NURS 401_Oxygenation & Asthma
Trachea is shorter; angle of right bronchus at bifurcation is more acute (steeper slope)
Children
What are some A&P differences in the respiratory system or that affect the respiratory system of children?
Fewer alveoli
Less flow between alveoli
Lower Hgb
Lower SV
Higher metabolic rate
Average respiratory rate for a newborn
30-60
Average respiratory rate for infants
30
Average respiratory rate for preschoolers
25
Average respiratory rate for school age
20
Average respiratory rate for adolescents & adults
12-18
Airway edema, although serious with any age, is especially dangerous with this population r/t level of diameter decrease it causes
Newborns (small airway of 4mm can decrease to 2mm)
Mechanisms that facilitate or impair the body's ability to supply oxygen to cells
Oxygenation
Which of the following individuals would be at greatest risk for pneumonia
- A 37 year old who recently delivered via a cesarean birth
- An 8 year old with a history of allergies and asthma
- A 55 year old who fractured fibula
- A 72 year old who has the flu
D. A 72 year old who has the flu
A patient is scheduled to have a ventilation/perfusion (V/Q) scan. The nurse knows this is to diagnose:
- Asthma
- Pulmonary fibrosis
- Pulmonary embolus
- COPD
3. Pulmonary embolus
When teaching the patient with asthma about the use of the peak flow meter, the nurse instructs the patient to:
- Increase the use of rescue inhalers (albuterol) if the meter indicates the yellow zone
- Carry the flow meter at all times
- Close your mouth around the mouthpiece and inhale quickly when measuring peak flow
- Go to the emergency room if the meter indicate the yellow zone
1. Increase the use of rescue inhalers (albuterol) if the meter indicates the yellow zone
You monitor your patient oxygen saturation during exercise and finds that it drops from 94% to 87%. The nurse interprets this data
- The patient requires higher concentration of oxygen during ambulation
- The patient needs to be on bedrest
- The patient needs a blood transfusion to increase oxygen carrying capacity
- The patient requires more deep breathing and use of the incentive spirometry
1. The patient requires higher concentration of oxygen during ambulation
Your patient has chronic COPD with hypercapnia. Which of the following would be the safest order for oxygen for this patient?
- 6 l/m via nasal cannula
- 50% oxygen via a rebreather mask
- 28% venturi mask
- Administer oxygen PRN only when patient complains of dyspnea
3. 28% venturi mask
Your patient is diagnosed with tuberculosis. Which of the following is most important in treatment
- Make sure that he is placed in a positive airflow room
- Institute droplet precautions immediately
- Ensure that the patient complete the full course of antibiotic treatment
- Encourage a high protein diet
3. Ensure that the patient complete the full course of antibiotic treatment
Jennie Dasher is recovering from and aortic valve replacement. Her intial blood gas values come back as: pH 7.5, PCO2 30, HCO3 22, PO2 92. These date support which acid base disturbance?
- Compensated respiratory alkalosis
- Uncompensated respiratory alkalosis
- Compensated respiratory acidosis
- Uncompensated respiratory acidosis
2. Uncompensated respiratory alkalosis
Act of inhaling & exhaling air to transport O2 to alveoli
Respiration
ACTUAL exchange of O2 & CO2 (breathing)
Ventilation
A continuous supply of oxygenated blood to every cell in the body (pumped to all parts)
Perfusion
What are the 3 main components that make up the umbrella of oxygenation?
Ventilation (breathing)
Diffusion (gas exchange)
Perfusion (pumping to all parts of body)
This age group is known for being obligated nose breathers
Newborns
Inadequate supply of O2 in the blood
Hypoxemia
What are some late S/S of hypoxemia?
Combative/coma
Dyspnea @ rest
Cyanosis
Cool, clammy skin
Low BP/HR
What are some early S/S of hypoxemia?
Irritability/restlessness
Tachypnea/dyspnea
High BP/HR
What are some red flags r/t hypoxemia?
Change in mentation:
LOC
Orientation
Irritability
Confusion
Lethargy
What other problems may result in S/S similar to SNS response to hypoxemia?
*Would require us to distinguish between whether or not it's hypoxemia
SNS response to:
Pain
Fear
Sepsis
Alphabet soup r/t oxygenation:
C = ?
Concentration
Alphabet soup r/t oxygenation:
F = ?
Fractional concentration
Alphabet soup r/t oxygenation:
E = ?
Expired
Alphabet soup r/t oxygenation:
I = ?
Inspired
Alphabet soup r/t oxygenation:
P = ?
Partial pressure
Alphabet soup r/t oxygenation:
Q = ?
Volume of blood
Alphabet soup r/t oxygenation:
S = ?
Saturation
Alphabet soup r/t oxygenation:
V = ?
Volume of gas
Alphabet soup r/t oxygenation:
a = ?
arterial
Alphabet soup r/t oxygenation:
c = ?
capillary
Alphabet soup r/t oxygenation:
v = ?
venous
Alphabet soup r/t oxygenation:
p = ?
pulse oximetry
Alphabet soup r/t oxygenation:
A = ?
Alveolar
This is a measure of the hydrogen ion concentration
pH
Alphabet soup r/t oxygenation:
pCO2 = ?
Partial pressure of CO2
Alphabet soup r/t oxygenation:
pO2 = ?
Partial pressure of O2
Alphabet soup r/t oxygenation:
SO2 = ?
Saturation of O2
Alphabet soup r/t oxygenation:
HCO3 = ?
Bicarbonate
"Gold standard" for measuring oxygenation
ABG
If performing a radial ABG, which side should you stick?
Non-dominant hand
What type of patient would we not want to perform a brachial stick to obtain an ABG?
Obese (difficult to assess for hemostasis)
Where would you obtain an ABG on a newborn?
Umbilical artery line
ABG:
Normal PaO2
80-100
ABG:
Normal SaO2
95-100%
ABG:
Normal CO2
35-45
ABG:
Normal HCO3
22-26
ABG:
Normal Base Excess (BE)
-2.0 to 2.0 mEq/L
Hgb is almost fully saturated at this pO2
80-100 mm Hg
Hg saturation with O2 is high in the __1__ and is greatest in the __2__
1. Tissues
2. Lungs
If Hg experiences an increased affinity for O2, these manifestations will ensue
Lower temp
Lower pCO2
Lower 2, 3-DPG
Increased pH
The ease with which hemoglobin releases oxygen to the tissues is controlled by this
2, 3-DPG
If Hg experiences a decreased affinity for O2, these manifestations will ensue
Increased temp
Increased pCO2
Increased 2, 3-DPG
Lower pH
In what different situations can PaO2 & SaO2 not be consistent?
SpO2 <70%
Hg abnormality
Movement/exercise
Vasoconstriction (low perfusion)
Skin color
Intravascular/intradermal dyes
Bright fluorescent lights
Anemia
Hg & O2:
__1__ is the maximum amt. of O2 that can be combined with Hg, whereas __2__ is the actual amount of O2 being carried by Hg
1. Capacity
2. Saturation
How does O2 blood saturation affect Hg saturation?
If Hg isn't fully saturated, a high O2 blood content will result in high Hg
If Hg is highly saturated, a low O2 blood content will result in low Hg
Classical cyanosis is present when 5 g/dL of __1__ or greater is present, and is usually apparent when SaO2 is less than or equal to __2__
1. Deoxyhemoglobin
2. 85%
This sign is not a good indicator of oxygenation
Cyanosis
These 3 systems regulate acid-base balance
Buffer system (metabolic)
Kidneys (metabolic)
Lungs (respiratory)
This counteracts changes to pH due to ability to either absorb or release H+ ions
First line of defense vs. pH changes
Buffer system
3 main buffers of the buffer system of pH maintenance include:
HCO3
Phosphate
Protein
Can directly affect acid-base balance status more quickly & efficiently than all the buffer systems combined
Respiratory system
Can activate pH changes within 1-3 minutes
Respiratory system
Slower process; requires 1-5 days for complete activation to correct acid-base imbalances
Kidneys
How do kidneys react to changes in pH?
Regulate excretion or conservation of H+ & HCO3
How soon are pH buffer systems operational?
In utero
*Renal system limited in newborns
Do newborns have the ability to control pH using their respiratory system?
Yes, so long as pulmonary function is adequate
The renal buffer system is limited in its capacity to respond to pH changes in this age group
Newborns
pH <7.35
pCO2 >45mm Hg
Respiratory acidosis
pH <7.35
HCO3 <22mm Hg
Metabolic acidosis
The body has accumulated too much acid & doesn't have enough HCO3 to neutralize its effects
Metabolic acidosis
This acid-base imbalance is often r/t hyperventilation
Respiratory alkalosis
pH >7.45
pCO2 <35mm Hg
Respiratory alkalosis
pH >7.45
HCO3 >26mm Hg
Metabolic alkalosis
pH is abnormal
pCO2 & HCO3 abnormal
Partial compensation
pH is normal
pCO2 & HCO3 abnormal
Full compensation
At what age will most children first have respiratory symptoms indicative of asthma?
<4 years
What is one of the first signs that a person is having airway restriction indicative of asthma?
Cough
*Wheezing is a medium-late sign of asthma
What's the most common trigger for children's asthma attacks?
Viruses
These factors often predispose children to having asthma later in life
Parental asthma
Eczema/atopy
Asthma is an INFLAMMATORY disease with these 3 characteristics
Edema
Excess mucus production
Bronchospasm
Can mild asthma have a severe exacerbation?
Yes
This doesn't disappear along with the symptoms of asthma following treatment
Airway inflammation (chronically present regardless of symptoms)
In a large number of children, asthma remits at this point in life
Early adolescence/adulthood
This medication is both a bronchodilator & anticholinergic used to treat asthma; thus, you're treating inflammation via both sympathetic & parasympathetic routes
Atrovent (ipratropium bromide)
Incidence of asthma is greater in boys up until this point in life; after this point, it's more prevalent in girls
Until puberty
What are the 2 major groups of medications used to TX asthma?
Rescue & controller medications
Types of rescue medications for asthma
Beta 2's (albuterol, atrovent)
Oral steroids
Anticholinergics (atrovent)
Types of controller medications for asthma
Inhaled corticosteroids
Anti-leukotrienes (Montelukast)
Long-active beta 2's
Combo inhaled & long-acting (Advair, Symbicort)
What objective information is needed for asthma treatment?
Peak flow meters
Spirometry for child >5 yrs (or infant spirometry)
Exhaled nitric oxide measurement (normal eNO = 5-15 ppb)
Allergy testing
This helps w/diagnosis & ongoing TX decisions r/t asthma
Provides objective data for management
Measures obstruction to airflow in airways
Spirometry
Early phase of acute asthma exacerbation:
1. What causes symptoms?
2. What is the treatment?
1. Bronchoconstriction & inflammation
2. Beta 2 agonist (i.e. bronchodilator)
Late phase of acute asthma exacerbation:
1. What is happening to respiratory A&P?
2. What is the treatment?
1. Bronchial hyperresponsiveness
2. Bronchodilator & antiinflammatory medications
Early warning signs of asthma
Cough, throat clearing
Chest tightness
SOB
EXPIRATORY wheezing
Late warning signs of asthma
Cough, vomit
Stop to breathe when walking
Trouble walking normal distances
Accessory muscle use
INSPIRATORY & EXPIRATORY wheezing
What does giving a daily inhaled mcg dose of corticosteroid controller medication prevent?
Having to take an oral milligram dose of corticosteroid medication
What are some worrisome signs during an acute asthma exacerbation?
Climbing pCO2 (35-45)
No wheezing is ominous
Unable to say more than a few words
Confusion
Don't care what's happening around them (just care about oxygen)
Asthma guidelines address these 3 different age ranges
0-4
5-11
>12
How many puffs are in a normal dose of your rescue inhaler?
4
Analyze asthma severity chart on reverse side
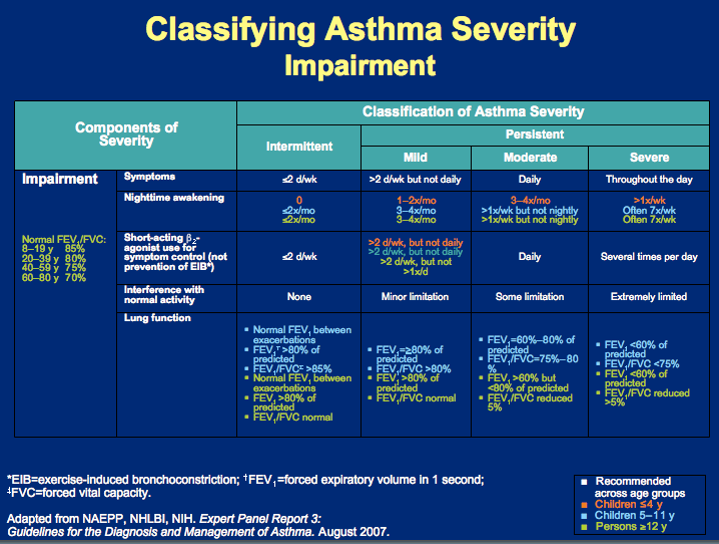
Along with rescue meds, this will most likely be added to the TX plan of a mild asthmatic
Low-dose ICS
Along with rescue meds, this will most likely be added to the TX plan of a moderate asthmatic
Medium-dose ICS
Along with rescue meds, this will most likely be added to the TX plan of a severe asthmatic
High-dose ICS + LABA or montelukast; potentially oral systemic corticosteroids depending on severity
What's the "Rule of 2's", as proposed by Baylor University?
Does your child use albuterol > 2x/week?
Does your child have symptoms @ night > 2x/month?
Do you refill your rescue med > 2x/year?
Peak flow < 20% from personal best blow?
What happens if there's a "yes" answer to any of the questions in the "Rule of 2's" from Baylor University?
Indicates asthma isn't under control
Chronic inflammation requiring a controller med
Indicates child has reached level of PERSISTENT asthma
The always-present inflammatory cells in the asthmatic's airway result in hyper-__1__ & hyper-__2__ airways that, when hit with a __3__, become further inflamed & edematous, increasing __4__ production & constricting of smooth muscle
1. Reactive
2. Sensitized
3. Trigger
4. Mucus
What's the ultimate goal of asthma treatment?
Prevention of exacerbations (which will prevent airway remodeling)
With a child of this age, they may help with minimal task, such as holding equipment
<2 yrs
With a child of this age, they may be able to get some equipment, ID some body parts involved in asthma, & help with TX
2-4 yrs
With a child of this age, parents are still responsible for care, but the child can learn early warning signs, triggers, and correct words to label body parts & symptoms
4-6 yrs
With a child of this age, parents are still needed, but child is starting to take more active care role; can set up equipment, recite meds & info, and link cause & effect
6-9 yrs
During normal, asymptomatic days, the asthmatic will take a/an __1__ (green zone); when entering the caution zone (yellow), where symptoms develop, the asthmatic will add a/an __2__; when symptoms are severe (red zone - danger), a/an __3__ will be added
1. Low-dose ICS
2. Rescue inhaler (albuterol)
3. Oral steroid
The nurse reviews an arterial blood gas report for a client with chronic obstructive pulmonary disease (COPD). The results are: pH 7.25; PCO2 62; PO2 70; HCO3 34. The nurse should first:
- Apply a 100% nonrebreather mask
- Assess the vital signs
- Reposition the client
- Prepare for intubation
B: Clients with chronic COPD have CO2 retention and the respiratory drive is stimulated when the PO2 decreases. The heart rate, respiratory rate, and the blood pressure should be evaluated to determine if the client is hemodynamically stable. Symptoms, such as dyspnea, should also be assessed. Oxygen supplementation, if indicated, should be titrated upward in small increments. There is no indication that the client is experiencing respiratory distress requiring intubation.
A client’s arterial blood gas values are as follows: pH 7.31; PaO2 80 mmHg; PaCO2 65 mmHg; HCO3 36 mEq/L. The nurse should assess the client for:
- Cyanosis
- Flushed skin
- Irritability
- Anxiety
B: The high PaCO2 level causes flushing due to vasodilation. The client also becomes drowsy and lethargic because carbon dioxide has a depressant effect on the central nervous system. Cyanosis is a sign of hypoxia. Irritability and anxiety are not common with a PaCO2 level of 65 mmHg but are associated with hypoxemia.