Describe the size, shape, location, and orientation of the heart in the thorax.
250 to 350 grams about the size of a fist, within the mediastinum and tilts toward the left side of the body
Name the coverings of the heart.
Pericardium – doubled-walled sac that encloses the heart.
•Fibrous Pericardium – superficial part of pericardium, protects, anchors and prevents the heart from overfilling
•Serous Pericardium – deep to the fibrous pericardium, a thin, slippery, two-layer serous membrane that forms a closed sac around the heart.
oParietal Layer – lines the internal surface off the fibrous pericardium and attaches to the large arteries exiting the heart.
oEpicardium – Visceral layer of the Serous Pericardium that lines the external heart surface
Describe the structure and function of each of the three layers of the heart wall.
•Endocardium – inside layer of the heart wall, sheet of endothelium, lines the heart chambers and covers the fibrous skeleton of the valves
•Myocadium – middle layer of heart wall, composed mainly of cardiac muscle, the layer that pumps
•Epicardium – Viseral layer of the Serous Pericardium that lines the external heart surface
Describe the structure and functions of the four heart chambers. Name each chamber and provide the name and general route of its associated great vessel(s).
Left Atria – left superior chamber of the heart that receives oxygenated blood from the lungs
Right Atria – right superior chamber of the heart the receives oxygen-poor blood from the body
Left Ventricle – left inferior chamber of the heart that pumps oxygenated blood to the body
Right Ventricle – left inferior chamber of the heart that pumps oxygen-poor blood to the lungs
Name the heart valves and describe their location, function, and mechanism of operation.
Ensure unidirectional blood flow through the heart
Semilunar Valve – valve between the left ventricle and the aorta
Pulmonary Semilunar Valve - valve between the right ventricle and the pulmonary trunk
Tricuspid Valve – the right (AV) atrioventricular valve, has three flexible cusps (flaps of endocardium reinforced by connective tissue cores)
Mitral Valve – the left (AV) atrioventricular valve, has two flexible cusps (flaps of endocardium reinforced by connective tissue) resembles the two-sided bishop’s miter
Trace the pathway of blood through the heart.
•Pulmonary circuit
Right atrium
tricuspid valve
right ventricle
pulmonary semilunar valve
pulmonary trunk
pulmonary arteries
lungs
pulmonary veins
left atrium
•Systemic circuit
Left atrium
mitral valve
Left ventricle
aortic semilunar
Name the major branches and describe the distribution of the coronary arteries.
•Left Coronary Artery – runs toward the left side of the heart and then divides into two major branches
oAnterior Interventricular Artery – follows the anterior interventricular sulcus and supplies blood to the interventricular septum.
oCircumflex Artery – supplies the left ventricle and the posterior walls of the left ventricle.
•Right Coronary Artery – courses to the right side of the heart, where it also gives rise to two branches
oRight Marginal Artery – serves the myocardium of the lateral side of the heart
oPosterior interventricular Artery – runs to the heart apex and supplies the posterior ventricular walls
Describe the structural and functional properties of cardiac muscle, and explain how it differs from skeletal muscle.
•Cardiac Muscle Cells – short, fat, branched, interconnected, striated and contracts by sliding filament mechanism
•Differences in Cardiac and Skeletal Contraction
•Means of Stimulation – each skeletal muscle fibers must be stimulated to contract but some cardiac muscle cells are self-excitable
•Organ vs. Motor Unit Contraction – Only muscle fibers stimulated by nerve fibers contract. In cardiac muscle, either all fibers in the heart contract as a unit or the heart does not contract at all.
•Length of Absolute Refractory Period – in skeletal muscle contractions lasts 15-100ms with brief refractory period 1-2ms. In Cardiac muscle the refractory period lasts over 200ms nearly as long as the contraction
Briefly describe the events of cardiac muscle cell contraction.
1.Depolarization – is due to Na+ influx through the fast voltage-gated Na+ Cannels. A positive feedback cycle rapidly opens many Na+ channels, revealing the membrane potential. Channel inactivation ends this phase
2.Plateau Phase – is due to Ca2+ influx through sllow Ca2+ channels. This keeps cell depolarized because few K+ channels are open
3.Repolarization – is due to Ca2+ channels inactivating and K+ channels opening. This allows K+ influx, which brings the membrane potential back to its resting voltage
Name the components of the conduction system of the heart, and trace the conduction pathway.
The conduction starts at the pacemaker region called the Sinoatrial Node (SA node) which is just under where the superior vena cava enters the right atrium. From here the conduction passes to the Atrioventricular Node (AV node) which is just to the right of the septum. From here the stimulation is passed through the Atrioventricular (AV) Bundle (Bundle of His) which carries the conduction to the septum where two Bundle Branches pick it up. These branches carry the conduction to the base of the septum where they separate into the Purkinje Fibres (Subendocardial Conducting Network). These fibers carry the conduction all around the heart.
Draw a diagram of a normal electrocardiogram tracing. Name the individual waves and intervals, and indicate what each represents
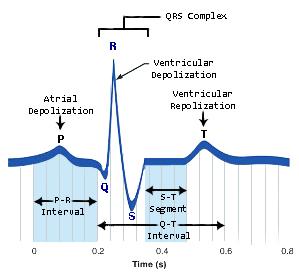
Name some abnormalities that can be detected on an ECG tracing.
Evidence of coronary artery disease, locate damaged heart tissue, and detect other cardiovascular disorders.
An ECG tracing can provide a baseline examination of the tissues of the heart and can show whether a heart attack, or myocardial infarction, has occurred. Following a heart attack, an ECG can be used to examine the electrical activity in various areas and tissues of the heart and to help find damaged areas.
Describe normal heart sounds, and explain how heart murmurs differ.
Two sounds (lub-dup) associated with closing of heart valves
oFirst sound occurs as AV valves close and signifies beginning of systole
oSecond sound occurs when SL valves close at the beginning of ventricular diastole
•Heart murmurs: abnormal heart sounds most often indicative of valve problems
Describe the timing and events of the cardiac cycle.
The cardiac cycle is the sequence of events in one heartbeat.
It can be divided into three stages:
1.Diastole: the chambers of the heart (atria and ventricles) are relaxed and filling up with blood from the veins. The atrioventricular valves (bicuspid on the left and tricuspid on the right) are open and the semilunar valves (pulmonary and aortic) are closed. This stage lasts for about 0.4 second.
2.Atrial systole: the atria contract and top up the ventricles. This takes about 0.1 second.
3.Ventricular systole: the ventricles contract and pump blood out of the heart into the arteries. During this stage the atrioventricular valves are closed and the semilunar valves are open. This takes about 0.3 second.
The total cycle takes about 0.8 second while the subject is resting. This gives a heart rate of about 75 beats per minute.
Name and explain the effects of various factors regulating stroke volume and heart rate.
•Three main factors affect SV
1. Preload: intrinsic factors
degree of stretch of cardiac muscle cells before they contract (Frank-Starling law of the heart)
Increased venous return distends (stretches) the ventricles and increases contraction force
2. Contractility: extrinsic factors called inotropic agents (mscell)
contractile strength at a given muscle length, independent of muscle stretch and EDV
Affected by ion exchange across membranes of heart ms cells
Increased contractility = increased SV—due to ↑cytoplasmiccalcium ions
+ inotropicagents ↑contractility/-agents ↓contractility
3. Afterload
pressure that must be overcome for ventricles to eject blood
Hypertension increases afterload, resulting in increased ESV and reduced SV
•Factors that affect HR (time)
1. Chronotropic factors: + chronotropicfactors ↑HR, -chronotropicfactors ↓HR
2. Chemical regulation
Hormones: epinephrine/norepinephrine, thyroxine (thyroid hormone)
Ionic balance: intra-and extracellular (Ca and K)
3. ANS controls: most important extrinsic controls affecting HR
Sympathetic ns stimulates pacemaker cells which will ↑HR
•Atrial (Bainbridge) reflex: a sympathetic reflex initiated by increased venous return. Blood puts stretch on atrial walls and stimulates SA node as well as atrial stretch receptors which activates sympathetic reflexes
Parasympathetic ns inhibits pacemaker cells which ↓HR
Vagal tone: heart at rest, dominant influence is inhibitory
4. Age - Fetus has fastest HR
5. Gender - Females faster than males
6. Exercise - Increases HR
7. Body temperature - Increases with increased temperature
Explain the role of the autonomic nervous system in regulating cardiac output.
Exerts the most important extrinsic controls affecting heart rate
When emotional or physical stressors, such as fright, anxiety, or exercise, activate the sympathetic nervous system, sympathetic nerve fibers release norepinephrine at their cardiac synapses. The heart responds by beating faster.
Developmental Aspects of the Heart
• Embryonic heart chambers
1. Sinus venous
2. Atrium
3. Ventricle
4. Bulbus cordis
• Fetal heart structures that bypass pulmonary circulation
1. Foramen ovale connects the two atria
2. Ductus arteriosus connects the pulmonary trunk and the aorta
• Congenital heart defects
1. Lead to mixing of systemic and pulmonary blood
2. Involve narrowed valves or vessels that increase the workload on the heart
Provide examples of age-related changes in heart function.
Sclerosis (stiff) and thickening of valve flaps
Decline in cardiac reserve – less able to respond to sudden and prolonged stressors
Fibrosis of cardiac muscle (scared)
Atherosclerosis - condition in which an artery wall thickens as a result of the accumulation of fatty materials such as cholesterol.
