What are the primary reasons for Venous vascular leg exam?
- Assess for DVT (Deep Vein Thrombosis)
- Evaluate the Saphenous veins for potential bypass conduit
- Evaluate for Venous Reflux
How do the deep veins course?
adjacent to major arteries and have the same names as the arteries (exception- IVC)
How much blood do the deep veins in the legs carry?
85% of blood volume
Name the deep veins in the pelvis?
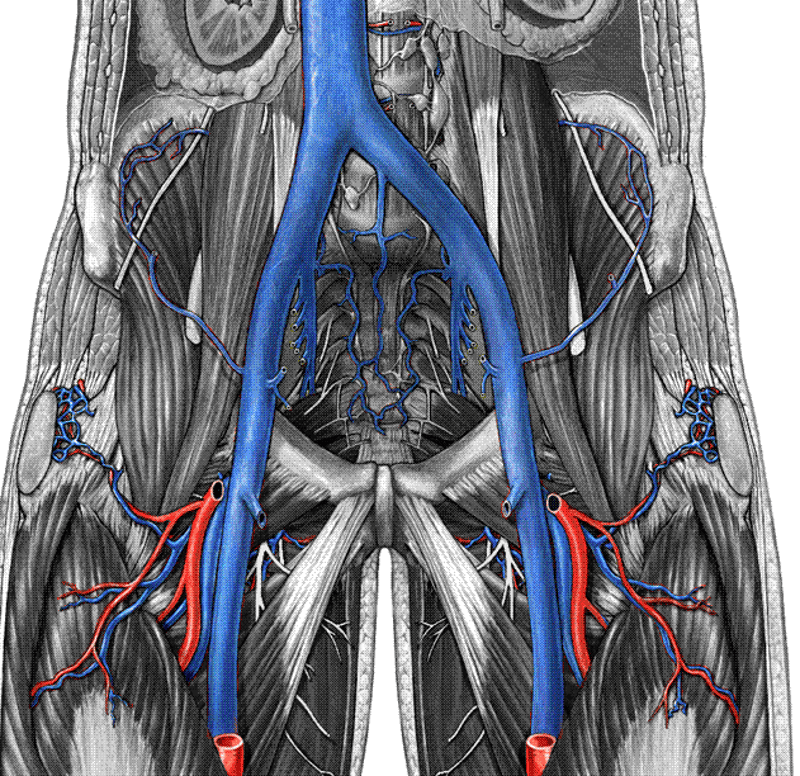
Inferior Vena Cava (IVC)
Common Iliac Vein (CIV)
Internal Iliac Vein (IIV)
External Iliac Vein (EIV)
What is another name for the internal iliac vein?
Hypogastric vein
Name the deep veins in the thigh.
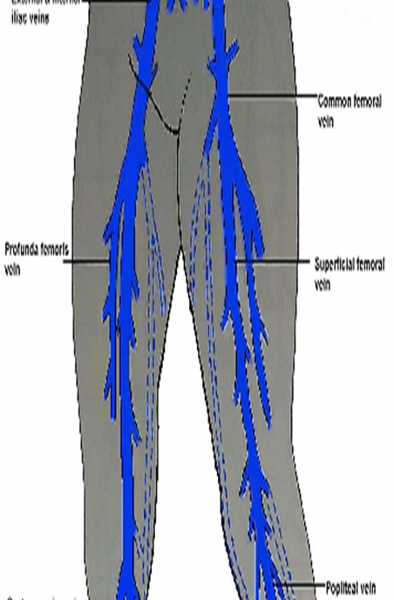
Common Femoral Vein (CFV)
Profunda Femoris Vein (PFV)
Femoral Vein (FV)
When does the external illiac become the common femoral
after it crosses the inguinal ligament
What is another name for the Profunda Femoris Vein?
Deep Femoral vein (DFV)
Where does the greater saphenous start and end?
starts at ankle
joins the common femoral at the groin
What was the Femoral vein previously known as?
Superficial Femoral Vein
Where is the Femoral vein?
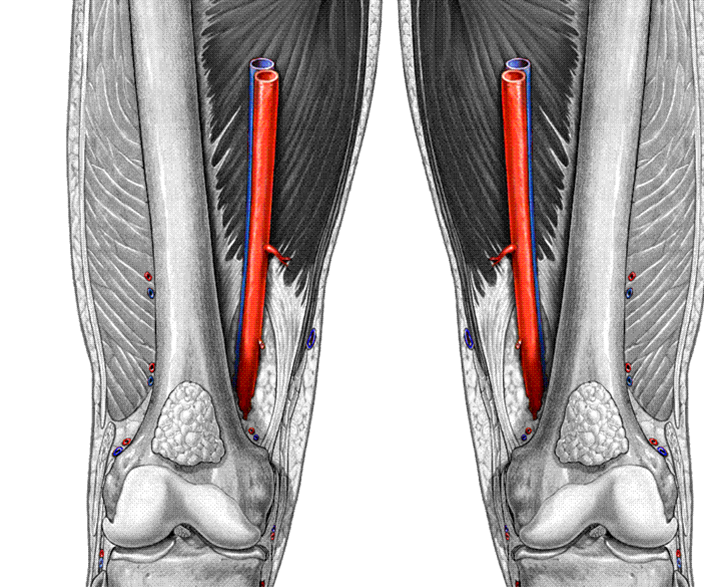
What is the name of the vein that runs behind the knee?
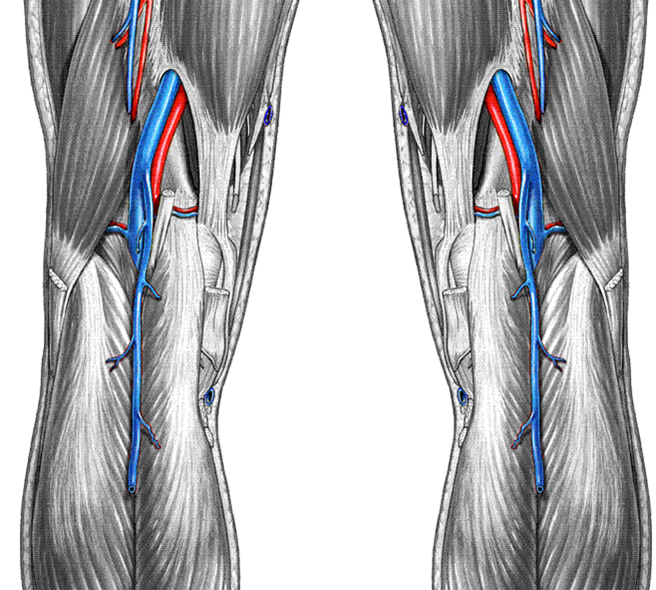
Popliteal vein (Pop V)
When does the femoral vein become the popliteal vein?
when the femoral crosses the adductor canal
Where is the Small Saphenous vein (SSV) ?
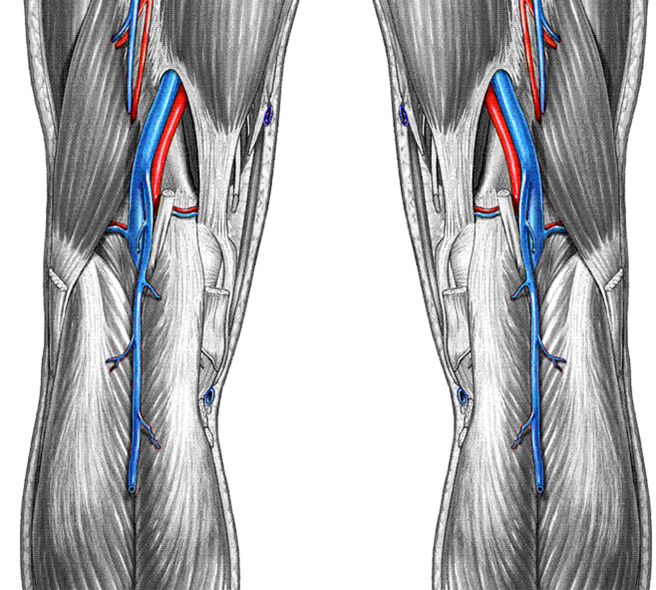
Small Saphenous vein (SSV)
What was the Small Saphenous vein (SSV) previously known as?
Lesser Saphenous Vein (LSV)
Name the veins in the calf.
Popliteal vein (Pop V)
Gastrocnemius Veins
Anterior Tibial Veins (ATVs)
Posterior Tibial Veins (PTVs)
Peroneal Veins (Per. V)
All veins below the knee there are _____ veins to every one artery.
two
2 veins to every 1 artery
The Anterior Tibial Veins (ATVs) courses ________.
lateral
The Posterior Tibial Veins (PTVs) courses ________.
medial
The Peroneal Veins (Per. V) courses ________.
deep medial
Explain the course of the large saphenous vein.
GSV courses along the medial aspect of the leg from the ankle to the groin where it enters the deep system at the CFV (Saphenofemoral junction)
What is the difference between the deep and superficial veins?
superficial lie above the muscle
deep veins lie within muscle
Explain the course of the small saphenous vein.
SSV courses up the posterior aspect of the lower leg from the Achilles tendon region to the Popliteal vein confluence in the Popliteal Fossa
How many cases of DVT a year?
1 - 10 million
How many cases of Pulmonary Embolus a year?
600,000 cases
How many death a year from Pulmonary Embolus?
200,000 deaths
What are the reasons for a BLE?
Stasis - bedrest - lack of movement
hypercoagulability
vein wall injury - stab, gunshot, IV drugs
thrombofilia
hormone replacement
What are the Risk factors for DVT?
post - operative state
previous DVT
cancer
thrombophilia
- ATIII, protein C, protein S, deficiency, APC resistance
- Antiphospholipid antibody or lupus anticoagulant
trauma
pregnancy
high dose estrogen RX
Immobility (long car or plane ride)
Bed-rest > 4 days
Lower limb paralysis
What are the symptoms of a DVT?
- persistent leg pain with acute onset
- persistent leg swelling
- calf pain/tenderness
- if patients have above symptoms, 50% chance of DVT
Leg swelling will be ________ if a DVT is present.
Leg swelling will be unilateral if a DVT is present.
Why are DVTs have low sensitivity?
Many DVTs are clinically asymptomatic
Why are DVTs have low specificity?
Non-thrombotic disorders can cause the same clinical symptoms as DVT
What symptom has high positive predictive value for DVT?
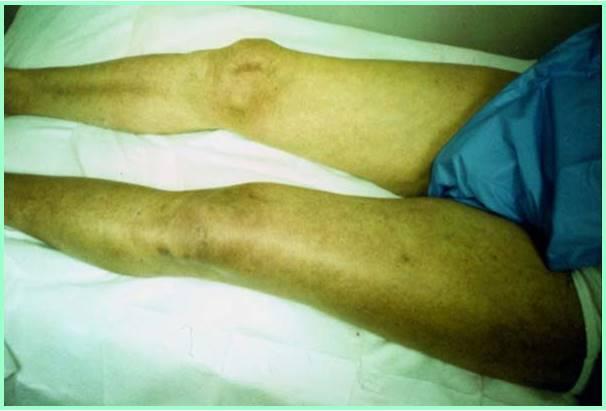
Phlegmasia cerulea dolens
What is Phlegmasia cerulea dolens?
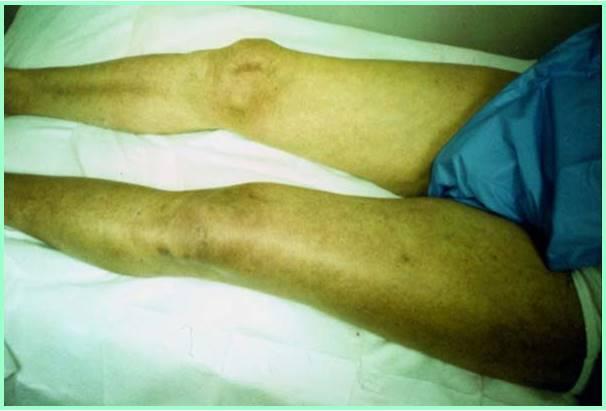
massive thigh and calf swelling
limb cyanosis
iIlio - femoral outflow obstruction
painful blue anemia
superficial thrombophlebitis
erythema / inflammation (swelling)
local tenderness
palpable cord or mass
usually more painful that DVT
What is the main problem with superficial thromboplebitis?
hurts like hell but probably will not throw an embolism unless proximal to the deep wein system.
What is the treatment with superficial thromboplebitis?
warm compress and aspirin
What should be looked for on a physical exam?
swelling
limb discoloration - venous insufficiency
stasis dermatitis, ulceration
varicose veins
palpable “cords” (STP-superficial thrombophlebitis)
What are the four parts o?f a Venous Duplex Techniques?
1.compressibility / coaptation of vein
2.visualization of thrombus
3.spectral Doppler - pos augmentation
4.color Doppler - wall to wall filling
What are the techniques used for a Venous Duplex Techniques?
Torso elevated 10-20 degrees - tilted bed
Leg rotated externally
Start at groin crease in transverse plane
What is coaptation?
close
phasic & spontaneous flow
...
site 1

site 2
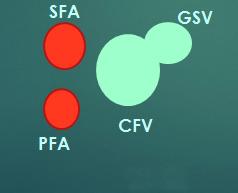
site 3
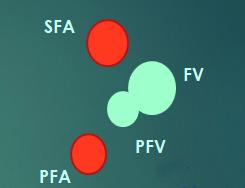
site 4

site 5+
...
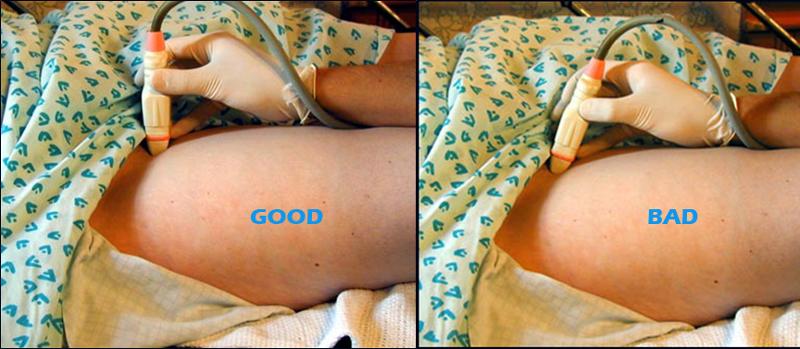
Why would you scan through the adductor canal?
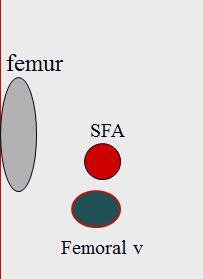
On many patients, this approach provides an excellent acoustic window to the FV and SFA in the adductor canal. However, you must compress from the posterior thigh
What is the Valsalva Maneuver?
During inspiration, diaphragm moves downward and increases intra-abdominal pressure.
IVC is compressed and venous outflow is temporarily reduced or stopped.
Flow resumes during exhalation
*bearing down like you are pooping stops slows blood flow
If there is no close and back filling during valsalva maneuver what does this mean?
reflux
Flow direction display
Traditionally, the Doppler waveform has been displayed below baseline
This is not necessary with duplex ultrasound systems.

Continuous venous flow in CFV?
proximal obstruction
Respiratory phasicity may not be present due to:
Shallow breathers, (patients with pulmonary embolus-PE).
Patients who are lying supine.
Patients who have their arms raised and hands behind their head.
Spinal cord injured patients due to reduced abdominal muscle tone.
Proximal DVT or extrinsic venous compression.
Where is cardiac activity most influential?
thoracic vessels.
Explain cardiac influence in the lower extremities
Cardiac influence is usually not apparent or is reduced in the lower extremities
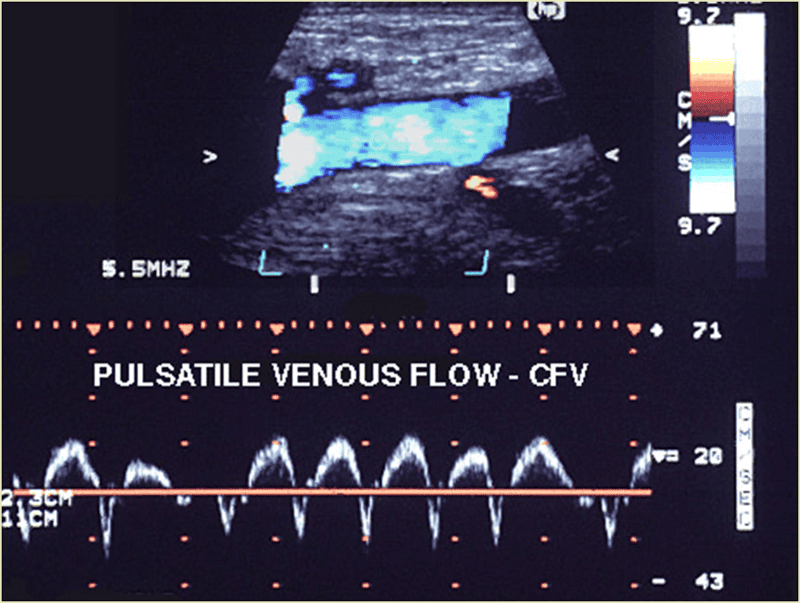
Pulsatile flow due to congestive heart failure
Where should you begin with Calf imaging?
at the ankle
Which vessel should be identified first in the calf?
PTV
What plain are the calf vessels imaged?
You may use color Doppler in transverse plane, but it’s not as good as in long view
What are some methods to improve calf vein visualization?
Leg dependent position
Maximum vein dilation
****Don’t expect spontaneous flow
What is the leg dependent position?
reverse trndenburg
When do we examine the anterior tibial veins?
Don’t bother !
Too tedious
Too small
They’re rarely involved unless there is extensive DVT in other vessels
Explain the importance of Gastroc vein thrombosis.
May be clinically important if thrombus extends to popliteal vein.
So, determine the extent of thrombus
What should you do if the patient has tenderness in her calf?
If the patient is symptomatic (tenderness), look for muscular vein thrombosis
Why must you augment most of the time in the calf?
Flow in calf veins is usually not spontaneous, you often must augment flow by squeezing the calf or ankle.
Explain the most important perspective of bilateral lower extremity exam
thrombus anywhere from the popliteal to the iliac veins is life
threatening.
****Calf vein DVT may cause PE but thrombus
is too small to be fatal.
What is the Criteria for Venous Thrombosis?
Absence of vein compressibility
Visualization of thrombus
Vein distention
Abnormal Doppler signals
Reduced / absent augmentation
Reduced / absent color filling
What is the sonographic appearance of acute DVT?
vein distended
somewhat hypo-echoic
no collaterals
maybe free floating
Tail!!!!!!!!!!
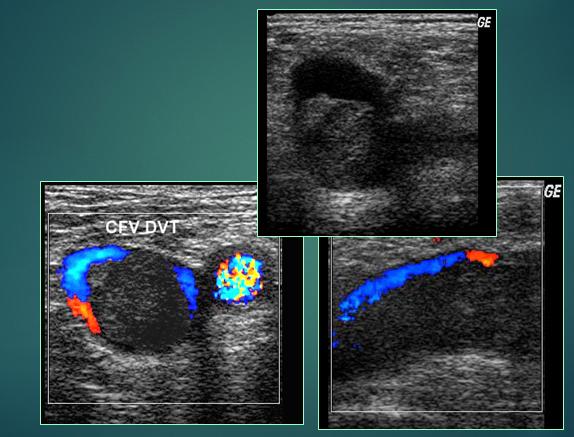
Acute DVT CFV
What must you do if PTV or peroneal vein thrombus is detected?
You must look carefully in the distal pop vein for propagation. It’s a difficult region to image.
What will eventually happen with chronic?
vein will eventually open back up & flow again
What are the symptoms of chronic DVT?
echogenic thrombus - more echogenic then acute
vein smaller than artery
presence of collaterals
recannalization
constricted vein
What us a Baker's cyst?
Synovial lining and fluid bulge into the popliteal space.
May dissect into calf muscles or along intermuscular septums
What is another name for a baker's cyst?
Synovial cyst
What should you do to confirm a baker's cyst?
Rule out calf hematoma by demonstrating communication with joint space
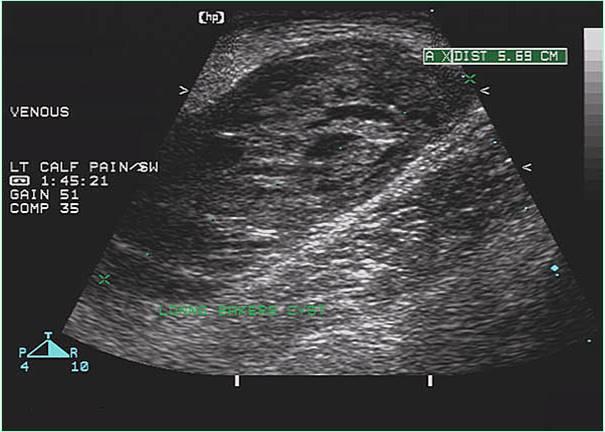
...
How do you tell the difference between a Calf hematoma and a baker's cyst?
absence of joint space communication helps differentiate from Baker’s cyst
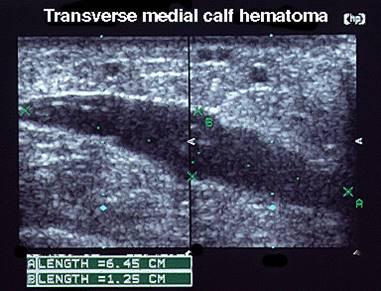
Calf hematoma
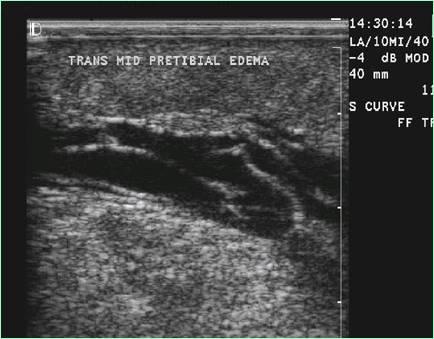
Lymphedema
What is the sonographic appearance of a Lymphedema?
“Ant farm” appearance
What is Lymphedema?
Lymphedema refers to swelling that generally occurs in one of your arms or legs. Sometimes both arms or both legs swell.
Lymphedema is most commonly caused by the removal of or damage to your lymph nodes as a part of cancer treatment. It results from a blockage in your lymphatic system
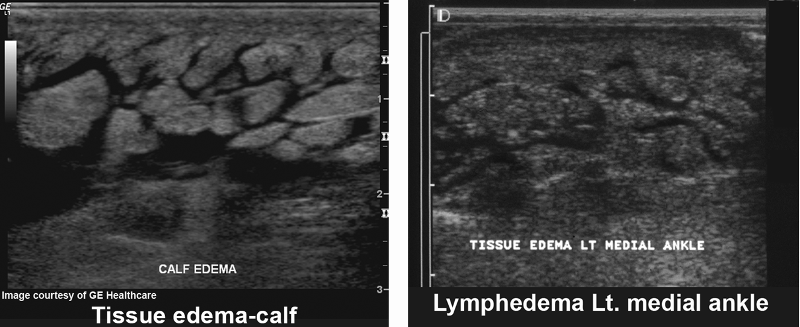
Lymphedema
Where are Lymph nodes commonly seen?
Commonly seen in the groin region.
When are lymph nodes commonly seen?
Kidney-shaped and can be swollen in the presence of systemic infection, malignancy,
What should be done when lymph nodes are seen?
Should be measured in three dimensions and reported.
What is May Thurner Syndrome?
May-Thurner syndrome (MTS) is caused when the left iliac vein is compressed by the right iliac artery.
Why is May Thurner syndrome dangerous?
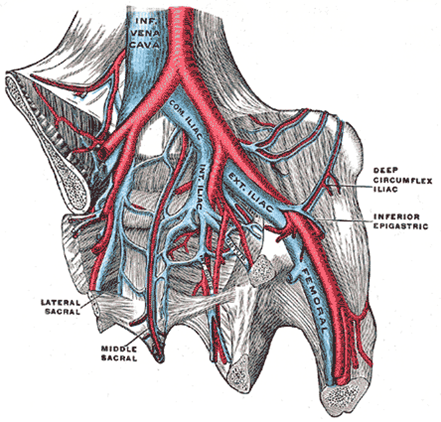
increases the risk of deep vein thrombosis (DVT) in the left extremity
VENOUS
acute onset SX
limb swelling
persistent pain calf/thigh
local tenderness
palpable “cord”
chest pain/SOB
ARTERIAL
progressive SX
intermittent pain when walking
foot/limb coolness
limb pallor
gangrene, tissue necrosis
Venous Insufficiency/
Venous Incompetence/ Venous Reflux
Primary
Congenital absence or defect of valves
Secondary
Post- phlebitic: valves damaged by venous thrombosis, and/or chronic outflow obstruction
How many valves are there in the IVC?
0
How many valves are there in the CIV?
0
How many valves are there in the EIV?
0
How many valves are there in the FV?
4
How many valves are there in the Pop?
2
How many valves are there in the PTV?
10
How many valves are there in the ATV?
10
How many valves are there in the ATV?
10
What are the 3 pump systems in the lower extremities?
Foot pump
Thigh pump
Calf veno-motor pump
What is the foot pump responsible for?
primes the calf pump
Thigh pump
Calf veno-motor pump
What is the thigh pump responsible for?
ejects thigh blood volume
What is the Calf veno-motor pump responsible for?
major ejection
Facilitates venous return to heart
Reduces the effect of hydrostatic pressure
Reduces venous pooling
Is dependent on competent valves and muscle contraction
What are the veins in the calves?
PTV’s
Peroneals
ATV’s
Gastrocs
Soleal sinuses
Greater & Small Saphenous
Perferators
How does the Veno-motor Pump work?
Muscle contraction squeezes blood upward, valves prevent return
What is the efficiency of the calf veno-motor pump is dependent upon?
1)The ability of the calf skeletal muscles to contract.
2)The competency of the venous valves.
3)The patency of outflow veins.
What can cause perforators?
Increased deep vein intraluminal pressure may cause perforators
What is a perforator?
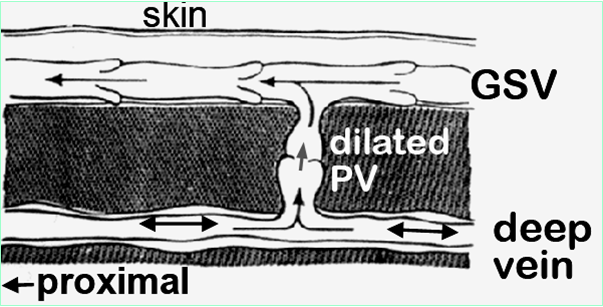
shunt venous blood from Superficial to deep system) to dilate and become incompetent.
What are the Venous insufficiency symptoms?
Recurrent swelling (walking all day)
Varicose veins-Spider veins
Venous claudication - tired achy legs at end of day
Stasis dermatitis - pigment stain from leak
Ulceration
What is Stasis dermatitis ?
pigment stain from leak
What is Venous claudication?
tired achy legs at end of day
Explain the Flow patterns in upper extremities- central veins
Cardiac pulsatility is usually apparent and pronounced.
Respiratory variation occurs, but flow during inspiration INCREASES, due to changes in thoracic pressure.
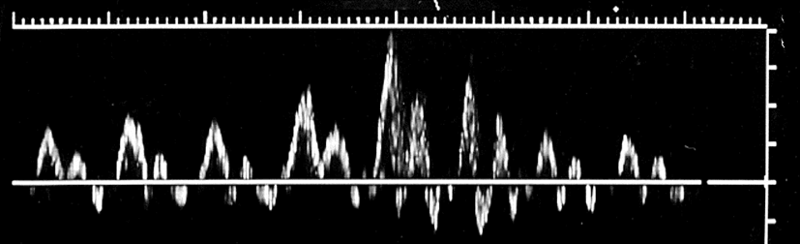
subclavian
What is the difference between a midline and a Picc catheter?
midline ends in the subclavian before the cephalic
picc ends just outside the heart in the SVC
What are the Indications for UE venous duplex?
Pain and swelling in arm or neck
PE
Dilated SF veins of the arm or shoulder
Palpable cord in arm (SVT)
Infusion difficulty with indwelling catheters
Pre-op assessment for hemodialysis access placement
What are the Deep Veins of the upper extremity?
SVC
Innominate
Subclavian
Axillary
Brachial
Radial
Ulnar
What are the superficial Veins of the upper extremity?
Basilic
Cephalic
Median cubital
What is the Patient position for evaluation of proximal veins?
Supine for maximum venous filling
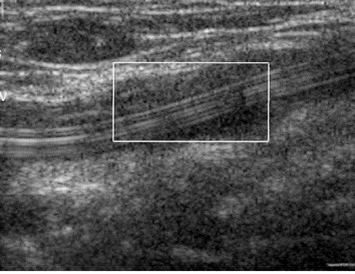
...
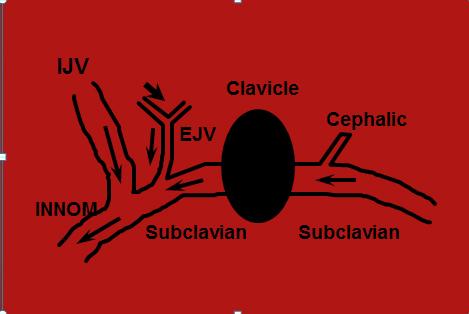
...
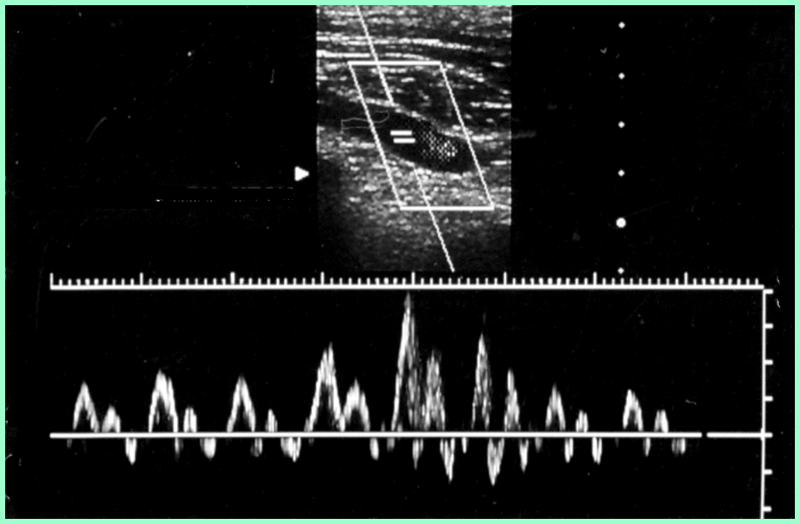
Normal upper venous flow
What are the normal characteristics of upper venous flow?
respiratory phasicity
cardiac influence
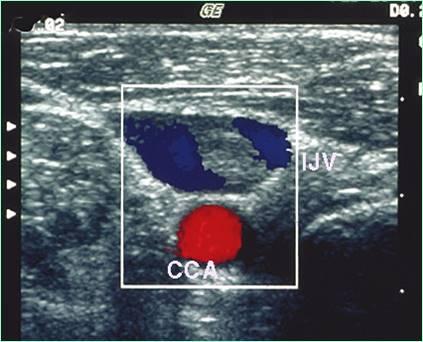
...
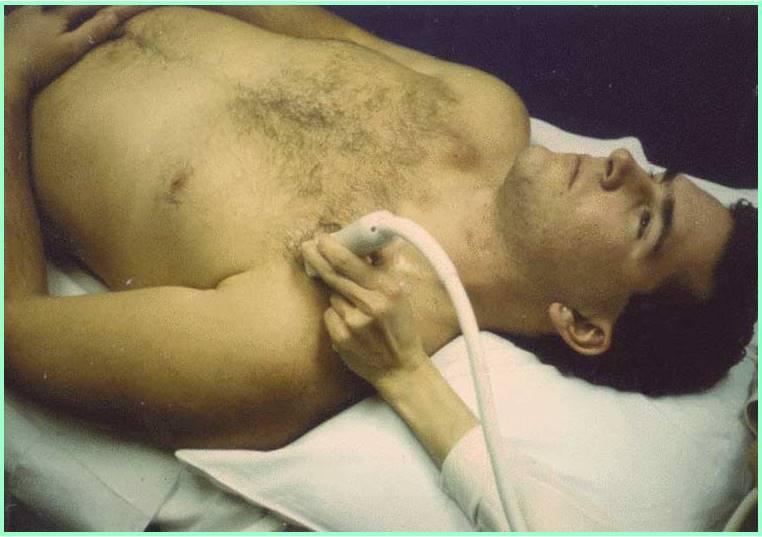
Infraclavicular Subclavian Vein
What will alleviate transient axillary vein compression?
Abduct arm to alleviate transient axillary vein compression
Arm veins
Use compression- release method
Pulsatile- phasic flow may be absent
Very superficial veins need standoff
Assess flow direction in all proximal veins
Bilateral comparison of proximal veins for waveform symmetry
Waveform assessment priority for prox veins
...
What is the rule about when an artery bifurcates?
before venous anastomosis
What is important when looking for reflux?
augmentation
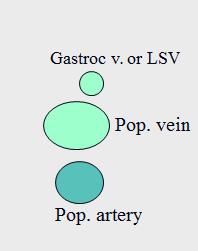
If the vein is above the artery, where are you?
popliteal
What does continuous flow in the common femoral vein indicate?
proximal thrombosis
WHat is the easiest vein the identify below the knee?
posterior tibial
How do you find the peroneal veins?
posterior and deep to the PTV
If calf is swollen due to venous instruction what is involved?
popliteal
Where does DVT usually originate in the calf?
Soleal vein
Where is the soleus located?
small sinus that drains into PTV & Perotoneal
What does the gastrocnemius vein drain?
head of calf
drains into popliteal
What does poor augmentation indicate?
obstruction between transducer & augmentation
recanalization GSV with residual fibrous band is also called?
scaring
What is sub acute?
between acute and chronic
What is the treatment for a free floating thrombus?
NO AUGMENTATION!!!!!!!!!!!!
heprin/lebenen shot immediately
What will lymphedema cause with augmentation?
difficult augmenatation
What is progressive sx?
cholesterol problems
smoking
BP issues
What causes foot/limb coolness
limb pallor
gangrene
tissue necrosis
lack of arterial flow
The venous system is a ____ pressure system?
low
The rule for valves is
more distal more valves
What will venous obstruction in illiac, femoral or popliteal vein cause
sweeling & venous swelling
Why is dilated perforators a problem?
when veins stretch valves cannot "touch" and fully shut anymore
What is Paget–von Schrötter disease?
is a form of upper extremity deep vein thrombosis(DVT), in the axillary or subclavian veins.
What else is Paget–von Schrötter disease called?
"effort-induced thrombosis"
How many veins and arteries for the brachial, radial & ulnar?
2 veins
1 artery
Where does the basilic dump into?
axillary or brachial
What should be done when there is a thrombus in the basilic vein?
document how far it is from deep system
What is upper extremity exam not as accurate as the lower extremity exam?
confidence & volume