Which branch of the Autonomic Nervous System innervates blood vessels? Which layers of the blood vessel wall do these nerves innervates? What are effectors (cells that carry out the response)?
Smooth muscle is regulated by sympathetic vasomotor nerve fibers of the autonomic nervous system. These nerves innervate the tunica media. The effectors are smooth muscle cells
When vascular smooth muscle contracts, what happens to the diameter of the blood vessel? What is this called?
When smooth muscle contract there is a reduction in lumen diameter, this is called vasoconstriction.
Name the type of artery that matches each description:
(a)major role in dampening the pulsatile pressure of heart contractions
(b)vasodilation or constriction to determine blood flow to individual capillary beds
(c)have the thickest tunica media relative to their lumen size
(a)elastic arteries - major role in dampening the pulsatile pressure of heart contractions
(b)arterioles - vasodilation or constriction to determine blood flow to individual capillary beds
(c)muscular arteries - have the thickest tunica media relative to their lumen size
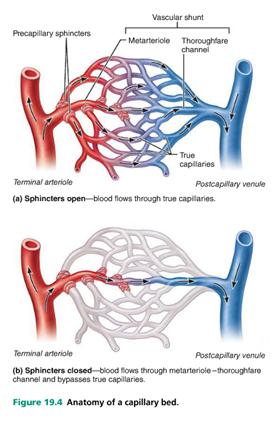
Look at figure 19.4 and assume that the capillary bed depicted is in your calf muscle.
Which condition (a) or (b) – would the bed be in if you were doing calf raises at the gym?
Capillary bed A
(a) What is the function of valves in veins?
(b) What forms the valves?
a) Valves prevent blood from flowing backwards
b) Valves are formed from folds of the tunica intima
In the systemic circuit, which contains more blood-arteries or veins- or is it the same?
Veins contain more blood than arteries. At any given time there is 60% of the body’s blood in the veins
List 3 factors that determine resistance in a vessel?
Which of these factors is physiologically most important?
blood viscosity, vessel length, and vessel diameter, Vessel diameter is most important
blood viscosity
vessel length
vessel diameter
Vessel diameter is most important
Suppose vasoconstriction decreases the diameter of a vessel to one-third its size. What happens to the rate of flow through that vessel?
Calculate the expected size of the change.
The rate of flow would decrease 81-fold from its original flow. (3X3x3x3=27)
Describe the baroreceptor reflex changes that occur to maintain blood pressure when you rise from a lying-down to a standing position.
When you stand up, the baroreceptors will sense a drop in your blood pressure. They quickly take action to make sure that blood continues to flow to the brain, kidneys, and other important organs. The baroreceptors cause the heart to beat faster and harder. They also cause the small arteries (arterioles) and veins to narrow.
The kidneys play an important role in maintaining MAP by influencing which variable?
Explain how renal artery obstruction could cause secondary hypertension.
The kidneys play an important role by influencing blood volume.
The blood pressure in the kidneys is lower than the rest of the body. This triggers direct and indirect renal mechanisms to increase blood pressure by increasing blood volume.
Suppose you are in a bicycle race.
What happens to the smooth muscle in the arterioles supplying your leg muscles?
What is the key mechanism in this case?
The smooth muscle relaxes, dilating the vessels and supplying more oxygen and nutrients to the exercising muscles.
The key is autoregulation by intrinsic metabolic controls
If many arterioles in your body dilated at once, you would expect MAP to plummet. What prevents MAP from decreasing during your bicycle race?
Extrinsic mechanisms, primarily the SNS, and cardiac output increases
Suppose OPif rises dramatically - say because of a serious bacterial infection in the surrounding tissue.
(a) Predict how fluid flow will change in this situation.
(b) Now calculate the NFP at the venous end of the capillary in figure 19.17 if OPif increases to 10mm Hg.
(c) in which direction does fluid flow at the venous end of the capillary now – in or out?
a) an increase in interstial fluid osmotic pressure would pull more fluid from the capillaries causing edema
b) an in crease in osmotic pressure to 10mg would increase the outward pressure on both, arterial and venous (1mm Hg) ends
c) Fluid would flow out of the venous end of the capillary rather than in.
Your neighbor, Bob, calls you because he thinks he is having an allergic reaction to a medication. You find Bob on the verge of losing consciencness and having trouble breathing. When paramedics arrive, they note his blood pressure is 63/38 and he has a rapid, theady pulse.
Explain Bob’s low blood pressure and rapid heart rate.
Bob is suffering from anaphylactic shock due to an allergic reaction to his medication. His blood pressure is low because of widespread vasodilation triggered by the massive release of histamine. His rapid heart rate is a result of the baroreceptor reflex triggered by his low blood pressure. This activates his sympathetic nervous system, increasing heart rate, in an attempt to raise his blood pressure.
Which paired artery supplies most of the tissues of the head except for the brain and orbits?
the external carotid arteries supplies most of the tissue of the head.
Name the arterial anastomosis at the base of the cerebrum?
the cerebral arterial circle, aka the circle of willis
Name the four unpaired arteries that emerge from the abdominal aorta.
celiac trunk
superior mesenteric arteries
inferior mesenteric arteries
and the median sacral artery
You are assessing the circulation in the leg of a diabetic patient at the clinic. Name the artery you palpitate in each of these three locations.
Behind the knee,
behind the medial malleolus of the tibia,
on the dorsum of the foot.
In what important way does the area drained by the vertebral veins differ from the area served by the vertebral arteries?
The vertebral arteries supply the brain with oxygenated blood but the vertebral veins do not drain much of the deoxygenated blood from the brain.
Which veins drain the dural venous sinuses and where do these veins terminate?
the internal jugular veins, each internal jugular vein joins a subclavian vein to form a brachiocephalic vein
What is a portal system?
What is the function of the hepatic portal system?
a system where two capillary beds occur in series
to transport venous blood from the digestive organs to the liver for processing before it enters the rest of the systemic circulation
Name the leg veins that often become varicosed?
The great and small saphenous veins
List three differences between systemic arteries and veins with respect to their general pathways and courses?
arteries run deep, veins run deep and superficial
venous pathways are more interconnected than arterial pathways, the brain and digestive systems have unique venous drainage systems
the arterial drainage system is not different
Name three fetal shunts that are occludes shortly after birth. Which structures does each shunt bypass?
The foramen ovale and the ductus arteriosus both bypass the fetal lungs. The ductus venosus bypasses the liver
Name three common age-related vascular problems?
varicose veins
atherosclerosis
hypertension
