What are the eight main segments of the GI tract?
Mouth, Pharynx, Esophagus, Stomach, Small Intestine, Large Intestine, Rectum, and Anus
What are the four accessory organs of the GI tract?
Salivary Glands, Liver, Gallbladder, and Pancreas
What are the defenses against microorganisms in the GI tract?
- Layer of mucus coating intestinal surfaces
- Secretory IgA
- Peristalsis keeps microbes moving
- Saliva (includes lysozyme, lactoferrin)
- Stomach (has extremely low pH)
- Bile is antimicrobial
- GALT (gut-associated lymphoid tissue) - Includes Peyer's patches and isolated lymphoid follicles
Describe the normal biota of the oral microbiome
- Dominated by bacterial species
- Methane-producing archaea
- Fungi (Candida albicans is the most common)
- Few protozoa species
- Virome is still being studied
Describe the normal biota of the gut microbiome, specifically the esophagus and stomach
- Consists of 200 different species
- Most common types belong to Firmicutes (Streptococcus, Staphylococcus, Clostridium, and Bacillus species)
Describe the normal biota of the gut microbiome, specifically the large intestine
- The large intestine is known to have billions of microorganisms (10^11)
- Includes bacteria, fungi, and several protozoa
Describe the normal biota of the accessory organs
Accessory organs (salivary glands, pancreas, liver, gallbladder) are free of normal biota
What are the three functions of normal gut biota?
- Protective function
- Teach immune system to react properly to microbial antigens
- Aid digestion and provide nutrients that we cannot produce ourselves
True or False: A diverse gut microbiome is associated with better health
True; When the gut microbiome loses its diversity, deviations from gastrointestinal -- and systemic -- health can occur. Disruptions may come from antibody treatment, illness, pregnancy, or dietary changes.
Saliva, sIgA, lysozyme, tonsils, and adenoids are defenses of the _________.
Oral Cavity
GALT, lymphoid tissue, Peyer's patches, appendix, sIgA, and rich normal biota are defenses of the ________
rest of the GI tract
Dental Caries (AKA tooth decay)
- Most common infectious disease of human beings
- Dissolution of the tooth surface due to the metabolic action of bacteria (results in minor to complete disruption of enamel; destruction of deeper layers can result in infection of the pulp)
Main causes of dental caries (AKA tooth decay)
Streptococcus mutans and S. sobrinus
The pulp contains _______
Blood vessels and nerves
_____ ___ dissolves the enamel of the tooth.
Lactic Acid
What are some stages in the development of dental caries?
- Incidence of dental carries varies according to carbohydrate consumption, oral hygiene, and genetic factors
- Streptococci produce sticky polymers of glucose, called fructans and glucan, aiding in the formation of plaque biofilm
Stages in Plaque Development and Cariogenesis
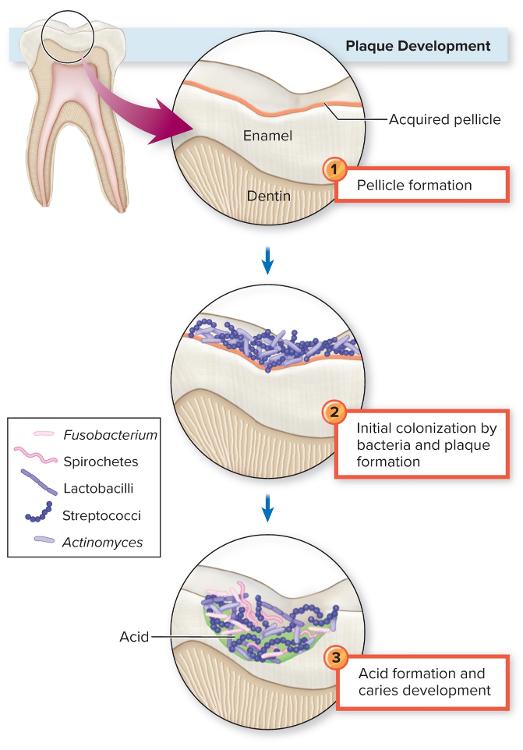
The bacteria forms a biofilm (can be made of multiple bacteria and some fungi) called plaque which is usually fuzzy.
The initial stage of periodontal disease is ______
Gingivitis
What are the signs of gingivitis?
- Swelling
- Loss of normal contour
- Patches of redness
- Increased bleeding
What are some other signs of periodontisis?
- Development of spaces or pockets between tooth and gingiva
- Disease extends into the periodontal membrane and cementum
- Deeper involvement increases the size of pockets, causes bone resorption, and tooth loss
Stages in Soft Tissue Infection, Gingivitis, and Periodontitis
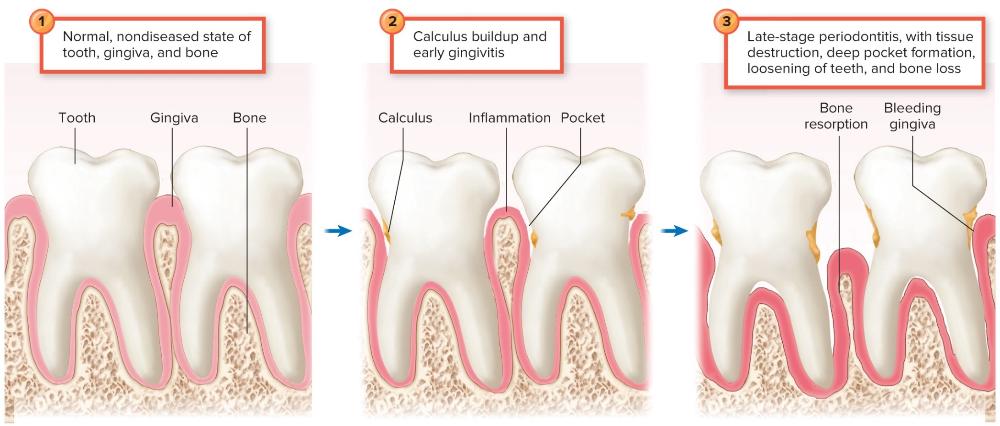
An individual's risk for dental caries or periodontitis is directly related to:
- Presence of Methanobrevibacter oralis
- Behavior (lack of flossing will put you at risk)
- Genetic influences
- Tooth position
- Presence of mineralized plaque called calculus
The most severe form of periodontal disease is ___________________________ which progresses to ___________________.
Necrotizing Ulcerative Gingivitis; Necrotizing Ulcerative Periodonitis
What is the difference between NUG and NUP?
NUP is associated with advanced bone destruction
What is commonly referred to as "trench mouth" reflecting the poor dental health of soldiers in World War l?
Necrotizing Ulcerative Gingivitis and Periodontitis
Signs and symptoms of NUG and NUP
- Severe pain, bleeding, pseudomembrane formation, and necrosis
- NUP is associated with advanced bone destruction
An infection in the accessory salivary glands ______.
Mumps
What is Mumps caused by?
Paramyxovirus (A single-stranded RNA virus)
What are some signs and symptoms of the Mumps?
- Fever, nasal discharge, muscle pain, malaise
- Followed by inflammation of the salivary glands, producing swelling of cheeks
Mumps is associated with a distinctive and painful swelling ____.
At the angle of the jaw
What is the average incubation period for Mumps?
2-3 weeks
True or False: Viral multiplication in salivary glands is followed by invasion of other organs, especially the testes, ovaries, thyroid gland, pancreas, meninges, heart, and kidney.
True
What are some complications of Mumps?
- Can invade other organs: testes, ovaries, thyroid glands, pancreas, meninges, heart, and kidney
- Occurs in 20%-30% of young adult males where infection localizes in the epididymis and testes; does not cause sterility.
What are some effects of paramyxoviruses?
- It causes cell to cell fusion, causing giant cells that are multi-nucleated.
- A virus-infected cell is modified by the insertion of proteins called HN spikes into its cell membrane. The HN spikes immediately bind an uninfected neighboring cell, and in the presence of another type of spike called F spikes, two cells permanently fuse.
- A chain reaction of multiple cell fusion then produces a syncytium with cytoplasmic inclusion bodies, which is useful for diagnostic.
____ is a sharp or burning pain emanating from the abdomen.
Gastritis
_________ are lesions in the mucosa of the stomach or uppermost portion of the small intestine.
Gastric or Peptide Ulcers
Severe ulcers can be accompanied by:
Bloody stools, vomiting, or both
When are symptoms of gastritis the worst?
Worse at night, after eating, or under conditions of psychological stress
What is the causative agent of gastritis and gastric ulcers?
Helicobacter pylori
Is Helicobacter pylori gram-negative or positive? What is the morphology of H. pylori?
Gram-Negative; Rod
The best treatment of gastritis and gastric ulcers is: _____________.
Clarithromycin
How is gastritis and gastric ulcers transmitted?
Oral-Oral; Fecal-Oral
Urea breath test is one way to diagnose _____________.
H. pylori
- This test is a noninvasive method in which patients ingest urea that has radioactive tag on the carbon molecule. If Helicobacter is present, the bacterium's urease breaks down the urea and the patient exhales the radioactively labeled carbon.
True or False: Acute diarrhea can occur without vomiting.
False; Acute diarrhea can occur with or without vomiting.
Diarrhea is defined as ____ or more loose stools in a __-hour period.
Diarrhea is defined as 3 or more loose stools in a 24 hour period.
- In the United States: average of 1.2 to 1.9 cases per person per year
- A third of cases are transmitted by contaminated food
- In tropical countries, children experience more than 10 episodes per year
- More than 700,000 children die from diarrhea per year, mostly in developing countries
The most common and deadliest cause of foodborne illness in the United States is ________
Salmonella
Is Salmonella (S. enterica) gram-negative or positive?
Gram-Negative
What antigens are used to identify gram-negative enterics?
- H - flagellar antigen
- K - Capsular antigen
- O - Cell wall antigen, the polysaccharide portion of LPS
Salmonella is motile... which means...
- They ferment glucose with acid and sometimes gas; and most of them produce hydrogen sulfide (H2S) but not urease.
- Grow readily on most laboratory media and can survive outside the host in inhospitable environments, such as freshwater and freezing temperatures.
- Resistant to chemicals such as bile and dyes, which are the bases for isolation on selective media.
What is a common factor of all salmonella?
They are acid producers
What are some signs and symptoms of Salmonella?
- Causes a variety of diseases resulting in 1 million cases and 400 deaths a year
- Salmonellosis - Enteric fever or gastroenteritis (can range from mild gastroenteritis such as vomitting, diarrhea, and mucosal irritation to fever and septicemia)
- Typhoid fever - Produced by a specific Salmonella; Salmonella enterica serotype Typhi
- Ability to cause disease is dependent on its ability to adhere to the gut mucosa (has a high ID50; many organisms have to be ingested for disease to result)
How can Salmonella be prevented?
The only prevention for salmonellosis is avoiding contact with the bacterium.
What is an important virulence factor for Salmonella?
Endotoxin
Is Shigella gram-negative or positive? What is the morphology of Shigella?
Gram-Negative; Straight Rod
Salmonella is ____ whereas Shigella is ____.
Motile; Nonmotile
What does nonmotile mean?
Unable to form endospores and produce unrease or H2S
Shigella is known to cause _____ ______.
Shigella dysenteriae
What is dysentery?
Diarrhea containing blood
What are symptoms of Shigella?
- Frequent, watery stools, fever, and intense abdominal pain
- Nausea and vomiting are common
- Dysentery
- Mucus from GI tract will also be present in stools
_____ __________ causes the most severe form, is uncommon in the United States, and occurs primarily in the Eastern Hemisphere.
Shigella dysenteriae
Shigella are primarily human _____. All produce a similar disease, including ____ ____, that can vary.
Parasite; Bloody Diarrhea
Where is Shigella dysenteriae most common?
This most severe form is primarily common in the Eastern Hemisphere. It is uncommon in the United States.
How is Shigellosis different from other GI tract infections?
- Shigella invades the villus cells of the large intestine rather than small intestine.
- Not as invasive as Salmonella and does not perforate the intestine or invade the blood
How does Shigella enter the intestinal mucosa?
It enters the intestinal mucosa by means of lymphoid cells in Peyer's patches. Once in the mucosa, Shigella instigates an inflammatory response that causes the extensive tissue destruction.
The endotoxin released by Shigella causes ____
Fever
The enterotoxin released by Shigella...
Affects the entire GI tract, damages the mucosa and villi, and gives rise to bleeding and secretion of mucus
The shiga toxin released by Shigella...
is responsible for more serious damage to the intestine as well as systemic effects; it interrupts protein synthesis in its target cells
Shigella is localized or systemic?
Localized to the intestines
Shiga-Toxin-Producing Escherichia coli (STEC)
- Another shiga toxin producer
- Some common signs and symptoms are those GI problems, and very rarely, sometimes you can see hemolytic uremic syndrome
- Toxins are identical to shiga toxins produced by Shigella
How is STEC transmitted?
Ingestion of undercooked beef and other contaminated foods and beverages
What is the hemolytic uremic syndrome?
Severe hemolytic anemia that can cause kidney damage and failure
Most common bacterial cause of diarrhea in the United States is _________
Campylobacter
What are some signs and symptoms of Campylobacter?
- Frequent watery stools, fever, vomiting, headaches, and severe abdominal pain
- Symptoms may last longer than 2 weeks and recur
Campylobacter jejuni is a Campylobacter species. What is the morphology?
Curved or Spiral Gram-Negative with polar flagella
Where are Campylobacter jejuni found?
These tend to be microaerophilic inhabitants of the intestinal tract, genitourinary tract, and oral cavity of humans and animals
How is Campylobacter transmitted?
Ingestion of contaminated beverages, food, water, milk, meat, and chicken
In a small number of cases of Campylobacter, infection can lead to a serious neuromuscular paralysis called ______________________
Guillain-Barre syndrome
What is the Guillain-Barre syndrome?
- Leading cause of acute paralysis in the US (good news is that many patients recover completely)
What is the prevention and treatment of Campylobacter?
- Rehydration and electrolyte-balance therapy
- Azithromycin in severely affected patients
- Prevention depends on rigid sanitary control of water and milk supplies and care in food preparation
Clostridioides difficile is a gram-________ bacteria and the morphology is ________.
Clostridioides difficile is a gram-positive, endospore-forming rod
True or False: Clostridioides difficile was once considered part of our normal biota (harmless).
True; It was once considered relatively harmless but now is known to cause a condition called pseudomembranous colitis, also known as antibiotic-associated colitis.
How is pseudomembranous colitis caused?
Pseudomembranous colitis is known as a antibiotic-associated colitis because in many cases, this infection is precipitated by therapy with broad-spectrum antibiotics. --> Major cause of diarrhea
Clostridioides difficile is able to superinfect the large intestine when drugs have distrupted the normal biota. It results in the production of two enterotoxins (A and B) which essentially results in...
necrosis in the wall of the intestine --> in more severe cases the colon is inflamed and gradually sloughs off loose, membranelike patches called pseudomembranes consisting of fibrin and cells --> if not stopped, perforation of the cecum and death can result
What is the predominant symptom of Clostridioides difficile?
Diarrhea (in some severe cases, it can cause abdominal cramps, fever, and leukocytosis)
What are some treatments of Clostridioides difficile?
- Withdrawal of antibiotics, replacement of fluids
- Fidaxomicin or vancomycin
- Fecal transplant
What is the morphology of vibrio cholerae?
Curved rod with a single polar flagellum
What are some characteristics of vibrio cholerae?
- Fermentative
- Grow on ordinary or selective media containing bile at 37 degrees Celsius
- Possess unique O and H antigens and other membrane receptor antigens
When are spikes of cholera seen?
Outbreaks of cholera are expected to happen after natural disasters, war, or large refugee movements
What are two types of cholera?
Class and El Tor
Signs and symptoms of Vibrio cholerae include:
- Vomiting
- Copious watery feces, "rice-water stool"
- Profuse water loss (so you get really dehydrated and that gives you hypotension --> get tachycardia --> go into shock)
- Loss of blood volume, acidosis, potassium depletion, muscle cramps, severe thirst, flaccid skin, and sunken eyes; convulsions and coma in young children
- Hypotension, tachycardia, cyanosis, shock
- 55% to 70% mortality rate
What is the toxin produced by Vibrio cholerae and what role does the toxin play?
Produces cholera toxin which disrupts the normal physiology of intestinal cells, causing them to shed large amounts of electrolytes into the intestine
What are some pathogenesis and virulence factors of Vibrio cholerae?
- Cholera toxin
- Uses quorum sensing to regulate the expression of virulence factors
What type of environment promotes growth of Vibrio?
Warm, monsoon, alkaline, and saline conditions
Treatment of Vibrio cholerae?
Oral Rehydration Therapy
Who found the use of sari's to help filter out water?
Rita Cowell helped reduce the amount of cholera in endemic areas, where she helped understand cholera could be found in dormant water and the water can be filtered using sari's.
Non-cholera vibrios lack the _____.
Cholera toxin
True or False: It is more common to experience an infection with a non-cholera species of Vibrio than a V. cholerae infection.
True; These infections are called vibrioses.
What are the prominent causative agents of Non-Cholera Vibrio (aka vibriosis)?
V. vulnificus and V. parahaemolyticus
What three factors increase the chance of vibrioses?
- Increased consumption of raw oysters
- Increased awareness; more people are diagnosed
- A warming climate increases the microbe's habitats
Cryptosporidium is a type of _________.
Protozoa
Describe crytosporidium
- The oocyst form is resilient and can immediately infect
- Once inside the intestines, the oocytes releases sporozytes that attach to the epithelium of small intestines where it will live inside. It will eventually make more of these protozoa that are released into the gut and release through the stool to infect others
- The symptoms are similar to other gastroenteritis, and these are very resistant to chlorine and other disinfectants
- Symptoms include headache, sweating, vomiting, severe abdominal cramps, and diarrhea
Crytosporidium outbreaks occur in ______.
Swimming pools
What are Rotaviruses?
- Double-stranded RNA with an inner and outer capsid
- Primary cause of morbidity and mortality resulting from diarrhea
How is Rotavirus transmitted?
Fecal-Oral Route, including contaminated food, water, and fomites
How is Rotavirus treated?
- Via oral replacement therapy
- RotaTeq and Rotarix are live attenuated vaccines
What is the most common food-borne virus in the United States? Why?
Norovirus; It has a low infectious dose (1 to 20 viruses)
What are symptoms of norovirus?
Profuse, watery diarrhea for 3 to 5 days, vomiting in the early stages, mild fever
How is norovirus transmitted?
- Fecal-Oral transmission or via contamination of food and water
- Many outbreaks associated with cruise ships
What is food poisioning?
- Food poisoning is nausea and vomiting accompanied by diarrhea, often companions that shared a meal suffer the same fate
- Symptoms are caused by exotoxin (therefore, sometimes thought of as an intoxication rather than infection)
- Occasionally comes from nonmicrobial sources such as fish, shellfish, or mushrooms
- This is acute diarrhea with vomiting caused by exotoxins
What are the three exotoxins that cause food poisoning?
- Staphylococcus aeureus exotoxin
- Bacillus cereus exotoxin
- Clostridium perfringens exotoxin
This exotoxin that causes food poison is associated with custards, sauces, cream pastries, processed meats, chicken salad, or ham
Staphylococcus aureus
Staphylococcus aureus exotoxin characteristics:
- Thrives due to high salt tolerance
- Enterotoxin is heat stable and induces symptoms of cramping, nausea, vomiting, and diarrhea
- Onset within 1-6 hr, recovery within 24 hours
- Self-limiting, antibiotics are warranted
Bacillus cereus exotoxin is gram-________ bacterium that lives in the _____.
Bacillus cereus exotoxin is gram-positive bacterium that lives in the soil.
Two forms of bacillus cereus exotoxin are:
- Emetic (vomiting) from frequently tied to fried rice that has been cooked and kept warm for long periods of time
- Diarrheal form associated with cooked meats or vegetables held at a warm temperature for long periods of time (profuse, watery diarrhea that lasts about 24 hours)
Clostridium perfringens exotoxin is also the causative agent of __________.
Clostridium perfringens exotoxin is also the causative agent of gas gangrene.
Describe Clostridium perfringens exotoxin
- Contaminates meat, fish, and beans that have not been cooked thoroughly enough to destroy endospores
- Endospores germinate in foods, C. perfringens cells enter the small intestine and release exotoxin
- Abdominal pain, diarrhea, and nausea in 8 to 16 hr
- Also causes enterocolitis similar to that caused by C. difficile
What defines chronic diarrhea?
- Diarrhea that lasts longer than 14 days
- Can have an infectious or noninfectious cause; Irritable bowel syndrome (can be caused by microbiota or genetic), ulcerative colitis
- Microbes in this section cause chronic diarrhea in otherwise healthy people
Enteroaggregative E. Coli (EAEC)
- Associated with chronic disease, particularly in children
- Adheres to human cells in aggregates rather than single cells
- Stimulates large amounts of mucus in the gut
- Transmission through food and water
Cyclospora cayetanensis
- Emerging protozoan pathogen; numerous outbreaks in United States and Canada
- Fecal-oral transmission from fresh produce and water
- Oocytes can be visualized when feces is exposed to UV light
- Only infectious when sporulated oocyst are ingested
- Symptoms: watery diarrhea, stomach cramps, bloating, fever, and muscle aches
Giardia duodenalis is commonly known as:
- Giardia intestinalis
- Giardia lamblia
Giardia duodenalis is a __________.
Protozoa
Describe the morphology of Giardia duodenalis
- Symmetrical heart shape with organelles positioned in such a way that it resembles a face with four pairs of flagella emerging from the ventral surface
Signs and symptoms of Giardia duodenalis:
- Diarrhea of long duration
- Abdominal pain
- Flatulence
- Greasy and malodorous stools
In Giardia duodenalis, the presence of this protozoa leads to malabsorption of _____ in the digestive tract.
In Giardia duodenalis, the presence of this protozoa leads to malabsorption of fat in the digestive tract. Usually results in significant weight loss
True or False: Giardia duodenalis; Superficial invasion by trophozoites causes damage to the epithelial cells, edema, and infiltration by white bloods, which is irreversible.
True
Where is Giardia isolated from?
- Beavres
- Cattles
- Coyotes
- Cats
- Human Carriers
Although trophozoites and cysts escape in the stool, _____ play a greater role in transmission. Why?
Although trophozoites and cysts escape in the stool, cysts play a greater role in transmission. Giardia cysts can survive for 2 months in environment and are usually ingested with water and food or swallowed after close contact with infected people or contaminated objects.
True or False: Giardiasis can easily be diagnosed from feces.
False; Giardiasis can be difficult to diagnose because the organism is shed in feces only intermittently.
Where do outbreaks of Giardia occur?
Epidemics can be traced to water from mountain streams as well as chlorinated municipal water.
True or False: The treatment for Giardia is a vaccine.
False; No human vaccine is available. Avoiding drinking from freshwater sources is the major preventive measure. The agent is killed by boiling, ozone, and iodine; however, the amount of chlorine used in municipal water supplies does not destroy the cysts.
Entamoeba is a _________.
Entamoeba is an amoeba that are widely distributed in aqueous habitats.
The Entamoeba histolytica has a relatively simple life cycle that alternates between ________ that is motile by means of __________ and a _____, ______, nonmotile _______.
The Entamoeba histolytica has a relatively simple life cycle that alternates between trophozoite that is motile by means of pseudopods and a smaller, compact, nonmotile cyst.
- Trophozoite lacks most of organelles and has a single nucleolus called karyosome.
- The mature cyst is encased in a thin yet tough wall and contains four nuclei as well as chromatoidal bodies, which are actually dense clusters of ribosomes.
Entamoeba hysolytica
- Secrete enzymes that dissolve tissues
- Exist in intestinal and extraintestinal forms
- Humans are primary hosts; infection through food and water contaminated with cysts
Intestinal Amoebiasis
- Initial targets are cecum, appendix, colon, and rectum
- Actively penetrates deeper layers of mucosa leaving ulcers
- Dysentery along with abdominal pain, diarrhea, fever, and weight loss
- Can lead to hemorrhage, perforation, appendicitis, and amoebomas
- Goes to intestine
Extraintestinal Amoebiasis
- Amoeba invade the viscera of the peritoneal cavity invading the liver
- Goes to the liver
In general, what is hepatitis?
Hepatitis is the inflammatory disease of the liver:
- Necrosis of hepatocytes
- Response by mononuclear white blood cells that swells and disrupts the liver architecture
- Interferes with excretion of bile pigments and causes bilirubin to accumulate in blood and tissues, causing jaundice (yellowing of the skin and eyes)
Hepatitis A
- Non-enveloped, single-stranded RNA enterovirus
- Signs and symptoms include subclinical or vague flu-like symptoms, fever, nausea, abdominal pain, dark urine -- may have jaundice (in only about 10% of the cases)
- Transmitted via fecal-oral, associated with deficient personal hygiene and lack of public health measures
- Vaccine is available, but if contracted, bed rest and plenty of fluid are key for management
- There is no cure
Hepatitis B
- Enveloped DNA virus (able to integrate)
- Signs and Symptoms: Fever, chills, malaise (usually asymptomatic), abdominal discomfort, diarrhea, and nausea; rashes and arthritis may occur; cause of hepatocellular carcinoma
- Transmitted by minute amounts of blood (sexual, parental, and vertical)
- Vaccine is available, but there is no cure
- Vaccine is important for health care workers and students, patients receiving multiple transfusions, immunodeficient persons, and cancer patients
- No cure
- 4-6 weeks to see positive test
Hepatitis C
- Enveloped RNA virus
- Silent epidemic: 3.5 million Americans infected
- Transmission via blood transfusions and needle sharing
- Signs and symptoms include fever, fatigue, loss of appetite, nausea, vomiting, abdominal pain, dark urine, and juandice
- About 2 weeks for a positive test and symptoms
- No Vaccine
- Two drug regimen: Sofosbuvir (a nucleotide analog that “fools” the RNA polymerase of the virus) and simeprevir (a protease inhibitor)
______________ is a hallmark of helminthic infection.
Eosinophilia is a hallmark of helminthic infection
What are some general clinical considerations (pathogenesis and virulence factors) of helminth infections?
- Specialized mouthparts for attachment and feeding, enzymes to liquefy and penetrate tissues, and cuticle for protection from host defenses
- Definitive host: Host in which the adult worm reproduces sexually
Diagnosis of helminth diseases include:
- Eosinophilia
- Discovery of eggs, larvae, or adult worms in stool or tissues
What are some prevention and treatment of helminth diseases?
- No vaccines available
- Regular treatment with antihelminthic drugs
- Proper sewage disposal
- Avoiding using human feces as fertilizer
- Disinfection of water supply
- Thoroughly washing and cooking vegetables and meats
- Freezing foods
Describe cycles A and B of basic helminth life and transmission.

Describe cycles C and D of basic helminth life and transmission.

The most common worm disease of children in temperate zones is _______________.
Enterobius vermicularis
Enterobius vermicularis is a _______ disease.
Pinworm
Enterobius vermicularis is a life cycle ___ type.
Enterobius vermicularis is a life cycle A type.
The hallmark of Enterobius vermicularis is ____________.
The hallmark of Enterobius vermicularis is anal itching
Is the Enterobius vermicularis fatal?
The infection is not fatal and most cases are asymptomatic. When one member of the family is diagnosed, the entire family should be tested and/or treated because it is likely that multiple members are infected.
Trichuris trichuria is ________ and is life cycle ________.
Trichuris trichuria is whipworm and is life cycle A.
In the Trichuris trichuria, _____ are the sole host.
In the Trichuris trichuria, humans are the sole host.
Where is the highest incidence of Trichuris trichuria?
In the tropics and subtropics that have poor sanitation
In Trichuris trichuria, females lay _______ to ______ eggs daily in the bowel.
3,000 to 5,000
What are symptoms of Trichuris trichuria?
- Localized hemorrhage of the bowel
- Dysentery
- Loss of muscle tone
- Rectal prolapse (can be fatal in children)
Diphyllobothrium latum is a _______ disease in which _____ are definitive host and ____ are intermediate host.
Diphyllobothrium latum is a tapeworm disease in which humans are definitive host and fish are intermediate host.
- Can be transmitted via sushi and sashimi
- Also transmitted in the Great Lakes, Alaska, and Canada
- Symptoms include abdominal discomfort or nausea, anemia
Hymenolepsis species includes ____ ______ and its life cycle is _____. There are two species _______ ____ and ______ ______.
Hymenolepsis species includes small tapeworms and its life cycle is C. There are two species Hymenolepis nana and Hymenolepsis diminuta.
- Hymenolepsis nana - Dwarf tapeworm
- Hymenolepsis diminuta - Rat tapeworm
Taenia solium causes ___________
Cysticerosis
Taenia solium is a ______.
Tapeworm
Cysticercosis occurs when...
Cysticercosis occurs when humans ingest tapeworm eggs rather than infected meat
What is the life cycle of Taenia solium?
Life Cycle C
Where is Taenia solium distributed?
Distributed worldwide, but concentrated in areas where humans live in close proximity with pigs or eat undercooked pork
Fasciola heptica is a ____ ____ common in sheep, cattle, goats, and other mammals.
Liver fluke
Symptoms of Fasciola hepatica
vomiting, diarrhea, hepatomegaly, and bile obstruction if infected with a large number of flukes
Who is the definitive host of Fasciola hepatica?
Mammals
Liver and intestinal disease is caused by...
Fasciola hepatica
Schistosomiasis is a _______ disease
Liver
The causative organism of Schistosomiasis is...
Schistosoma masoni and S. japonicum
Schistosoma masoni and S. japonicum similarities:
- Morphologically and geographically distinct
- Similar life cycles, transmission methods, and disease manifestations
- Can invade intact skin
Signs and Symptoms of Schistomiasis
- Itchiness in the area where the worm enters the body, fever, chills, diarrhea, and cough
- Chronic infection: hepatomegaly, liver disease, splenomegaly
- Bladder obstruction, and blood in the urine
- Can cause a granulomatous response in the nervous system and heart
Pathogenesis, Diagnosis of Schistosomiasis
- Pathogenesis and virulence factors:
- Parasite coats its outer surface with proteins from the bloodstream, cloaking itself from the host defense system
- Diagnosed through identifying eggs in urine or feces
- Cycle of infection cannot be broken as long as people are exposed to untreated sewage
- Praziquantel is the drug of choice
Life Cycle of Schistosoma is ___
D
Streptococcus mutans
- Gram-Positive
- Causes Dental Caries
Helicobacter pylori
- Gram-Negative
- Causes Gastritis/Gastric Ulcers
Clostridium perfringen
- Gram-Positive, Endospore-Forming Bacteria
- Causes antibiotic-associated diarrhea
Hepatitis A
- RNA Virus
- Causes "Infectious" Hepatitis
Hepatitis B
- DNA Virus
- Causes "Serum" Hepatitis
Hepatitis C
- RNA Virus
- Causes "Serum" Hepatitis
Schistosomas
- Helminths - Trematodes
- Causes Schistosomiasis
Rotavirus
- RNA Virus
- Causes Acute Diarrhea
Mumps virus
- RNA Virus
- Causes Mumps
Giardia duodenalis
- Protozoa
- Causes Chronic Diarrhea
Enterobius vermicularis
- Helminths - Nematodes
- Causes intestinal distress
Taenia solium
- Helminths - Cestodes
- Causes Cysticerosis ( Formation of sacs of fluid (cysts) to form in your body)
- Pork tapeworm
Fasciola hepatica
- Helminths - Trematodes
- Causes liver and intestinal disease
Salmonella
- Gram-Negative
- Causes Acute Diarrhea
Shigella
- Gram-Negative
- Causes Acute Diarrhea and Dysentery
Shiga toxin-producing E. Coli
- Gram-Negative
- Causes Acute Diarrhea plus Hemolytic Syndrome
Other E. coli
- Gram-Negative
- Causes Acute or Chronic Diarrhea
Campylobacter
- Gram-Negative
- Causes Acute Diarrhea
Clostridioides difficile
- Gram-Positive, Endospore-Forming Bacteria
- Causes antibiotic-associated diarrhea
Vibrio cholerae
- Gram-Negative
- Causes cholera
Non-cholera Vibrio species
- Gram-Negative
- Causes Vibrioses
Cryptosporidium
- Protozoa
- Causes Acute Diarrhea
Rotavirus
- RNA Virus
- Causes Acute Diarrhea
Norovirus
- RNA Virus
- Causes Acute Diarrhea
Staphylcoccus aureus
- Gram-Positive
- Causes Food Poisoning
Bacillus cereus exotoxin
- Gram-Positive, Endospore-Forming Bacteria
- Causes Food Poisoning
Clostridium perfringens exotoxin
- Gram-Positive, Endospore-Forming Bacteria
- Causes Food Poisoning