First Line of Defense

- non specific defense
- mechanical barrier
- such as: unbroken skin or mucous membrane
- blocks the entry of bacteria and other harmful substances into the tissues
- body secretions such as tears and saliva that contain enzymes that destroy potentially damaging material
Second Line of Defense
- includes the non specific processes of phagocytosis and inflammation
Phagocytosis
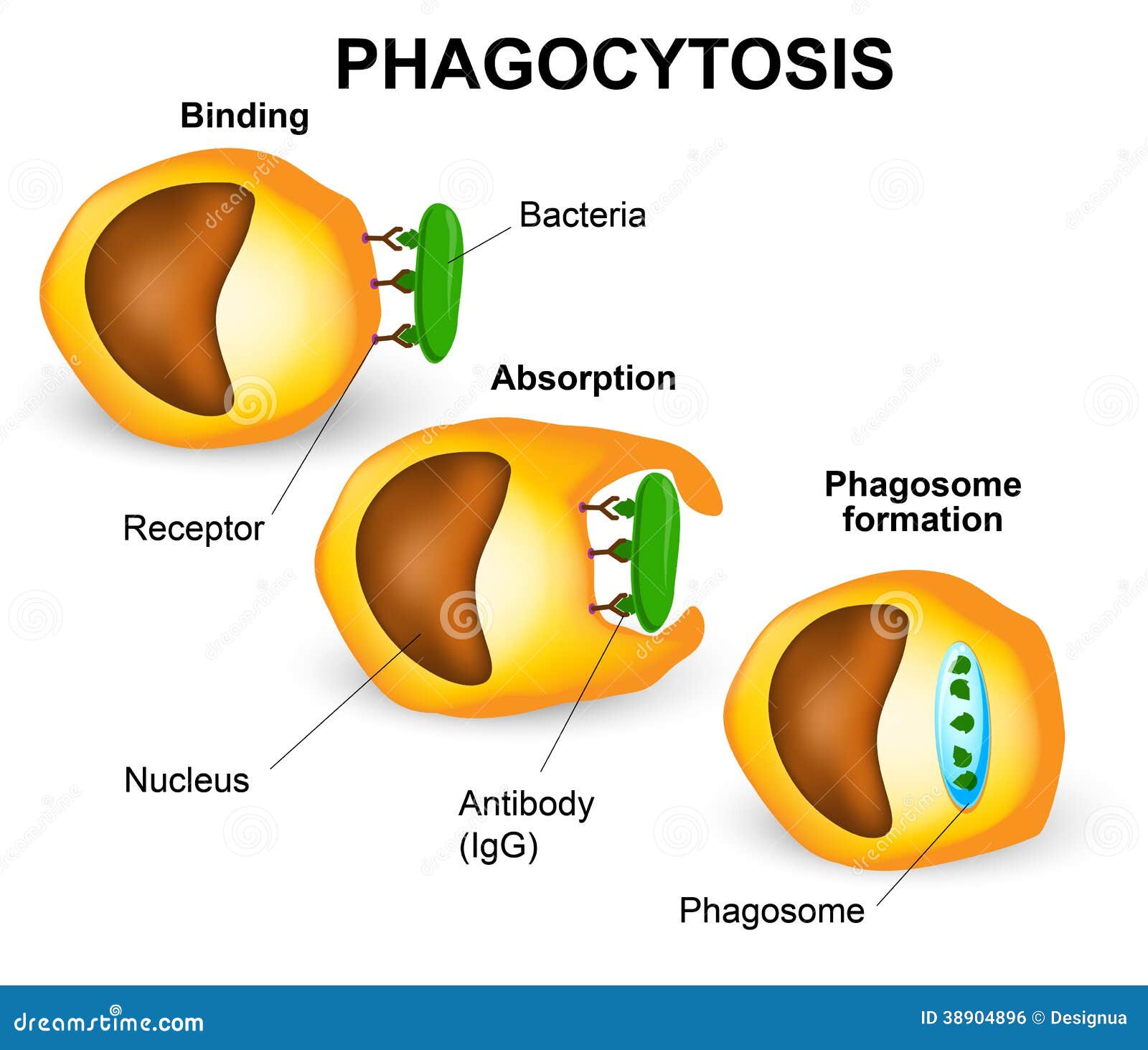
- process by which neutrophils and macrophages engulf and destroy bacteria, cell debris, or foreign matter
Neutrophils
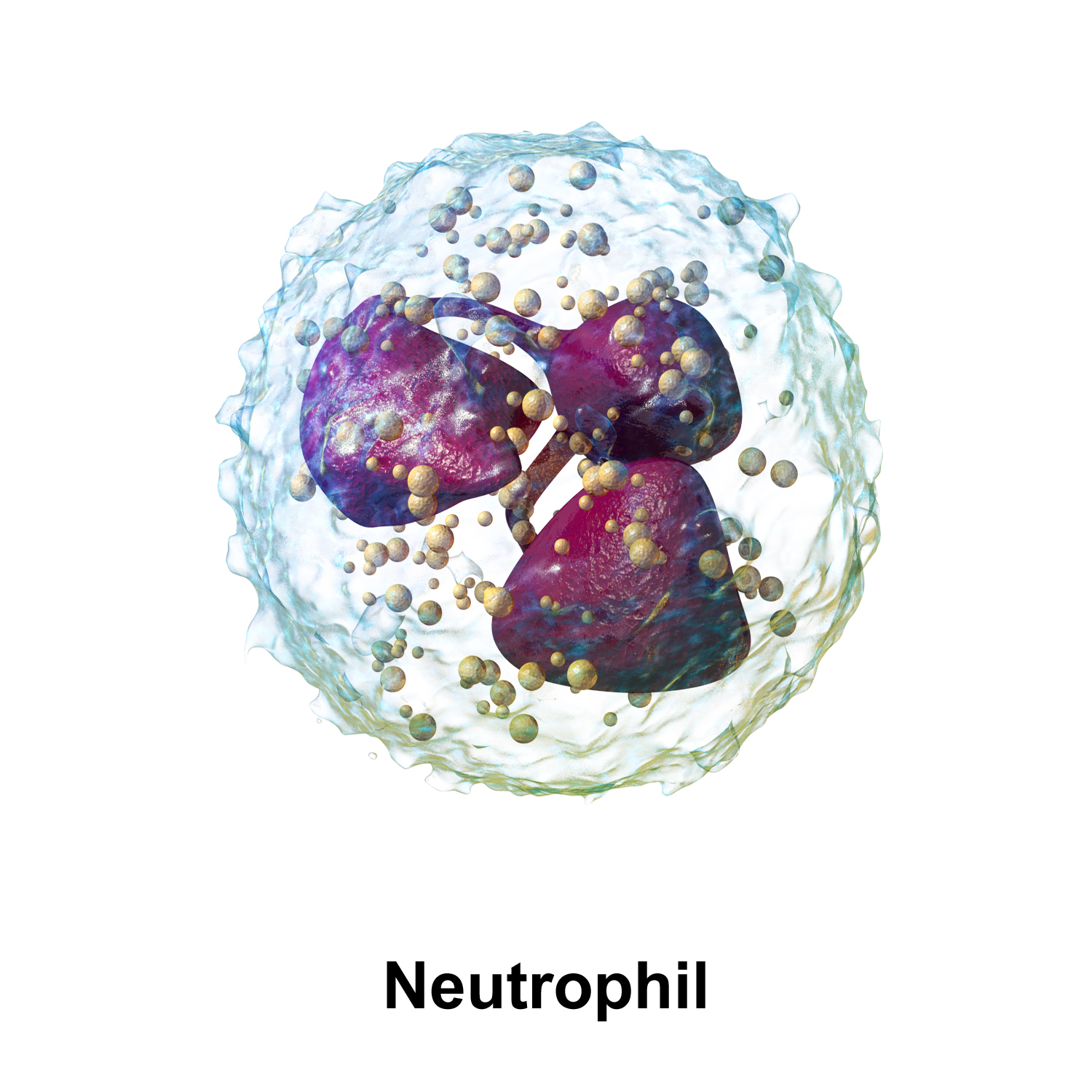
- a leukocyte
- phagocytosis of microorganisms
Inflammation
suffix: -itis
- a sequence of events intended to limit the effects of injury or a dangerous agent in the body
- is intended to localize and remove an injurious agent
- the general signs and symptoms serve as a warning of a problem which may be hidden within the body
- non specific response
- results in redness, swelling, warmth, and pain
Interferons
- nonspecific agents
- protect uninfected cells against viruses
Third Line of Defense

- specific defense
- provides protection by stimulating the production of specific antibodies and sensitized lymphocytes
Normal Capillary Exchange

- usually not all capillaries in a particular capillary bed are
open
- unless the cells' metabolic needs are not being met by the blood supply to the area
- or an accumulation of wastes occurs
Arterial End of Capillary
- movement of fluid, electrolytes, oxygen, and nutrients
- based on net hydrostatic pressure (pushes things out)
Venous End of Capillary
- hydrostatic pressure is decreased
- osmotic pressure
(pulls things in)- relatively high
- b/c plasma proteins remain within the vessels
Glucocorticoids
- acts as an anti-inflammatory by decreasing capillary permeability
Causes of Inflammation
- direct physical damage
- such as: cuts or sprains
- caustic chemicals
- such as: acids or drain cleaner
- ischemia or infarction
- local deficiency of blood
- allergic reactions
- extremes of heat and cold
- foreign bodies
- ex: splinter or glass
- infection
Steps of Inflammation
- An injury to capillaries and tissue cells will result in the
following reactions:
- Bradykinin is released from injured cells
- Bradykinin activates pain receptors
- Sensation of pain stimulates mast cells and basophils to release histamine
- Bradykinin and Histamine cause
capillary dilation
- results in an increase in blood flow and increased capillary permeability
- Break in skin allows bacteria to enter the tissue
- results in migration of neutrophils and monocytes to the site of injury
- Neutrophils phagocytize bacteria
- Macrophages (mature monocytes) leave the bloodstream and phagocytose microbes
Acute Inflammation
- When tissue injury occurs, the damaged mast cells and platelets release chemical mediators into the interstitial fluid and blood.
- examples of chemical mediators:
- histamine
- serotonin
- prostaglandins
- leukotrienes
- Chemical mediators affect blood vessels and nerves in the damaged area
-
Cytokines
- serve as communication in the tissue fluids sending messages to induce fever
Histamine
- released immediately from granules in mast cells and exert their effects at once
- immediate vasodilation and increase capillary permeability to form exudate
Leukotrienes
- synthesized from arachidonic acid in mast cells
- responsible for the later effects
- prolongs inflammation
- vasodilation
- increased capillary permeability
- chemotaxis
Hyperemia
- increased blood flow to a particular area
Increase in Capillary Permeability
- allows plasma proteins to move into interstitial space along with fluid.
- Increased fluid dilutes any toxic material, while globulins serve as antibodies, and fibrinogen forms fibrin mesh around the area to localize the injurious agent
Chemotaxis
- attract cells of the immune system
- first Neutrophils and later monocytes and macrophages
Vasodilation
- relaxation of smooth muscles causing an increase in the diameter of arterioles
Basophils
- release of histamine, leading to inflammation
Eosinophils
- numbers are increased in allergic responses
T Lymphocytes
- active in cell-mediated immune response
B Lymphocytes
- produce antibodies
Monocytes
- phagocytosis
Macrophages
- active in phagocytosis
- mature monocytes that have migrated into tissues from the blood
Diapedesis
- The movement or passage of blood cells, especially white blood cells, through intact capillary walls into surrounding body tissue.
Redness and Warmth
(inflammation symptom)
- caused by increased blood flow into the damaged area
Swelling or Edema
(inflammation symptom)
- caused by the shift of protein and fluid into the interstitial space
Pain
(inflammation symptom)
- results from increased pressure of fluids on the nerves; release of chemical mediators (ex: Bradykinin & prostaglandins)
Loss of Function
(inflammation symptom)
- may develop if cells lack nutrients
- edema may interfere with movement
Exudate
- a collection of interstitial fluid formed in an inflamed area
Serous/Watery Exudate
- watery
- consists primarily of:
- fluid
- some proteins
- and some white blood cells
- occurs with allergic reactions and burns
Fibrinous Exudate
- thick and sticky
- high cell and fibrin content
- increases the risk of scar tissue in the area
Purulent
- thick, yellow-green
- contains more leukocytes, cell debris, and microorganisms
- indicates bacterial infection
- aka "pus"
Abscess
- localized pocket of purulent exudate in a solid tissue
Other General Manifestations of Inflammation
- mild fever (pyrexia)
- if inflammation is extensive
- malaise
- feeling unwell
- fatigue
- headache
- anorexia
- loss of appetite
Pyrogens
- fever-producing substances
- circulate in the blood and cause the body temperature control system in the hypothalamus to be reset at a higher level
Leukocytosis
- increased white blood cells in the blood
- especially neutrophils
Differential Count
- the proportion of each type of WBC
- may be helpful in distinguishing viral from bacterial infection
Cell Enzymes in blood
- may be elevated in the blood in the presence of severe inflammation and necrosis
- helpful in locating the site of necrotic cells
Ulcers
- erosion of tissue
Infection & Inflammation
- infection may develop in an inflamed tissue b/c microorganisms can more easily penetrate when the skin is damaged and blood supply is impaired
- some microbes resist phagocytosis
- inflammatory exudate provides an excellent medium for microorganisms to reproduce and colonize the inflamed area
Chronic Inflammation
- may develop following an acute inflammation, when causative agent is not completely eradicated
Characteristics of Chronic Inflammation
- less swelling and exudate
- presence of more lymphocytes, macrophages, and fibroblasts than acute inflam
- more tissue destruction occurs
- more collagen is produced resulting in more fibrous scar tissue
Granuloma
- small mass of cells with a necrotic center covered by connective tissue
- may develop around foreign objects such as splinter
Acetylsalicylic Acid (ASA)
- an anti-inflammatory agent
- decrease prostaglandin synthesis, reducing the inflammatory response
- decrease pain and fever
- DO NOT GIVE TO CHILDREN WITH VIRAL INFECTIONS DUE TO RISK OF LEADING TO REYES SYNDROME
- aspirin
Acetaminophen
- decreases fever and pain
- does not diminish the inflammatory response
- TYLENOL or PARACETAMOL
Nonsteroidal Anti-Inflammatory Drugs (NSAIDs)
- has anti-inflammatory, analgesic, antipyretic activities
- act by reducing production of prostaglandins
- used to treat inflammation in musculoskeletal system
Anti-Inflammatory Effects of Glucocorticoids
- act as an anti-inflammatory by decreasing capillary permeability
- enhance effectiveness of epinephrine and norepinephrine
- reduced number of leukocytes and mast cells, decreasing the release of histamine and prostaglandins
- reduces immune response
RICE Therapy for Injuries
- Rest
-
Ice
- cold causes vasoconstriction, decreasing edema and pain
-
Compression
- reduces the accumulation of fluid
-
Elevation
- improve fluid flow away from damaged area
Resolution
- the process that occurs when there is minimal tissue damage
- the damage cells recover and tissue returns to normal within a short period
- ex: sunburn
Regeneration
- the healing process that occurs in damaged tissue in which the cells are capable of mitosis
- the damaged tissue is replaced by identical tissue from the proliferation of nearby cells
Replacement
- takes place when there is extensive tissue damage
- cells are incapable or mitosis
- functional tissue replaced by scar tissue
- loss of function
The Healing Process
- the process of tissue repair begins following injury when a blood clot forms and seals the area
- after 3 to 4 days foreign material and cell debris has been removed granulation tissue grows into the gap
Complication due to Scar Formation
- loss of function
- results from the loss of normal cells
and lack of specialized structures or normal organization in
scar tissue
- ex: hair follicles, nerves, receptors
- results from the loss of normal cells
and lack of specialized structures or normal organization in
scar tissue
Contractures and Obstructions
- scar tissue is nonelastic
- shrinks over time
- contracture
- An abnormal, often permanent shortening, as of muscle or scar tissue, that results in distortion or deformity, especially of a joint of the body
Adhesions
- bands of scar tissue joining two surfaces that are normally separated
Hypertrophic Scar Tissue
- overgrowth of fibrous tissue
- leads to hard ridges of scar tissue or keloid formation
Ulceration
- blood supply may be impaired around scar
- results in further tissue breakdown and ulceration at future time
Burn
- a thermal (heat) or nonthermal (electrical or chemical) injury to the body, causing acute inflammation and tissue destruction
- may be mild or severe
- classified by the depth of skin damage and the percentage of body surface area involved
Superficial Partial-Thickness Burns (First Degree)
- involves epidermis and may involve upper part of dermis
- little, if any, blister formation
- usually appears red and painful but readily healed without scar tissue
Deep Partial-Thickness Burn (second degree)
- involve the destruction of the epidermis and part of the dermis
- area is red, edematous, blistered, and often hypersensitive
- easily infected
Full Thickness Burns (third and fourth degree)
- destruction of all skin layers and underlying tissues
- burn area may be painless b/c of destruction of the nerves
Effects of Burn Injury
- both local and systemic
- shock
- dehydration and edema
- respiratory problems
- pain
- infection
Hematocrit
- the percentage of RBCs in a volume of blood