1) The urinary system does all of the following except
A)
excreting excess albumin molecules.
B) regulating blood
volume.
C) helping to stabilize blood pH.
D) eliminating
organic waste products.
E) regulating plasma concentrations of electrolytes.
A) excreting excess albumin molecules.
2) Functions of the urinary system include all of the following
except
A) regulation of blood volume and blood pressure.
B)
regulation of plasma concentration of certain ions.
C) helping to
stabilize blood pH.
D) conservation of valuable
nutrients.
E) storage of fat-soluble vitamins.
E) storage of fat-soluble vitamins.
3) The urinary function of elimination occurs through the
A)
liver.
B) glomerulus.
C) kidney.
D) ureter.
E) urethra.
E) urethra.
4) Urine is carried to the urinary bladder by
A) blood
vessels.
B) lymphatics.
C) the ureters.
D) the
urethra.
E) the calyces.
C) the ureters.
5) Each of the following organs is part of the urinary system except
the
A) kidney.
B) urinary bladder.
C) rectum.
D)
ureter.
E) urethra.
C) rectum.
6) Urine is temporarily stored in the
A) urethra.
B)
urinary bladder.
C) kidney.
D) ureter.
E) trigone.
B) urinary bladder.
7) Urine is carried from the urinary bladder to the outside of the
body by the
A) urethra.
B) glomerulus.
C) convoluted
tubule.
D) ureter.
E) collecting duct.
A) urethra.
8) Which of the following activities is not related to kidney
function?
A) control of hydrogen ion and pH in the blood
B)
control of wastes in the blood
C) lipid digestion
D)
regulation of blood pressure
E) maintenance of various blood ion concentrations
C) lipid digestion
9) The excretory functions of the urinary system are performed by
the
A) urethra.
B) ureters.
C) glomerulus.
D)
urinary bladder.
E) kidneys.
E) kidneys.
10) When the bladder is full, urine is eliminated through the process
known as
A) beta-oxidation.
B) defecation.
C)
emesis.
D) micturition.
E) segmentation.
D) micturition.
11) A glomerulus is
A) the expanded end of a nephron.
B) a
knot of capillaries within the renal corpuscle.
C) the source of
erythropoietin.
D) attached to the collecting duct.
E) the
horseshoe-shaped segment of the nephron.
B) a knot of capillaries within the renal corpuscle.
12) All of the following are true of the kidneys except that they
are
A) located in a position that is retroperitoneal.
B)
surrounded by a fibrous capsule.
C) located partly within the
pelvic cavity.
D) held in place by the renal fascia.
E)
covered by peritoneum.
C) located partly within the pelvic cavity.
13) The prominent indentation on the medial surface of the kidney is
the
A) calyx.
B) pelvis.
C) ureter.
D)
hilum.
E) pyramid.
D) hilum.
14) The renal sinus is
A) the innermost layer of kidney
tissue.
B) part of a renal pyramid.
C) an internal cavity
lined by the fibrous capsule.
D) a large branch of the renal
pelvis.
E) a renal corpuscle.
C) an internal cavity lined by the fibrous capsule.
15) The outermost layer of the kidney is the
A) renal
cortex.
B) renal medulla.
C) major calyx.
D) fibrous
capsule.
E) renal pelvis.
D) fibrous capsule.
16) The cavity of the kidney that receives urine from the calyces is
called the
A) renal papilla.
B) renal pelvis.
C) renal
medulla.
D) renal cortex.
E) renal sinus.
B) renal pelvis.
17) Blood leaves the glomerulus through a blood vessel called
the
A) afferent arteriole.
B) efferent arteriole.
C)
vasa recta.
D) interlobular arteriole.
E) renal vein.
B) efferent arteriole.
18) The condition called ________ is especially dangerous because the
ureters or renal blood
vessels can become twisted or kinked
during movement.
A) polycystic kidney disease
B) floating
kidney
C) pyelonephritis
D) renal calculi
E) renal failure
B) floating kidney
19) The ________ delivers urine to a minor calyx.
A) nephron
loop (loop of Henle)
B) distal convoluted tubule
C)
papillary duct
D) renal corpuscle
E) ureter
C) papillary duct
20) Typical renal blood flow is about ________ ml/min under resting
conditions.
A) 500
B) 800
C) 1200
D) 1800
E) 2500
C) 1200
21) In the renal corpuscle, the visceral layer is a layer of
specialized cells called
A) glomerulocytes.
B)
juxtaglomerular cells.
C) tubular cells.
D) macula densa
cells.
E) podocytes.
E) podocytes.
22) What is the proper order for the structures of the renal
corpuscle through which a substance travels during filtration?
1.
filtration slit (slit pore)
2. capsular space
3. basement
membrane
4. fenestrated endothelium
A) 4, 3, 2, 1
B) 4,
1, 2, 3
C) 4, 3, 1, 2
D) 3, 1, 4, 2
E) 2, 4, 3, 1
C) 4, 3, 1, 2
23) Capillaries that surround the proximal convoluted tubules
are
A) proximal capillaries.
B) corticoradiate
capillaries.
C) vasa recta capillaries.
D) efferent
arterioles.
E) peritubular capillaries.
E) peritubular capillaries.
24) ________ is/are an inflammatory disorder of the glomeruli that
affects the filtration mechanism of the kidneys.
A)
Glomerulonephritis
B) Floating kidney
C) Polycystic kidney
disease
D) Pyelonephrosis
E) Kidney stones
A) Glomerulonephritis
25) Glomerulonephritis may occur as a consequence of an infection
with the bacterium
A) Clostridium difficile.
B)
varicella.
C) Streptococcus.
D) MRSA.
E) Salmonella.
C) Streptococcus.
26) ________ is an inherited abnormality that affects the development
and structure of kidney tubules.
A) Glomerulonephritis
B)
Polycystic kidney disease
C) Nephrolithiasis
D) Renal
failure
E) Hematuria
B) Polycystic kidney disease
27) Renal columns are
A) internal cavities lined by the fibrous
capsule.
B) expanded ends of the ureters.
C) the basic
functional units of the kidney.
D) bundles of tissue that extend
between pyramids from the cortex.
E) conical structures that are
located in the renal medulla.
D) bundles of tissue that extend between pyramids from the cortex.
28) The expanded beginning of the ureter connects to the
A)
renal sinus.
B) renal pelvis.
C) renal calyx.
D) renal
hilum.
E) renal corpuscle.
B) renal pelvis.
29) Major calyces are
A) large branches of the renal
pelvis.
B) expanded ends of nephrons.
C) basic functional
layers of the kidney.
D) conical structures that are located in
the renal medulla.
E) the expanded ends of renal pyramids.
A) large branches of the renal pelvis.
30) Glomerular (Bowmanʹs) capsule and the glomerulus make up
the
A) renal pyramid.
B) nephron loop (loop of
Henle).
C) renal corpuscle.
D) renal papilla.
E)
collecting tubule system.
C) renal corpuscle.
31) The region known as the macula densa is part of
A) the
proximal convoluted tubule.
B) the distal convoluted
tubule.
C) the collecting duct.
D) the nephron loop (loop of
Henle).
E) glomerular (Bowmanʹs) capsule.
B) the distal convoluted tubule.
32) The cells of the macula densa, the juxtaglomerular cells, and the
extraglomerular mesangial cells form the
A) renal
corpuscle.
B) filtration membrane.
C) nephron loop (loop of
Henle).
D) juxtaglomerular complex.
E) afferent arteriole.
D) juxtaglomerular complex.
33) You have been diagnosed with lupus erythematosus, a very severe
autoimmune disorder with a wide variety of associated organ-related
problems. Your doctor is particularly worried about how this will
affect your kidney function. He says that you are susceptible to
________ because of the lupus.
A) polycystic kidney
B)
glomerulonephritis
C) cystitis
D) diabetes
E) renal calculi
B) glomerulonephritis
34) Filtrate first passes from the glomerular capsule to the
A)
nephron loop (loop of Henle).
B) proximal convoluted
tubule.
C) distal convoluted tubule.
D) collecting
duct.
E) minor calyx.
B) proximal convoluted tubule.
35) The portion of the nephron that empties into the collecting duct
is the
A) nephron loop (loop of Henle).
B) proximal
convoluted tubule.
C) distal convoluted tubule.
D) papillary
tubule.
E) calyx.
C) distal convoluted tubule.
36) Which of the following descriptions best matches the term renal
papilla?
A) It releases renin.
B) It creates high
interstitial NaCl concentration.
C) Final urine enters
here.
D) Initial filtrate enters here.
E) It is the tip of
the medullary pyramid.
E) It is the tip of the medullary pyramid.
37) The efferent arteriole of a nephron divides to form a network of
capillaries within the cortex called the ________ capillaries.
A)
peritubular
B) glomerular
C) vasa recta
D)
cortical
E) efferent
A) peritubular
38) The primary function of the proximal convoluted tubule is
A)
filtration.
B) reabsorption of ions, organic molecules, vitamins,
and water.
C) secretion of acids and ammonia.
D) secretion
of drugs.
E) adjusting the urine pH.
B) reabsorption of ions, organic molecules, vitamins, and water.
39) The following is a list of the blood vessels that carry blood to
the kidney. In what order does blood pass through these vessels
starting at the renal artery?
1. afferent arteriole
2.
arcuate artery
3. interlobar artery
4. segmental
artery
5. glomerulus
6. cortical radiate artery
7.
efferent arteriole
8. peritubular capillary
A) 4, 6, 2, 3,
1, 5, 7, 8
B) 4, 3, 2, 6, 1, 5, 7, 8
C) 4, 3, 2, 6, 7, 5, 1,
8
D) 4, 6, 2, 3, 7, 5, 1, 8
E) 4, 3, 6, 2, 1, 5, 7, 8
B) 4, 3, 2, 6, 1, 5, 7, 8
40) The filtration barrier in the renal corpuscle consists of which
three layers?
A) filtration slits, foot processes, and slit
pores
B) fenestrations, matrix, and foot processes
C)
fenestrated endothelium of glomerulus, basement membrane of
glomerulus, and podocyte filtration slits
D) basement membrane of
glomerulus, foot processes, and capsular outer layer
E) podocyte
filtration slits, matrix cells in the glomerulus, and extraglomerular
mesangial cells
C) fenestrated endothelium of glomerulus, basement membrane of glomerulus, and podocyte filtration slits
41) Eighty percent of nephrons in the human kidney are located in the
________ and have short nephron loops.
A) cortex
B)
medulla
C) pyramids
D) capsule
E) pelvis
A) cortex
Nephrons located close to the medulla with long nephron loops are
called ________ nephrons.
A) cortical
B)
juxtaglomerular
C) vasa recta
D) juxtamedullary
E) Henle
D) juxtamedullary
43) The ________ is a capillary bed that parallels the nephron loop
(loop of Henle).
A) glomerulus
B) peritubular capillary
bed
C) afferent arteriolar bed
D) collecting duct
E)
vasa recta
E) vasa recta
44) The majority of glomeruli are located in the ________ of the
kidney.
A) vasa recta
B) medulla
C) cortex
D)
pelvis
E) calyces
C) cortex
45) Which of the following components of the nephron is largely
confined to the renal medulla?
A) glomerular (Bowmanʹs)
capsule
B) distal convoluted tubule
C) collecting
ducts
D) proximal convoluted tubule
E) glomerulus
C) collecting ducts
46) Each kidney has about ________ nephrons.
A) 100,000
B)
500,000
C) 1 million
D) 1.25 million
E) 5 million
D) 1.25 million
47) The majority of renal innervation is by the
A)
parasympathetic nervous system.
B) vagus nerve.
C) somatic
nervous system.
D) sympathetic nervous system.
E) enteric
nervous system.
D) sympathetic nervous system.
48) The proximal convoluted tubule cells are
A) cuboidal cells
with microvilli.
B) cuboidal cells without microvilli.
C)
squamous cells.
D) columnar cells with microvilli.
E)
columnar cell without microvilli.
A) cuboidal cells with microvilli.
49) The region of the nephron containing intercalated cells primarily
associated with pH balance is the
A) glomerulus.
B) proximal
convoluted tubule.
C) nephron loop.
D) collecting
duct.
E) papillary duct.
D) collecting duct.
50) Modified smooth muscle cells in the wall of the afferent
arteriole that secrete renin are called
A) macula densa
cells.
B) juxtaglomerular cells.
C) extraglomerular
mesangial cells.
D) podocytes.
E) principal cells.
B) juxtaglomerular cells.
51) Which of the following substances should not be filtered?
A)
glucose
B) water
C) proteins
D) amino acids
E)
fatty acids
C) proteins
52) The functional units of kidneys where blood is filtered and urine
produced are called
A) pyramids.
B) nephrons.
C)
calyces.
D) lobules.
E) lobes.
B) nephrons.
53) Glomerular blood flow is unique because it flows
A) through
a glomerular portal vein.
B) directly from the renal artery into
the glomerular capillaries.
C) from arteriole to capillary bed to
arteriole.
D) from arteriole to capillary bed to vasa
recta.
E) through the peritubular capillaries then into the
glomerular capillaries.
C) from arteriole to capillary bed to arteriole.
54) An important structure for blood pressure regulation is
the
A) collecting duct.
B) nephron loop.
C) papillary
duct.
D) proximal convoluted tubule.
E) juxtaglomerular complex.
E) juxtaglomerular complex.
60) The filtration of plasma takes place in the
A) nephron loop
(loop of Henle).
B) distal convoluted tubule.
C) papillary
duct.
D) renal corpuscle.
E) ureter.
D) renal corpuscle.
61) Reabsorbed water and solutes enter into the
A) afferent
arteriole.
B) efferent arteriole.
C) peritubular
fluid.
D) tubular fluid.
E) glomerulus.
C) peritubular fluid.
62) ________ is the most abundant organic waste.
A)
Glucose
B) Albumin
C) Carbon dioxide
D) Sodium
E) Urea
E) Urea
63) The process that transports solutes, including many drugs, into
the tubular fluid is called
A) filtration.
B)
reabsorption.
C) absorption.
D) excretion.
E) secretion.
E) secretion.
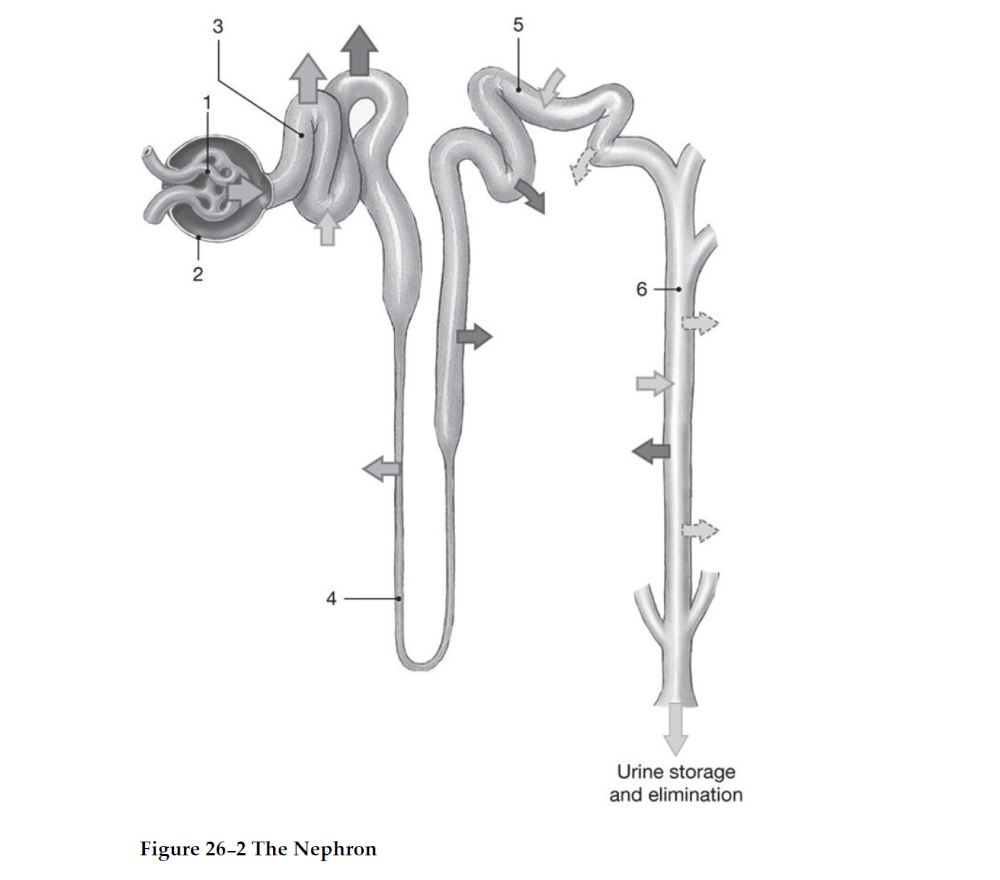
64) What physiological process occurs at the structure labeled
ʺ1ʺ?
A) reabsorption
B) excretion
C) secretion
D)
filtration
E) micturition
D) filtration

65) Where does most nutrient reabsorption occur?
A) 2
B)
3
C) 4
D) 5
E) 6
B) 3

66) Which area(s) allow variable water reabsorption and is/are
sensitive to the hormone ADH?
A) 1
B) 3
C) 4
D) 5
and 6
E) 3 and 6
D) 5 and 6

67) Where would penicillin be secreted?
A) 6
B) 5
C)
4
D) 3
E) 3 and 4
B) 5

68) Where does secretion mostly occur?
A) 5
B) 1
C)
3
D) 4
E) 2
A) 5

69) Which area is sensitive to aldosterone?
A) 2
B)
1
C) 4
D) 3
E) 5
E) 5

70) Identify the structure labeled ʺ5.ʺ
A) proximal convoluted
tubule
B) distal convoluted tubule
C) collecting
duct
D) nephron loop
E) glomerulus
B) distal convoluted tubule

71) Identify the structure labeled ʺ6.ʺ
A) proximal convoluted
tubule
B) distal convoluted tubule
C) collecting
duct
D) nephron loop
E) glomerulus
C) collecting duct
72) The process of filtration is driven mainly by
A) active
transport.
B) blood osmotic pressure.
C) blood hydrostatic
pressure.
D) renal pumping.
E) solvent drag.
C) blood hydrostatic pressure.
73) Approximately ________ liters of glomerular filtrate enter
glomerular capsules each day.
A) 480
B) 180
C)
125
D) 18
E) 1.8
B) 180
74) Under normal conditions, glomerular filtration depends on three
main pressures. From the list below, what are these three main
pressures?
1. glomerular hydrostatic pressure
2. capsular
hydrostatic pressure
3. capsular colloid osmotic pressure
4.
blood colloid osmotic pressure
5. urinary bladder hydrostatic
pressure
A) 1, 2, and 3 are correct.
B) 2, 3, and 4 are
correct.
C) 3, 4, and 5 are correct.
D) 1, 2, and 4 are
correct.
E) 2, 4, and 5 are correct.
D) 1, 2, and 4 are correct.
75) Which of the following formulas will allow you to calculate
correctly the net filtration pressure (NFP)? (Hint: CsHP is capsular
hydrostatic pressure.)
A) FP = GHP + CsHP - BCOP
B) FP = GHP
- (CsHP + BCOP)
C) FP = CsHP + GHP - BCOP
D) FP = BCOP - GHP
+ CsHP
E) FP = BCOP + (GHP - CsHP)
B) FP = GHP - (CsHP + BCOP)
76) Measurement of the functions of a nephron reveals a glomerular
capillary pressure of 69 mm Hg, and a pressure in the capsular space
of 15 mm Hg. Assuming that the blood colloid osmotic pressure is 30 mm
Hg, and that essentially no plasma proteins are filtered by the
glomerulus, what is the net filtration pressure in this case?
A)
30 mm Hg
B) 24 mm Hg
C) 69 mm Hg
D) 84 mm Hg
E) 99
mm Hg
B) 24 mm Hg
77) One mechanism the kidney uses to raise systemic blood pressure is
to
A) increase secretion of renin by the juxtaglomerular
complex.
B) decrease secretion of aldosterone.
C) increase
release of angiotensin II by the adrenal glands.
D) increase
filtration into glomerular (Bowmanʹs) capsule.
E) decrease
urinary albumin concentration.
A) increase secretion of renin by the juxtaglomerular complex.
78) Calculate filtration pressure (FP) in a nephron with a glomerular
hydrostatic pressure of 55
mm Hg, a blood colloid osmotic
pressure of 25 mm Hg, and a capsular hydrostatic pressure of
15
mm Hg.
A) FP = 10 mm Hg
B) FP = 95 mm Hg
C) FP = 55 mm
Hg
D) FP = 45 mm Hg
E) FP = 15 mm Hg
E) FP = 15 mm Hg
79) Blood colloid osmotic pressure (BCOP) in the glomerulus is
generated by
A) blood pressure.
B) presence of albumin
proteins in blood plasma.
C) constriction of the efferent
arteriole.
D) protein in the filtrate.
E) filtrate in the
capsular space.
B) presence of albumin proteins in blood plasma.
80) The main force that causes filtration in a nephron is
A)
blood colloid osmotic pressure.
B) glomerular hydrostatic
pressure.
C) osmotic pressure of the urine.
D) capsular
hydrostatic pressure.
E) reabsorption in proximal convoluted
tubule pulls filtrate from blood.
B) glomerular hydrostatic pressure.
81) Substances larger than ________ are normally not allowed to pass
through the filtration membrane.
A) sodium ions
B)
glucose
C) albumin
D) amino acids
E) urea
C) albumin
82) Sympathetic stimulation of the kidney can do all of the following
except
A) produce powerful vasoconstriction of the afferent
arterioles.
B) increase the glomerular filtration rate.
C)
trigger renin release.
D) produce renal ischemia.
E) reduce
blood flow to kidneys.
B) increase the glomerular filtration rate.
83) The filtration pressure at the glomerulus is equal to
A)
glomerular hydrostatic pressure - (capsular hydrostatic pressure +
interstitial fluid osmotic pressure).
B) capsular hydrostatic
pressure + capsular colloid osmotic pressure +
glomerular
hydrostatic pressure.
C) glomerular hydrostatic
pressure - (capsular hydrostatic pressure + blood colloid osmotic
pressure).
D) (capsular hydrostatic pressure + capsular colloid
osmotic pressure) - glomerular
hydrostatic pressure.
E)
glomerular hydrostatic pressure - (capsular hydrostatic pressure +
capsular colloid osmotic pressure).
C) glomerular hydrostatic pressure - (capsular hydrostatic pressure + blood colloid osmotic pressure).
84) The amount of filtrate produced by the kidneys each minute is
called the
A) net filtration pressure.
B) colloid
pressure.
C) plasma volume.
D) kidney filtrate
volume.
E) glomerular filtration rate.
E) glomerular filtration rate.
85) A drug that inhibits angiotensin converting enzyme (ACE) may lead
to all of the following except
A) less secretion of
aldosterone.
B) increased urinary loss of sodium.
C)
reduction of blood pressure.
D) decreased sodium
reabsorption.
E) increased fluid retention.
E) increased fluid retention.
86) All of the following would result in an increase in renin release
except
A) decreased blood pressure at the glomerulus.
B)
blockage in the renal artery.
C) increased blood volume.
D)
stimulation of juxtaglomerular cells.
E) decreased osmotic
concentration at the macula densa.
C) increased blood volume.
87) Immediate local responses of the kidney to changes in blood flow
to maintain GFR occur via
A) autoregulation.
B)
countercurrent multiplication.
C) hormonal regulation.
D)
autonomic regulation.
E) cephalic reflexes.
A) autoregulation.
88) Damage to the glomerular filtration membrane allowing proteins
into the capsular space would result in all of the following
except
A) an increase in capsular colloid osmotic
pressure.
B) a decrease in blood colloid osmotic
pressure.
C) an increase in net filtration pressure.
D) an
increase in GFR and fluid loss.
E) a decrease in capsular
hydrostatic pressure.
E) a decrease in capsular hydrostatic pressure.
89) Tubular reabsorption involves all of the following except
A)
active transport.
B) facilitated diffusion.
C)
cotransport.
D) countertransport.
E) stem cell movements.
E) stem cell movements.
90) Reabsorption of filtered glucose from the lumen in the PCT is
largely by means of
A) diffusion.
B) facilitated
diffusion.
C) active transport.
D) cotransport.
E) countertransport.
D) cotransport.
91) Secretion of hydrogen ion by the PCT is by the process of
A)
diffusion.
B) facilitated diffusion.
C) active
transport.
D) cotransport.
E) countertransport.
E) countertransport.
92) Chloride ion is reabsorbed in the thick ascending limb by
A)
simple diffusion.
B) facilitated diffusion.
C) active
transport.
D) cotransport with Na and K ions.
E)
countertransport for bicarbonate ion.
D) cotransport with Na and K ions.
93) The renal threshold for glucose is approximately ________
mg/dl.
A) 75
B) 90
C) 100
D) 140
E) 180
E) 180
94) The concentration at which all of the carriers in renal tubules
for a given substance are
saturated is the
A) tubular
maximum.
B) hydrostatic threshold.
C) blood colloid
maximum.
D) osmotic pressure.
E) renal threshold.
A) tubular maximum.
95) The ________ is the plasma concentration at which a specific
compound will begin appearing in the urine.
A) tubular
maximum
B) hydrostatic threshold
C) blood colloid
maximum
D) osmotic pressure
E) renal threshold
E) renal threshold
96) The process of ________ involves a carrier protein that can
transport a molecule across the cell membrane down its concentration
gradient.
A) simple diffusion
B) facilitated
diffusion
C) osmosis
D) bulk transport
E) active transport
B) facilitated diffusion
97) A transport mechanism that can move a substance against a
concentration gradient by using cellular energy is
A) simple
diffusion.
B) facilitated diffusion.
C) osmosis.
D)
bulk transport.
E) active transport.
E) active transport.
98) In the process of ________, two substances are moved across a
cell membrane in the same direction without directly using cellular
energy. One of the substances can be moved against a concentration
gradient by this process.
A) countertransport
B)
cotransport
C) simple diffusion
D) active transport
E) co-osmosis
B) cotransport
99) Diuretics are used for all of the following reasons
except
A) to reduce body weight.
B) to reduce water
retention.
C) to reduce blood pressure.
D) to treat
congestive heart failure.
E) to reduce glucose levels.
E) to reduce glucose levels.
100) The majority of water is reabsorbed by osmosis in the
A)
proximal convoluted tubule.
B) nephron loop.
C) distal
convoluted tubule.
D) collecting duct.
E) papillary duct.
A) proximal convoluted tubule.
101) The majority of cotransporters and countertransporters are
linked to the reabsorption of what ion?
A) hydrogen
B)
sodium
C) potassium
D) bicarbonate
E) chloride
B) sodium
102) Prolonged aldosterone stimulation of the distal convoluted
tubule may result in
A) hypercalcemia.
B)
hypocalcemia.
C) hypokalemia.
D) hyperkalemia.
E) alkalosis.
C) hypokalemia.
103) Which of the following is not a normal constituent of
urine?
A) hydrogen ions
B) urea
C) large
proteins
D) amino acids
E) creatinine
C) large proteins
104) The ________ test is often used to estimate the glomerular
filtration rate.
A) inulin
B) glucose tolerance
C) CBC
or complete blood count
D) specific gravity
E) creatinine clearance
E) creatinine clearance
105) Basically, what occurs in the countercurrent multiplier
process?
A) Sodium is pumped into the blood while potassium is
actively transported out of the blood back into the tissues.
B) A
higher sodium concentration is produced in the renal medulla that
osmotically draws out water, reducing it within the tubules and the
urine.
C) Glucose and sodium are cotransported from urine back
into blood.
D) Creatinine is actively transported out of the
blood into urine.
E) Uric acid is excreted into the kidney
tubules while urea is reabsorbed in the nephron loop.
B) A higher sodium concentration is produced in the renal medulla that osmotically draws out water, reducing it within the tubules and the urine.
106) The ability to form concentrated urine depends on the functions
of the
A) proximal convoluted tubule.
B) distal convoluted
tubule.
C) collecting duct.
D) nephron loop (loop of
Henle).
E) nephron loop, distal convoluted tubule and the
collecting duct.
E) nephron loop, distal convoluted tubule and the collecting duct.
107) The mechanism for producing a concentrated urine involves all of
the following except
A) the secretion of antidiuretic hormone
(ADH) by the posterior pituitary gland.
B) aquaporins being
inserted into the membranes of the collecting duct cells.
C) a
high concentration of NaCl in the interstitial fluid that surrounds
the collecting ducts.
D) an increase in facultative water
reabsorption.
E) obligatory water reabsorption in the proximal
convoluted tubule.
E) obligatory water reabsorption in the proximal convoluted tubule.
108) A patient excretes a large volume of very dilute urine on a
continuing basis. This is may be due to
A) excessive ADH
secretion.
B) absence of ADH.
C) hematuric oliguria.
D)
overproduction of aldosterone.
E) dilation of the afferent arterioles.
B) absence of ADH.
109) Antidiuretic hormone
A) increases the permeability of the
collecting ducts to water.
B) is secreted in response to low
potassium ion in the blood.
C) causes the kidneys to produce a
larger volume of very dilute urine.
D) is secreted by the
anterior pituitary.
E) release is insensitive to the osmolarity
of interstitial fluid.
A) increases the permeability of the collecting ducts to water.
110) If a urine sample is distinctly yellow in color, which of the
following will be true?
A) Its pH is below normal.
B) It
will have the odor of ammonia.
C) It will contain large amounts
of urobilin.
D) It will contain excess chloride ion.
E) It
will have a high pH.
C) It will contain large amounts of urobilin.
111) When the level of ADH (antidiuretic hormone) decreases,
A)
a concentrated urine is produced.
B) less urine is
produced.
C) the osmolarity of the urine decreases.
D)
permeability to water in the collecting system increases.
E)
water reabsorption increases in the nephron loop.
C) the osmolarity of the urine decreases.
112) As the filtrate passes through the renal tubules, approximately
what percentage is reabsorbed and returned to the circulation?
A)
1
B) 38
C) 63
D) 74
E) 99
E) 99
113) In response to increased levels of aldosterone, the kidneys
produce
A) a larger volume of urine.
B) urine with a higher
concentration of sodium ions.
C) urine with a lower concentration
of potassium ions.
D) urine with a lower concentration of sodium
ions.
E) urine with less glucose.
D) urine with a lower concentration of sodium ions.
114) Which of the following is a not a true statement regarding the
countercurrent multiplication
system?
A) The thin limb of
the nephron loop is permeable to water.
B) The thick limb of the
nephron loop is permeable to solutes.
C) Osmotic concentration in
the nephron loop decreases as fluid flows toward the bottom of the
loop.
D) Tubule fluid arrives at the DCT at about 100
mOsm/L.
E) The maximum solute concentration is about 1200 mOsm/L.
C) Osmotic concentration in the nephron loop decreases as fluid flows toward the bottom of the loop.
115) Excess release of natriuretic peptides would cause
A) a
large volume of concentrated urine.
B) a large volume of dilute
urine.
C) a small volume of concentrated urine.
D) a small
volume of dilute urine.
E) a small volume of urine void of sodium.
B) a large volume of dilute urine.
116) The final composition of urine is represented by which of the
following statements?
A) Urine = substances reabsorbed +
substances secreted.
B) Urine = substances filtered + substances
reabsorbed + substances secreted.
C) Urine = substances secreted
- substances reabsorbed - substances filtered.
D) Urine =
substances filtered - substances reabsorbed + substances
secreted.
E) Urine = substances reabsorbed - substances secreted
- substances filtered.
D) Urine = substances filtered - substances reabsorbed + substances secreted.
117) The ureters and urinary bladder are lined by ________
epithelium.
A) stratified squamous
B) pseudostratified
columnar
C) simple cuboidal
D) transitional
E) simple columnar
D) transitional
118) The detrusor muscle
A) moves urine along the ureters by
peristalsis.
B) compresses the urinary bladder and expels urine
through the urethra.
C) functions as the internal urinary
sphincter.
D) functions as the external urinary
sphincter.
E) surrounds the renal pelvis.
B) compresses the urinary bladder and expels urine through the urethra.
119) The inability of the kidneys to excrete adequately to maintain
homeostasis is
A) glomerulonephritis.
B) polycystic kidney
disease.
C) calculi.
D) renal failure.
E) hematuria.
D) renal failure.
120) The area of the urinary bladder bounded by the openings of the
two ureters and the urethra is called the
A) renal
pelvis.
B) JG apparatus.
C) pyramid.
D)
trigone.
E) vasa recta.
D) trigone.
121) Insoluble deposits that form within the urinary tract from
calcium salts, magnesium salts, or uric acid are called kidney stones
or renal
A) calculi.
B) plaque.
C) caries.
D)
otoliths.
E) lithotrophs.
A) calculi.
122) You complain to the doctor about constant pain and discomfort in
the low back area. What test might logically be recommended?
A)
an MRI
B) a pyelogram
C) a liver biopsy
D) an
angiogram
E) a liver enzyme assay
B) a pyelogram
123) The pontine storage center controls micturition by
A)
stimulating bladder contractions.
B) increasing contraction of
the detrusor muscle.
C) relaxing the internal urethral
sphincter.
D) increasing contraction of the external urethral
sphincter and reducing detrusor muscle activity.
E) stimulating
the voiding reflex.
D) increasing contraction of the external urethral sphincter and reducing detrusor muscle activity.
124) Which of the following statements is false regarding
micturition?
A) When you relax the external urethral sphincter,
the internal sphincter will relax.
B) Urination will be completed
despite voluntary opposition.
C) Parasympathetic nervous control
is involved with the micturition reflex.
D) Stretch receptors in
the bladder are stimulated by the warm temperature of the
urine.
E) Bladder contractions can force open the internal
urethral sphincter.
D) Stretch receptors in the bladder are stimulated by the warm temperature of the urine.
125) Changes that occur in the urinary system with aging include all
of the following except
A) a decline in the number of functional
nephrons.
B) a reduction in the GFR (glomerular filtration
rate).
C) increased sensitivity to ADH.
D) problems with the
micturition reflex.
E) loss of sphincter muscle tone.
C) increased sensitivity to ADH.
126) Your doctor has diagnosed you with prostatitis, an inflammation
and swelling involving the
prostate gland. One of your primary
symptoms is
A) dribbling urination.
B) renal
failure.
C) hematuria.
D) glycosuria.
E) large amounts
of dilute urine.
A) dribbling urination.
127) Each of the following organ systems excretes wastes to some
degree except the ________ system.
A) urinary
B)
integumentary
C) digestive
D) endocrine
E) respiratory
D) endocrine
1) In which region of the kidney is a glomerulus located?
A)
fibrous capsule
B) renal hilum
C) medullary pyramid
D)
renal cortex
E) renal medulla
D) renal cortex
2) What structure connects the proximal convoluted tubule to the
distal convoluted tubule?
A) renal corpuscle
B) collecting
duct
C) papillary duct
D) glomerular capsule
E) nephron loop
E) nephron loop
3) What four factors shown result in an increased blood volume?
A) increased sodium retention, increased fluid consumption,
increased fluid retention, and constriction of systemic veins
B)
decreased cardiac output, decreased fluid retention, decreased sodium
retention, and systemic vasodilation
C) increased glomerular
hydrostatic pressure, increased blood colloid osmotic pressure,
decreased capsular hydrostatic pressure, decreased capsular colloid
osmotic pressure
D) decreased glomerular hydrostatic pressure,
decreased blood colloid osmotic pressure, increased capsular
hydrostatic pressure, increased capsular colloid osmotic
pressure
E) increased sodium excretion, increased potassium
retention, decreased fluid
consumption, increased fluid retention
A) increased sodium retention, increased fluid consumption, increased fluid retention, and constriction of systemic veins
4) Aldosterone-sensitive portions of the distal convoluted tubule and
collecting duct allow for the exchange of which ions?
A)
reabsorption of hydrogen ions in exchange for chloride ions
B)
reabsorption of chloride ions in exchange for hydrogen ions
C)
reabsorption of sodium ions in exchange for potassium ions
D)
reabsorption of potassium ions in exchange for sodium ions
E)
reabsorption of bicarbonate ions in exchange for hydrogen ions
C) reabsorption of sodium ions in exchange for potassium ions
5) ADH creates a (small or large) volume of (dilute or concentrated)
urine.
A) small; dilute
B) small; concentrated
C)
large; dilute
D) large; concentrated
B) small; concentrated
6) The (ureter or urethra) transports urine to the bladder.
A)
ureter
B) urethra
A) ureter