graphical user interface
A type of software that provides a front-end structure/interface that presents information in a familiar format leading to a natural style of interaction through the use of icons and a mouse
interoperability
the ability to transfer data from one system to another system
data mart
a subset of the data warehouse that is usually oriented to a specific business line or team (smaller database)
clinical data repository
is a real time database that consolidates data from a variety of clinicalsources to present a unified view of a single patient
executive information system
a type of management information systemthat facilitates and supports senior executive information and decision-making needs
business continuity plan
a plan to help ensure that business processes can continue during a time of emergency or disaster
database that stores the data in tables
relational
how to handle versioning of documents in the EDMS
Display the second version but identify that a previous version exists
probabilistic algorithm
The comparison methodology that identifies multiple records that represent the same person
use cases
a series of related interactions between a user and a system that enables the user to achieve a goal
database that must be able to store video, images, and audio
relational
DICOM
Digital Imaging and Communications in Medicine
Digital Imaging and Communications in Medicine (DICOM)
a standard for handling, storing, printing, and transmitting information in medical imaging
HL7 EHR functional model
provides Healthcare service providers and IT providers a standardized reference list and model of functions to be present in an Electronic Health Record System
incidental disclosure
a secondary use or disclosure that cannot reasonably be prevented, is limited in nature, and that occurs as a result of another use ordisclosure that is permitted by the Rule
privacy incident
A (reportable) breach is the unauthorized acquisition, access, use, or disclosure of PHI in a manner not permitted by law or regulation and which compromises the security and privacy of the PHI
How long must the training records for the HIPAA privacy training be kept before destruction?
7 years
spoliation
negligent, reckless, and intentional destruction of evidence
workforce clearance procedure
ensures that the access to the ePHI is appropriate (Before an employee can be given access to the EHR, someone has to determine what they have access to)
degaussing
To neutralize or rebalance the magnetic field of a magnetized object, such as a computer monitor or the read/write head of a disk drive or tape recorder
Physical safeguards include
tools to control access to computer systems and fire protection
denial of service
an interruption in an authorized user's access to a computer network, typically one caused with malicious intent
spyware
software that enables a user to obtain covert information about another's computer activities by transmitting data covertly from their hard drive
phishing
the activity of defrauding an online account holder of financial information by posing as a legitimate company
virus (worm, Trojan Horse)
a piece of code that is capable of copying itself and typically has a detrimental effect, such as corrupting the system or destroying data
malware
software that is intended to damage or disable computers and computer systems
minimum necessary rule
requires that department of mental health, its offices, facilities, programs and Workforce Members, when using, disclosing, or requesting PHI, must make reasonable efforts to limit PHI to the minimum amount necessary to accomplish the intended purpose of the use, disclosure or request
limited data set
may be disclosed to an outside party without a patient’s authorization if certain conditions are met
intrusion detection
a device or software application that monitors network or system activities for malicious activities or policy violations and produces electronic reports to a management station
why would you are conduct a risk assessment?
to prevent breach of confidentiality
CAPTCHA
a program or system intended to distinguish human from machine input, typically as a way of thwarting spam and automated extraction of data from websites
A certification agency validates the use of encryption between two organization's websites. How?
hypertext markup language
digital certificate
an electronic document used to prove ownership of a public key
The HIPAA security rule impacts
clinical data repository
The security rule only applies to
e-PHI
The three components of a security program
protecting the privacy of data
ensuring the integrity of data
ensuring the availability of data
security token
a small hardware device that the owner carries to authorize access to a network service. The device may be in the form of a smart card or may be embedded in a commonly used object such as a key fob
What would be an example of two-factor authentication?
password and token
A covered entity includes
health care providers who perform specified actions electronically
covered entities
(1) health plans, (2) health care clearinghouses, and (3) health care providers who electronically transmit any health information in connection with transactions for which HHS has adopted standards.
information system activity review
procedures to regularly review records of information of system activity, such as audit logs, access reports, and security incident tracking reports
What type of digital signature uses encryption?
digital signature
Breach notification is required unless
the probability of PHI being compromised is low
You have been assigned the responsibility of performing an audit to confirm that all of the workforce's access is appropriate for their role in the organization. This process is called
workforce clearance procedure
SWOT analysis
a study undertaken by an organization to identify its internal strengths and weaknesses, as well as its external opportunities and threats
Electronic protected health information (ePHI)
any protected health information that is covered under HIPAA security regulations and is produced, saved, transferred or received in an electronic form
cracker
an individual with extensive computer knowledge whose purpose is to breach or bypass internet security or gain access to software without paying royalties. The general view is that, while hackers build things, crackers break things.
SSL (Secure Sockets Layer)
the standard security technology for establishing an encrypted link between a web server and a browser
CCOW )Clinical Context Object Workgroup)
an Health Level Seven International standard protocol designed to enable disparate applications to synchronize in real time, and at the user-interface level
packet filter
a firewall technique used to control network access by monitoring outgoing and incoming packets and allowing them to pass or halt based on the source and destination Internet Protocol (IP) addresses, protocols and ports
To prevent their network from going down, a company has duplicated much of its hardware and cables. This duplication is called
redundancy
All patients except ______________ must be given a notice of privacy practices.
inmates
Who/which entity would the Privacy Act of 1974 apply to?
the federal government
an example of an administrative safeguard would include
training
what is the timeframe the facility must provide to a patient who has asked to view his medical record?
30 days
private key encryption
A private key is a tiny bit of code that is paired with a public key to set off algorithms for text encryption and decryption.
Public encryption uses a private and public key
You are reviewing your privacy and security policies, procedures, training program, and so on, and comparing them to the HIPAA and ARRA regulations. You are conducting a
risk assessment
Intrusion detection systems analyze
network traffic
Someone accessed the covered entity's electronic health record and sold the information that was accessed. This person is known as
a cracker
Before we can go any further with our risk analysis, we need to determine what systems/information need to be protected. This step is known as
system characterization
The hospital has received a request for an amendment. How long does the facility have in order to accept or deny the request?
60 days
Average daily census includes
adult and pediatrics, but NOT newborns
relative risk (formula)
RR = risk exposed divided by risk not exposed
The primary difference between an experimental (randomized) clinical trial and other observational study designs is that in an experimental trial, the
investigator determines who is and who is not exposed
sequence organizations use when collecting statistics to increase their knowledge
data → information → facts → knowledge
variable sampling
The process of predicting a given variable of a population through sampling.
convenience sampling
is made up of people who are easy to reach
stratified sampling
the researcher divides the population into separate groups, called strata. Then, a probability sample (often a simple random sample ) is drawn from each group.
systematic sampling
a type of probability sampling method in which sample members from a larger population are selected according to a random starting point and a fixed, periodic interval
A distribution is said to be positively skewed when the mean is
shifted to the right
interrater reliability
the degree of agreement among raters. It gives a score of how much homogeneity, or consensus, there is in the ratings given by judges.
When very long length of stay is calculated in the average length of stay, this will
result in a special cause variation in the average length of stay
common cause variation
fluctuation caused by unknown factors resulting in a steady but random distribution of output around the average of the data
special cause variation
a shift in output caused by a specific factor such as environmental conditions or process input parameters. It can be accounted for directly and potentially removed and is a measure of process control
case-control study model
A study that compares patients who have a disease or outcome of interest (cases) with patients who do not have the disease or outcome (controls), and looks back retrospectively to compare how frequently the exposure to a risk factor is present in each group to determine the relationship between the risk factor and the disease.
prospective studies
watches for outcomes, such as the development of a disease, during the study period and relates this to other factors such as suspected risk or protection factor(s). The study usually involves taking a cohort of subjects and watching them over a long period.
elements of negligence must be present in order to recover damages
duty of care; breach of duty of care; suffered an injury; defendant's conduct caused the plaintiff harm
Spoliation addresses what method of discovery?
e-discovery
What would be considered "best practice" for handling fax transmission of a physician's orders?
Treat faxed orders like verbal orders and require authentication of the orders by appropriate medical staff within the required period
One of the greatest threats to the confidentiality of health data is
disclosure of information for purposes not authorized in writing by the patient
A written consent from the patient is required from this entity in order to learn a patient's HIV status
insurance companies
In this type of facility the Privacy Act of 1974 permit patients to request amendments to their medical record
Department of Defense health care facility
slander
The action or crime of making a false spoken statement damaging to a person's reputation; make false and damaging statements about someone
defamation
the action of damaging the good reputation of someone; slander or libel
libel
a published false statement that is damaging to a person's reputation; a written defamation
perjury
the offense of willfully telling an untruth in a court after having taken an oath or affirmation
The legislation that required all federally funded facilities to inform patients of their rights under state law to accept or refuse medical treatment is known as
Patient Self-Determination Act
To be admitted into court as evidence, medical records or health information are introduced as
business records or exception to hearsay rule
The doctrine that the decisions of the court should stand as precedents for future guidance is
stare decisis
Who determines the retention period for health records?
state and federal governments
What health care system has to comply with the requirements of the Freedom of Information Act?
veterans' hospitals
When a health care facility fails to investigate the qualifications of a physician hired to work as an independent contractor in the emergency room and is accused of negligence, the health care facility can be held liable under
corporate negligence
corporate negligence
the legal doctrine that holds health-care facilities, such as hospitals, nursing homes and medical clinics, responsible for the well-being of patients
contributory negligence
failure of an injured plaintiff to act prudently, considered to be a contributory factor in the injury suffered, and sometimes reducing the amount recovered from the defendant
respondeat superior
"let the master answer"
a US legal doctrine which states that, in many circumstances, an employer is responsible for the actions of employees performed within the course of their employment.
general negligence
a failure to exercise the care that a reasonably prudent person would exercise in like circumstances
tort
a wrongful act or an infringement of a right (other than under contract) leading to civil legal liability
A valid authorization for the disclosure of health information should not be
dated prior to discharge of the patient
Which type of law is constituted by rules and principles determined by legislative bodies?
statutory law
statutory law
the term used to define written laws, usually enacted by a legislative body
case law
the law as established by the outcome of former cases
common law
the part of law that is derived from custom and judicial precedent rather than statutes
administrative law
the body of law that regulates the operation and procedures of government agencies
The Darling v. Charleston Community Memorial Hospital case established the this doctrine for hospitals to observe and changed the way hospitals dealt with liability.
doctrine of corporate negligence
In what circumstance would a release of information without the patient's authorization be permissible?
release to state workers' compensation agencies
HIM professionals have a duty to maintain health information that complies with
federal statutes, state statutes, and accreditation standards
Courts have released adoption records based on
a court order for good cause
The minimum record retention period for patients who are minors is
age of majority plus the statute of limitations
Hospitals that destroy their own medical records must have a policy that
ensures records are destroyed and confidentiality is protected
The premise that charitable institutions could be held blameless for their negligent acts is known as
doctrine of charitable immunity
Substance abuse records cannot be redisclosed by a receiving facility to another health care facility unless the
patient gives written consent
What legal requirement would compel you to produce the original record for the court?
best evidence rule
best evidence rule
a legal principle that holds an original copy of a document as superior evidence
constitutional law
refers to rights carved out in the federal and state constitutions
The body of law founded on custom, natural justice and reason, and sanctioned by usage and judicial decision is known as
common law
doctrine of res ipsa loquitur
a doctrine that infers negligence from the very nature of an accident or injury, in the absence of direct evidence on how any defendant behaved
Under the RBRVS, each HCPCS/CPT code contains three components, each having assigned relative value units. These three components are
physician work, practice expense, and malpractice insurance expense
The category “Commercial payers” includes private health information and
employer-based group health insurers
Under APCs, payment status indicator "V" means
clinic or emergency department visit (medical visits)
What would be considered "technical" components?
radiologic technicians, radiological equipment, and radiological supplies.
Currently, which prospective payment system is used to determine the payment to the "physician" for physician services covered under Medicare Part B, such as outpatient surgery performed on a Medicare patient?
APCs
This is the amount the facility actually bills for the services it provides.
charges
lifetime reserve days
Original Medicare covers up to 90 days in a hospital per benefit period and offers an additional 60 days of coverage with a high coinsurance. These 60 reserve days can be used only once during your lifetime but do not have to be applied towards the same hospital stay.
The Health Insurance Portability and Accountability Act (HIPAA) requires the retention of health insurance claims and accounting records for a minimum of ____ years, unless state law specifies a longer period.
six
These are assigned to every HCPCS/CPT code under the Medicare hospital outpatient prospective payment system to identify how the service or procedure described by the code would be paid.
payment status indicator
This best describes the situation of a provider who agrees to accept assignment for Medicare Part B services
The provider cannot bill the patients for the balance between the MPFS amount and the total charges
This is the difference between what is charged and what is paid.
contractual allowance`
the OIG's Workplan
This document is published by the Office of Inspector General (OIG) every year. It details the OIG's focus for Medicare fraud and abuse for that year. It gives health care providers an indication of general and specific areas that are targeted for review. It can be found on the Internet on CMS's Web site.
Medicare Physician Fee Schedule (MPFS)
This prospective payment system replaced the Medicare physician payment system of "customary, prevailing, and reasonable (CPR)" charges whereby physicians were reimbursed according to their historical record of the charge for the provision of each service.
In 1987, OBRA helped shift the focus in long-term care to patient outcomes. As a result, core assessment data elements are collected on each SNF resident as defined in the
MDS
OBRA mandates
comprehensive functional assessments of long-term care residents using the Minimum Data Set for Long-Term Care
When health care providers are found guilty under any of the civil false claims statutes, the Office of Inspector General is responsible for negotiating these settlements and the provider is placed under a
Corporate Integrity Agreement
Corporate Integrity Agreement (CIA)
an enforcement tool used by the Office of the Inspector General (OIG) within the Department of Health and Human Services (HHS), to improve the quality of health care and to promote compliance to health care regulations
You want to construct a data display for a frequency distribution. You will use a
frequency polygon or histogram
patient encounter
All cases where the EP and the patient have an actual physical encounter with the patient in which they render any service to the patient should be included in the denominator as seen by the EP.
analytic study design
groups of subjects are compared in order to estimate the magnitude of association between exposures and outcomes
descriptive study
Any study that is not truly experimental
The best form/graph for demonstrating trends over time would be
line graph
If a constant is added to all measurements within a sample
the standard deviation remains the same
A researcher has repeated the same study 10 times. Each time the study is repeated, the p value decreases. As the p value approaches zero, the
chance that the results are due to a sampling error decreases
empiricism
the theory that all knowledge is derived from sense-experience
inductive reasoning
a logical process in which multiple premises, all believed true or found true most of the time, are combined to obtain a specific conclusion, is often used in applications that involve prediction, forecasting, or behavior.
deductive reasoning
a logical process in which a conclusion is based on the concordance of multiple premises that are generally assumed to be true, is sometimes referred to as top-down logic.
The name given to the error committed when the null hypothesis is rejected and it is actually true is
type I error
type I error
the incorrect rejection of a true null hypothesis (a "false positive")
type II error
the failure to reject a false null hypothesis (a "false negative")
null hypothesis
(in a statistical test) the hypothesis that there is no significant difference between specified populations, any observed difference being due to sampling or experimental error
alternative hypothesis
the hypothesis to be accepted if the null hypothesis is rejected
selection bias
the selection of individuals, groups or data for analysis in such a way that proper randomization is not achieved, thereby ensuring that the sample obtained is not representative of the population intended to be analyzed.
Given a positively skewed frequency distribution
larger frequencies are concentrated at the low end of the variable
central tendency
the degree of clustering of the values of a statistical distribution that is usually measured by the arithmetic mean, mode, or median.
You have made a list of the advantages and disadvantages of a measure of central tendency.
The measure of central tendency you are describing is the
mode
Measurements within sample A are assumed to be more variable than measurements within sample B when
individuals within sample A differ more from one another than individuals within sample B
descriptive stats
a set of brief descriptive coefficients that summarizes a given data set, which can either be a representation of the entire population or a sample
T test
a statistical examination of two population means. examines whether two samples are different and is commonly used when the variances of two normal distributions are unknown and when an experiment uses a small sample size.
ANOVA
analysis of variance, a statistical method in which the variation in a set of observations is divided into distinct components
gross (hospital) death rate
total inpatient deaths x 100/total discharges = % death rate
Fetal deaths and outpatient deaths are not included in this calculation.
the direct method, bed turnover
adult and peds discharges/total adult and peds beds = % turnover
Twelve new cases of a certain disease occurred during the month of August. If 4,000 persons were at risk during August, then the
incidence was 3 per 1,000 persons
prevalence
the fact or condition of being prevalent; commonness
incidence
the occurrence, rate, or frequency of a disease, crime, or something else undesirable
Multiple births are _____ delivery
one
fetal deaths are counted as
deliveries
According to current theory in the quality management field, should concurrent data collection or retrospective data collection be utilized?
Concurrent and retrospective data collection methods are both necessary in order to effect meaningful interventions and contain costs.
The person or group who is overall responsible and accountable for maintaining the quality and safety of patient care is the
Board of Directors (BOD) or governing body
type of review in which a physician's record is reviewed by his or her professional colleagues
peer review
What is the best tool for differentiating between common cause variation and special cause variation?
control chart
To properly implement performance improvement (PI), organizations should ensure that all employees participate in an integrated, continuous PI program. This is known as ______.
shared leadership
Which quality management theorist focused on zero defects as the goal of performance improvement efforts?
Crosby
The U.S. federal government's CMS substitutes compliance of its Conditions of Participation requirements to hospitals that already have accreditation awarded by various other agencies that include the Joint Commission, CARF, AOA, or AAAHC. This is known as
deemed status
The FOCUS PDCA model used in performance improvement is best known for its change strategy technique of
Plan, Do, Study, Act
UCL (upper control limit)
A value that indicates the highest level of quality acceptable for a product or service.
What criterion is critical in selecting performance indicators for a health information management department?
The indicators must include the most important aspects of performance
affinity diagram
a tool that gathers large amounts of language data (ideas, opinions, issues) and organizes them into groupings based on their natural relationships (Viewgraph 1). The Affinity process is often used to group ideas generated by Brainstorming.
flowchart
a diagram of the sequence of movements or actions of people or things involved in a complex system or activity
What quality indicator would identify improvement needs in hospital electronic transmission of health care claims and remittances to allow interoperability with ICD-10 codes?
an increase in 5010 rejections
5010 rejections
HIPAA form/rejections
Your hospital is required by the Joint Commission and CMS to participate in national benchmarking on specific disease entities for quality of care measurement. This required collection and reporting of disease-specific data is considered
a series of core measures
core measures
standardized best practices designed to improve patient care
clinical pertinence review
a retrospective review of patient medical records to ensure proper documentation
The Recovery Audit Contractor (RAC) program was developed to identify and reduce improper payments for
Medicare claims
What feature is a trademark of an effective PI program?
a continuous cycle of improvement projects over time
The type of indicator about the placement and number of fire extinguishers would be a(n)
structure
The manager of the utilization review department wants to monitor and evaluate the prevention of inappropriate admissions. When would the manager need to collect data?
prospective review
When the policy and procedures manual no longer reflect current practices, it creates a situation that becomes a risk management issue because
policy and procedures should represent the normal course of business
If administrators of a home health agency wanted to measure the outcomes of adult patients receiving their agency's services, which tool would they use?
OASIS
Which data bank is a result of HIPAA legislation?
Health Care Integrity and Protection Data Bank
The responsibility for performing quality monitoring and evaluation activities in a departmentalized hospital is delegated to the
clinical chairpersons of medical staff committees or ancillary department directors
Most acute care facilities use this type of screening criteria for utilization review purposes to determine the need for inpatient services and justification for continued stay
severity of illness/intensity of service criteria (SI/IS)
The quality review process of invasive and noninvasive procedures to ensure performance of appropriate procedure, preparation of patient, monitoring and postoperative care, and education of patient describes
surgical review
nominal group technique
a group process involving problem identification, solution generation, and decision making
Which quality management theorist believed that merit raises, formal evaluations, and quotas established through benchmarking hinder worker productivity and growth?
W. Edwards Deming
What quality indicator would identify improvement needs in hospital electronic transmission of health care claims and remittances to allow interoperability with ICD-10 codes?
an increase in 5010 rejections
The Joint Commission on-site survey process incorporates tracer methodology, which emphasizes surveyor review by means of
both system tracers and patient tracers
Storyboards are a method used in health care that
graphically display a performance improvement project conducted
The medical malpractice crisis of the 1970s prompted the development of _____________________ in health care facilities.
risk management
The primary advantage of concurrent quality data collection is that
chart completion issues can be remedied promptly
The Joint Commission's emphasis on improving quality of patient care for a participating facility is exemplary through the required self-assessment process tool known as
intracycle monitoring
intracycle monitoring
helps organizations with their continuous standards compliance efforts. Every accredited organization has access to an ICM Profile, an online workspace on The Joint Commission Connect extranet.
real-time analytics
the use of, or the capacity to use, all available enterprise data and resources when they are needed. It consists of dynamic analysis and reporting, based on data entered into a system less than one minute before the actual time of use.
focused standards asessment
provides organizations with an easy-to-use, interactive standards self-assessment scoring tool and is located within the ICM Profile
total quality management (TQM)
A management approach to long–term success through customer satisfaction. All members of an organization participate in improving processes, products, services, and the culture in which they work.
What feature distinguishes the Nominal Group Technique (NGT) from brainstorming?
NGT determines the importance of responses through a rating system
What quality improvement (QI) tool uses criteria to weigh different alternatives? This display would assist in viewing all relevant information at the same time.
a decision matrix
PDSA
Plan-Do-Study-Act
PDSA method
a “trial-and-learning” method to test changes quickly to see how they work
The U.S. federal government's CMS substitutes compliance of its Conditions of Participation requirements to hospitals that already have accreditation awarded by various other agencies that include the Joint Commission, CARF, AOA, or AAAHC. This is known as
deemed status
The process of reviewing and validating qualifications, granting professional or medical staff membership, and awarding delineated privileges is called the _____.
credentialing
What is this chart:
affinity diagram
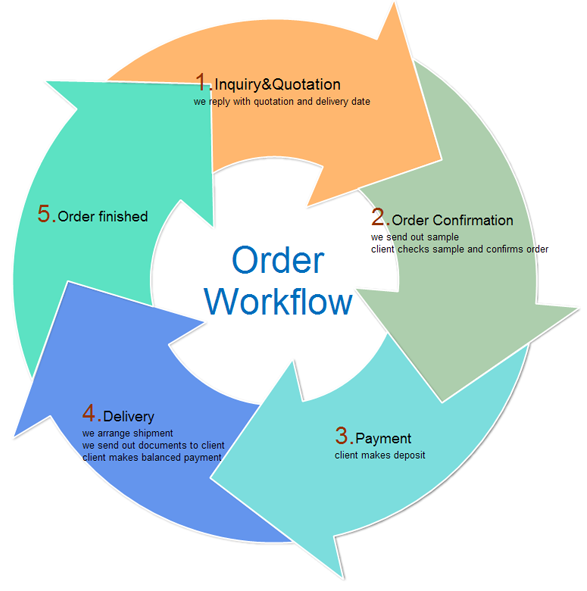
What is this chart:
arrow diagram
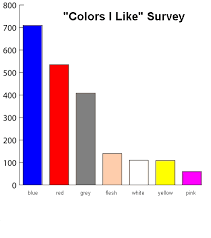
What is this chart:
bar chart
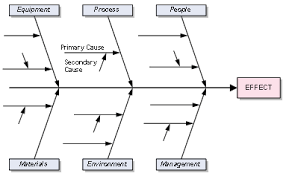
What is this chart:
cause-and-effect diagram
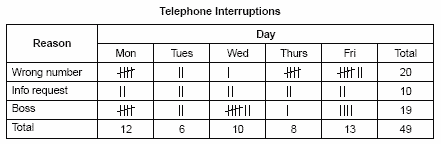
What is this chart:
checksheet
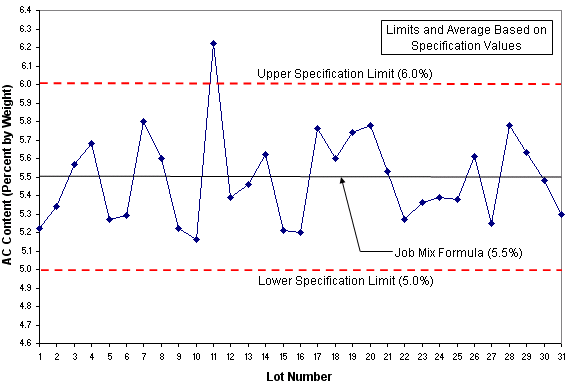
What is this chart:
control chart
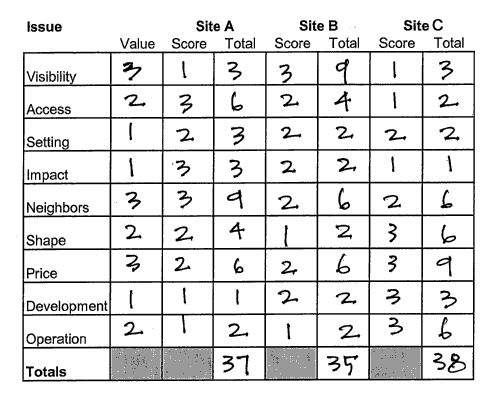
What is this chart:
decision matrix
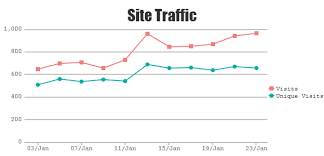
What is this chart:
line chart
What is this chart:
Pareto chart
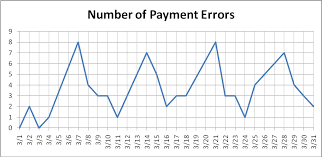
What is this chart:
run chart
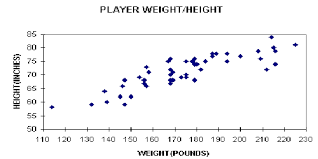
What is this chart:
scatter diagram
The Occupational Safety and Health Act of 1970, the Americans with Disability Act, and the Vocational Rehabilitation Act are all federal legislation designed to
keep the workplace safe and accessible to all employees and customers
"Qualified employees should be given priority when vacancies within the organization occur" is an example of
a policy of the organization
when setting productivity levels, a supervisor must
determine the productivity standards for each area and job function
A job analysis includes the
collection of data to determine the content of a job
A rule
predecides issues
Personal experience is
subjective
first trimester
week 1 through week 12
second trimester
week 13 to week 27
third trimester
week 28 to the birth
In project management, the series of specific tasks that determine the overall project duration is referred to as
critical path
project network
is always drawn from left to right to reflect project chronology
The formalized road map that describes how your institution executes the chosen strategy defines
strategic planning
the Wagner Act
The National Labor Relations Act (NLRA), which serves as the foundation for U.S. labor laws and collective bargaining
Strong lateral relationships within a facility are most likely when
individual departments cooperate together to achieve organizational goals
storytelling
a tool for strategic thinking
executive dashboard
a manager's version of a pilot's cockpit that contains all the critical information for leading the organization
payback period (formula)
initial investment/annual cash flow
Lilly Ledbetter Fair Pay Act
An amendment to the Civil Rights Act of 1964 that extends the 180-day statute of limitations previously applied to the filing of an equal-pay lawsuit
unity of command
an employee is responsible to only one supervisor, who in turn is responsible to only one supervisor, and so on up the organizational hierarchy
grievance procedure
a means of dispute resolution that can be used by a company to address complaints by employees, suppliers, customers, and/or competitors
span of control
the area of activity or number of functions, people, or things for which an individual or organization is responsible
organizational function
an organization's reporting relationships are grouped based on specialty, or functional area
replacement chart
a forecasting technique used in succession planning to help companies visualise key job roles, current employees and existing and future vacancies. Positions are mapped alongside information such as potential replacements, gender and promotion potential.
A basic concept of office layout and workflow is that the
paper moves to the employee
strategic plans
Written documents that assist an organization in achieving its objectives and carrying out its mission statement
calculate the minimum number of FTEs for transcription (formula)
lines per day X workdays per month / lines transcribed per month
cost per line (formula)
total hours worked X hourly cost / lines per month
The span of control in an organization refers to the
number of people who report to one supervisor
information governance
An initiative that focuses on the view that data as a strategic asset needs to be protected and accounted for across all levels of the health care enterprise
percentage of cost variance (formula)
budgeted expense – actual expense = ?
? X 100 / budgeted expense
A job analysis includes the
collection of data to determine the content of a job
Maslow's hierarchy of needs
From bottom up on the pyramid: "physiological", "safety", "belongingness/love", "esteem", "self-actualization",
Love and belongingness needs
friendship, intimacy, affection and love, - from work group, family, friends, romantic relationships.
Biological and Physiological needs
air, food, drink, shelter, warmth, sex, sleep
Safety needs
protection from elements, security, order, law, stability, freedom from fear
Esteem needs
achievement, mastery, independence, status, dominance, prestige, self-respect, respect from others
Self-Actualization needs
realizing personal potential, self-fulfillment, seeking personal growth and peak experiences
percentage of time was spent on coding (formula)
Remember to convert the hours to minutes!
Charts coded X minutes per chart = ? minutes coding
Hours worked X 60 minutes = ? minutes worked
Minutes coding / minutes worked = % spent on coding
sequence of steps most effective in order to improve efficiency and productivity
Know the objective
break down the work into component activities
group activities into proper organizational units
job grading
a systematic way of determining the value/worth of a job in relation to other jobs in an organization
factor comparison
A scientific method designed to rank job roles based on a breakdown of factors rather than the role as a whole. The ultimate goal is to assign the relative parts of each job role a financial value i.e. the amount of compensation offered for that part of the role.
job ranking
jobs are arranged in order of their value or merit to the organization
The MDS is designed for use in
long-term care facilities
APCs, payment status indicator "T" means
significant procedure, multiple procedure reduction applies.
in-service
(of training) intended for those actively engaged in the profession or activity concerned.
information system analysis phases
the health information managers primary goal is to provide a system that meets user or department needs and that also supports the strategic objectives of the enterprise including current and emerging privacy and security concerns
initiation IS life cycle
is the method through which organizations make decisions to invest in particular information systems
implementation IS life cycle
involves making the system operational in the organization
operations IS life cycle
personnel (clinical and administrative) who use the systems grow dependent on them to do their jobs. (It is running well and meeting the needs of the department.)
What type of system would be purchased to provide information on the census, update the master patient index, and distribute demographic data?
executive information system
The patient has the right to control access to his or her health information. This is known as
privacy
scope creep
in project management refers to uncontrolled changes or continuous growth in a project's scope. This can occur when the scopeof a project is not properly defined, documented, or controlled. It is generally considered harmful.
ombudsman
an official appointed to investigate individuals' complaints against maladministration, especially that of public authorities
Donabedian's framework
structure, process, and outcome
nuchal rigidity
impaired neck flexion resulting from muscle spasm (not actual rigidity) of the extensor muscles of the neck; usually attributed to meningeal irritation
Human Resources use a systematic procedure to determine the relative worth of a position to the organization. When this approach is used, compensation for the position is most likely based on
job evaluation
root cause analysis
fishbone diagram
Fulguration of anal warts. Identify the approach.
External
The most important consideration in planning the office layout for a Health Information Services department is the
workflow
Spinal fusion cervical C1-C2 (root operation)
Fusion
In statistics, the notation "ΣXY" means
multiplied each pair of the X and Y scores, then summed their values
Removal of a foreign body right external auditory canal (root operation)
Extirpation
Angioplasty abdominal iliac artery (root operation)
Dilation
forming stage
The stage of group development when the team discusses its purpose, defines and assigns tasks, establishes timelines, and begins forming personal relationships.
storming stage
The stage of group development when the team clarifies its goals and its strategy for achieving them (often-contentious).
norming stage
The stage of group development when the team establishes its values for how individuals will interact and collaborate.
performing stage
The stage of group development when team members have productive relationships and are able to communicate and coordinate effectively and efficiently.
The Phalen's wrist flexor test is a noninvasive method for diagnosing
carpal tunnel syndrome
Radiology codes would be used for
the supervision and interpretation
What federal legislation passed in 1986 gave immunity from legal action to practitioners regarding some peer review process activities?
Healthcare Quality Improvement Act
Colon polyp fulguration (root operation)
Destruction
myelomeningocele
a congenital condition that is the most severe neural tube defect
An area identified for needed improvement through benchmarking and continuous quality improvement is known as a
key performance indicator
Percutaneous placement of pacemaker lead. Identify the approach.
Percutaneous
Stopping of postoperative tonsillectomy hemorrhaging is coded to which root operation?
Control
Which endocrine gland secretes epinephrine, which activates the “fight or flight” response and increases blood pressure and metabolism?
adrenal medulla
Needlesticks, patient or employee falls, medication errors, or any event not consistent with routine patient care activities would require risk reporting documentation in the form of an
incident report
Excision gallbladder (root operation)
Resection
A major disadvantage of cross-sectional studies is that
the time sequence of exposure and disease is usually not known
Removal deep left vein thrombosis (root operation)
Extirpation
A histogram is a valuable tool for representing
a frequency distribution with continuous-interval data
delineation of privileges
(Physician credentialing) those specific services and procedures that a physician is deemed qualified to provide or perform
The Director of a Health Information Department prepared a document in which the following information could be obtained: job title, reporting line, span of control, and routes of promotion. The document she was preparing was a(n)
organizational chart
An elevated serum amylase would be characteristic of
acute pancreatitis
A complete redo of a knee replacement requiring a new prosthesis is coded to which root operation(s)?
Removal, Replacement
What process is mandatory for health care facilities?
licensure
With the passage of Medicare (Title XVIII of the Social Security Act) in 1965, what function became mandatory?
utilization review
The PQRS is a reporting system established by the federal government for physician practices who participate in Medicare for
quality measure reporting
PQRS
Physician Quality Reporting System
Dilation of the ureter with insertion of a stent is coded to which root operation?
Insertion
cross-sectional or prevalence studies are known for
concurrently describing characteristics and health outcomes at one specific point in time
The standard deviation of a particular set of measures was found to be 20.00. The sample variance would then be:
400
Diabetic microvascular disease occurs
as a direct result of elevated serum glucose
cells produce histamine in a type I hypersensitivity reaction
mast cells
Which type of joint, such as the sutures of the skull, has no movement?
synarthrosis
Percutaneous needle biopsy left lung (root operation)
Excision
In the Medical Surgical Section, the seventh character position represents?
Qualifier
Lithotripsy left ureter with removal of fragment (root operation)
Extirpation
ERCP. Identify the approach.
Endoscopic
ERCP
Endoscopic retrograde cholangiopancreatography
Scabies, a highly contagious condition that produces intense pruritus and a rash, is caused by
itch mites
The most fatal type of lung cancer is
small cell cancer
Ligation right fallopian tube (root operation)
Occlusion
ESWL left ureter. Identify the approach.
External
ESWL
Extracorporeal shock wave lithotripsy
EGD
esophagogastroduodenoscopy
scalar
(of a quantity) having only magnitude, not direction. a scalar quantity.
chain of command principle
(sometimes called the scaler chain) is the formal line of authority, communication, and responsibility within an organization. The chain of command is usually depicted on an organizational chart.
According to Frederick Herzberg, challenging work, recognition of workers and their accomplishments, and employee self-improvement are examples of
motivators
Removal cardiac pacemaker (root operation)
Removal
What method of performance appraisal requires the supervisor to document exceptional behavior by the employee?
Critical Incident Method
Creation of arteriovenous graft brachial artery left arm for hemodialysis (root operation)
Insertion
The Six Sigma methodology differs from other quality improvement models by defining improvement opportunities using
critical quality tree
The credentialing process requires healthcare facilities to
watch the provider perform surgery
What process assists a health care facility in continuously looking at the ways that problems develop and seeking ways to prevent problems from happening in the future?
performance improvement
incumbent
necessary for (someone) as a duty or responsibility
Iatrogenic
of or relating to illness caused by medical examination or treatment
Staging
is a system for documenting the extent or spread of cancer
The special form or view that plays the central role in planning and providing care at skilled nursing, psychiatric, and rehabilitation facilities is the
interdisciplinary patient care plan
Release of information has increased its use of part-time prn clerical support in order to respond to increased requests for release of information. The budget variance report will reflect
the increase in the cost of part-time clerical support for ROI but not the increase in revenue from this area
RHIO
regional health information organization
regional health information organization (RHIO)
a type of health information exchange organization (HIO) that brings together health care stakeholders within a defined geographic area and governs health information exchange among them for the purpose of improving health and care in that community.
The purpose of a Health Information Exchange (HIE) is to
improve health care delivery and information gathering
A _________uses a private tunnel through the Internet as a transport medium between locations for secure access and transmission.
VPN
Authentication is one of the components necessary to produce a legal document in an EHR. This means
identifying who created a document and when
An effective means of protecting the security of computerized health information would be to
develop clear policies on data security that are supported by the top management of the facility
In order to prevent the accidental introduction of a virus into your facility's local area network, your facility has a policy that strictly prohibits
downloading executable files from electronic bulletin boards
RFP
request for proposal
The decision makers in the HIM department have decided to use the decision analysis matrix method to select coding software. Use of this method will help ensure
consistent criteria are used to evaluate the alternatives/vendors
A section of a job description states that the incumbent will handle day-to-day operations in the transcription and release of information areas. This section defines the
scope of responsibility in the job
You are calculating the fee schedule payment amount for physician services covered under Medicare Part B. You already have the relative value unit figure. The only other information you need is
a national conversion factor
Down syndrome, Edwards' syndrome, and Patau's syndrome are all examples of __________defects.
chromosomal
In your state, it is legal for minors to seek medical treatment for a sexually transmitted disease without parental consent. When this occurs, who would be expected to authorize the release of the medical information documented in this episode of care to the patient's insurers?
the patient
WORM technology
a data storage technology that allows information to be written to a disc a single time and prevents the drive from erasing the data
WORM
write once, read many
the primary consideration when making retention decisions must be
statutory requirements
Identification of threats and vulnerabilities, security measures, and implementation priorities are part of a health care organization's
risk management plan
What condition is always considered "present on admission" (POA)?
congenital conditions
You have been asked to reduce your department's operating budget by 20%. In order to do so, you will have to effect reductions in your largest budget line. You will have to make cuts in
personnel
The coding supervisor tends to deal with issues as they come up, prioritizing only when problems are pressing or appear to be important to upper management. This crisis manager is particularly weak in which management function?
planning
The transcriptionists have collected data on the number and types of problems with the dictation equipment. The best tool to display the data they collected is a
Pareto chart
A union campaign is being conducted at your facility. As a department manager, it is appropriate for you to tell employees that
you are opposed to the union
A common goal of the Office of the National Coordinator for Health Information Technology, RHIOs, and a national infrastructure for information is
sharing information among providers
Health information exchange is a term used to refer to a
"plan in which health information is shared among providers."
Your HIM department is moving to a new location and in order to arrange your employees and functions for optimal work flow efficiency and to decide which employees need to be placed close to each other, the tool you decide to use is a
flow process chart
In reviewing the policies on release of information in respect to the privacy rules, you note that it is still acceptable to allow release of protected health information without patient permission to
the quality assurance committee for review purposes
The purpose of the Correct Coding Initiative is to
detect and prevent payment for improperly coded services
A run or line chart would be most useful for collecting data on
waiting time in the Pediatrics Clinic
E-mails and text messages are
considered health care business records and are subject to the same regulations as records created in face-to-face patient encounters
Critical to implementations and project success, the WBS
lists steps needed to complete the project
Evidence-based management and decision making is an emerging model now used to make more informed decisions. The premise of this model is
using the best clinical and research practices available
Community Hospital reported an average LOS in December of 3.7 days with a standard deviation of 23. This information indicates that
there was a large variation in the LOS at Community Hospital
PACS
Picture archiving and communication systems
Access to radiologic images has been improved through the use of
PACS
Picture archiving and communication systems (PACS) provide
a means to store and rapidly access digitized file images
The committee that is preparing your acute care hospital for an electronic health record is planning for an imaging system for record archiving in the immediate future. They are looking for a solution for data interfacing or integration of the imaging system into other computer systems. You recommend
Health Level 7 standards.
A patient has written to request a copy of his own record. When the clerk checked the record, it was noted that the patient was last admitted to the psychiatric unit of the facility. You advise the clerk to
contact the patient's attending physician before complying.
A p value of less than 0.05 is what researchers commonly use to reject the null hypothesis. A smaller p value may place interpretation of the results of the study at risk for a
sampling error
Joanie Howell presents to Dr. Franklin requesting rhinoplasty. Because Howell is covered by Medicare, Dr. Franklin must provide Howell with
an Advance Beneficiary Notice, because Howell's rhinoplasty may not be medically necessary
The protocol that allows a browser to connect to a server and authenticate identities for data transfer is known as a(n) ____________ connection.
secure socket layer
Generally, CMS requires the submission of a claim (CMS 1450) for inpatient services provided to a Medicare beneficiary for inpatient services. An exception to this requirement would be when
the beneficiary refuses to authorize the submission of a bill to Medicare
According to CPT, a biopsy of the breast that involves removal of only a portion of the lesion for pathologic examination is
incisional
a checklist for assessing an obstetric patient's lochia, fundus, and perineum would be on what type of document
postpartum record
The discharge diagnosis for this inpatient encounter is rule out myocardial infarction. The coder would assign
a code for a myocardial infarction
A piece of objective data collected upon initial assessment of the patient is the
vital signs
A major key to forms control in this setting is
giving each form or view an identifiable name, number, and revision date
As part of a team responsible for revenue analysis at your facility, you recommend a yearly review of
the OIG Workplan
compression fracture of the vertebrae as a result of bone metastasis
a pathologic fracture
A technique that uncovers new information from existing information by probing data sets is known as
data mining
The 2014 AHIMA Foundation's “Clinical Documentation Improvement Job Description Summative Report” identified that most Clinical Documentation Improvement Specialists report directly to the
HIM Department
The use of "public" and "private" keys is part of what type of data protection?
Encryption
The CFO of your facility asks you to prepare a budget for the fiscal year based on the past volume and expected capacity for the coming year. This process is an example of using the "_____________" budgeting method.
fixed budget
Reference checks are conducted on potential employees to help assess the applicant's fit with the position and also to
confirm the accuracy of information provided on the application
ORYX is a program that was developed by
Joint Commission to link patient outcomes to accreditation
The most sophisticated level of interoperability of an EHR and other such systems is the ______________ level.
semantic
define the Global Surgical Package
all necessary services normally furnished by a surgeon before, during, and after a procedure defined by Medicare.
DME / HME
home medical equipment (HME) / durable medical equipment (DME)
ER physician performs an LP and orders a CSF analysis with a bacterial culture and sensitivity. The physician is attempting to comfirm a diagnosis of
meningitis due to Neisseria meningitidis-positive cerebrospinal fluid.
Which department will most likely be responsible for taking corrective action regarding the number of insurance claims requiring resubmission due to errors (not related to coding) not exceeding 3%?
Business Office
root cause analysis
a method of problem solving used for identifying the root causes of faults or problems and is reportable to the Joint Commission
To ensure consistency of coverage among trainers, you may want to develop
training manuals
In statistics, the notation "ΣXY" means
multiplied each pair of the X and Y scores, then summed their values
Information Governance
the activities and technologies that organizations employ to maximize the value of their information while minimizing associated risks and costs.
information governance initiative
a cross-disciplinary consortium and think tank dedicated to advancing the adoption of information governance practices and technologies through research, publishing, advocacy and peer-to-peer networking.
What is the stage where teams may experience disequilibrium?
storming
delineation of privileges
specific services and procedures that a physician is deemed qualified to provide or perform
When a physician orders a liver panel, what tests would be included?
albumin, bilirubin, alkaline phosphatase
pulmonary angiography
Pulmonary blood vessels are x-rayed to detect arteriovenous malformations.
Direct angiography
the injection of radiocontrast into the circulation with subsequent fluoroscopy (direct X-ray visualisation) of the lungs
lung scan
a nuclear scanning test that is most commonly used to detect a blood clot that is preventing normal blood flow to part of a lung (pulmonary embolism)
Staging
the progression of cancer
RFP
request for proposal
What system might an HIM Director most likely recommend in the early stages of the project as a transition strategy for having the entire health record content recorded in discrete form within the next 10 years?
electronic document management system
A final progress note is an appropriate discharge summary for
the delivery a healthy 8-pound baby without complications for either mother or child, and both discharged within 36 hours of admission
A surgical operation is
one or more surgical procedures performed at one time for one patient using a common approach or for a common purpose
A patient is admitted through the emergency department. Three days after admission, the physician documents uncontrolled diabetes mellitus. What is the "present on admission" (POA) indicator for uncontrolled diabetes mellitus?
"N"
respondeat superior
"let the master answer"
a US legal doctrine which states that, in many circumstances, an employer is responsible for the actions of employees performed within the course of their employment.
WBS
work breakdown structure
work breakdown structure (WBS)
a chart in which the critical work elements, called tasks, of a project are illustrated to portray their relationships to each other and to the project as a whole.
S-subjective
records what the patient states is the problem
O-objective
records what the practitioner identifies through history, physical examination, and diagnostic tests
A-assessment
combines the subjective and objective into a conclusion
P-plan
what approach is going to be taken to resolve the problem
ABN
Advance Beneficiary Notice
Advance Beneficiary Notice (ABN)
also known as a waiver of liability
a notice you should receive when a provider or supplier offers you a service or item they believe Medicare will not cover. ABNs only apply if you have Original Medicare, not if you are in a Medicare Advantage private health plan.
Generally, CMS requires the submission of a claim (CMS 1450) for inpatient services provided to a Medicare beneficiary for inpatient services. An exception to this requirement would be when
the beneficiary refuses to authorize the submission of a bill to Medicare
CMS 1500
Health Insurance Claim Form
CMS 1450
(aka UB-04 at present)
can be used by an institutional provider to bill a Medicare fiscal intermediary (FI) when a provider qualifies for a waiver from the Administrative Simplification Compliance Act (ASCA) requirement for electronic submission of claims. It is also used for billing of institutional charges to most Medicaid State Agencies.
an obstetric patient's lochia, fundus, and perineum may be found on what document?
postpartum record
As the Information Security Officer at your facility, you have been asked to provide examples of technical security safeguards adopted as a result of HIPAA legislation. Which of the following would you provide?
surge protectors
You are conducting an educational session on benchmarking. You tell your audience that the key to benchmarking is to use the comparison to
improve your department's processes
The most sophisticated level of interoperability of an EHR and other such systems is the ______________ level.
semantic
PDSA cycle
is shorthand for testing a change—by planning it, trying it, observing the results, and acting on what is learned.
You are implementing a quality improvement plan that utilizes the PDSA cycle. If you correctly implement PDSA, which phase of the project will take the most of your time?
P-planning
The EHR system implementation team is using simulated patients and simulated patient information to add progress notes, nurses' notes, and so on, to the EHR prior to implementation. Which system development life cycle phase is the team involved in?
analysis
What Web 2.0 technology would you recommend for someone who wants to share their battle with cancer?
a blog
Your facility has decided to implement the new laboratory information system on one unit and then add more units as your confidence in the system grows. What go-live model are you using?
pilot
You need a system that will work with your existing system but not necessarily from the same vendor. What type of system are you looking for?
interfaced
What type of system would be purchased to provide information on the census, update the master patient index, and distribute demographic data?
executive information system
You have been asked to develop scenarios that will be used to design and program a new release of information system. These scenarios will include the processes to be used in detail. What are you designing?
use cases
The patient has the right to control access to his or her health information. This is known as
privacy
A record destruction program should include
the method of destruction
2 techniques a facility would employ for access control
automatic logoff and unique user identification
You are defining the designated record set for South Beach Healthcare Center. What would be included?
discharge summary
Mountain Hospital has discovered a security breach. Someone hacked into the system and viewed 50 medical records. According to ARRA, what is the responsibility of the covered entity?
All individuals must be notified within 60 days.
The information system has just notified you that someone has attempted to access the system inappropriately. This process is known as
intrusion detection
an example of administrative safeguards under the security rule would be
monitoring the computer access activity of the user
The police came to the HIM Department today and asked that a patient's right to an accounting of disclosure be suspended for two months. What is the proper response to this request?
"Certainly officer. We will be glad to do that as soon as we have the request in writing."
To prevent their network from going down, a company has duplicated much of its hardware and cables. This duplication is called
redundancy
HIPAA states that release to a coroner is allowed. State law says that the coroner must provide a subpoena.
Follow the state law since it is stricter.
the Privacy Act of 1974 applies to the
federal government
an example of an administrative safeguard would be
training
Richard has asked to view his medical record. Within what timeframe must the facility provide this record to him?
30 days
You are reviewing your privacy and security policies, procedures, training program, and so on, and comparing them to the HIPAA and ARRA regulations. You are conducting a
risk assessment
Your department was unable to provide a patient with a copy of his record within the 30-day limitation. What should you do?
Write the patient and tell him that you will need a 30-day extension.
A patient signed an authorization to release information to a physician but decided not to go see that physician. Can he stop the release?
Yes, as long has it has not been released already
Miles has asked you to explain the rights he has via HIPAA privacy standards. What is one of his HIPAA-given rights?
He can ask to be contacted at an alternative site.
Before we can go any further with our risk analysis, we need to determine what systems/information need to be protected. This step is known as
system characterization
The hospital has received a request for an amendment. How long does the facility have in order to accept or deny the request?
60 days
The main layers of the epidermis
stratum corneum
stratum lucidium
stratum granulosm
stratum spinosum
stratum germinativum (aka stratum basale)
How can Graves' disease be treated?
radioactive iodine therapy, antithyroid drugs, and surgery
When a decubitus ulcer has progressed to a stage in which osteomyelitis is present, the ulcer has extended to the
bone
United States healthcare providers are concerned about a possible pandemic of avian flu because
there is no vaccine currently available, it is caused by a group of viruses that mutate very easily, and the causative virus is being spread around the world by migratory birds.
Clinical manifestations of this disease include polydipsia, polyuria, polyphagia, weight loss, and hyperglycemia. What test(s) would be ordered to confirm the disease?
glucose tolerance test
Henrietta Dawson presents with a chief complaint of pain and weakness in her arms and neck. After an H and P and a review of diagnostic tests that include a myelogram, her doctor diagnoses a herniated nucleus pulposus at the _________ level of her spine.
cervical
A physician prescribes a diuretic for his patient. He could be treating
congestive heart failure, pulmonary edema, or mitral stenosis.
unity of command
an employee is responsible to only one supervisor, who in turn is responsible to only one supervisor, and so on up the organizational hierarchy
Research has shown that productivity increases when
employees are rewarded for extra output, it becomes the primary goal of management, and it is measured.
Employers may be able to demonstrate that age is a reasonable requirement for a position. Such an exception to the Age Discrimination in Employment Act (ADEA) is called a
bona fide occupational qualification
As a new RHIA and coding manager, how likely is it that you will participate on committees?
Occasionally, mostly with your staff.
Which appraisal method places the employees into a set of ordered groups (e.g., top 10%, above average 20%, middle 40%) on the basis of a global measure?
forced ranking
The teaching method selected by an instructor influences the student's ability to understand the material. Instructor-led classrooms work best when
in-depth training and interaction are desired.
Under the Immigration Reform and Control Act
applicant must have I-9 documentation, noncitizens may not be discriminated against, and undocumented workers may not be hired
Mission Health Systems has contracted with an agency to conduct recruitment and screening of potential candidates. This approach is called
outsourcing
The term "hard coding" refers to
HCPCS/CPT codes that appear in the hospital's chargemaster and will be included automatically on the patient's bill.
The Correct Coding Initiative (CCI) edits contain a listing of codes under two columns titled "comprehensive codes" and "component codes." According to the CCI edits, when a provider bills Medicare for a procedure that appears in both columns for the same beneficiary on the same date of service code
only the comprehensive code
Under Medicare Part B
collections are restricted to only the deductible and coinsurance due at the time of service on an assigned claim.
fees are restricted to charging no more than the "limiting charge" on nonassigned claims.
providers must file all Medicare claims.
The _______________ is a statement sent to the provider to explain payments made by third-party payers.
remittance advice
What type of filing system is being used if records are filed in the following order: 12-23-75, 12-34-29, 12-35-71, 13-42-14, and 14-32-79?
straight numeric
In a terminal digit filing system, what would be the record number immediately in front of record number 01-06-26?
00-06-26
Some advantages of a computerized master patient index are
it solves most space and retrieval problems
it allows access to data alphabetically, phonetically, or by date of birth, social security number, medical record, or billing number
it provides other departments with immediate access to the information maintained in the master patient index.
Lewis-Beck Medical Center has been collecting data on patient satisfaction for six months. It is ready to start retrieving data from the database to improve clinical services. Which tool should be used?
SQL
What would be the most cost-effective and prudent course of action for the storage or disposition of 250,000 records at a large teaching and research hospital?
scanning all 250,000 records for a cost of $195,000
A health information manager develops a formal plan or record retention schedule for the automatic transfer of records to inactive storage and potential destruction based on
volume of research, statute of limitations, and readmission rate
University Hospital, a 900-bed tertiary health care organization, is undergoing an information systems development. What system would best meet its needs?
Application service provider model
A file area has limited space, medium file activity, and two file clerks. The HIM department would benefit from choosing which type of storage equipment?
compressible filing units
The hospital administrator is making a strategic decision by querying various institutional databases for information. What type of system is the hospital administrator using?
executive information system
Case finding methods for patients with diabetes include a review of
medication lists
billing data
health plans
The master patient index must, at a minimum, include sufficient information to
uniquely identify the patient
an advantage of straight numeric filing over terminal digit filing
The training period is short
For a health care facility to meet its document destruction needs, the certificate of destruction should include
location of destruction, unique and serialized transaction number, and acceptance of fiduciary responsibility
A health care facility has made a decision to destroy computerized data. AHIMA recommends what as the preferred method of destruction for computerized data?
magnetic degaussing
Color coding of record folders is used to assist in the control of
misfiles
Factors to consider when developing a record retention program include
cost of space to maintain paper records, legal requirements as determined by statute of limitations, and record usage in the facility determined by health care provider activity
Strategies when purchasing an electronic health record system include
identify system requirements, recognize stakeholders from different organizational levels and engage them appropriately, and determine return on investment or cost-benefit analysis.
What data cannot be retrieved from the MEDPAR?
Non-Medicare patient data
When evaluating an outside contract microfilm company, important factors to rate would include
cost, emergency returns, and storage after filming
data retrieval tools
sound
icons
color
In your facility, the health care providers from every discipline document progress notes sequentially on the same form. Your facility is utilizing
integrated progress notes
You try to convince the entire health care team to consistently enter data into the patient's record at the time and location of service instead of waiting for retrospective analysis to alert them to complete the record. You are proposing
point-of-care documentation
Which of the four distinct components of the problem-oriented record serves to help index documentation throughout the record?
problem list
The foundation for communicating all patient care goals in long-term care settings is the
interdisciplinary plan of care
You notice on the admission H&P that Mr. McKahan, a Medicare patient, was admitted for disc surgery, but the progress notes indicate that due to some heart irregularities, he may not be a good surgical risk. Because of your knowledge of COP regulations, you expect that a _______________ will be added to his health record.
consultation report
As a new HIM manager of an acute care facility, you have been asked to update the facility's policy for a physician's verbal orders in accordance with Joint Commission standards and state law. Your first area of concern is the qualifications of those individuals in your facility who have been authorized to record verbal orders. For this information, you will consult the
Hospital Bylaws, Rules, and Regulations
The first patient with cancer seen in your facility on January 1, 2015, was diagnosed with colon cancer with no known history of previous malignancies. The accession number assigned to this patient is
15-0001/00
Gerda Smith has presented to the ER in a coma with injuries sustained in a motor vehicle accident. According to her sister, Gerda has had a recent medical history taken at the public health department. The physician on call is grateful that she can access this patient information using the area's
RHIO
In determining your acute care facility's degree of compliance with prospective payment requirements for Medicare, the best resource to reference for recent certification standards is the
Federal Register
Data reliability implies
that data are consistent no matter how many times the same data are collected and entered into the system
Accessibility implies
that data are available to authorized people when and where needed
Legibility implies
data that are readable
Completeness implies
that all required data are present in the information system
Data comprehensiveness
refers specifically to the presence of all required data elements
Quantitative analysis involves
checking for the presence or absence of necessary reports and/or signatures
Qualitative analysis may involve
checking documentation consistency, such as comparing a patient's pharmacy drug profile with the medication administration record
Data Elements for Emergency Departments
recommended data set for hospital-based emergency departments
Uniform Hospital Data Set
required data set for acute care hospitals
Minimum Data Set
required data set for long-term care facilities
ORYX
an initiative of Joint Commission whereby five core measures are implemented to improve safety and quality of health care
Data accuracy denotes that
data are correct values
Data comprehensiveness denotes that
all data items are included
Data granularity denotes that
the attributes and values of data should be defined at the correct level of detail
Data precision denotes that
data values should be just large enough to support the application of process
Time and means of arrival is required on
ED records only
Evidence of known advance directive is required on
inpatient records only
Problem list is required on
ambulatory records by the third visit
One record documentation requirement shared by BOTH acute care and emergency departments is
patient's condition on discharge
The Minimum Data Set is a basic component of the
long-term care RAI
UHDDS is used in
acute care
OASIS is used in
home health
DEEDS is used in
emergency departments
The federally mandated resident assessment instrument used in long-term care facilities consists of three basic components, including the new care area assessment, utilization guidelines, and the
MDS
In creating a new form or computer view, the designer should be most driven by
needs of the users
Managers are
Held responsible for handling the organization’s resources
The practice of management is
Influenced by the context of the organization
Systems thinking
Is an objective way of looking at ideas and processes
A graphic representation of the organization’s formal structure is called
An organizational chart
The mission statement
Is updated regularly as part of the strategic planning process
Supervisory managers are primarily responsible for
Monitoring everyday performance
Developing, implementing, and revising the organization’s policies is the role of
Middle managers
Ultimate responsibility for the operation of healthcare organizations lies with
The board of directors
Planning, organizing, controlling, decision making, and leadership are the functions of
Management
Strategic planning is primarily concerned with
How the organization will respond to changes in the environment
Within an organization it is the supervisor’s role to determine
How the work will be accomplished by the team
In modern management theory, control is most important when applied to
Processes and other resources
The director of the department is Bob. Sally, the coding supervisor and five other supervisors, report to Bob. Tim and 10 other coders report to Sally. This describes what management concept?
Chain of command
Strengthening others by sharing information and power is a characteristic of
Leadership
A summary of the position, a list of duties, and the qualifications required to perform the job are all elements of a
Position description
Performance standards are used to
Communicate performance expectations
Position descriptions, policies and procedures, training checklists, and performance standards are all examples of
Human resource tools
Procedures should be complete enough so that
Anyone generally competent for that position can perform the task
The department’s orientation checklist would include a
Review of communication policies
Description of how to request time off
Review of departmental goals
During training, the employee should be
Encouraged to ask questions
Teams often fail to succeed when
The leader dominates the team
Setting a clear deadline is an important step in
Delegation
Discovering each individual’s talents and maximizing them is the role of the
Coach
Periodic performance reviews
Encourage good performance
Disciplinary action
Should be documented at each step
Constructive confrontation is one form of
Conflict management
Grievance procedures
Are defined in the union contract
On-the-job training
Is one option for staff development
During times of change, it is important for the supervisor to
Hold on to the vision
The budget
Is the financial plan for the coming time period
Zero-based budgeting is not
Based on work volume and unit cost
Before beginning to budget at the department level, it is important to understand
What the organization’s budget assumptions are
Monitoring ongoing revenues and expenses and verifying actual expenses are important steps in
Financial control
What is the goal of clinical practice guidelines?
To standardize clinical decision making
What is the largest healthcare standards-setting body in the world?
Joint Commission
What is not a responsibility of a healthcare organization’s quality management department?
Using medical peer review to identify patterns of care
What are the responsibilities of a healthcare organization’s quality management department?
Helping departments to identify potential clinical quality problems
Participating in regular departmental meetings across the organization
Determining the method for studying potential problems
Problems in patient care and other areas of the healthcare organization are usually symptoms inherent in a
System
Define utilization management
It is a set of processes used to determine the appropriateness of medical services provided during specific episodes of care.
What are types of utilization review?
Preadmission utilization review
Discharge utilization review
Documentation utilization review
What is the role of the case manager?
Coordinate medical care and ensure the necessity of the services provided to beneficiaries
What roles are representative of the ombudsman in patient advocacy?
Mediator
Listener
Partner
A hospital’s C-section rate is an example of a
Clinical performance measure
The process that involves ongoing surveillance and prevention of infections so as to ensure the quality and safety of healthcare for patients and employees is known as
Infection control
The traditional approach to assuring quality was to study a process only when there was failure to
Meet established standards
Donabedian proposed three types of quality indicators: structure indicators, process indicators, and
Outcome indicators
Many organizations and quality experts define quality as meeting or exceeding
Customer expectations
What is a technique used to generate a large number of creative ideas from a group?
Brainstorming
What is a data collection tool that records and compiles observations or occurrences?
Checksheet
What is used to plot the points for two variables that may be related to each other in some way?
Scatter diagram
The leader of the coding performance improvement team wants all of her team members to clearly understand the coding process. What would be the best tool for accomplishing this objective?
flowchart
The medical transcription improvement team wants to identify the cause of poor transcription quality. What tool would best aid the team in identifying the root cause of the problem?
Fishbone diagram
According to the Pareto principle
20 percent of the sources of a problem are responsible for 80 percent of its actual effects
is a methodology for assessing compliance with Joint Commission standards during the survey process.
Tracer methodology
are contracted to the federal government to use medical peer review, data analysis, and other tools to identify patterns of care and outcomes that need improvement and then to work cooperatively with facilities and individual physicians to improve care.
QIOs
refers to initiatives and programs that reward organizations and providers for quality outcomes.
Pay for performance
refers to computerized systems into which physicians or hospital staff directly enter medication orders and therefore benefit from immediate alerts and pharmaceutical information in order to reduce the frequency of medication errors.
CPOE
are Joint Commission’s standards for improving patient safety.
NPSGs
QIO
Quality Improvement Organization
Which piece of legislation created a program for detecting fraudulent health plans?
Health Insurance Portability and Accountability Act of 1996
Which of the following is a basic assumption of normative decision theory?
Decision makers have total knowledge of the available options.
Which of the following is an advantage of the case-control study design?
The case-control study design requires few subjects relative to other study designs.
LTC
Long term care