What management goal should be a PRIORITY, if you have a patient that is high risk for a pressure injury (PI)?
- Educate them and their caregivers on the importance of proper nutrition.
- Apply a moisture barrier cream daily to protect their skin from incontinence.
-
- Use foam cushions to support their body in her current position.
Est. a repositioning schedule to relieve pressure on vulnerable areas every 1-2 hrs.
For patients at high risk of PIs, repositioning should be the PRIORITY because it helps redistribute pressure and prevents prolonged pressure on the same areas, which is the primary cause of PIs. While nutrition is important, it is secondary to the immediate need to offload pressure. Moisture management is important but does not directly address the key risk of pressure, which is the main cause of injury in high-risk patients. Foam cushions may help with pressure distribution, but without regular repositioning, they are insufficient to prevent PIs on their own.
- Address key risk factors when setting goals: Such as-
Limited mobility, poor nutrition, moisture, and comorbidities elevate PI risk. High-risk patients require frequent repositioning, advanced support surfaces, and nutritional monitoring.
- Tailor interventions to risk levels: Such as-
Adjust care plans for high-, moderate-, and low-risk patients with strategies ranging from proactive skin care to basic prevention routines.
- Participate in regular interdisciplinary meetings: Such as-
Interdisciplinary collaboration is integral to providing effective patient-centered care
Support Surface Goals: When caring for pt.'s at risk for PI's it's important to use appropiate support surfaces for PI prevention.
- Redistribute Pressure: Refers to a support surface’s ability to spread body weight across a wider area, which helps reduce pressure on specific points and lowers the risk of PIs.
- Enhance Immersion: Indicates how much the body sinks into the support surface. Deeper immersion (e.g., sinking 6 inches) leads to improved pressure distribution compared to shallower immersion (e.g., sinking 4 inches).
- Promote Envelopment: Describes how well a support surface conforms to the body's shape, reducing concentrated pressure on the skin and improving comfort.
Guidelines for Using Support Surfaces: Support surfaces alone cannot prevent or heal PIs; they must be part of a comprehensive prevention and treatment plan. Key considerations include
- Patient Immobility: Assess the level of immobility or inactivity.
- Pressure Redistribution Needs: Consider features that enhance pressure redistribution, control the microclimate, and reduce shear and friction.
- Patient Size and Weight: Determine if the patient needs a bariatric bed based on their size and weight.
- Patient Positioning: Ensure the patient can be repositioned to offload pressure from affected areas.
- Fall and Entrapment Risks: Consider the risks of falls and entrapment associated with the support surface, such as overlays.
- Patient Preferences: Factor in the patient’s previous experiences and preferences with support surfaces.
Alternating Pressure (AP) Mattresses /Overlays
Mattresses and overlays that are designed to reduce the risk of PIs by periodically redistributing pressure across different areas of the body (Baranoski & Ayello, 2020). These surfaces use air cells that inflate and deflate cyclically, creating alternating high and low-pressure zones. The alternating inflation and deflation of air cells shift pressure from one area of the body to another.
Air Fluidized Beds
These beds are filled with tiny beads suspended in warm air, creating a fluid-like effect. When a patient lies on the bed, their body is partially immersed in the beads, which contour around them, distributing their weight evenly. The fluid-like environment allows the patient’s body to float, minimizes shear and pressure, boosts immersion and envelopment, significantly reducing the risk of PIs.
Air Fluidized Beds
These beds also help manage the microclimate by wicking away moisture and maintaining a consistent temperature. This helps keep the skin dry and reduces the risk of maceration and moisture-associated skin damage (MASD).
Air Fluidized Beds: Contraindication
For use with patients who have an unstable spinal cord injury.
Air Fluidized Beds are best for what stage PIs
Consider an air-fluidized bed for patients with stage 3 or 4 PIs (EPUAP et al., 2019).
Mattress Considerations
When choosing a mattress, you want to factor in the patient’s weight and how the mattress can distribute that weight, as follows (Baranoski & Ayello, 2020; EPUAP et al., 2019): For At-Risk Patients
Use reactive air or high-specification reactive single-layer foam mattresses or overlays.
Mattress Considerations
When choosing a mattress, you want to factor in the patient’s weight and how the mattress can distribute that weight, as follows (Baranoski & Ayello, 2020; EPUAP et al., 2019): For Patients with Existing PIs
Choose a support surface that offers better pressure redistribution, shear reduction, and microclimate control. This is especially important if:
- The patient cannot be repositioned off PI areas.
- The patient has injuries on two or more turning surfaces.
- The injury fails to heal or worsens.
- The patient is at high risk for additional PIs or is experiencing inadequate pressure redistribution, also commonly referred to as “bottoming out”
Mattress Considerations
When choosing a mattress, you want to factor in the patient’s weight and how the mattress can distribute that weight, as follows (Baranoski & Ayello, 2020; EPUAP et al., 2019): Advanced Surfaces for Severe Injuries
Consider alternating pressure, low air loss beds, or air-fluidized surfaces, particularly for patients with stage 3 or 4 PIs. However, be cautious with air-fluidized beds as they can increase the risk of dehydration due to high airflow.
Sarah develops a Stage 1 PI on her heel. Which support surface intervention is MOST appropriate to prevent the PI from worsening?
Place a pillow under the knees to elevate the legs.
Use a heel suspension device to offload pressure completely from the heels.
Apply a soft foam dressing directly to the heel and avoid further interventions.
Increase the frequency of turning to every 3 hours.
Use a heel suspension device to offload pressure completely from the heels.
*A heel suspension device is MOST appropriate to promote healing because it effectively offloads all pressure from the heel. Placing a pillow under the knees to elevate the legs may inadvertently increase pressure on the heels rather than relieve it. While a dressing may protect the skin, it does not adequately offload pressure from the heel. While more frequent turning is beneficial, it may not fully address the need for targeted offloading of the heel.
- Understand support surface goals: Support surfaces
Redistribute pressure, enhance immersion, and conform to the body’s shape to minimize concentrated pressure points and improve comfort.
- Match surfaces to patient needs: For at-risk patients
Use foam overlays or reactive mattresses; for those with existing PIs or severe injuries, consider high-tech solutions like alternating pressure or low air loss beds to manage microclimates and prevent worsening.
- Incorporate offloading strategies: Use devices like heel suspension devices or specialty pillows to
ift high-risk areas entirely off surfaces, reducing pressure on bony prominences such as heels or elbows.
- Maintain and monitor effectiveness: Regularly inspect support surfaces for...
wear, ensure proper fit and positioning, and avoid excessive bedding that can hinder pressure redistribution. Perform hand checks or use pressure mapping to detect "bottoming out."
Positioning for Critically Ill considerations
These patients may require careful repositioning strategies that account for hemodynamic and oxygen stabilization. These strategies include frequent, small, gradual shifts in body positions.
Tips for effective positioning:
Many strategies can be used to position a patient effectively. These strategies should (Gould et al., 2023)
- Include techniques like 30-degree lateral positioning and the use of assistive devices to reduce friction and shear.
- Be done frequently, especially when signs of pressure-related skin changes are observed.
- Provide optimal offloading and pressure redistribution.
- Avoid positioning patients directly on areas with erythema, PIs, or medical devices.
- Use assistive devices like transfer sheets to reduce friction and shear.
- Consider potential pressure points from bedding, shoes, surgical stockings, medical devices, or wheelchair foot pedals.
The Rule of 30
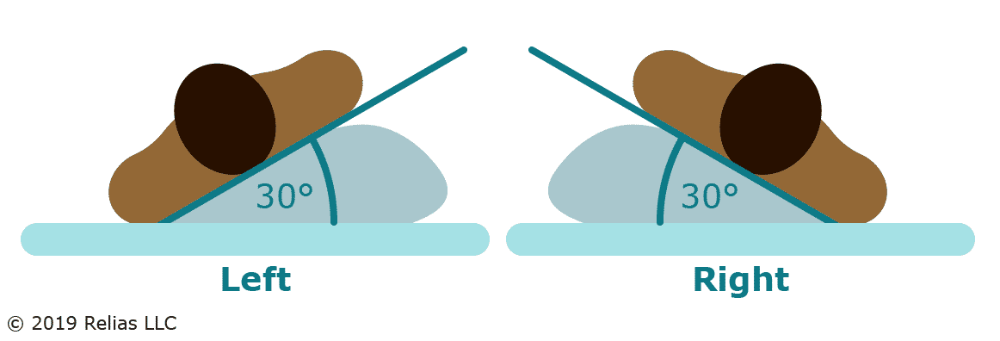
Keep the head of the bed elevated no more than 30° to reduce pressure (EPUAP et al., 2019).
Rotate patients 30° on their side in a lateral motion to offload pressure from the greater trochanters and distribute weight on fattier tissue areas.
The semi-Fowler's position is preferred when elevation above 30° is medically necessary.
The Five Pillow Rule
The “5 Pillow Rule” is a positioning technique used to prevent pressure injuries by using five pillows placed strategically to support various parts of the body when the patient is lateral in bed:
- Under the legs: To elevate the heels off the bed
- Between the ankles: Prevents friction and pressure between the ankles
- Between the knees: Maintains proper alignment and reduces pressure
- Behind the back: Supports the back in a lateral position
- Under the head: Ensures proper neck alignment and comfort
Heel Positioning:
Heels are one of the most common areas on which a PI can develop in bedbound patients.
Heel Positioning: Thus, it is important to position the heel in such a way to keep pressure off them, as follows:
At-Risk or Stage 1 and 2 PIs
Ensure heels are free of the bed surface, using a pillow or foam cushion under the calves for short-term relief (stage 1 or 2 PIs) (EPUAP et al., 2019). Some facilities may have specially designed suspension devices for heels.
Heel Positioning: Thus, it is important to position the heel in such a way to keep pressure off them, as follows:
Long-Term Support
Consider heel suspension devices for long-term use, especially in patients with stage 3 or greater PIs (EPUAP et al., 2019). When positioning heels, ensure the pressure is taken off completely so that the patient's leg weight spreads out over the lower part of the leg. Be careful not to put pressure on the Achilles tendon and the popliteal vein behind.
Heel Positioning:
For those who spend most of their time seated, consider the following recommendations (EPUAP et al., 2019).
Dynamic Weight Shifting
This means leaning the chair back and lifting the legs to decrease stress on the lower back. Ensure the feet are well supported and angle the seat from 25° to 30°. This helps avoid sliding down and reduces stress on the lower back, sitting bones, and tailbone.
Heel Positioning:
For Seated patients-
Repositioning should occur every hour for seated patients (National Pressure Injury Advisory Panel [NPIAP], 2023). Encourage pressure relief maneuvers such as:
- Weight shifting during functional activities
- Standing up and sitting back in the chair
- Leaning forward or sideways
- Arm lifts/pushups
Micro shifts (5° to 10° or a 5 to 10 second lift) with a return to the same position may not be sufficient for pressure relief
Sarah is still having difficulty mobilizing and cannot sit out of bed. What is the MOST appropriate positioning strategy?
Position Sarah prone for prolonged periods to relieve pressure on her back.
Use continuous lateral rotation therapy and maintain the patient in a 30° lateral position.
Elevate the head of the bed to 45° and place a pillow under the knees.
Reposition the Sarah once per shift and use foam padding for support.
Use continuous lateral rotation therapy and maintain the patient in a 30° lateral position.
Continuous lateral rotation therapy combined with the 30° lateral position helps redistribute pressure and reduce the risk of PIs, particularly when unable to mobilize or sit out of bed. Prone positioning can increase the risk of PIs on the face and chest if not carefully managed. Elevating the head of the bed to 45° and placing a pillow under the knees may increase pressure on the sacrum and heels, leading to a higher risk of PIs. Repositioning once per shift is insufficient for preventing pressure injuries in a high-risk, immobile patient.
- Develop effective repositioning schedules:
Tailor repositioning plans to the patient’s condition, mobility, and risk level. Use strategies like the 30° lateral position or continuous lateral rotation therapy to offload pressure for immobile patients.
- Incorporate supportive positioning techniques:
Use tools such as the “5 Pillow Rule” for proper alignment, heel suspension devices to protect vulnerable areas, and friction-reducing sheets to minimize shear forces.
- Encourage mobilization when appropriate:
Facilitate early movement, including sitting and ambulation, as soon as medically feasible. Gradually increase sitting duration while monitoring tissue tolerance.
- Reposition seated patients hourly:
For chair-bound patients, implement dynamic weight-shifting techniques like leaning, standing, or arm push-ups to relieve pressure on the sacrum, sitting bones, and heels.
PIs in darker skin tones
PIs in patients with darker skin tones, potentially missing early signs. To mitigate these biases when examining a darker skin tone, practice the following:
- Inspect the skin for discoloration using tangential light or slightly moisten the skin.
- Palpate the skin for
temperature, changes in consistency, and edema:
- Cool skin may indicate underlying necrosis.
- Induration and hardness may signal early skin damage.
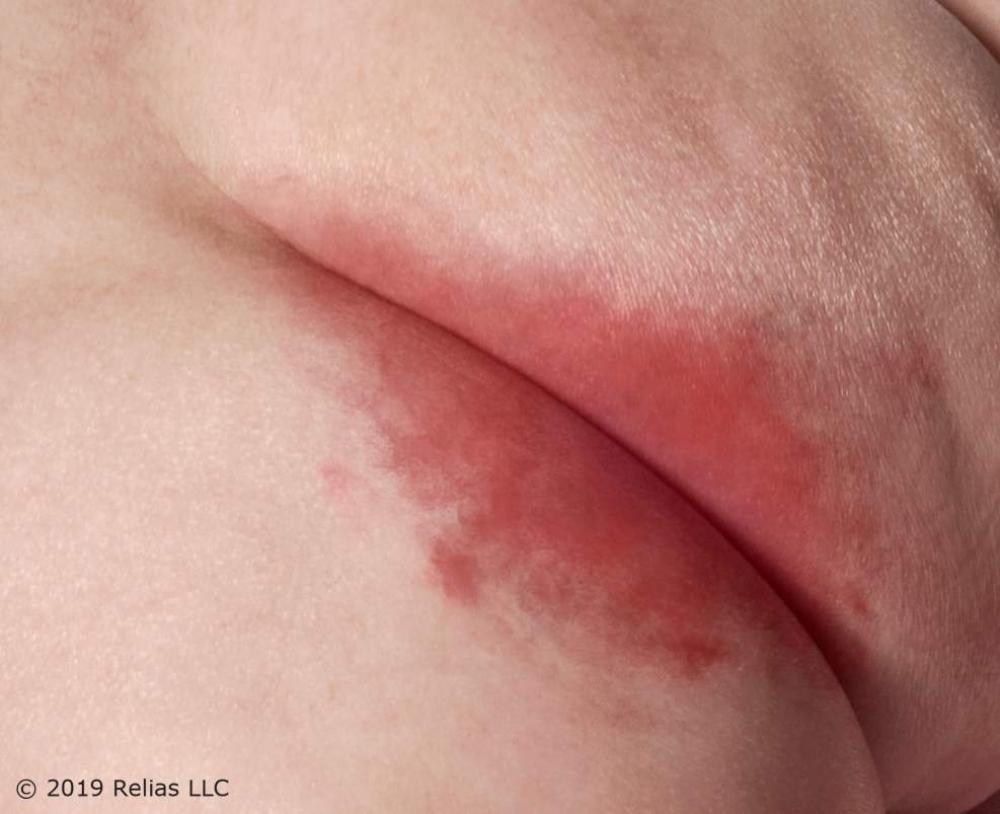
What is this rash called
ITD appears as a mirror image in skin folds, as linear and partial-thickness wounds (Baranoski & Ayello, 2020). These may progress from mild redness to intense inflammation, with erosion, oozing, exudate, maceration, and crusting.
ITD
ITD, or intertrigo , is an inflammatory condition that occurs in opposing skin surfaces due to moisture buildup (Baranoski & Ayello, 2020). It commonly affects skin folds under the breasts, in the axillae, or the inguinal and abdominal regions, especially in those with obesity.
ITD treatment
- Use a personalized skincare regime.
- Avoid irritants or friction with skin care.
- Gently pat the skin dry and consider using absorptive fabrics to reduce moisture.
Candida Infections
Candida infections, or yeast infections-
Thrive in warm, moist environments (Flowers, 2020). Candidiasis is one of the most common skin diseases in the elderly due to alterations in the skin barrier function of the skin. Diagnosis is usually made on basis of clinical presentation but can be confirmed by skin scrapings under a microscope.
ITD caused by candida will look like
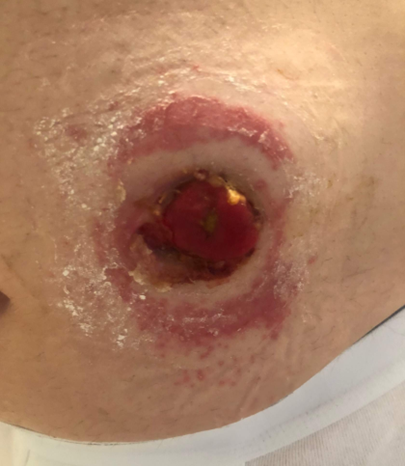
Consolidated or patchy areas with small round red papules, pustules, and satellite lesions. The area is typically tender and pruritic.
They may also appear as partial-thickness wounds with a beefy pink base, although not all skin rashes are caused by Candida; some may be due to dermatophytes or bacteria.
Common locations for ITD caused by Candida
You will often see them in areas, such as:
- Axillae
- Groin
- Peristomal skin
- Body folds
- Gluteal region
- Between the breasts
Candida Risk Factors
- Exposure to excessive moisture
- Antibiotic/steroid use
- Poorly controlled diabetes
- Poor hygiene
- Weak immune system
Light Versus Dark Skin- Candida
Candida presents as a bright red central area with satellite lesions in light-skinned patients. In darker-skinned patients, it may appear as a lighter or darker skin tone or develop into a darker red or purplish hue.
To manage Candida infections (Baranoski & Ayello, 2020; Flowers, 2020)
- Provide meticulous skincare and hygiene.
- Use pH-balanced, no-rinse cleansers.
- Ensure thorough drying of the skin.
- Apply over-the-counter (OTC) or prescription antifungal powders or creams (e.g., Nystatin, Ketoconazole, Miconazole)
Antifungal Practice Tips:
- It's crucial to continue using the antifungal for the full course of 2 weeks and then reassess, even if symptoms improve, to ensure the infection is completely eradicated.
- Overusing antifungal products can cause skin irritation, redness, burning, stinging, swelling, or other side effects including antifungal resistance.
Antimicrobial textiles specifically designed for wicking moisture away from body folds are effective but can be expensive.
Examples of such textiles include:

- InterDry® Moisture Wicking Fabric
- Remedy® DriGo-HP™ Antibacterial Wicking Sheets
- DermaTex™ Ag Moisture Wicking Fabric
Severe or non-responsive cases may require systemic treatment.
Moisture Barrier Creams and Ointments
Applied to the skin after drying helps keep the skin intact and reduce the risk of PIs. Barrier creams form a protective layer on the skin, preventing moisture from urine or feces causing irritation or breakdown. They are essential for patients with frequent incontinence to protect the skin from MASD.
Moisture Barrier Creams and Ointments
Petroleum-Based Ointments:
- Effective for creating a seal that reduces transepidermal water loss, but can leave a greasy residue that interferes with dressing adherence
Moisture Barrier Creams and Ointments
Zinc Oxide-Based:
- Offers mechanical protection and repels irritants from the skin but is thicker and more difficult to remove
Moisture Barrier Creams and Ointments
Silicone-Based: (e.g., dimethicone)
- Permeable to water vapor, allows the skin to breathe while preventing moisture-associated damage and less greasy residue than petroleum
Moisture-Associated Skin Damage (MASD)
MASD results from prolonged exposure to moisture rather than pressure (Baranoski & Ayello, 2020).
MASD has been subdivided into key areas with specific best practice statements around prevention and management for each area (Flecther et al., 2020):
- Incontinence-associated dermatitis (IAD)
- Peristomal dermatitis
- Intertriginous dermatitis (intertrigo)
- Periwound maceration
Incontinence-Associated Dermatitis (IAD)
A subset of MASD, IAD occurs due to prolonged exposure to urine or stool. It commonly affects the buttocks, perineum, inner thighs, or groin (Baranoski & Ayello, 2020). IAD presents as consolidated or patchy areas of skin damage or partial-thickness wounds without necrosis, which is associated with pressure-related ischemia.
Blisters Under Incontinence Briefs
Blisters caused by pressure from leg bands or waistbands of incontinence briefs are classified as PIs. However, blisters or skin tears resulting from adhesive tabs are categorized as medical adhesive-related skin injuries (MARSI).
What does (MARSI) stand for?
Medical adhesive-related skin injuries
Sarah has started to show early signs of incontinence-associated skin breakdown in the sacral area. What would be the BEST skincare approach in this situation?
Apply a petrolatum-based ointment as needed.
Use a pH-balanced no-rinse cleanser and moisture barrier cream.
Thoroughly wash all the zinc oxide barrier from the area with every reapplication.
Cover the area with a hydrocolloid dressing and change it daily.
Use a pH-balanced no-rinse cleanser and moisture barrier cream.Using a pH-balance no-rinse cleanser and moisture barrier cream would be BEST because they protect it from further moisture-related damage and skin breakdown. Applying a petrolatum-based ointment may offer some protection but does not address the need for regular cleansing and immediate intervention. Zinc oxide barriers should not be scrubbed off with every cleansing and reapplication. Hydrocolloid dressings are not the best first-line intervention for early skin breakdown due to moisture; managing incontinence directly is more important.
- Implement personalized skin care:
Use pH-balanced cleansers and barrier products to protect the skin from breakdown. Avoid over-cleaning, hot water, or harsh rubbing to maintain skin integrity, especially after incontinence episodes.
- Address risks in skin folds and periwound areas:
Monitor for moisture buildup, redness, or signs of Candida infections, especially in skin folds. Treat intertriginous dermatitis (ITD) with gentle drying and antifungal creams as needed.
- Identify and treat related conditions:
Differentiate between pressure injuries, MASD, and IAD (incontinence-associated dermatitis) for appropriate intervention. MASD results from prolonged moisture exposure and may require targeted hygiene and barrier protection.
- Manage incontinence effectively:
Use no-rinse cleansers, pre-moistened wipes, and moisture barrier creams to protect sacral and perineal skin from irritation. Incorporate absorbent pads, briefs, or fecal control systems to reduce moisture exposure.
The TIMERS principle used for wound care management stands for (Bowers & Franco, 2020):
T
Tissue management
I
Infection control and inflammation
M
Moisture balance
E
Edges of wound
R
Repair/regeneration
S
Social factors
Debridement
Debridement promotes healing by removing devitalized tissue and biofilm and should align with the patient’s condition and management goals.
TRUE / FALSE
Multiple debridement sessions may be needed until only healthy granulation tissue remains
True
Wound Cleansing
Cleanse the wound and peri-wound with every dressing change unless contraindicated. Choose a noncytotoxic cleanser for uninfected wounds or a cytotoxic one for infected wounds. Irrigate at appropriate pressure and address tunneling and undermining.
Debridement Guidelines
Remove necrotic tissue or biofilm to promote healing. Methods include surgical (sharp), autolytic, bio-surgical (maggots), enzymatic, and mechanical debridement. Select the method based on the patient's condition, pain tolerance, and management goals.
B
Biosurgical (maggots)
E
Enzymatic
A
Autolytic
M
Mechanical debridement
S
Sharps (conservative, surgical)
Moisture Balance
Maintain a moist wound environment. Match dressing type to wound characteristics (e.g., alginates for drainage, hydrogels for dry wounds). Use silicone-based dressings for fragile skin to minimize trauma.
B
E
A
M
S
Bio surgical - maggots
Enzymatic
Autolytic
Mechanical debridement
Sharps (conservative, surgical)
Infection Management
Monitor for signs of infection, including delayed healing, redness, or exudate. Address biofilm based on clinical signs or tissue biopsy if available. Use systemic antibiotics only for systemic infection (e.g., sepsis, cellulitis).
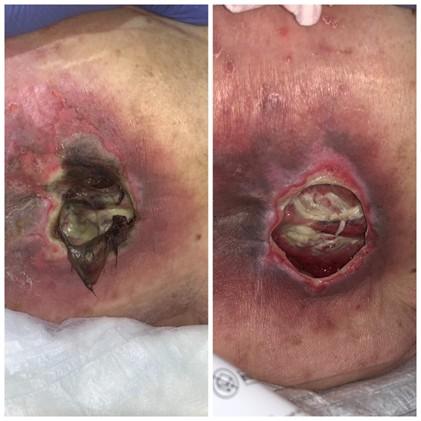
When to Debride:
* Image of unstageable sacral PI
Mechanical, autolytic, enzymatic, and/or biological methods may be considered if there is no urgent need for sharp debridement (EPUAP et al., 2019).
In general, debridement can be considered when there is evidence of:
- Biofilm (suspected or confirmed).
- Delayed wound healing (e.g., > 4 weeks).
- Failure of standard wound care measures, including antibacterial therapy.
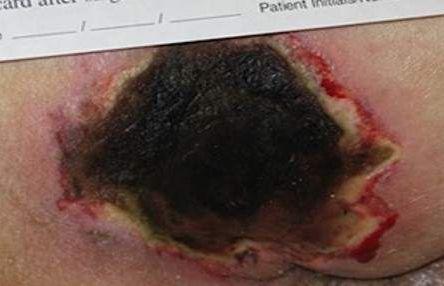
Eschar
The need to debride eschar should be assessed with every ___ ___ (EPUAP et al., 2019).
dressing change
Dry, stable eschar
Should NOT be disturbed in ischemic limbs and heels.
* However, removal of eschar may be considered if wound infection is suspected.
Signs / Symptoms of Unstable Eschar include:
- Redness
- Pain or tenderness
- Swelling
- Fluctuance
- Crepitus
- Wound odor
- Exudate
fluctuance
Is a wave-like or boggy, soft, "squishy" sensation felt when palpating a swelling or lump
Alert the patient’s primary healthcare provider if unstable eschar is present, as the patient may require immediate ___ ____ (EPUAP et al., 2019).
surgical debridement
WOUND TYPE: Draining/exudative
DRESSING: To control drainage while keeping it off the peri-wound:
- Calcium alginate
- Absorbent dressings containing collagen
- Composite
- Foam
- Hydrocolloid
WOUND TYPE:
Infected/inflamed
DRESSING:
- Silver-impregnated
- Cadexomer iodine
- Polyhexamethylene biguanide (PHMB)
WOUND TYPE: Necrotic
To debride dead tissue
DRESSING:
- Collagenase (enzymatic)
- Medical grade honey-impregnated (autolytic)
- Hydrocolloid (autolytic)
- Maggots (biologic)
WOUND TYPE: Dry (nondraining)
DRESSING: To add moisture-
- Collagen gel
- Composite
- Hydrocolloid
- Hydrogel
- Transparent film
- Medical grade honey
___-___ dressings (e.g., foam) can minimize pain or trauma during dressing changes, especially for fragile skin (EPUAP et al., 2019).
Silicone-based
- Delayed healing
- Increased wound size or depth
- Friable tissues
- Increased pain or redness
Biofilm, often resistant to antimicrobials, may require management based on clinical signs or tissue biopsy (EPUAP et al., 2019).
Characteristics that indicate the presence of infection
Antiseptics
Antiseptics used to manage the bioburden of wounds include (Norman et al., 2016):
- Cadexomer iodine
- Silver
- Medical grade honey
- Methylene blue
- Hypochlorous acid
- PHMB
- Sodium hypochlorite
- Povidone Iodine
- Acetic acid
The choice of antiseptic depends on the patient and the wound's condition.
____ ____ are reserved for confirmed systemic infections, like cellulitis or sepsis, and abscesses that require drainage to prevent further spread (EPUAP et al., 2019).
Systemic antibiotics
__________ may need surgical interventions and treatment with IV antibiotics under the guidance of an infectious disease specialist. Sepsis, gas gangrene, and necrotizing fasciitis are all examples of such infections.
Severe, limb- or life-threatening infections
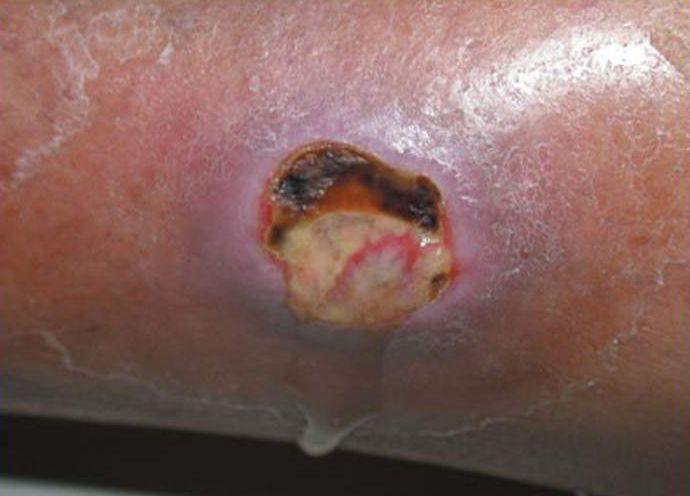
What type of dressing can be used to manage the exudate of this wound?
Hydrogel dressing
Transparent film dressing
Calcium alginate dressing
Collagenase dressing
Calcium alginate dressing
Calcium alginate dressings are highly absorbent, making them ideal for wounds with moderate to heavy exudate. They help manage wound drainage while also promoting autolytic debridement, which assists in removing slough and necrotic tissue. Hydrogel dressings are more appropriate for dry wounds, as they add moisture to the wound bed. Transparent film dressings are best used for superficial wounds or wounds with minimal exudate, as they do not absorb exudate and are not suited for wounds with necrotic tissue. While collagenase dressings are useful for enzymatic debridement, they are not the best choice for wounds with high exudate because they do not manage moisture as effectively as calcium alginate.
___ ___ dressings are highly absorbent, making them ideal for wounds with moderate to heavy exudate.
Calcium alginate
Nutritional Guidelines- Consider the following recommendations for patients with PIs (EPUAP et al., 2019):
Protein
1.2 to 1.5 g/kg/day or adjust based on patient needs
Nutritional Guidelines- Consider the following recommendations for patients with PIs (EPUAP et al., 2019):
Calories
30-35 kcal/kg/day
Nutritional Guidelines- Consider the following recommendations for patients with PIs (EPUAP et al., 2019):
Fortified Foods
Add to diet if nutritional needs are unmet
Nutritional Guidelines- Consider the following recommendations for patients with PIs (EPUAP et al., 2019):
Nutritional Supplements
Add to diet if nutritional needs are unmet
Fortified Foods
Products that have nutrients—specifically vitamins, minerals, or fiber—added to them that are not naturally present or are present in small amounts
Role Nutrition and Hydration:
- Stage 2 or Greater PI Patients with a PI that is Stage 2 or greater or who are at risk for being or are malnourished may require (EPUAP et al., 2019):
- High caloric and protein intake.
- Supplements with arginine, zinc, and antioxidants as appropriate.
- Select dressings based on wound type: Use alginates Remember Maintain moisture balance with dressings tailored to the wound’s condition to promote healing and protect fragile skin.
for draining wounds
Select dressings based on wound type: Use Hyrogels
dry wounds
Select dressings based on wound type: Use Silver-Impregnated dressings for
Infected wounds
- Address infection and eschar appropriately:
Monitor for infection signs like delayed healing or exudate, using antiseptics like silver or medical honey as needed. Debride unstable eschar carefully to remove biofilm or necrotic tissue but avoid disturbing dry eschar on ischemic areas like heels.
- Ensure adequate nutrition:
Patients with Stage 2 or higher PIs require 1.2 to 1.5 g/kg/day of protein and 30 to 35 kcal/kg/day. Add supplements like arginine, zinc, and antioxidants to support healing in malnourished or at-risk patients.