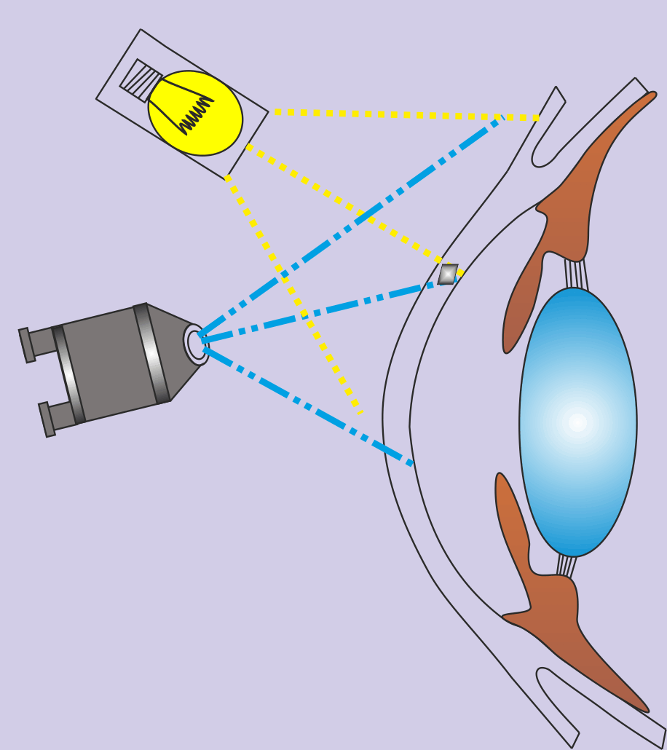
Diffuse Illumination
A wide beam of light is directed obliquely at the cornea with no attempt to focus the light. Low magnification, low illumination is used. It provides a good over all picture of the cornea but no fine details can be seen. It is used primarily for a general survey of the eye.
Uses:
- To assess the lids, lacrimal, and lashes
- to help assess contact lens fit (TBUT)
When observing the break up of fluorescein on the cornea, it is best to use the widest, most diffuse illumination to encompass as much of the cornea as possible.
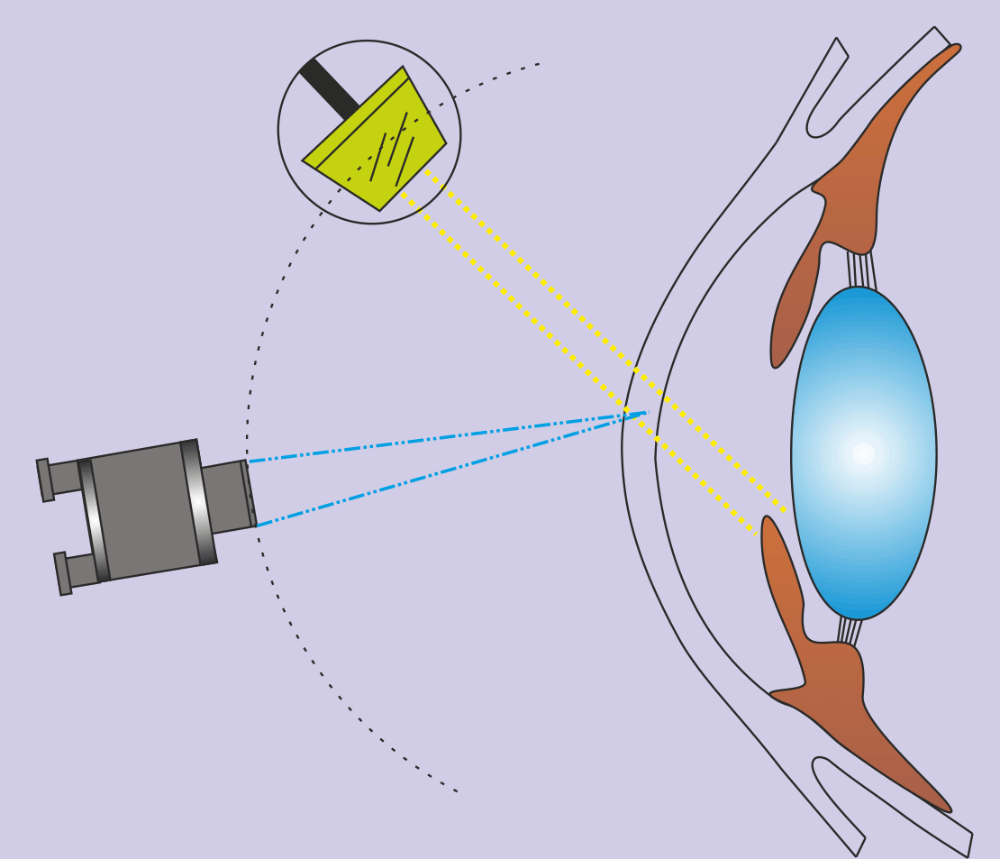
Direct Focal Illumination
The microscope and the beam of light are focused on the same area.
There are three types of direct focal illumination:
1) optic
section,
2) parallelepiped
3) conical beam.
Optic section is used to see all layers of the cornea. With it,
is possible to determine distortions in the corneal contour
(thickness/thinness) and the depth of foreign bodies or opacities in
the cornea.
Parallelepiped is the most common type of direct illumination. It provides a broader view of the anterior and posterior corneal surfaces. It is used to help assess any surface irregularities which may exist. It is used to assess the extent of a corneal scar or infiltration can be observed along with the presence of folds or striae in Descemet's membrane. It is often used with fluorescein in helping to determine the fit of a contact lens.
Conical Beam is the most sensitive method for observing flare or relucency in normal aqueous humor in the anterior chamber. A small round or square beam of light is used to asses the status of the anterior chamber by oscillating between the cornea and the lens. Using high magnification it resembles light penetrating fog.
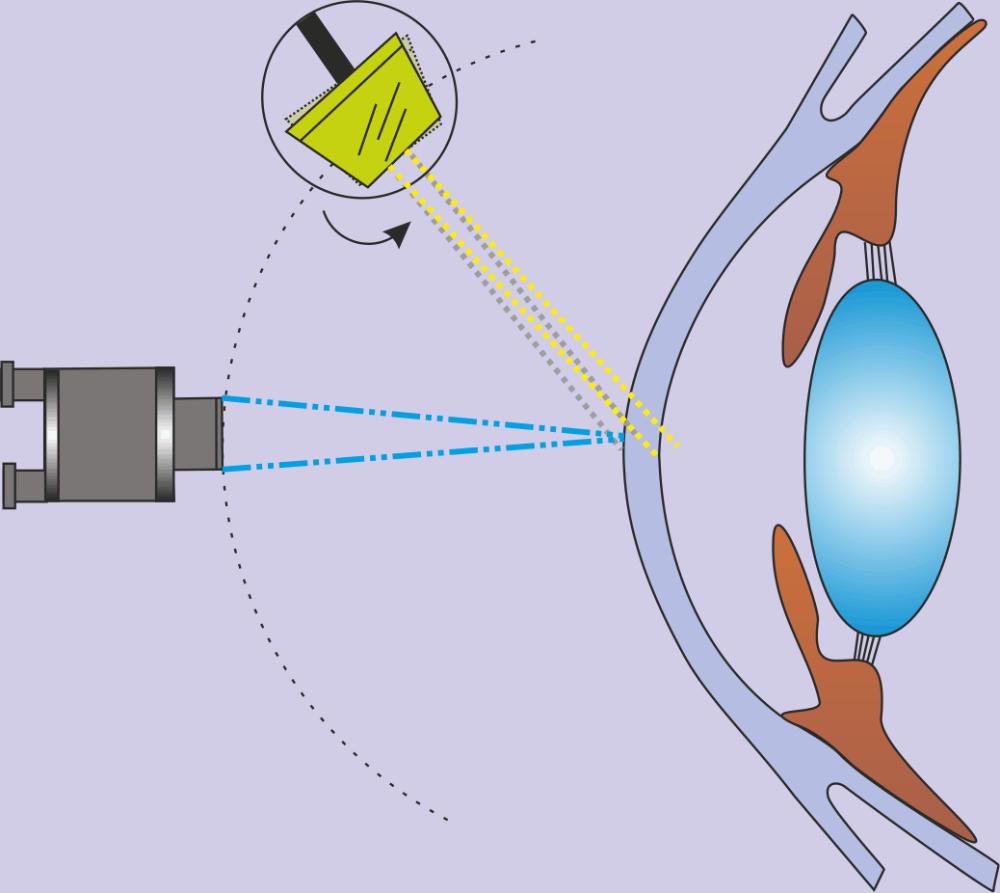
Indirect Illumination
The observer focuses the microscope on an area immediately adjacent to the illuminated position. It is particularly valuable for studying the iris for pathology.
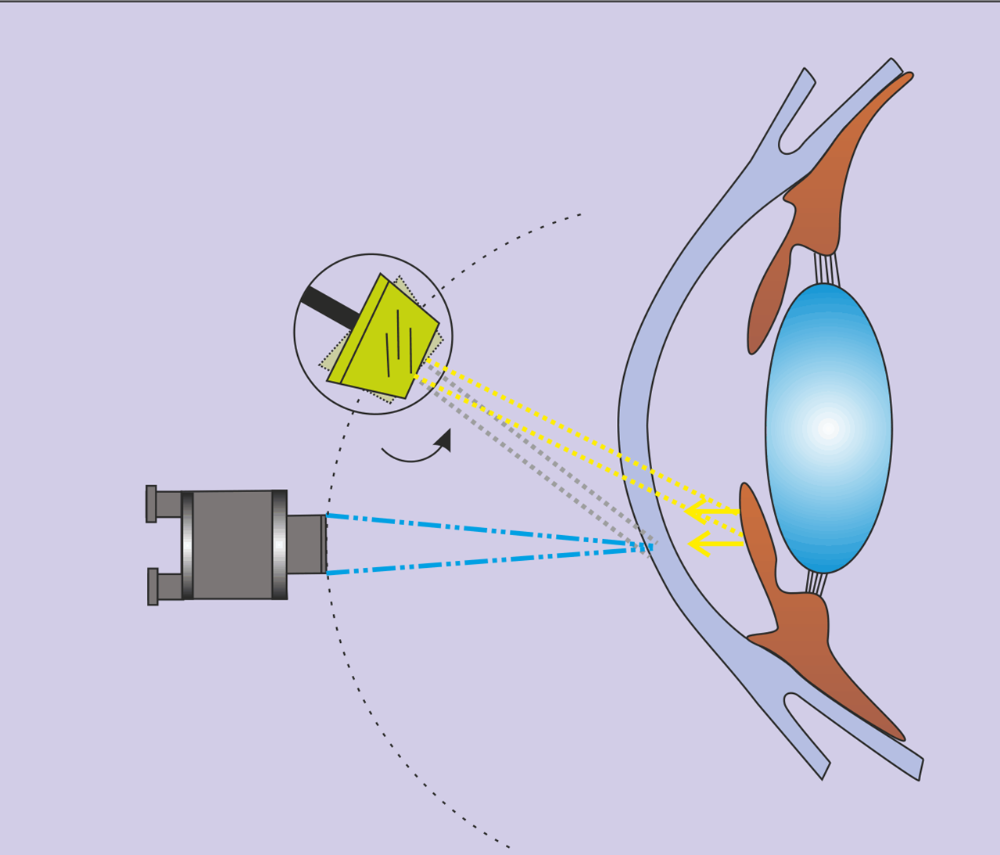
Retro Illumination
The light is focused on the deeper structures such as the iris, lens or retina while the microscope is focused to study the more anterior structures in the reflected light. Most typically, the light is reflected from the iris in order to study the cornea. It can be useful for the examination of corneal edema and to view blood vessels that have invaded the cornea. It can also be used to study deposits on Descemet’s membrane.
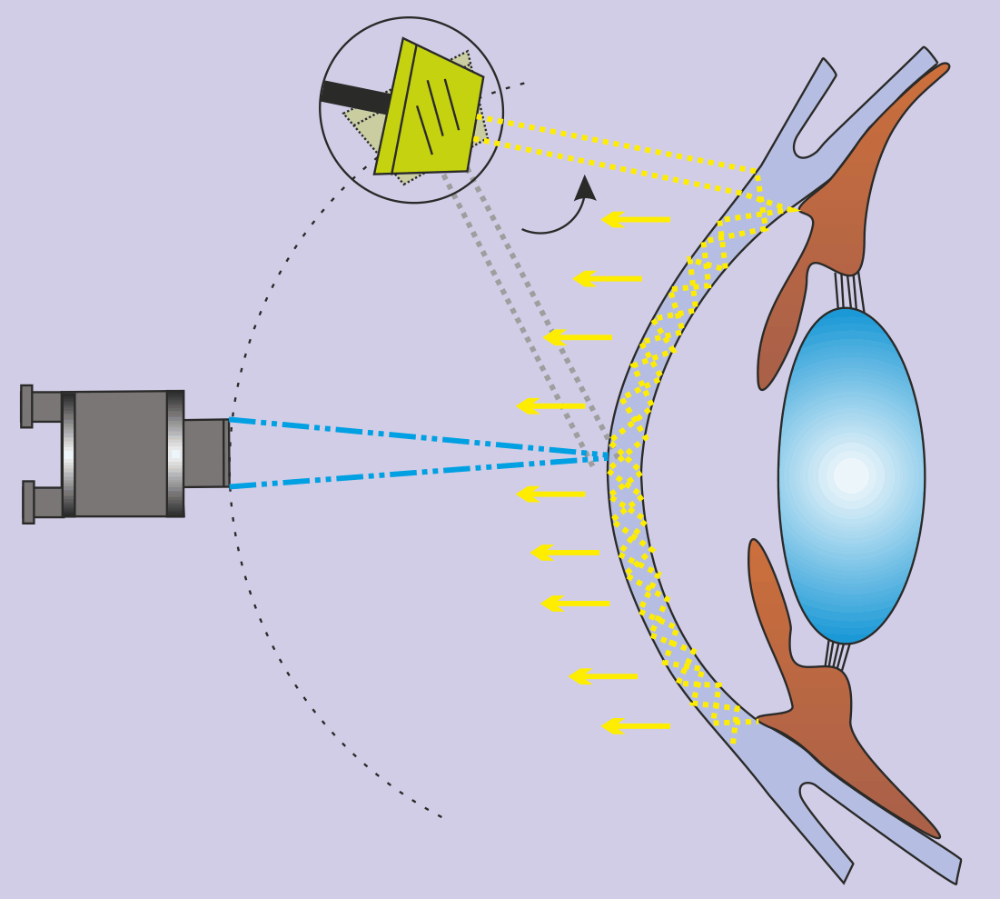
Sclerotic Scatter
A broad beam of light is focused at the temporal limbus so it transilluminates through to the nasal limbus. The microscope is then focused sharply on the cornea. Sclerotic scatter and the unaided eye is used to detect the presence of corneal edema which appears as a foggy patch of cotton. The angle between the slit lamp beam and the eye is typically 40-60 degrees, but can be greater. In the case of gross corneal edema, a green filter may be applied along with high magnification.
Specular reflection
Accomplished by aligning the microscope along the angle of reflection, which splits the patient's gaze splits in half
Uses:
- best for viewing the endothelium
- to see the surface of the crystalline lens, hazy lenses, epithelial edema
Cobalt Blue Filter
A cobalt blue filter is often used after the instillation of fluorescein to observe staining patterns and lens fit.
White Filter
Used to decrease ultraviolet rays and minimally decrease light intensity. It is used primarily for routine examination.
Neutral Density Filter
Decreases light intensity about 10%. Used to examine eyelids and conjunctiva. Useful for photophobic patients.
Green Filter (red free)
Makes red or brown objects blacker. Useful for observing blood vessels.