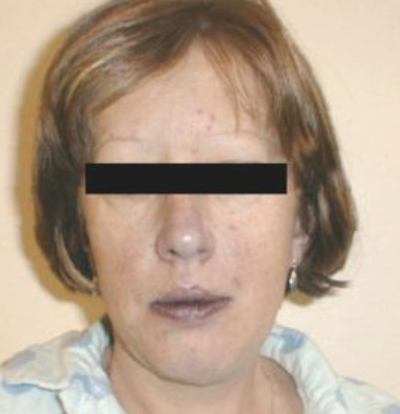
cyanosis
[central/peripheral] cyanosis can be seen in the lips, tongue, and cheeks
central
[central/peripheral] cyanosis can be seen in the fingers and indicates diminshed blood flow to the local area
peripheral
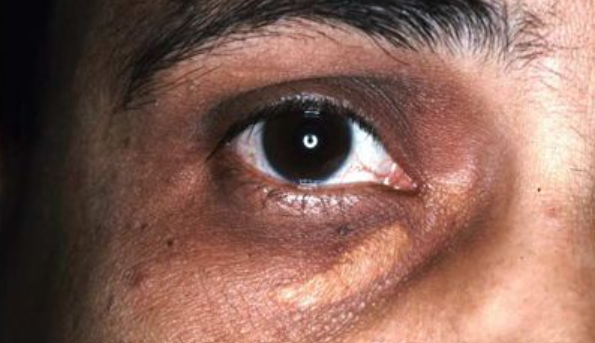
xanthelasma
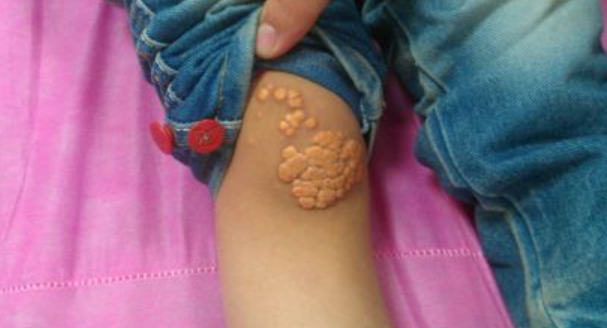
xanthomas
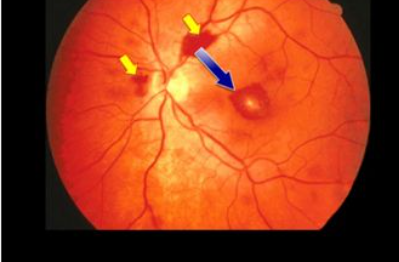
roth spots
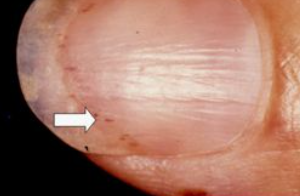
splinter hemorrhages
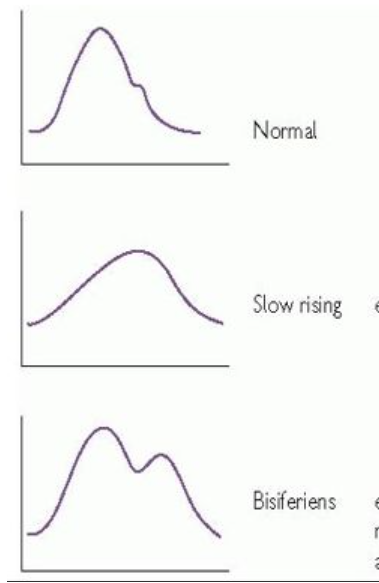
normal
aortic stenosis
aortic stenosis mixed w mitral regurgitation
A patient has a 28 mm Hg systolic BP difference between arms on repeated measurements. Which finding is most likely being suggested?
A) Normal adult variation
B) Perioral cyanosis
C) Retinal embolization
D) Vascular abnormality
D. Vascular abnormality
During a cardiovascular exam, a patient has an abnormal respiratory rate. Which paired interpretation is most appropriate?
A) Cardiac decompensation or lung disorder
B) Normal finding in all adults
C) Specific for infective endocarditis
D) Diagnostic of aortic regurgitation
A. Cardiac decompensation or lung disorder
A 2-month-old is evaluated for suspected congenital aortic narrowing. Which bedside comparison is most important?
A) Eye plaques and extensor nodules
B) Palms and soles for hemorrhages
C) Arm-leg pulses and blood pressures
D) Right-left pupillary light reflexes
C. Arm-leg pulses and blood pressures
In infants and children, comparing pulses and blood pressure between the arms and legs is most useful for diagnosing which condition?
A) Coarctation of the aorta
B) Familial hypercholesterolemia
C) Infective endocarditis
D) Aortic regurgitation
A. Coarctation of the aorta
A newborn has bluish discoloration around the lips but otherwise appears well. Which statement best applies?
A) Always indicates endocarditis
B) Always indicates aortic stenosis
C) Confirms systemic hypoxemia
D) Can be normal in infants
D. Can be normal in infants
A clinician suspects digital clubbing and asks the patient to oppose the dorsal surfaces of corresponding fingernails. Which test is being used?
A) Allen test
B) Schamroth window test
C) Homan sign
D) Pulsus parvus test
B. Schamroth window test
Soft yellow plaques around a patient’s eyelids are noted during inspection. Which term best describes this finding?
A) Janeway lesions
B) Roth spots
C) Xanthelasma
D) Osler nodes
C. Xanthelasma
Xanthelasma is best described as which lesion-location pairing
A) Soft yellow plaques; around eyes
B) Painful nodules; digit tips
C) Painless macules; palms and soles
D) Hemorrhages; beneath fingernails
A. Soft yellow plaques; around eyes
A patient has hard yellow-orange eruptive lesions of varying size over extensor surfaces. Which lesion is most likely?
A) Xanthelasma
B) Janeway lesion
C) Osler node
D) Xanthoma
D. Xanthoma
Which description best matches xanthomas rather than xanthelasma?
A) Soft plaques around eyelids
B) Hard eruptive extensor lesions
C) Retinal lesions with white centers
D) Painless hemorrhagic palm lesions
B. Hard eruptive extensor lesions
A patient with familial hypercholesterolemia has hard yellow-orange lesions over extensor joints. Which finding is being described?
A) Xanthomas
B) Osler nodes
C) Roth spots
D) Splinter hemorrhages
A. Xanthomas
Which lipid-associated lesion is commonly found around the eyes as soft yellow macules or plaques?
A) Xanthoma
B) Osler node
C) Xanthelasma
D) Janeway lesion
C. Xanthelasma
Which set contains classic peripheral or ocular signs of infective endocarditis?
A) Xanthomas, xanthelasma, clubbing, cyanosis
B) Roth spots, splinters, Osler, Janeway
C) Parvus, tardus, bounding, bisferiens
D) Coarctation, cyanosis, clubbing, xanthomas
B. Roth spots, splinters, Osler, Janeway
A patient with suspected infective endocarditis has fundoscopic round hemorrhagic retinal lesions with pale centers. Which finding is present?
A) Roth spots
B) Janeway lesions
C) Osler nodes
D) Xanthelasma
A. Roth spots
Roth spots in infective endocarditis are best described as which finding?
A) Painless hemorrhages on soles
B) Painful nodules on digits
C) Yellow lipid plaques near eyes
D) Retinal hemorrhages with white centers
D. Retinal hemorrhages with white centers
A patient with infective endocarditis has painful erythematous subcutaneous nodules on the fingertips. Which lesion is being described?
A) Janeway lesions
B) Roth spots
C) Osler nodes
D) Xanthomas
C. Osler nodes
A patient with infective endocarditis has painless hemorrhagic macules on the soles. Which lesion is most likely?
A) Janeway lesions
B) Osler nodes
C) Xanthomas
D) Roth spots
A. Janeway lesions
Which finding is classified as a sign of infective endocarditis rather than lipid deposition?
A) Xanthelasma
B) Splinter hemorrhages
C) Xanthomas
D) Schamroth window
B. Splinter hemorrhages
A patient has a small, delayed, slow-rising carotid upstroke. Which valve lesion is most classically associated?
A) Aortic stenosis
B) Aortic regurgitation
C) Mitral stenosis
D) Tricuspid regurgitation
A. Aortic stenosis
The carotid pulse of aortic stenosis is classically described by which phrase?
A) Pulsus bisferiens
B) Bounding pulse
C) Corrigan pulse
D) Pulsus parvus et tardus
D. Pulsus parvus et tardus
Aortic stenosis produces which carotid pulse contour?
A) Large and bounding
B) Painless and hemorrhagic
C) Small, delayed, slow-rising
D) Double positive upstroke
C. Small, delayed, slow-rising
A patient has a large, bounding carotid pulse on exam. Which lesion best matches this pulse finding?
A) Aortic stenosis
B) Aortic regurgitation
C) Coarctation of aorta
D) Infective endocarditis
B. Aortic regurgitation
Which carotid pulse finding best matches aortic regurgitation
A) Large and bounding
B) Small and delayed
C) Two narrowly spaced waves
D) Absent femoral pulse
A. Large and bounding
A patient has mixed aortic stenosis and regurgitation. Which carotid pulse is expected?
A) Pulsus paradoxus
B) Pulsus alternans
C) Pulsus parvus
D) Pulsus bisferiens
D. Pulsus bisferiens
Pulsus bisferiens is best described as which carotid pulse pattern?
A) Slow single delayed wave
B) Weak collapsing upstroke
C) Two narrowly spaced positive waves
D) Normal pulse with respiratory variation
C. Two narrowly spaced positive waves
Which condition has pulsus bisferiens as a cardinal finding?
A) Aortic stenosis only
B) Hypertrophic cardiomyopathy
C) Pulmonary valve stenosis
D) Mitral regurgitation
B. Hypertrophic cardiomyopathy
A patient has two narrowly spaced positive carotid waves. Which term best describes this pulse?
A) Pulsus bisferiens
B) Pulsus parvus
C) Pulsus tardus
D) Pulsus paradoxus
A. Pulsus bisferiens
A public health researcher stratifies heart disease mortality by sex. Which pattern is most consistent with epidemiologic data
A) Equal deaths in both sexes
B) More than half in males
C) Mostly pediatric female deaths
D) Predominantly young female deaths
B. More than half in males
A 58-year-old smoker with uncontrolled hypertension and elevated LDL asks which modifiable factors most strongly increase heart disease risk. Which set is most appropriate?
A) HTN, LDL, smoking
B) HDL, exercise, estrogen
C) Fever, anemia, obesity
D) Bradycardia, vagal tone, age
A. HTN, LDL, smoking
A 19-year-old from a resource-limited region develops chronic valvular disease after recurrent untreated pharyngitis. Which acquired heart disease is most common in patients under 25?
A) Bacterial endocarditis
B) Hypertrophic cardiomyopathy
C) Rheumatic heart disease
D) Aortic dissection
C. Rheumatic heart disease
A global health team studies populations with very high rates of acute renal failure and rheumatic heart disease. Which populations are especially affected?
A) Inuit, Scandinavians, Japanese
B) Indigenous Australians, Maori, Pacific Islanders
C) Central Europeans, Greeks, Koreans
D) Ashkenazi Jews, Italians, Russians
B. Indigenous Australians, Maori, Pacific Islanders
A clinician wants to focus rheumatic heart disease screening in the region with the highest reported prevalence, including Fiji. Which region is most appropriate?
A) Pacific region
B) Mediterranean region
C) Caribbean region
D) Central Europe
A. Pacific region
A patient who injects street drugs develops fever and a new murmur. Which diagnosis is most directly associated with this risk factor?
A) Rheumatic fever
B) Bacterial endocarditis
C) Metabolic syndrome
D) Viral pericarditis
B. Bacterial endocarditis
A patient with bacterial endocarditis develops stroke-like symptoms, renal infarcts, and splenic lesions. Which mechanism best explains these systemic findings?
A) Isolated vagal overactivity
B) Persistent bacteremia with spread
C) Primary phrenic nerve irritation
D) Sympathetic ganglion failure
B. Persistent bacteremia with spread
Which complication pattern best matches bacterial endocarditis?
A) Valvular damage plus metastatic infection
B) Isolated pericardial pain
C) Pure coronary vasospasm
D) Reversible insulin resistance
A. Valvular damage plus metastatic infection
A patient with hypertension, hyperglycemia, central obesity, abnormal cholesterol, and abnormal triglycerides is diagnosed with a syndrome that increases CVD, stroke, and type 2 diabetes risk. What is the alternate name?
A) Rheumatic syndrome
B) Endocarditis syndrome
C) Insulin resistance syndrome
D) Neurocardiac syndrome
C. Insulin resistance syndrome
Which set contains the five defining risk factors of metabolic syndrome?
A) HTN, hyperglycemia, central obesity, dyslipidemia
B) Fever, murmur, bacteremia, emboli
C) Cyanosis, clubbing, dyspnea, syncope
D) Bradycardia, hypotension, anemia, edema
A. HTN, hyperglycemia, central obesity, dyslipidemia
A patient with acute pericarditis has sharp pain referred to the shoulder. Which pericardial layer and nerve best explain pain transmission?
A) Visceral pericardium; vagus nerve
B) Parietal pericardium; phrenic nerve
C) Epicardium; cervical cardiac nerve
D) Myocardium; thoracic splanchnic nerve
B. Parietal pericardium; phrenic nerve
During cardiac surgery, manipulation of one pericardial layer produces no pain despite direct contact. Which layer is being manipulated?
A) Parietal pericardium
B) Fibrous pericardium
C) Visceral pericardium
D) Pleural pericardium
C. Visceral pericardium
A student traces ventricular depolarization through the heart wall. Which direction best describes normal spread of electrical impulses?
A) Epicardial to endocardial
B) Endocardial to epicardial
C) Apex to venous sinus
D) Pericardial to pleural space
B. Endocardial to epicardial
Which cardiac structures receive both sympathetic and parasympathetic fibers?
A) SA and AV nodes
B) Papillary muscles
C) Coronary valves
D) Ventricular myocardium
A. SA and AV nodes
A lesion selectively disrupts sympathetic cardiac fibers. Which cardiac region would be most affected because it is predominantly sympathetically innervated?
A) Parietal pericardium
B) Ventricular musculature
C) Tracheal bifurcation
D) Visceral pericardium
B. Ventricular musculature
A spinal cord lesion from T1 to T5 disrupts which cardiac neural pathway?
A) Parasympathetic vagal fibers
B) Sympathetic cardiac fibers
C) Phrenic pericardial fibers
D) Visceral pain fibers
B. Sympathetic cardiac fibers
Preganglionic sympathetic fibers to the heart descend to T1-T5 and then synapse where?
A) Thoracic and cervical sympathetic ganglia
B) Medullary cardiovascular nuclei
C) Aortic arch baroreceptors
D) Tracheal bifurcation plexuses
A. Thoracic and cervical sympathetic ganglia
Postganglionic sympathetic fibers reach the cardiac plexus by traveling through which nerves?
A) Vagus nerves
B) Phrenic nerves
C) Cervical cardiac nerves
D) Recurrent laryngeal nerves
C. Cervical cardiac nerves
The cardiac plexus is formed by postganglionic sympathetic fibers joining parasympathetic fibers. Where is it located?
A) Near renal artery bifurcation
B) Near aortic arch and tracheal bifurcation
C) Within the pericardial cavity
D) Below the diaphragm only
B. Near aortic arch and tracheal bifurcation
A brainstem lesion affects areas that normally regulate sympathetic and parasympathetic output to the heart through cardioexcitatory and cardioinhibitory regions. Which structure is involved?
A) Medullary cardiovascular center
B) Cerebellar vermis
C) Hypothalamic thirst center
D) Basal ganglia
A. Medullary cardiovascular center
A patient has a sudden drop in arterial pressure. Which receptor-location pair first detects this change for rapid cardiovascular reflex control?
A) Osmoreceptors; hypothalamus
B) Chemoreceptors; renal cortex
C) Stretch receptors; aortic arch and carotid sinus
D) Pain receptors; parietal pericardium
C. Stretch receptors; aortic arch/carotid sinus
A patient becomes acutely hypotensive after blood loss. How do aortic arch and carotid sinus baroreceptors help raise cardiac output?
A) Increase impulses to medulla
B) Decrease impulses to medulla
C) Increase vagal inhibition
D) Decrease sympathetic output
B. Decrease impulses to medulla
On inspection of the anterior chest, which cardiac chamber forms most of the anterior cardiac surface?
A) Right ventricle
B) Left ventricle
C) Right atrium
D) Left atrium
A. Right ventricle
During a cardiac exam, where should the normal point of maximal impulse usually be palpated?
A) Left 2nd ICS; sternal border
B) Right 4th ICS; midclavicular line
C) Left 5th ICS; midclavicular line
D) Left 3rd ICS; parasternal line
C. Left 5th ICS; midclavicular line
A patient’s PMI is displaced laterally and inferiorly from its usual location. Which interpretation is most appropriate?
A) Normal athletic variant
B) Heart enlargement
C) Aortic valve closure
D) Reduced venous return
B. Heart enlargement
A murmur is difficult to classify as pulmonic versus aortic. Which auscultation site is especially useful for these sounds?
A) Apex
B) Tricuspid area
C) Right 2nd ICS
D) Erb point
D. Erb point
Erb point is located at which auscultation site?
A) Left 3rd intercostal space
B) Right 2nd intercostal space
C) Left 5th midclavicular space
D) Right lower sternal border
A. Left 3rd intercostal space
Which valve closure event produces the first heart sound, S1?
A) Aortic and pulmonic closure
B) Mitral and tricuspid closure
C) Mitral and aortic closure
D) Tricuspid and pulmonic closure
B. Mitral and tricuspid closure
Which valve closure event produces the second heart sound, S2?
A) Aortic and pulmonic closure
B) Mitral and tricuspid closure
C) Mitral and aortic closure
D) Tricuspid and pulmonic closure
A. Aortic and pulmonic closure
A clinician hears a valve opening sound during auscultation. What does this usually imply about that valve?
A) It is physiologically silent
B) It is pathologically damaged
C) It is normally closing
D) It is completely absent
B. It is pathologically damaged
A patient with mitral stenosis has an audible sound shortly after S2. Which term best describes opening of a narrowed AV valve
A) Ejection click
B) Pericardial knock
C) Opening snap
D) Dicrotic notch
C. Opening snap
A patient with aortic stenosis has an audible sound near the start of systole. Which term best describes opening of a damaged semilunar valve?
A) Ejection click
B) Opening snap
C) Third heart sound
D) Venous hum
A. Ejection click
Which timing best matches an opening snap from a pathologically narrowed AV valve?
A) During systole
B) During diastole
C) During atrial repolarization
D) During valve closure
B. During diastole
Which timing best matches an ejection click from a pathologically narrowed semilunar valve?
A) During diastole
B) During passive filling
C) During systole
D) During isovolumetric relaxation
C. During systole
The mitral component of S1, written M1, occurs when which pressure relationship closes the mitral valve?
A) LA pressure exceeds LV pressure
B) Aortic pressure exceeds LV pressure
C) LV pressure exceeds LA pressure
D) RV pressure exceeds RA pressure
C. LV pressure exceeds LA pressure
The tricuspid component of S1, written T1, occurs when which pressure relationship closes the tricuspid valve?
A) RV pressure exceeds RA pressure
B) RA pressure exceeds RV pressure
C) LV pressure exceeds LA pressure
D) Pulmonary pressure exceeds RV pressure
A. RV pressure exceeds RA pressure
Which cardiac-cycle interval occurs between AV valve closure and semilunar valve opening?
A) Systolic ejection
B) Isovolumetric relaxation
C) Rapid ventricular filling
D) Isovolumetric contraction
D. Isovolumetric contraction
The pulmonic valve opens when right ventricular pressure exceeds which pressure?
A) Right atrial systolic pressure
B) Pulmonary artery diastolic pressure
C) Aortic diastolic pressure
D) Left atrial pressure
B. Pulmonary artery diastolic pressure
The aortic valve opens when left ventricular pressure exceeds which pressure?
A) Aortic diastolic pressure
B) Left atrial pressure
C) Pulmonary diastolic pressure
D) Right ventricular pressure
A. Aortic diastolic pressure
Which cardiac-cycle period occurs between semilunar valve opening and semilunar valve closing?
A) Isovolumetric contraction
B) Passive ventricular filling
C) Systolic ejection
D) Isovolumetric relaxation
C. Systolic ejection
On an arterial pressure tracing, ejection ends and the aortic and left ventricular curves separate. What is this point called?
A) Opening snap
B) Dicrotic notch
C) Point of maximal impulse
D) Erb point
B. Dicrotic notch
The incisura/dicrotic notch occurs simultaneously with which event?
A) Mitral valve closure
B) Tricuspid valve opening
C) Aortic valve closure
D) Pulmonic valve opening
C. Aortic valve closure
The aortic component of S2 is written A2 and corresponds to closure of which valve?
A) Aortic valve
B) Pulmonic valve
C) Mitral valve
D) Tricuspid valve
A. Aortic valve
The pulmonic valve closes when right ventricular pressure falls below which pressure?
A) Right atrial pressure
B) Aortic diastolic pressure
C) Left ventricular pressure
D) Pulmonary diastolic pressure
D. Pulmonary diastolic pressure
The pulmonic component of S2 is commonly written as which abbreviation?
A) M1
B) T1
C) A2
D) P2
D. P2
Which cardiac-cycle interval occurs between semilunar valve closure and AV valve opening?
A) Isovolumetric relaxation
B) Isovolumetric contraction
C) Systolic ejection
D) Rapid ejection
A. Isovolumetric relaxation
The tricuspid valve opens when which pressure relationship occurs?
A) RV pressure exceeds RA pressure
B) RA pressure exceeds RV pressure
C) LV pressure exceeds LA pressure
D) Aortic pressure exceeds LV pressure
B. RA pressure exceeds RV pressure
The mitral valve opens when which pressure relationship occurs?
A) LV pressure exceeds LA pressure
B) LA pressure exceeds LV pressure
C) RV pressure exceeds RA pressure
D) Aortic pressure exceeds LV pressure
B. LA pressure exceeds LV pressure
A 58-year-old with mitral regurgitation and congestive heart failure has a low-frequency early diastolic sound. Which heart sound is most associated with adult volume overload from regurgitant lesions or CHF?
A) S4
B) S3
C) Split S1
D) A2
B. S3
A clinician hears a soft sound immediately before S1 during late diastole, when atrial contraction adds the final 10% to 20% of ventricular filling. Which heart sound is this?
A) S2
B) S3
C) S4
D) Opening snap
C. S4
A 23-year-old healthy adult has an S4, while a 55-year-old with the same sound is suspected of having a stiff ventricle. Which interpretation is most accurate?
A) Normal young; abnormal older
B) Always pathologic at all ages
C) Normal older; abnormal young
D) Only caused by regurgitation
A. Normal young; abnormal older
A 62-year-old with long-standing hypertension has a noncompliant ventricle and an S4. Which remodeling pattern best explains this finding?
A) Eccentric hypertrophy
B) Chamber dilation only
C) Ventricular wall thinning
D) Concentric hypertrophy
D. Concentric hypertrophy
Which condition is a major cause of a stiff, noncompliant ventricle associated with S4 in adults older than 30?
A) Coronary heart disease
B) Isolated pulmonic regurgitation
C) Physiologic S2 splitting
D) Perioral cyanosis
A. Coronary heart disease
A clinician is trying to hear splitting of S1. Which auscultation area is most appropriate?
A) Mitral area
B) Aortic area
C) Pulmonic area
D) Tricuspid area
D. Tricuspid area
In normal S2 splitting, which valve closure occurs first?
A) Aortic valve closure
B) Pulmonic valve closure
C) Tricuspid valve closure
D) Mitral valve closure
A. Aortic valve closure
A healthy patient has wider separation between A2 and P2 during inspiration than expiration. Which finding is present?
A) Fixed S2 splitting
B) Paradoxical S2 splitting
C) Physiologic S2 splitting
D) Pathologic S1 splitting
C. Physiologic S2 splitting
Physiologic splitting of S2 is most prominent during which phase of respiration? A) Forced expiration B) Breath holding C) Valsalva release D) Inspiration
D. Inspiration
A healthy person’s heart rate rises slightly during inspiration. Which interpretation is most appropriate? A) Always pathologic B) Normal respiratory variation C) Sign of aortic stenosis D) Evidence of CHF
B. Normal respiratory variation
On an arterial waveform, a positive wave immediately follows the dicrotic notch. What is this wave called?
A) Dicrotic wave
B) Percussion wave
C) Tidal wave
D) Pulse pressure
A. Dicrotic wave
A waveform component occurs during peak velocity of arterial flow and reflects the rate of flow in the artery. Which wave is this?
A) Dicrotic wave
B) Tidal wave
C) Jugular wave
D) Percussion wave
D. Percussion wave
A waveform component occurs during peak systolic pressure and is related to pressure in the vessel. Which wave is this?
A) Dicrotic wave
B) Percussion wave
C) Tidal wave
D) Venous wave
C. Tidal wave
Which definition best describes arterial blood pressure?
A) Venous pressure near right atrium
B) Lateral arterial wall pressure
C) Difference between BP values
D) Stroke volume entering arteries
B. Lateral arterial wall pressure
Systolic blood pressure is best defined as which pressure, and what primarily regulates it?
A) Peak pressure; SV and compliance
B) Lowest pressure; peripheral resistance
C) Mean pressure; venous return
D) Pulse difference; arterial recoil
A. Peak pressure; SV and compliance
Diastolic blood pressure is best defined by which pairing?
A) Peak pressure; stroke volume
B) Pulse difference; vessel compliance
C) Mean pressure; cardiac output
D) Lowest pressure; peripheral resistance
D. Lowest pressure; peripheral resistance
A patient has BP 150/90 mm Hg. Which value represents the pulse pressure?
A) 40 mm Hg
B) 50 mm Hg
C) 60 mm Hg
D) 90 mm Hg
C. 60 mm Hg
A patient lying flat has systolic BP measured in both arms and legs. Which leg-arm systolic difference is normally expected?
A) Legs 5 mm Hg lower
B) Legs 15–20 mm Hg higher
C) Legs equal to arms
D) Legs 40 mm Hg higher
B. Legs 15–20 mm Hg higher
Jugular venous pulse is clinically useful because the jugular venous system is directly continuous with which chamber?
A) Right atrium
B) Left atrium
C) Right ventricle
D) Left ventricle
A. Right atrium
Which bedside finding gives direct information about pressures on the right side of the heart?
A) Carotid pulse contour
B) Point of maximal impulse
C) Radial pulse amplitude
D) Jugular venous pulse
D. Jugular venous pulse
What is the most common cause of right-sided CHF?
A) Primary tricuspid stenosis
B) Isolated pulmonic stenosis
C) Left-sided CHF
D) Pericardial cyst
C. Left-sided CHF
A patient with coronary heart disease reports exertional substernal chest discomfort relieved by rest. What is the true symptom of CHD?
A) Cyanosis
B) Angina pectoris
C) Xanthelasma
D) Pulsus bisferiens
B. Angina pectoris
Which pairing correctly matches heart sound location with where it is loudest?
A) S1 apex; S2 base
B) S1 base; S2 apex
A. S1 apex; S2 base
A 62-year-old with exertional substernal chest pressure has myocardial oxygen demand exceeding coronary supply. Which mechanism best explains angina?
A) Pericardial stretch without ischemia
B) Myocardial hypoxia from supply-demand imbalance
C) Pulmonary venous rupture from stenosis
D) Cerebral hypoperfusion during standing
B. Myocardial hypoxia from supply-demand imbalance
A patient describes chest discomfort by clenching a fist over the sternum. Which classic sign of angina is being demonstrated?
A) Levine sign
B) Kussmaul sign
C) Homan sign
D) Schamroth sign
A. Levine sign
When chest pain is truly cardiac in origin, which two causes are most common?
A) Mitral stenosis and COPD
B) PDA and pulmonary embolism
C) Coronary atherosclerosis and aortic valvular disease
D) Primary biliary cirrhosis and hypertriglyceridemia
C. Coronary atherosclerosis and aortic valvular disease
A patient wakes at night gasping for air and also becomes short of breath when lying supine. Which symptom is this?
A) Orthopnea
B) Platypnea
C) Trepopnea
D) Paroxysmal nocturnal dyspnea
D. Paroxysmal nocturnal dyspnea
A patient reports recurrent nighttime episodes of shortness of breath that force him to sit upright. This symptom is relatively specific for which disease?
A) Familial hypercholesterolemia
B) Congestive heart failure
C) Primary biliary cirrhosis
D) Aortic valvular disease
B. Congestive heart failure
A patient now sleeps with four pillows because lying flat causes dyspnea. Which symptom is being described?
A) Orthopnea
B) Trepopnea
C) Platypnea
D) Posttussive dyspnea
A. Orthopnea
A patient has shortness of breath only during activity. Which paired causes best match dyspnea on exertion?
A) PDA and tendon xanthomata
B) Levine sign and angina
C) Chronic CHF and severe pulmonary disease
D) Carotid sinus hypersensitivity and micturition
C. Chronic CHF and severe pulmonary disease
A patient becomes dyspneic only when lying on the left side but improves on the right side. Which positional dyspnea is this?
A) Platypnea
B) Trepopnea
C) Orthopnea
D) Paroxysmal nocturnal dyspnea
B. Trepopnea
A patient with chronic congestive heart failure reports trepopnea. Which side do these patients usually prefer lying on?
A) Left side
B) Supine
C) Prone
D) Right side
D. Right side
A patient is breathless while upright but improves after lying down. Which symptom is being described?
A) Platypnea
B) Orthopnea
C) Trepopnea
D) Dyspnea on exertion
A. Platypnea
A patient briefly loses consciousness because cerebral blood flow is inadequate, then rapidly recovers. Which term best describes this event?
A) Angina
B) Cyanosis
C) Syncope
D) Orthopnea
C. Syncope
A patient faints after standing and reports dizziness, blurred vision, and profound weakness beforehand. Which mechanism best fits?
A) Bronchial vein rupture
B) Peripheral autonomic limitation
C) Patent ductus arteriosus shunting
D) Tendon lipid deposition
B. Peripheral autonomic limitation
Which symptom cluster best matches orthostatic hypotension
A) Hemoptysis, cyanosis, clubbing
B) PND, orthopnea, edema
C) Dizziness, blurred vision, weakness
D) Chest pain, Levine sign, xanthomas
C. Dizziness, blurred vision, weakness
An older man faints while straining during nighttime urination after heavy alcohol intake. Which syncope type is most likely?
A) Vasovagal syncope
B) Carotid sinus syncope
C) Posttussive syncope
D) Micturition syncope
D. Micturition syncope
Is the most common fainting type and may be caused during sudden, stressful, or painful experiences such as receiving bad news or seeing blood
A) Vasovagal syncope
B) Orthostatic syncope
C) Micturition syncope
D) Posttussive syncope
A. Vasovagal syncope
What syncope is associated with a hypersensitive carotid sinus and is most common in older adults?
A) Posttussive syncope
B) Carotid sinus syncope
C) Vasovagal syncope
D) Orthostatic hypotension
B. Carotid sinus syncope
A patient with carotid sinus hypersensitivity has one subtype causing bradycardia and another causing hypotension without bradycardia. Which pairing is correct?
A) Vasodepressor; cardioinhibitory
B) Posttussive; orthostatic
C) Cardioinhibitory; vasodepressor
D) Micturition; vasovagal
C. Cardioinhibitory; vasodepressor
A patient with COPD faints after a severe coughing spell. Which syncope type is most likely?
A) Carotid sinus syncope
B) Micturition syncope
C) Orthostatic syncope
D) Posttussive syncope
D. Posttussive syncope
A patient with congestive heart failure has ankle swelling that is equal bilaterally and worsens throughout the day. Which finding best matches CHF edema?
A) Symmetric dependent edema
B) Unilateral morning edema
C) Painful digital nodules
D) Lower-extremity cyanosis only
A. Symmetric dependent edema
A patient with mitral stenosis develops hemoptysis. Which mechanism best explains the bleeding?
A) Pulmonary artery rupture
B) Bronchial vein rupture
C) Aortic valve calcification
D) Coronary plaque rupture
B. Bronchial vein rupture
In mitral stenosis, hemoptysis occurs because bronchial veins are exposed to what abnormal condition?
A) Low venous pressure
B) Low lymphatic pressure
C) High back pressure
D) High arterial oxygen
C. High back pressure
A child has cyanosis limited to the lower extremities due to a right-to-left shunt through a persistent fetal vessel. Which diagnosis-linked finding is this?
A) Orthostatic cyanosis from CHF
B) Central cyanosis from COPD
C) Perioral cyanosis from infancy
D) Differential cyanosis from PDA
D. Differential cyanosis from PDA
Differential cyanosis refers to cyanosis isolated to which body region?
A) Lower extremities
B) Upper extremities
C) Face and lips
D) Palms and soles
A. Lower extremities
Stony-hard, slightly yellowish masses are found on the extensor tendons of the fingers. Which association is most important?
A) Infective endocarditis
B) Familial hypercholesterolemia
C) Preeclampsia D) Mitral stenosis
B. Familial hypercholesterolemia
Which locations are common sites for tendon xanthomata besides finger extensor tendons?
A) Retina and conjunctiva
B) Palms and soles
C) Achilles and plantar tendons
D) Bronchial and pulmonary veins
C. Achilles and plantar tendons
A rare, progressive, often fatal liver disease occurs primarily in females and may be associated with lipid skin findings. Which disease is this?
A) Primary biliary cirrhosis
B) Rheumatic heart disease
C) Bacterial endocarditis
D) Congestive heart failure
A. Primary biliary cirrhosis
A 54-year-old woman with cholestatic liver disease has positive anti-mitochondrial antibodies. Which diagnosis is most strongly supported by this antibody pattern?
A) Infective endocarditis
B) Primary biliary cirrhosis
C) Acute rheumatic fever
D) Familial hypertriglyceridemia
B. Primary biliary cirrhosis
A patient with primary biliary cirrhosis and markedly elevated cholesterol has multiple nodular yellow lesions on the hand. Which skin finding is most likely being shown?
A) Tuberous xanthomata
B) Osler nodes
C) Erythema marginatum
D) Splinter hemorrhages
A. Tuberous xanthomata
A child has sudden crops of yellow papules in the setting of a familial fat metabolism disorder. Which lipid disorder types are classically associated with eruptive xanthomata?
A) Types II and III
B) Types III and V
C) Types I and IV
D) Types II and IV
C. Types I and IV
A febrile child has disc-shaped erythematous lesions with raised edges after untreated streptococcal pharyngitis. Which diagnosis is suggested?
A) Infective endocarditis
B) Primary biliary cirrhosis
C) Familial hypercholesterolemia
D) Acute rheumatic fever
D. Acute rheumatic fever
A patient has erythema with reddened disc-shaped areas and raised borders. Which term best describes this rash?
A) Janeway lesions
B) Erythema marginatum
C) Eruptive xanthomata
D) Palatal petechiae
B. Erythema marginatum
A child with wide-set eyes, strabismus, low-set ears, upturned nose, and mandibular hypoplasia should be evaluated for which cardiac lesion?
A) Mitral valve prolapse
B) Pulmonic regurgitation
C) Coarctation of aorta
D) Supravalvular aortic stenosis
D. Supravalvular aortic stenosis
Williams-Beuren Syndrome, often referred to as "elfin facies"
A child with moon facies and widely spaced eyes is being screened for congenital heart disease. Which lesion is particularly associated?
A) Pulmonic stenosis
B) Aortic regurgitation
C) Mitral stenosis
D) Tricuspid stenosis
A. Pulmonic stenosis
A patient with expressionless facies, puffy eyelids, and loss of the outer third of the eyebrow may develop which cardiac complication?
A) Infective endocarditis
B) Cardiomyopathy
C) Aortic coarctation
D) Rheumatic carditis
B. Cardiomyopathy
A 62-year-old with an oblique bilateral earlobe crease is found to have significant coronary disease. Which sign is this?
A) Levine sign
B) Schamroth sign
C) Lichstein sign
D) Roth sign
C. Lichstein sign
A patient has soft yellow plaques on the eyelids. Which associated disorder should be considered, although the finding is less specific than xanthoma?
A) Hyperlipoproteinemia
B) Acute rheumatic fever
C) Cor pulmonale
D) Aortic coarctation
A. Hyperlipoproteinemia
A 32-year-old has a corneal arcus on eye exam. Which condition should this raise suspicion for?
A) Primary biliary cirrhosis
B) Hypercholesterolemia
C) Pulmonic stenosis
D) Infective endocarditis
B. Hypercholesterolemia
A clinician notes a bluish ring around an older patient’s cornea. Which term best describes this finding?
A) Roth spot
B) Xanthelasma
C) Arcus senilis
D) Hypertelorism
C. Arcus senilis
A patient has corneal opacities from sarcoidosis. Which cardiovascular-pulmonary complications should be considered
A) Cor pulmonale or myocardial involvement
B) Coarctation or aortic dissection
C) Rheumatic fever or mitral stenosis
D) Endocarditis or palatal petechiae
A. Cor pulmonale or myocardial involvement
A tall patient with lens displacement is evaluated for a cardiac murmur. Which syndrome and valve lesion are most associated?
A) Turner; coarctation
B) Noonan; pulmonic stenosis
C) Marfan; aortic regurgitation
D) Ehlers-Danlos; mitral stenosis
C. Marfan; aortic regurgitation
A patient with fever and a new murmur has conjunctival hemorrhages on exam. Which diagnosis is most strongly suggested?
A) Primary biliary cirrhosis
B) Infective endocarditis
C) Familial hypercholesterolemia
D) Hypothyroid cardiomyopathy
B. Infective endocarditis
A child with hypertelorism is being screened for congenital heart disease. Which lesions are especially associated?
A) MVP and mitral stenosis
B) AR and coarctation
C) Pulmonic and supravalvular AS
D) PDA and tricuspid stenosis
C. Pulmonic and supravalvular AS
A patient with a high-arched palate is being evaluated for congenital cardiac abnormalities. Which association is most likely?
A) Aortic stenosis
B) Mitral valve prolapse
C) Pulmonic regurgitation
D) Tricuspid atresia
B. Mitral valve prolapse
A patient with fever, new murmur, and small hemorrhagic lesions on the palate is suspected of having which diagnosis?
A) Acute rheumatic fever
B) Primary biliary cirrhosis
C) Infective endocarditis
D) Coarctation of aorta
C. Infective endocarditis
A girl with short stature and webbed neck is found to have upper-extremity hypertension. Which associated lesion is most likely?
A) Pulmonic stenosis
B) Mitral valve prolapse
C) Aortic regurgitation
D) Coarctation of aorta
D. Coarctation of aorta
A child with webbed neck but normal female karyotype is suspected of Noonan syndrome. Which cardiac lesion is classically associated?
A) Pulmonic stenosis
B) Aortic regurgitation
C) Mitral stenosis
D) Tricuspid regurgitation
A. Pulmonic stenosis
A patient with pectus excavatum is evaluated for associated cardiac connective-tissue findings. Which association is most accurate?
A) Turner; coarctation
B) Marfan; mitral valve prolapse
C) Noonan; aortic regurgitation
D) PBC; pulmonic stenosis
B. Marfan; mitral valve prolapse
A patient with pectus carinatum has features of a connective tissue disorder. Which syndromic association is most accurate
A) Marfan and Ehlers-Danlos
B) Turner and Noonan
C) PBC and sarcoidosis
D) Rheumatic fever and CHD
A. Marfan and Ehlers-Danlos
A child with a suspected congenital heart defect has an extra phalanx and polydactyly on exam. Which cardiac lesion is most associated with these limb findings?
A) Pulmonic stenosis
B) Atrial septal defect
C) Mitral valve prolapse
D) Aortic regurgitation
B. Atrial septal defect
A tall patient with long, slender fingers has a diastolic murmur consistent with aortic regurgitation. Which syndrome is most suggested?
A) Turner syndrome
B) Noonan syndrome
C) Down syndrome
D) Marfan syndrome
D. Marfan syndrome
A girl has short stature, cubitus valgus, and medial deviation of the extended forearm. Which syndrome best matches these findings?
A) Turner syndrome
B) Marfan syndrome
C) Noonan syndrome
D) Ehlers-Danlos syndrome
A. Turner syndrome
During BP measurement, Korotkoff sounds disappear after initially appearing and then reappear at a lower pressure. What is this silence called?
A) Pulse deficit
B) Paradoxical pulse
C) Auscultatory gap
D) Dicrotic notch
C. Auscultatory gap
A child has supravalvular aortic stenosis. Which interarm BP pattern may be detected?
A) Equal pressures bilaterally
B) Right high; left low
C) Left high; right low
D) Both arms hypotensive
B. Right high; left low
A child with coarctation is evaluated for associated congenital cardiac lesions. Which pair is most classically associated?
A) ASD and pulmonic stenosis
B) MVP and tricuspid stenosis
C) PDA and mitral stenosis
D) Bicuspid aortic valve and VSD
D. Bicuspid aortic valve and VSD
A child has elevated blood pressure in both arms. Which additional measurement is essential to help rule out coarctation of the aorta?
A) Jugular venous pressure
B) Apical pulse only
C) Lower-extremity blood pressure
D) Hepatojugular reflex
C. Lower-extremity blood pressure
A trauma patient develops pericardial fluid accumulation, impaired diastolic filling, low cardiac output, and shock. Which condition is present?
A) Pulmonary hypertension
B) Cardiac tamponade
C) Cardiomegaly
D) Auscultatory gap
B. Cardiac tamponade
A patient with suspected cardiac tamponade has an exaggerated inspiratory fall in systolic blood pressure. Which clinical sign is being described?
A) Pulse deficit
B) Dicrotic wave
C) Right ventricular rock
D) Paradoxical pulse
D. Paradoxical pulse
A patient with an irregularly irregular rhythm has fewer radial pulses than apical beats. What does this difference represent
A) Auscultatory gap
B) Paradoxical pulse
C) Pulse deficit
D) Physiologic splitting
C. Pulse deficit
The hepatojugular reflex is performed during a cardiac exam to estimate which aspect of cardiac function?
A) Left atrial size
B) Right ventricular function
C) Aortic valve mobility
D) Coronary blood flow
B. Right ventricular function
A positive hepatojugular reflex correlates best with pulmonary artery wedge pressure and indicates which hemodynamic state?
A) Decreased venous return
B) Reduced central blood volume
C) Increased central blood volume
D) Isolated peripheral vasodilation
C. Increased central blood volume
A patient’s PMI is laterally displaced and palpable in two interspaces during the same respiratory phase. Which finding is suggested?
A) Cardiomegaly
B) Pulmonary stenosis
C) Atrial septal defect
D) Cardiac tamponade
A. Cardiomegaly
A clinician compares ventricular apical impulses. Which distinction is most accurate?
A) RV localized; LV diffuse
B) RV absent; LV diffuse
C) RV diffuse; LV localized
D) RV systolic; LV diastolic
C. RV diffuse; LV localized
A systolic impulse is palpated in the second intercostal space just left of the sternum. Which condition should be suspected?
A) Mitral stenosis
B) Aortic regurgitation
C) Pulmonary hypertension
D) Pericardial tamponade
C. Pulmonary hypertension
A sustained left parasternal impulse with lateral retraction is described as a right ventricular rock. What does it suggest?
A) Enlarged right ventricle
B) Small left ventricle
C) Aortic valve stenosis
D) Normal apical impulse
A. Enlarged right ventricle
A systolic murmur is accompanied by a palpable thrill. What minimum murmur grade does this imply on a I–VI scale?
A) Grade II or higher
B) Grade III or higher
C) Grade IV or higher
D) Grade VI only
C. Grade IV or higher
A murmur becomes louder with inspiration. Which origin is most likely?
A) Left-sided heart sound
B) Right-sided heart sound
C) Pericardial friction rub
D) Aortic arch bruit
B. Right-sided heart sound
A murmur begins with S1 and continues throughout systole until S2. Which term best describes it?
A) Early diastolic murmur
B) Systolic ejection murmur
C) Holosystolic murmur
D) Opening snap
C. Holosystolic murmur
Which alternative term is commonly used for a murmur that occurs throughout systole?
A) Pansystolic murmur
B) Presystolic murmur
C) Protodiastolic murmur
D) Continuous murmur
A. Pansystolic murmur
A murmur begins after S1 and ends immediately before S2 rather than occupying all of systole. Which murmur type is this
A) Opening snap
B) Systolic ejection murmur
C) Holosystolic murmur
D) Diastolic rumble
B. Systolic ejection murmur
A murmur begins after S2 and persists through the entire diastolic interval until S1. Which term best describes this murmur?
A) Holosystolic
B) Crescendo-decrescendo
C) Holodiastolic
D) Midsystolic
C. Holodiastolic
A clinician describes a murmur as rumbling, blowing, harsh, musical, machinery-like, or scratchy. Which murmur feature is being characterized?
A) Quality
B) Timing
C) Radiation
D) Intensity
A. Quality
A clinician suspects a pericardial friction rub. Which maneuver best helps auscultate this sound?
A) Supine during inspiration
B) Standing after squatting
C) Left lateral after exercise
D) Sitting, expiration breath-hold
D. Sitting, expiration breath-hold
A scratching chest sound disappears when the patient holds their breath in expiration. Which origin is most likely?
A) Pericardial
B) Pleural
C) Valvular
D) Carotid
B. Pleural
A healthy patient’s A2–P2 separation during inspiration is being evaluated. Where is physiologic S2 splitting best heard?
A) Mitral area, sitting forward
B) Tricuspid area, standing upright
C) Pulmonic area, lying supine
D) Aortic area, left lateral
C. Pulmonic area, lying supine
Why does lying supine help widen the A2–P2 split during inspiration?
A) Increases venous return
B) Decreases pulmonary return
C) Delays aortic closure
D) Shortens right ventricular systole
A. Increases venous return
A patient has variable loudness of S1 between beats. Which factor most directly affects S1 intensity?
A) Pulmonary artery pressure
B) Valve position at contraction
C) Aortic wall compliance
D) Respiratory phase only
B. Valve position at contraction
The angle through which an AV valve closes during ventricular contraction is called what?
A) Valve excursion angle
B) Annular recoil angle
C) Commissural tension angle
D) Arc of coaptation
D. Arc of coaptation
A patient has systemic hypertension with forceful semilunar valve closure. Which heart sound change is expected?
A) Increased S2 intensity
B) Decreased S1 intensity
C) Fixed S2 splitting
D) Opening snap
A. Increased S2 intensity
Calcification and fibrosis of aortic and pulmonic valves would most directly produce which auscultatory effect?
A) Louder valve opening
B) Louder S1 closure
C) Softer S2 closure
D) Fixed S2 splitting
C. Softer S2 closure
A patient with right bundle branch block has delayed right ventricular systole. Which S2 finding is expected?
A) Paradoxical splitting
B) Widened splitting
C) Fixed splitting
D) Single S2
B. Widened splitting
A condition shortens left ventricular systole so A2 occurs earlier than normal. Which S2 pattern results?
A) Fixed splitting
B) Single S2
C) Paradoxical splitting
D) Wide splitting
D. Wide splitting
A patient has delayed left ventricular emptying from severe aortic stenosis. Which S2 splitting pattern is expected?
A) Paradoxical splitting
B) Fixed splitting
C) Physiologic splitting
D) Normal wide splitting
A. Paradoxical splitting
A child has a fixed split S2 that does not vary with respiration. Which lesion is classically associated?
A) Ventricular septal defect
B) Atrial septal defect
C) Mitral regurgitation
D) Aortic stenosis
B. Atrial septal defect
A high-pitched sound occurs early in systole at the onset of ejection from a deformed aortic valve. Which sound is this?
A) Opening snap
B) Midsystolic click
C) Pericardial rub
D) Ejection click
D. Ejection click
Ejection clicks are produced by opening of pathologically deformed valves in which valve class?
A) AV valves
B) Venous valves
C) Semilunar valves
D) Coronary valves
C. Semilunar valves
A midsystolic click is heard in a patient with valve prolapse. Which valves are most associated with this sound?
A) Mitral or tricuspid
B) Aortic or pulmonic
C) Pulmonic or tricuspid
D) Aortic or mitral
A. Mitral or tricuspid
A patient with mitral stenosis has a sharp sound shortly after S2 due to abnormal valve opening. Which sound is present?
A) Ejection click
B) Opening snap
C) Dicrotic notch
D) Midsystolic click
B. Opening snap
An opening snap is best described as which valve event?
A) Systolic semilunar closure
B) Diastolic semilunar opening
C) Systolic AV closure
D) Diastolic AV opening
D. Diastolic AV opening
A murmur is described as “blowing.” Which hemodynamic pattern most likely produces this quality?
A) Large gradient, variable flow
B) Small gradient, flow-dependent
C) Large gradient, high flow
D) Low pressure, no turbulence
A. Large gradient, variable flow
A murmur is described as “rumbling.” Which hemodynamic pattern best explains this quality?
A) Large gradient, high flow
B) Large gradient, variable flow
C) Small gradient, flow-dependent
D) Semilunar valve ejection
C. Small gradient, flow-dependent
A murmur is described as “harsh.” Which hemodynamic pattern best explains this quality?
A) Small gradient, slow flow
B) Low gradient, low flow
C) Variable flow, no gradient
D) Large gradient, high flow
D. Large gradient, high flow
A crescendo-decrescendo systolic murmur is produced by turbulence across the aortic valve during systole. Which murmur category is this?
A) Diastolic AV murmur
B) Systolic ejection murmur
C) Regurgitant systolic murmur
D) Holodiastolic murmur
B. Systolic ejection murmur
A patient has mitral regurgitation with retrograde flow from the left ventricle to left atrium during systole. Which murmur type is expected?
A) Regurgitant systolic murmur
B) Systolic ejection murmur
C) Diastolic AV murmur
D) Opening snap
A. Regurgitant systolic murmur
Regurgitant systolic murmurs such as mitral or tricuspid regurgitation usually have which timing?
A) Early diastolic only
B) Midsystolic only
C) Holosystolic or pansystolic
D) Late diastolic only
C. Holosystolic or pansystolic
A murmur begins after S2 when a narrowed mitral valve opens during ventricular filling. Which murmur type is this?
A) Systolic ejection murmur
B) Regurgitant systolic murmur
C) Holosystolic murmur
D) Diastolic AV murmur
D. Diastolic AV murmur