Instructions for Side by Side Printing
- Print the notecards
- Fold each page in half along the solid vertical line
- Cut out the notecards by cutting along each horizontal dotted line
- Optional: Glue, tape or staple the ends of each notecard together
BMD 330 Chapter 23 - Infectious Diseases Manifesting in the Gastrointestinal Tract
front 1 What are the eight main segments of the GI tract? | back 1 Mouth, Pharynx, Esophagus, Stomach, Small Intestine, Large Intestine, Rectum, and Anus |
front 2 What are the four accessory organs of the GI tract? | back 2 Salivary Glands, Liver, Gallbladder, and Pancreas |
front 3 What are the defenses against microorganisms in the GI tract? | back 3
|
front 4 Describe the normal biota of the oral microbiome | back 4
|
front 5 Describe the normal biota of the gut microbiome, specifically the esophagus and stomach | back 5
|
front 6 Describe the normal biota of the gut microbiome, specifically the large intestine | back 6
|
front 7 Describe the normal biota of the accessory organs | back 7 Accessory organs (salivary glands, pancreas, liver, gallbladder) are free of normal biota |
front 8 What are the three functions of normal gut biota? | back 8
|
front 9 True or False: A diverse gut microbiome is associated with better health | back 9 True; When the gut microbiome loses its diversity, deviations from gastrointestinal -- and systemic -- health can occur. Disruptions may come from antibody treatment, illness, pregnancy, or dietary changes. |
front 10 Saliva, sIgA, lysozyme, tonsils, and adenoids are defenses of the _________. | back 10 Oral Cavity |
front 11 GALT, lymphoid tissue, Peyer's patches, appendix, sIgA, and rich normal biota are defenses of the ________ | back 11 rest of the GI tract |
front 12 Dental Caries (AKA tooth decay) | back 12
|
front 13 Main causes of dental caries (AKA tooth decay) | back 13 Streptococcus mutans and S. sobrinus |
front 14 The pulp contains _______ | back 14 Blood vessels and nerves |
front 15 _____ ___ dissolves the enamel of the tooth. | back 15 Lactic Acid |
front 16 What are some stages in the development of dental caries? | back 16
|
front 17 Stages in Plaque Development and Cariogenesis | back 17 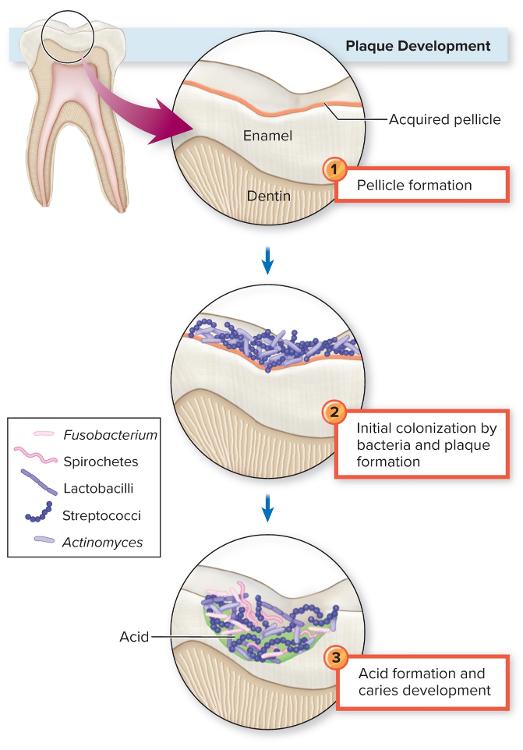 The bacteria forms a biofilm (can be made of multiple bacteria and some fungi) called plaque which is usually fuzzy. |
front 18 The initial stage of periodontal disease is ______ | back 18 Gingivitis |
front 19 What are the signs of gingivitis? | back 19
|
front 20 What are some other signs of periodontisis? | back 20
|
front 21 Stages in Soft Tissue Infection, Gingivitis, and Periodontitis | back 21 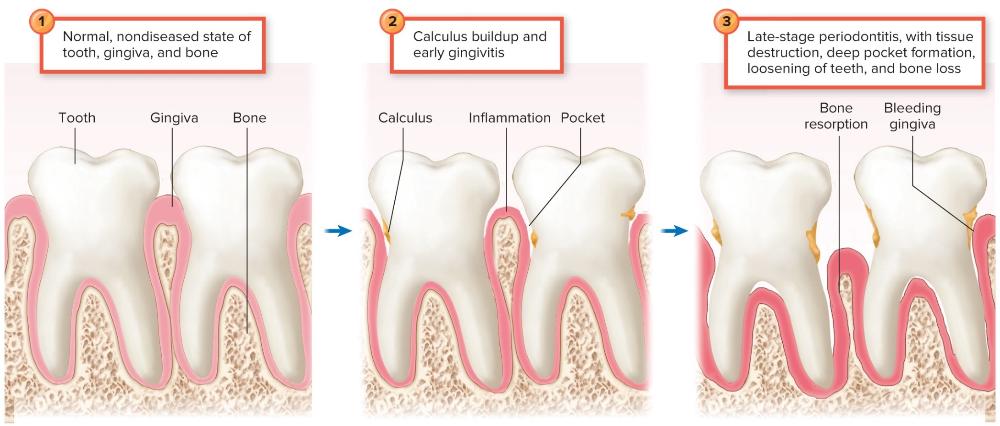 |
front 22 An individual's risk for dental caries or periodontitis is directly related to: | back 22
|
front 23 The most severe form of periodontal disease is ___________________________ which progresses to ___________________. | back 23 Necrotizing Ulcerative Gingivitis; Necrotizing Ulcerative Periodonitis |
front 24 What is the difference between NUG and NUP? | back 24 NUP is associated with advanced bone destruction |
front 25 What is commonly referred to as "trench mouth" reflecting the poor dental health of soldiers in World War l? | back 25 Necrotizing Ulcerative Gingivitis and Periodontitis |
front 26 Signs and symptoms of NUG and NUP | back 26
|
front 27 An infection in the accessory salivary glands ______. | back 27 Mumps |
front 28 What is Mumps caused by? | back 28 Paramyxovirus (A single-stranded RNA virus) |
front 29 What are some signs and symptoms of the Mumps? | back 29
|
front 30 Mumps is associated with a distinctive and painful swelling ____. | back 30 At the angle of the jaw |
front 31 What is the average incubation period for Mumps? | back 31 2-3 weeks |
front 32 True or False: Viral multiplication in salivary glands is followed by invasion of other organs, especially the testes, ovaries, thyroid gland, pancreas, meninges, heart, and kidney. | back 32 True |
front 33 What are some complications of Mumps? | back 33
|
front 34 What are some effects of paramyxoviruses? | back 34
|
front 35 ____ is a sharp or burning pain emanating from the abdomen. | back 35 Gastritis |
front 36 _________ are lesions in the mucosa of the stomach or uppermost portion of the small intestine. | back 36 Gastric or Peptide Ulcers |
front 37 Severe ulcers can be accompanied by: | back 37 Bloody stools, vomiting, or both |
front 38 When are symptoms of gastritis the worst? | back 38 Worse at night, after eating, or under conditions of psychological stress |
front 39 What is the causative agent of gastritis and gastric ulcers? | back 39 Helicobacter pylori |
front 40 Is Helicobacter pylori gram-negative or positive? What is the morphology of H. pylori? | back 40 Gram-Negative; Rod |
front 41 The best treatment of gastritis and gastric ulcers is: _____________. | back 41 Clarithromycin |
front 42 How is gastritis and gastric ulcers transmitted? | back 42 Oral-Oral; Fecal-Oral |
front 43 Urea breath test is one way to diagnose _____________. | back 43 H. pylori
|
front 44 True or False: Acute diarrhea can occur without vomiting. | back 44 False; Acute diarrhea can occur with or without vomiting. |
front 45 Diarrhea is defined as ____ or more loose stools in a __-hour period. | back 45 Diarrhea is defined as 3 or more loose stools in a 24 hour period.
|
front 46 The most common and deadliest cause of foodborne illness in the United States is ________ | back 46 Salmonella |
front 47 Is Salmonella (S. enterica) gram-negative or positive? | back 47 Gram-Negative |
front 48 What antigens are used to identify gram-negative enterics? | back 48
|
front 49 Salmonella is motile... which means... | back 49
|
front 50 What is a common factor of all salmonella? | back 50 They are acid producers |
front 51 What are some signs and symptoms of Salmonella? | back 51
|
front 52 How can Salmonella be prevented? | back 52 The only prevention for salmonellosis is avoiding contact with the bacterium. |
front 53 What is an important virulence factor for Salmonella? | back 53 Endotoxin |
front 54 Is Shigella gram-negative or positive? What is the morphology of Shigella? | back 54 Gram-Negative; Straight Rod |
front 55 Salmonella is ____ whereas Shigella is ____. | back 55 Motile; Nonmotile |
front 56 What does nonmotile mean? | back 56 Unable to form endospores and produce unrease or H2S |
front 57 Shigella is known to cause _____ ______. | back 57 Shigella dysenteriae |
front 58 What is dysentery? | back 58 Diarrhea containing blood |
front 59 What are symptoms of Shigella? | back 59
|
front 60 _____ __________ causes the most severe form, is uncommon in the United States, and occurs primarily in the Eastern Hemisphere. | back 60 Shigella dysenteriae |
front 61 Shigella are primarily human _____. All produce a similar disease, including ____ ____, that can vary. | back 61 Parasite; Bloody Diarrhea |
front 62 Where is Shigella dysenteriae most common? | back 62 This most severe form is primarily common in the Eastern Hemisphere. It is uncommon in the United States. |
front 63 How is Shigellosis different from other GI tract infections? | back 63
|
front 64 How does Shigella enter the intestinal mucosa? | back 64 It enters the intestinal mucosa by means of lymphoid cells in Peyer's patches. Once in the mucosa, Shigella instigates an inflammatory response that causes the extensive tissue destruction. |
front 65 The endotoxin released by Shigella causes ____ | back 65 Fever |
front 66 The enterotoxin released by Shigella... | back 66 Affects the entire GI tract, damages the mucosa and villi, and gives rise to bleeding and secretion of mucus |
front 67 The shiga toxin released by Shigella... | back 67 is responsible for more serious damage to the intestine as well as systemic effects; it interrupts protein synthesis in its target cells |
front 68 Shigella is localized or systemic? | back 68 Localized to the intestines |
front 69 Shiga-Toxin-Producing Escherichia coli (STEC) | back 69
|
front 70 How is STEC transmitted? | back 70 Ingestion of undercooked beef and other contaminated foods and beverages |
front 71 What is the hemolytic uremic syndrome? | back 71 Severe hemolytic anemia that can cause kidney damage and failure |
front 72 Most common bacterial cause of diarrhea in the United States is _________ | back 72 Campylobacter |
front 73 What are some signs and symptoms of Campylobacter? | back 73
|
front 74 Campylobacter jejuni is a Campylobacter species. What is the morphology? | back 74 Curved or Spiral Gram-Negative with polar flagella |
front 75 Where are Campylobacter jejuni found? | back 75 These tend to be microaerophilic inhabitants of the intestinal tract, genitourinary tract, and oral cavity of humans and animals |
front 76 How is Campylobacter transmitted? | back 76 Ingestion of contaminated beverages, food, water, milk, meat, and chicken |
front 77 In a small number of cases of Campylobacter, infection can lead to a serious neuromuscular paralysis called ______________________ | back 77 Guillain-Barre syndrome |
front 78 What is the Guillain-Barre syndrome? | back 78
|
front 79 What is the prevention and treatment of Campylobacter? | back 79
|
front 80 Clostridioides difficile is a gram-________ bacteria and the morphology is ________. | back 80 Clostridioides difficile is a gram-positive, endospore-forming rod |
front 81 True or False: Clostridioides difficile was once considered part of our normal biota (harmless). | back 81 True; It was once considered relatively harmless but now is known to cause a condition called pseudomembranous colitis, also known as antibiotic-associated colitis. |
front 82 How is pseudomembranous colitis caused? | back 82 Pseudomembranous colitis is known as a antibiotic-associated colitis because in many cases, this infection is precipitated by therapy with broad-spectrum antibiotics. --> Major cause of diarrhea |
front 83 Clostridioides difficile is able to superinfect the large intestine when drugs have distrupted the normal biota. It results in the production of two enterotoxins (A and B) which essentially results in... | back 83 necrosis in the wall of the intestine --> in more severe cases the colon is inflamed and gradually sloughs off loose, membranelike patches called pseudomembranes consisting of fibrin and cells --> if not stopped, perforation of the cecum and death can result |
front 84 What is the predominant symptom of Clostridioides difficile? | back 84 Diarrhea (in some severe cases, it can cause abdominal cramps, fever, and leukocytosis) |
front 85 What are some treatments of Clostridioides difficile? | back 85
|
front 86 What is the morphology of vibrio cholerae? | back 86 Curved rod with a single polar flagellum |
front 87 What are some characteristics of vibrio cholerae? | back 87
|
front 88 When are spikes of cholera seen? | back 88 Outbreaks of cholera are expected to happen after natural disasters, war, or large refugee movements |
front 89 What are two types of cholera? | back 89 Class and El Tor |
front 90 Signs and symptoms of Vibrio cholerae include: | back 90
|
front 91 What is the toxin produced by Vibrio cholerae and what role does the toxin play? | back 91 Produces cholera toxin which disrupts the normal physiology of intestinal cells, causing them to shed large amounts of electrolytes into the intestine |
front 92 What are some pathogenesis and virulence factors of Vibrio cholerae? | back 92
|
front 93 What type of environment promotes growth of Vibrio? | back 93 Warm, monsoon, alkaline, and saline conditions |
front 94 Treatment of Vibrio cholerae? | back 94 Oral Rehydration Therapy |
front 95 Who found the use of sari's to help filter out water? | back 95 Rita Cowell helped reduce the amount of cholera in endemic areas, where she helped understand cholera could be found in dormant water and the water can be filtered using sari's. |
front 96 Non-cholera vibrios lack the _____. | back 96 Cholera toxin |
front 97 True or False: It is more common to experience an infection with a non-cholera species of Vibrio than a V. cholerae infection. | back 97 True; These infections are called vibrioses. |
front 98 What are the prominent causative agents of Non-Cholera Vibrio (aka vibriosis)? | back 98 V. vulnificus and V. parahaemolyticus |
front 99 What three factors increase the chance of vibrioses? | back 99
|
front 100 Cryptosporidium is a type of _________. | back 100 Protozoa |
front 101 Describe crytosporidium | back 101
|
front 102 Crytosporidium outbreaks occur in ______. | back 102 Swimming pools |
front 103 What are Rotaviruses? | back 103
|
front 104 How is Rotavirus transmitted? | back 104 Fecal-Oral Route, including contaminated food, water, and fomites |
front 105 How is Rotavirus treated? | back 105
|
front 106 What is the most common food-borne virus in the United States? Why? | back 106 Norovirus; It has a low infectious dose (1 to 20 viruses) |
front 107 What are symptoms of norovirus? | back 107 Profuse, watery diarrhea for 3 to 5 days, vomiting in the early stages, mild fever |
front 108 How is norovirus transmitted? | back 108
|
front 109 What is food poisioning? | back 109
|
front 110 What are the three exotoxins that cause food poisoning? | back 110
|
front 111 This exotoxin that causes food poison is associated with custards, sauces, cream pastries, processed meats, chicken salad, or ham | back 111 Staphylococcus aureus |
front 112 Staphylococcus aureus exotoxin characteristics: | back 112
|
front 113 Bacillus cereus exotoxin is gram-________ bacterium that lives in the _____. | back 113 Bacillus cereus exotoxin is gram-positive bacterium that lives in the soil. |
front 114 Two forms of bacillus cereus exotoxin are: | back 114
|
front 115 Clostridium perfringens exotoxin is also the causative agent of __________. | back 115 Clostridium perfringens exotoxin is also the causative agent of gas gangrene. |
front 116 Describe Clostridium perfringens exotoxin | back 116
|
front 117 What defines chronic diarrhea? | back 117
|
front 118 Enteroaggregative E. Coli (EAEC) | back 118
|
front 119 Cyclospora cayetanensis | back 119
|
front 120 Giardia duodenalis is commonly known as: | back 120
|
front 121 Giardia duodenalis is a __________. | back 121 Protozoa |
front 122 Describe the morphology of Giardia duodenalis | back 122
|
front 123 Signs and symptoms of Giardia duodenalis: | back 123
|
front 124 In Giardia duodenalis, the presence of this protozoa leads to malabsorption of _____ in the digestive tract. | back 124 In Giardia duodenalis, the presence of this protozoa leads to malabsorption of fat in the digestive tract. Usually results in significant weight loss |
front 125 True or False: Giardia duodenalis; Superficial invasion by trophozoites causes damage to the epithelial cells, edema, and infiltration by white bloods, which is irreversible. | back 125 True |
front 126 Where is Giardia isolated from? | back 126
|
front 127 Although trophozoites and cysts escape in the stool, _____ play a greater role in transmission. Why? | back 127 Although trophozoites and cysts escape in the stool, cysts play a greater role in transmission. Giardia cysts can survive for 2 months in environment and are usually ingested with water and food or swallowed after close contact with infected people or contaminated objects. |
front 128 True or False: Giardiasis can easily be diagnosed from feces. | back 128 False; Giardiasis can be difficult to diagnose because the organism is shed in feces only intermittently. |
front 129 Where do outbreaks of Giardia occur? | back 129 Epidemics can be traced to water from mountain streams as well as chlorinated municipal water. |
front 130 True or False: The treatment for Giardia is a vaccine. | back 130 False; No human vaccine is available. Avoiding drinking from freshwater sources is the major preventive measure. The agent is killed by boiling, ozone, and iodine; however, the amount of chlorine used in municipal water supplies does not destroy the cysts. |
front 131 Entamoeba is a _________. | back 131 Entamoeba is an amoeba that are widely distributed in aqueous habitats. |
front 132 The Entamoeba histolytica has a relatively simple life cycle that alternates between ________ that is motile by means of __________ and a _____, ______, nonmotile _______. | back 132 The Entamoeba histolytica has a relatively simple life cycle that alternates between trophozoite that is motile by means of pseudopods and a smaller, compact, nonmotile cyst.
|
front 133 Entamoeba hysolytica | back 133
|
front 134 Intestinal Amoebiasis | back 134
|
front 135 Extraintestinal Amoebiasis | back 135
|
front 136 In general, what is hepatitis? | back 136 Hepatitis is the inflammatory disease of the liver:
|
front 137 Hepatitis A | back 137
|
front 138 Hepatitis B | back 138
|
front 139 Hepatitis C | back 139
|
front 140 ______________ is a hallmark of helminthic infection. | back 140 Eosinophilia is a hallmark of helminthic infection |
front 141 What are some general clinical considerations (pathogenesis and virulence factors) of helminth infections? | back 141
|
front 142 Diagnosis of helminth diseases include: | back 142
|
front 143 What are some prevention and treatment of helminth diseases? | back 143
|
front 144 Describe cycles A and B of basic helminth life and transmission. | back 144  |
front 145 Describe cycles C and D of basic helminth life and transmission. | back 145  |
front 146 The most common worm disease of children in temperate zones is _______________. | back 146 Enterobius vermicularis |
front 147 Enterobius vermicularis is a _______ disease. | back 147 Pinworm |
front 148 Enterobius vermicularis is a life cycle ___ type. | back 148 Enterobius vermicularis is a life cycle A type. |
front 149 The hallmark of Enterobius vermicularis is ____________. | back 149 The hallmark of Enterobius vermicularis is anal itching |
front 150 Is the Enterobius vermicularis fatal? | back 150 The infection is not fatal and most cases are asymptomatic. When one member of the family is diagnosed, the entire family should be tested and/or treated because it is likely that multiple members are infected. |
front 151 Trichuris trichuria is ________ and is life cycle ________. | back 151 Trichuris trichuria is whipworm and is life cycle A. |
front 152 In the Trichuris trichuria, _____ are the sole host. | back 152 In the Trichuris trichuria, humans are the sole host. |
front 153 Where is the highest incidence of Trichuris trichuria? | back 153 In the tropics and subtropics that have poor sanitation |
front 154 In Trichuris trichuria, females lay _______ to ______ eggs daily in the bowel. | back 154 3,000 to 5,000 |
front 155 What are symptoms of Trichuris trichuria? | back 155
|
front 156 Diphyllobothrium latum is a _______ disease in which _____ are definitive host and ____ are intermediate host. | back 156 Diphyllobothrium latum is a tapeworm disease in which humans are definitive host and fish are intermediate host.
|
front 157 Hymenolepsis species includes ____ ______ and its life cycle is _____. There are two species _______ ____ and ______ ______. | back 157 Hymenolepsis species includes small tapeworms and its life cycle is C. There are two species Hymenolepis nana and Hymenolepsis diminuta.
|
front 158 Taenia solium causes ___________ | back 158 Cysticerosis |
front 159 Taenia solium is a ______. | back 159 Tapeworm |
front 160 Cysticercosis occurs when... | back 160 Cysticercosis occurs when humans ingest tapeworm eggs rather than infected meat |
front 161 What is the life cycle of Taenia solium? | back 161 Life Cycle C |
front 162 Where is Taenia solium distributed? | back 162 Distributed worldwide, but concentrated in areas where humans live in close proximity with pigs or eat undercooked pork |
front 163 Fasciola heptica is a ____ ____ common in sheep, cattle, goats, and other mammals. | back 163 Liver fluke |
front 164 Symptoms of Fasciola hepatica | back 164 vomiting, diarrhea, hepatomegaly, and bile obstruction if infected with a large number of flukes |
front 165 Who is the definitive host of Fasciola hepatica? | back 165 Mammals |
front 166 Liver and intestinal disease is caused by... | back 166 Fasciola hepatica |
front 167 Schistosomiasis is a _______ disease | back 167 Liver |
front 168 The causative organism of Schistosomiasis is... | back 168 Schistosoma masoni and S. japonicum |
front 169 Schistosoma masoni and S. japonicum similarities: | back 169
|
front 170 Signs and Symptoms of Schistomiasis | back 170
|
front 171 Pathogenesis, Diagnosis of Schistosomiasis | back 171
|
front 172 Life Cycle of Schistosoma is ___ | back 172 D |
front 173 Streptococcus mutans | back 173
|
front 174 Helicobacter pylori | back 174
|
front 175 Clostridium perfringen | back 175
|
front 176 Hepatitis A | back 176
|
front 177 Hepatitis B | back 177
|
front 178 Hepatitis C | back 178
|
front 179 Schistosomas | back 179
|
front 180 Rotavirus | back 180
|
front 181 Mumps virus | back 181
|
front 182 Giardia duodenalis | back 182
|
front 183 Enterobius vermicularis | back 183
|
front 184 Taenia solium | back 184
|
front 185 Fasciola hepatica | back 185
|
front 186 Salmonella | back 186
|
front 187 Shigella | back 187
|
front 188 Shiga toxin-producing E. Coli | back 188
|
front 189 Other E. coli | back 189
|
front 190 Campylobacter | back 190
|
front 191 Clostridioides difficile | back 191
|
front 192 Vibrio cholerae | back 192
|
front 193 Non-cholera Vibrio species | back 193
|
front 194 Cryptosporidium | back 194
|
front 195 Rotavirus | back 195
|
front 196 Norovirus | back 196
|
front 197 Staphylcoccus aureus | back 197
|
front 198 Bacillus cereus exotoxin | back 198
|
front 199 Clostridium perfringens exotoxin | back 199
|