What is the difference between anabolism and catabolism?
Anabolism uses raw material to synthesize essential compounds and catabolism decomposes substances to provide energy cells need to function.
2. What two essential ingredients are required in catabolic reaction?
2. Oxygen and broken down organic molecules
What are organic molecules broken down by?
Intracellular enzymes
What are two other names for the digestive tract?
Gastrointestinal tract (GI) and alimentary canal
What is the distance of the digestive tract? What all does it pass through?
Oral cavity to anus; pharynx, esophagus, stomach, and small and large intestines
What are the six functions of the digestive system?
Ingestion, mechanical processing, digestion, secretion, absorption, and excretion
What is ingestion? When does it occur?
Bringing food in; when materials enter Digestive tract
What is mechanical processing?
The crushing and shearing
Where does digestion occur? What is it?
Stomach; chemical breakdown of food for absorption
What is secretion? How are thing secreted in the digestive tract?
Release of water, acids, enzymes, buffers, and salts; by epithelium and glandular organs
What occurs in absorption?
Organic substances move
What occurs in excretion?
Materials are removed
What do visceral smooth muscle cells rely on? Why?
Self-communication; lack direct connection with motor neuron
How are visceral smooth muscle cells arranged? How are they connected?
Sheets or layers; electronically by gap junction and mechanically by dense bodies
What kind of stimulation can visceral smooth muscle cells have? How are some stimulated?
Neural, hormonal, or chemical; pacesetter cells
Where are some visceral smooth muscle cells located?
Digestive tract walls, gallbladder, bladder, etc.
What does the plasticity of smooth muscle important for?
Allows organs to adapt shape and still contract
What is smooth muscle tone?
Normal background activity and tension due to various stimulations
What are the two types of movement and regulations of the digestive tract?
Peristalsis and segmentation
What is peristalsis?
Wave of muscle contraction that propel bolus through digestive tract
What is segmentation? Where does it occur?
Cycles of contraction that churn & fragment bolus; In many areas of small intestine & some of large
What is the primary stimulus for digestive activity?
Local factors
What are the short reflexes of neurons controlled by?
Myenteric plexus
What are long reflexes of neurons controlled by?
Interneurons and motor neurons
What are the primary stimulus types for digestive activities?
pH of lumen; physical distortion of DT wall, and presence of chemicals
What kinds of hormones control the digestive tract and where are they produced?
Peptides; enteroendocrine cells within epithelium
What are mesenteries? What two things do they do?
Double sheet of peritoneal membrane; provides access route for blood vessels, nerves, and lymphatic vessels- also stabilizes position of attached digestive organs
What does the peritoneal cavity do?
Encloses stomach and most of the intestines
What is the peritoneal cavity lined with? What are the parts of it? What does it secrete and why?
Serous peritoneum; parietal and visceral; peritoneal fluid to lubricate organs
What are the two mesenteries that exist during development?
Dorsal and ventral
What does the dorsal become?
Greater omentum, mesentery proper, & mesocolon
What does the ventral become?
Lesser omentum and falciform ligament
Which is more efficient in propelling intestinal content from one place to another: peristalsis or segmentation?
Peristalsis
What effect would a drug that blocks parasympathetic stimulation of the digestive tract have on peristalsis?
It would slow it down because the muscle tone would be increased
where does the majority of digestion happen?
stomach
what materials are found in the stomach? what do they create?
food, saliva, and gastric gland secretions; chyme
what are the regions found in the stomach?
fundus, cardia, body, and pylorus
where is the fundus found?
superior to esophageal connection
what does the cardia do and why?
secrete mucus to protect esophagus from acid/enzymes
what is the largest portion of the stomach?
body
what leads to the small intestine in the stomach?
pylorus
where is the lesser curvature found?
medal surface
where is the greater curvature found?
lateral and inferior surfaces
what is found in addition to circular and longitudinal layers in muscularis externa?
oblique muscle layer
what are rugae and what do they allow?
mucosal wrinkles that flatten when stomach fills; they allow muscles to expand
what are the pyloric structures?
pyloric antrum, pyloric canal, and pyloric sphincter
what portion of the pylorus is a smooth muscle band that regulates release of chyme into duodenum?
pyloric sphincter
what portion of the pylorus is empties into small intestine?
pyloric canal
what portion of the pylorus is connected the stomach body?
pyloric antrum
what do gastric glands secrete? where do gastic glands open? what do the stem cell at the neck do?
most of the acid and enzymes enabling gastric digestion; to stomach luman through gastric pits; replace cells lost into chyme
what do parietal cells secrete? what are these secretions used for?
intrinsic factor- B12 absorption; HCl- activates pepsinogen to keep stomach at pH~2
what do chief cells secrete? what does this secretion do?
pesinogen; becomes pepsin when activated
what is pepsin?
active proteolytic enzyme
what tow things are also secreted in infant? why?
rennin and gastric lipase to aid in digestion of milk
what are G cells? what do they produce?
enteroendocrine cells; variety of hormones
how is HCl produced?
carbonic anhydrace is sued to create bicarbonate ions and hydrogen ions from CO2 and H2O
where is hydrogen released in HCl production? what else is released here?
into gastric gland lumen; chloride
what happens to the bicarbonate? what is formed?
transported into blood; alkaline tide
what can production of acid and enzymes by the gastric mucosea be controlled/regulated by?
controlled by CNS regulated by short reflexes of ENS and hormones of digestive tract
what are the three phases of gastric control?
cephalic, gastric, and intestinal
what do many intestinal structures do?
add surface area to increase aborption
what are permanent transverse folds found mostly in the jejunum called?
plicae curcularis
what are cell membreane extensions on simple columnar cell linings of villi surfaces called?
microvilli
what are fingerlike projections on the mucosa called?
intestinal villi
what do these three things do together?
add 600 times more area for absorption compared to smooth, flat walls
where does 90% of absorption occur? where does the other 10% occur?
small intestine; large intestine
what are the three regions of the intestine?
duodenum, jejunum, and IIeum
describe the duodenum.
receives chyme from the stomach and digestive secretions from the liver, gallbladder and pancreas; mostly retroperitoneal; few pilcae circulari and small vili; many duodenal glands secreting mucus
what I the duodenum's main function?
neutralizes acidic chyme
describe and give the location of the jujunum. what happens here?
has numerous pilicae circularis and abundant, long vili; majority of chemical digestion and nutrient absorption
why does the IIeum have few pilicae curculare and stumpy vili?
not much absorption occurs here.
what does the iieum's submucosa contain? what does the iieum control?
aggregated lymphoid modules; material clow into cecum of large intestine
which four of the five major hormones that regulate digestive activities are produced by the duodenum?
gastrin, secretin, gastric inhibitory peptide,and cholecystokinin
are equal amounts of the hormones secreted every meal?
no only the amount needed of each is used
what is gastrin secreted by? where is this located?
secreted by G cells in the pyloric antrium and enteroendocrine cells of the duodenum
what stimulates gastrin particularly? what does it do?
food in the stomach and duodenum with high protein content; increases stomach mobility and production of gastric acids and enzymes
when is secretin released from the duodenum? what does it do?
when chyme arrives; increases secretion of bile from liver and buffers from pancreas. also decreases gastric motility and secretory rates. (neutralizes pH also)
which hormone is released by the duodenum when fats and carbohydrates enter the small intestine and inhibits gastric activity while increasing insulin release? what are secondary effects of this hormone?
gastric inhibitory peptide (GIP); stimulating duodenal glands, stimulating lipid synthesis in adipose, and increased skeletal muscle use
which hormone is released by the duodenum are secrete when chyme arrives especially when it is high in lipids and partially digested proteins? what does this hormone do?
cholecystokinin; increase enzyme production and secretion from pancreas and bile from gallbladder. also inhibits gastric activity and may reduce hunger sensation is CNS
regulation of gastric activity image

what are thew two central gastric reflexes? what are they under control by?
gastroenteric reflex and gastroileal reflex; under autonomic control
which gastric reflex increases motility secretion?
gastroenteric reflex
which gastric reflex triggers opening of ileocecal valve allowing passage of materials from small to large intestine?
gastroileal reflux
what are the major functions of the large intestine during peristalsis?
1. reabsorption of water and compaction of content into feces. 2. absorption of inportant vitimins liberated by bacterial action and 3. storage of feces prior to defication
what arethe three segments of the large intestine?
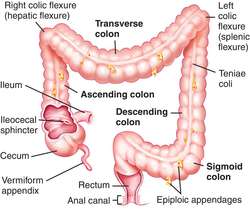
cecum, colon, and rectum
what does the cecum begin? what does it contain and what is attached to it?
compaction; contains ileocecal valve and has an appendix attached.
what does the appendix contain? what is the inflammation of the appendix called?
numerous lymphoid nodules; appendicitis
what are the four parts of the colon?
ascending, transverse, descending, and sigmoid
why is the rectum expandable? what triggers defecation urge?
for feces storage; fecal material within rectum
what are large intestine characteristics associated with fecal production?
diameter is larger and wall is thinner that small intestines, lack of villi, abundance of mucous cells, many intestinal glands dominated by mucous glands; and no digestive enzymes produced
what does mucus do in the large intestine?
provides lubercation for drier ad more compact fecal matter
which anal sphincter is voluntary? which is involuntary?
external; iternal
what two positive feedback loops are involved in defecation reflexes?
long and short
which reflex is coordinated by the sacral parasympathetic system and stimulates mass movement into feces?
long reflex
what is the other reflex responsible for?
stimulation of myeneric plexus to move feces in sigmoid colon and rectum
what are the major accessory digestive organs and what do they do?
*salivary glands-produce saliva with mucins and enzymes
gallbladder- store and concentrate bile
*pancreas- exocrine cells secrete buffers and digestive enzymes
*liver- many functions (200+)
*-also have vital metabolc and endocrine function
what is the larges visceral organ?
liver
how many lobes does the liver have and what are they?
4- left, right,caudate, and quadrate
what separates the left and right lobe ? what surrounds bare area? what marks fecal umbilical vein path?
falciform ligament; coronary ligament extension; round ligament
what separates left lobe and caudate lobe?
inferior vena cava
where is the quadrate lobe?
between the left lobe and gallbladder
what are the structures associated with the liver

gallbladder, common bile duct, and porta hepatis
what does the gallbladder do in association with the liver?
stores bile it produces temporarily
what does the common bile duct do?
carries bile from the liver and gallbladder to duodenum
what does the porta hepatis' function?
entry point for blood vessels and other structures from lesser omentum
what are the lobules of the liver separated by?
interlobular septa
what is in the corner of each lobule
a portal area or triad
what makes up the portal area?
branch of portal vein, branch of hepatic artery, and branch of bile duct
what ate the liver lobules composed of?
hepatocytes (liver cells)
what are liver sinusoids? where do they drain?
blood vessel with nutrients and solutes and are regulated by hepatocytes central vein
what else is found within the liver lobules?
phagocytic kupffer cells
give the steps of bile movement in the liver after it is secreted.
secreted bile drains into bile canaliculi then bile ductules then bile ducts of the portal triad
what is an effect if alcoholism and hepatitis?
degenerative changes in liver and constriction of blood supply
what can increased pressure die to clot or damage create? what are some things this may lead to?
portal hypertension; vessel distension and rupture or ascities due to serous fluid leakage
what are the three regions of the gallbladder?
fundus, body and neck
where does the gallbladder drain fluid?
cystic duct
what does the cystic duct merge with and what does it create
right and left common hepatic duct of liver to become common bile duct
besides storing bile, what else does the gallbladder do?
concentrate it
when and where is the bile released? what hormone controls it?
at mealtime into duodenum when hepatopancreatic sphinter is relaxed; CCK
what doe bile salts do? what is this process called?
break lipid droplets apart; emulsification
where is the pancreas
posterior to the stomach
what are the three parts of the pancreas?
head body and tail
what does the pancreatic duct meet and where? what does it do?
common bile duct at duodenal papilla and drains pancreatic juice into duodenum
what occurs in 3% to 10% of people
accessory pancreatic duct
what are pancreatic acini? what do they secrete?
organizational units made from pancreatic aciner cells; pancreatic enzymes
what can peridontal disease cause?
gingivitis, tooth decay, and tooth loss
what is mumps? where is it usually?
infection of salivary glands; parotid salivary gland
what other organs can mumps affect?
gonads and meninges
what is esophagitis usually caused by?
escaping stomach acids (GERD)
what can cause hepatitis?
drugs, alcohol, or infection
what is cirrhosis?
replacement of hepatocytes with scar tissue
what do the hepatitis viruses do?
destroy the liver cells
what causes the yellowness if skin and eyes with juandice?
accumulation of bilirubin
what are gallstones?
crystals of insoluble minerals and salts forming when bile becomes too concentrated.
what causes cholecystitis?
when gallstones block cystic duct
what can cause pancreatitis? where is it normally found?
duct blockage, viral infection, or toxic drugs; dogs
what are two types of peptic ulcers?
gastric and duodenal
what are over 80% of ulcers caused by? what are treatments for ulcers?
infection of helicobactor pylori bacterium; acid reducers or antibiotics for h. pylori if present.
what is what cause of enteritis and what does this disease cause?
infection by hiardia lamblia; diarrhea
what is dysentery and what does it cause?
inflammation of small and large intestine and causes bloody diarrhea
what gastritis?
inflammation of stomach lining
what is gastroenteritis? what causes it and where is it ususally found?
inflammation of stomach lining and intestine; pathogenic infection and found often in areas with poor sanitation and low water quality
what causes the diarrhea or constipation associated with colitis?
d- too much fluid or absorption capabilities compromised
c- excess water reabsorption due to slow moving feces
what people are more susceptible to colerectal cancer? what does this disease begin as?
people over 50 with diets that are high in animal fat and low in fiber; small localized tumors. (polyps)