | back 447 Cystic mass in place of brain parenchyma |
front 448 What is Turner syndrome? | back 448 congenital endocrine disorder
|
front 449 What is Cystic Hygroma? | back 449 Sign of Turner syndrome. Bad insertion of lymphatics into IJV.
|
front 450 What is the sonographic appearance of Cystic Hygroma? | back 450 Cystic mass in cervical region
|
front 451 What is a umbilical cord cyst? | back 451 benign
|
front 452 What is a placental hematoma? | back 452 collection of blood from detached placenta
|
front 453 What is a Corpus Luteum Cyst? | back 453 secretes progesterone to support pregnancy until placenta takes over.
|
front 454 What is the most common location of an ectopic pregnancy? | back 454 ampulla - 80%
|
front 455 How many maternal deaths are ectopic pregnancy? | back 455 10% |
front 456 What is the most dangerous area for ectopic? | back 456 interstitial AKA Cornial
|
front 457 What are the associated risks factors of an ectopic? | back 457 PID
|
front 458 What is the presentation of an ectopic? | back 458 Pain 97%
|
front 459 What do the beta hCG levels need to be to see an IUP? | back 459 500 IU/L trans vag
|
front 460 What will the Beta hCG levels be with ectopic? | back 460 lower than IUP |
front 461 BhCG levels double every ____________? | back 461 2 days 1st 6 weeks
|
front 462 What is a ring of fire? | back 462 Doppler
|
front 463 What is a heterotopic pregnancy? | back 463 simutaneous intrauterine and ectrauterine pregnancy
|
front 464 What is the cornual pregnancy ? | back 464 Ectopic pregnancy at cornual
|
front 465 How are ovarian ectopic pregnancies identify? | back 465 But complex mass on the ovary
|
front 466 What percent of pregnancies are abnormal? | back 466 4% |
front 467 What day should a live embryo be seen? | back 467 46
|
front 468 What is a blighted ovum? | back 468 a fertilized ovum that does not result in a embryo.
|
front 469 What are the signs of a blighted ovum? | back 469 Large gestation all sac without inter gestation all anatomy
|
front 470 What should the fetal heart rate be in first trimester? | back 470 90 to 170 bpm
|
front 471 Oligiohydramnios in 1st trimester | back 471 Poor prognosis
|
front 472 What is the sonographic appearance of a complete miscarriage? | back 472 Empty uterus
|
front 473 What is the sonographic appearance of a incomplete miscarriage? | back 473 gestational sac may be normal with embryo w/ no fetal heart rate
|
front 474 RPOC? | back 474 retained products of conseption |
front 475 What is a threatened abortion? | back 475 vaginal bleeding with a closed cervical OS in a preganancy of less
|
front 476 What are the three forms of tropoblastic disease? | back 476 hydatiform mole - growth that forms inside the womb (uterus) at the
|
front 477 What is the sonographic appearance of Gestational tropoblastic disease? | back 477 snowstorm late 1st
|
front 478 What are the two types of IUGR? | back 478 symmetrical
|
front 479 What are the risk factors for IUGR? | back 479 previous
|
front 480 What are the problems associated with IUGR? | back 480 increased risk of antepartum death
|
front 481 What usually causes symmetric IUGR? | back 481 1st trimester insult
|
front 482 What type of IUGR is most common? | back 482 asymmetric
|
front 483 What is suggestive of Head sparring IUGR? | back 483 BPD & HC normal
|
front 484 What is suggestive of femur sparring IUGR? | back 484 FL 90th percentile
|
front 485 What is the best indicator of IUGR? | back 485 AC
|
front 486 What is the best indicator for predicting a symmetrical IUGR? | back 486 HC/AC ratio
|
front 487 What is indicative of oligohydramnios?
| back 487 oligo< 5cm
|
front 488 What are the placental markers that indicate IUGR? | back 488 decreased placental thickness < 1.5 cm
|
front 489 What is the chance of fetal loss with CVS? | back 489 1% - 3%
|
front 490 What are the advantages of CVS? | back 490 early (10-12 weeks)
|
front 491 What are the benefits of amniocentesis?
| back 491 disgnose spina bifida
|
front 492 Why would amnio be performed? | back 492 advanced maternal age
|
front 493 What are physical features suggesting chromosomal abnormalities? | back 493 clenched hands
|
front 494 What is PUBS? | back 494 Percutaneous umbilical cord sampling
|
front 495 What is FISH? | back 495 experimental
|
front 496 Where is AFP found? | back 496 fetal spine
|
front 497 What are the causes of elevated AFP? | back 497 ectopia corditis
|
front 498 What are the causes of decreased AFP? | back 498 Trisomy 13, 18, 21
|
front 499 When do fetal AFP levels peak? | back 499 15 - 18 weeks. |
front 500 Trisomy 18 | back 500 Edwards not good usually fatal |
front 501 Trisomy 21 | back 501 downs |
front 502 Trisomy 13 | back 502 Patau's syndrom |