BMD 330 Chapter 21 - Infectious Diseases Manifesting in the Cardiovascular and Lymphatic Systems
The circulatory system is a ____ system which carries ____ to the tissues and ____ away.
The circulatory system is a closed system which carries oxygen to the tissues and carbon dioxide away.
- Heart - Pumps the blood
- Blood Vessels - Carry blood to and from all regions of the body
- Provides tissues with oxygen and nutrients
- Carries away carbon dioxide and waste products
Arteries
- Carry blood away from the heart
- Arterioles are smaller branches
Veins
- Carry blood toward the heart
- Venules are smaller viens
Capillaries
- Smallest blood vessels
- Connect venules and arterioles
True or False: Deoxygenated blood moves away from the heart.
False; Deoxygenated blood comes toward the heart to get oxygenated.
What system is the main source of immune cells and fluids?
Lymphatic System
The lymphatic systems consists of:
- Mainly lymphatic vessels - Roughly parallel the blood vessels
- Lymph nodes - Cluster at the groin, neck, armpit, and intestines
- Spleen - Responsible for filtration, prevention of infection, and RBC and platelet storage
Lymphatic systems collects what?
- Collects fluid that has left the blood vessels and entered tissues, filters it of impurities and infectious agents, and returns it to the blood
- Also used for fat transport and monitor for infectious agents
What is the main concern/problem of the cardiovascular system?
The cardiovascular system has access to the entire body, including the most sterilized environments like the brain --> So we need surveillance constantly and those are usually via WBCs
Defenses in the bloodstream?
- WBCs
- Lymphocytes - Adaptive immunity
- Phagocytes - Critical to innate and adaptive immune responses
White blood cells can be divided into:
- Granular
- Non-Granular
Non-Granular consists of (or can be further broken down into two categories):
- Lymphocyte - B and T cells
- Monocyte - Dendritic cells and Macrophages
Granular cells consists of
- Eosinophil
- Neutrophil
- Basophil
The suffice -emia means...
in the blood or the condition involves the blood
Viremia
Viruses that cause meningitis
Fungemia
Fungi in the blood
Bacteremia
Presence of bacteria in the blood
Septicemia
- Bacteria flourishing and growing in the bloodstream
- Can lead to decreased blood pressure, which leads to septic shock
What is the normal biota of the cardiovascular system?
None; because it is a closed system
COVID-19 is caused by severe ____ _____ syndrome coronavirus starting a pandemic in December ____.
COVID-19 is caused by severe acute respiratory syndrome coronavirus starting a pandemic in December 2019.
SARS-CoV-2 stands for...
Severe Acute Respiratory Syndrome Coronavirus #2
COVID-19 can access the ____________ system which causes it to....
COVID-19 can access the cardiovascular system and can spread throughout the body.
True or False: All coronaviruses infected humans.
False;
- Four other coronaviruses have infected humans causing minor upper respiratory infections.
- A different SARS virus caused an outbreak in 2003 starting in China
- In 2012, MERS-CoV started spreading in Middle Eastern countries
How did the pandemic begin?
- It has been thought that the coronavirus have been circulating in bats for a very long time
- It experienced one or more mutations to make it capable of infecting, multiplying, and transmitting among humans
- Humans contracted it in a wildlife market in Wuhan, China in 2019
SARS-CoV-2 is one of the ____ members of the ___________ family that infects humans.
SARS-CoV-2 is one of the seven members of the Coronaviridae family that infects humans.
What is the purpose of the spike (S) protein on SARS-CoV-2?
The S protein of the virus attaches to the ACE-2 host cell protein and uses it to initiate its entry into the cell
Where are the ACE-2 proteins found?
- Surface of cells in the lungs, brain, heart blood vessels, kidneys, liver, placenta, and GI tract
The viral particles of SARS-CoV-2 are transmitted via...
The viral particles of SARS-CoV-2 are transmitted via respiratory droplets
What type of virus is SARS-CoV-2? Enveloped or Non-Enveloped, RNA or DNA?
- Enveloped, positive-sense RNA viruses with spike (S) proteins
What causes much of the inflammation and damage in SARS-CoV-2?
- The damage usually comes from the cytokine storm (cytokines are usually not directed, so they try to kill any live cells whether it is our cells or the microbe) and sometimes we can develop autoimmunity.
- Cytokines is usually what causes majority of the damage and the inflammation.
There are three variants of SARS-CoV-2 due to mutations...
- Alpha - More contagious than the original virus
- Delta - Twice as transmissible than the original and more deadly
- Omicron - BA2 dominated in North America for the first half of 2022
Symptoms and Signs of COVID-19
- Most prominent is respiratory symptoms
- Infection can set off a cytokine storm, leading to hyperinflammation, both in lungs and in other organs, including digestive tract
- Systemic effects of the virus include skin rashes, muscle pain, heart damage, joint pain, and blood clots
- Considered Neurotrophic
- Up to one third of infections can be asymptomatic and many others are mild
What does neurotrophic mean?
- Loss of taste and smell, can lead to headaches and even long-term cognitive decline and dementia
What are some COVID-19 prevention and treatment?
- Mitigation efforts were initially put in place with the use of masks, social distancing, and handwashing.
- Emergency use authorization approval by the FDA in the United States was given to three vaccines
- Another vaccine (Paxlovid) was approved in late 2021 for patients with high risk for COVID complications, proved effective in controlling the infection if started soon after the infection
What were the 3 original vaccines approved by FDA for COVID-19?
- Pfizer BioNTech and Moderna consist of mRNA coding for spike protein of SARS-CoV-2
- Johnson and Johnson is an adenovirus viral vector vaccine encoding for the SARS-CoV-2 spike protein
What is endocarditis?
Inflammation of the inner lining of the heart (endocardium)
There are two types of endocarditis:
- Acute
- Subacute
What predisposes patients to endocarditis?
- Damage to heart valves or prosthetic heart valves
- Can also be caused by vascular trauma or circulating immune complexes
Signs and symptoms of acute endocarditis:
- (> a week)
- Fever, anemia, abnormal heartbeat, symptoms of heart attack, shortness of breath, and chills
- Abdominal or side pain, Janeway lesions (painless when touched), and Osler's nodes (painful when touched)
Signs and symptoms of subacute endocarditis
- About a month
- Similar to acute endocarditis
- Develop more slowly and are less pronounced
- Enlarged spleen, clubbed fingers, and toes
The causative agent of acute endocarditis is
The causative agent of acute endocarditis is Staphylococcus aureus, Streptococcus pyogenes, S. pneumoniae, and others.
The causative agent of subacute endocarditis is
The causative agent of subacute endocarditis is alpha-hemolytic streptococci
What is the most common mode of transmission for acute endocarditis?
Parental
What is the most common mode of transmission for subacute endocarditis?
Endogenous transfer of normal biota to bloodstream
Sepsis is also known as...
Sepsis is also known as septicemia which occurs when organisms are actively multiplying in the blood.
- Can be caused by many different bacteria and a few fungi
What are signs and symptoms of sepsis?
- Fever, altered mental state, shaking chills, and gastrointestinal symptoms
- Increased breathing rate, respiratory alkalosis, and low blood pressure resulting in loss of fluid from vasculature
Endotoxic show is a result of gram-______ bacteria multiplying in the bloodstream and releasing ____.
Endotoxic show is a result of gram-negative bacteria multiplying in the bloodstream and releasing endotoxin (usually the LPS).
What occurs as a result of endotoxic shock?
- Stimulate a massive inflammatory response mediated by cytokines
- Leads to drastic of blood pressure
- Gram-positive can instigate a similar series of events when fragments of the cell wall are released into the bloodstream
What is the virulence factor of sepsis?
Cell wall or membrane components
There are three manifestations of plague (PBS)...
- Pneumonic - Respiratory Disease
- Bubonic - Infection causes inflammation and necrosis of the lymph node or a bubo in the groin or axilla
- Septicemic ("Black Death") - Results in disseminated intravascular coagulation, subcutaneous hemorrhage, and purpura that degenerate into necrosis and gangreen; 30-50% mortality with treatment; 100% mortality without treatment
The causative organism of plague is...
Yersinia pestis
How it Yersinia pestis transmitted?
Via fleas; usually found on animals like rats
Pneumonic
- Respiratory droplets
- Looks similar to pneumonia
- Bloody/watery cough
Bubonic
- Bile of flea
- Swollen lymph nodes almost the size of eggs and they ooze pus
Septicemic
- Dissemination
- When bacteria is in the blood
- May experience gangreene
The number of bacteria require to initiate infection in bubonic (septicemic) cases is ______.
Only 3 to 50 cells
"Rabbit Fever"
Tularemia
What is Tularemia?
A zoonotic disease endemic throughout Northern Hemisphere
What are symptoms of Tularemia?
- Headache
- Backache
- Fever
- Chills
- Malaise
- Weakness
What are signs of Tularemia?
- Ulcerative skin lesions (most common sign to tell it is is Tularemia)
- Swollen lymph glands
- Conjunctival inflammation
- Sore Throat
- Intestinal Disruption
- Pulmonary involvement
What is the mortality rate of Tularemia for those without proper treatment?
30%
The causative agent of Tularemia is...
Francisella tularensis
Francisella tularensis is gram-________ and the infectious dose is _____.
Francisella tularensis is gram-negative and the infectious dose is 10 to 50.
Francisella tularensis is a faculative ________ bacterium.
Intracellular
Chief reservoirs of Francisella tularensis are:
- Rabbits and rodents
- Sometimes skunks, beavers, opossums, foxes, and other wild animals are also reservoirs
Lyme disease is a ____ acting, progressive syndrome in which ____ is an early symptom.
Lyme disease is a slow-acting, progressive syndrome in which bull's eye rash is an early symptom
What are some other signs and symptoms of Lyme Disease?
- Fever, headache, stiff neck, and dizziness, joint pain, and swollen lymphs
- Progresses to cardiac and neurological symptoms
- Develops into crippling polyarthritis after several weeks to months
The causative agent of Lyme Disease is ______ which has a ____ morphology.
The causative agent of Lyme Disease is Borrelia burgdoferi which has a spirochete morphology.
What is special about the virulence of Borrelia burgoferi?
It has the ability to adapt so it evades the immune system by changing antigens. It also has multiple proteins for attachment to host cells
Cycle of Lyme Disease
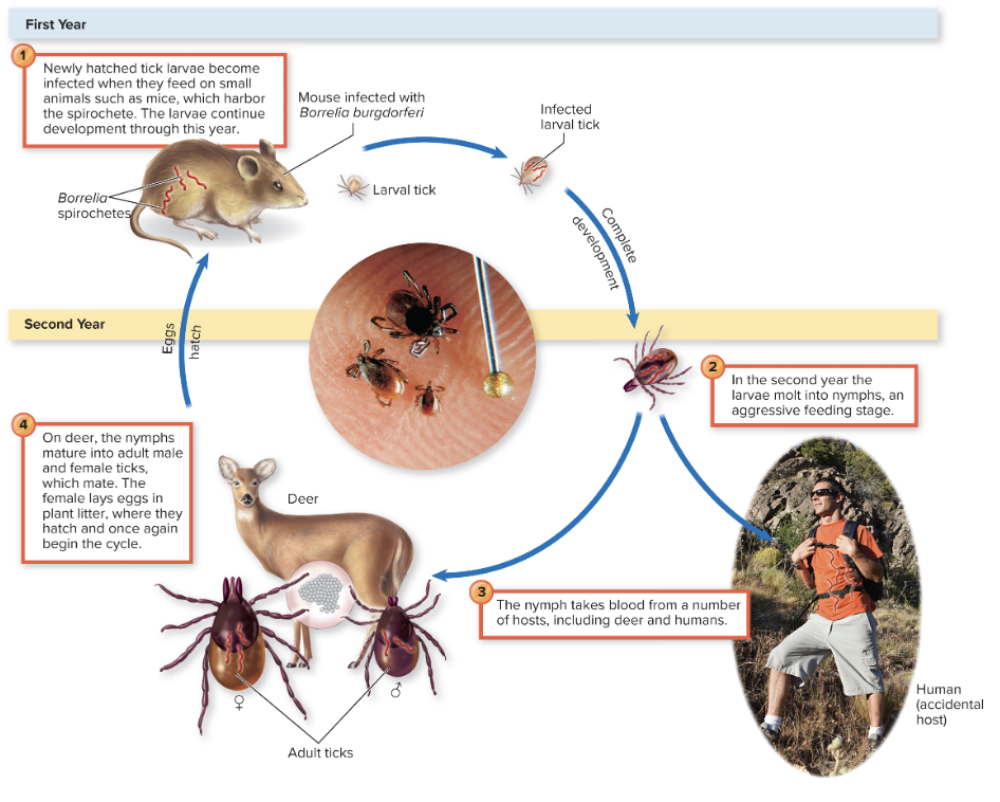
- We (humans) are the accidental hosts, but primarily they infect small animals who are bitten by larval ticks.
- They infect small mammals and ingest the bacteria. These infected ticks grow up and develop and feed on larger animals such as deer. And this is also where they tend to mate. But again, we are the accidental host and we are usually not a part of the life cycle (it cannot replicate or get back into the cycle once it gets into us)
What is the common mode of transmission of Borrelia burdgdorferi?
- Biological Vector (tick)
The ________ virus causes mono or infectious mononucleosis.
The Epstein-Barr virus causes mono or infectious mononucleosis.
The EBV is a ____-_____-4.
Herpes Simplex 4
Epstein-Barr Virus contains ____ form of DNA/RNA that is spliced into host _____.
Epstein-Barr Virus contains circular form of DNA that is spliced into host cell DNA
What allows EBV to evade the host immune respone?
Its latency and ability to splice into host cell DNA allows it to evade the host immune response.
Is EBV common?
Yes
- By adulthood, more than 90% of the world’s population has been infected with EBV
- Infection during the teen years results in disease about 30% to 77% of the time
- Usually, self-limiting
The most common symptom of mono is...
- Extreme fatigue and swollen spleen, which can cause spleen rupturing
- Can also cause sore throat and swollen limbs
Anthrax
- The pathogen multiplies in large numbers in the blood
- Septicemic anthrax is a possible outcome of all forms of anthrax
- Zoonotic disease of herbivores
- Infections can cause symptoms in various locations of the body:
- On the skin: cutaneous anthrax
- In the lungs: pulmonary anthrax
- In the gastrointestinal tract: gastrointestinal anthrax
- In the central nervous system: anthrax meningitis
Anthrax is usually found in the ____ and affects primarily _________.
Anthrax is usually found in the soil and affects primarily sheep and cattle.
What is the causative agent of anthrax?
Bacillus anthracis
Morphology of Bacillus anthracis?
- Gram-Positive Endospore-Forming Rod
What is the virulence factor of Bacillus anthracis?
Has a unique triple protein exotoxin (tripartite toxin) that causes a:
- Edema Factor: disruption to the water balance in host cells
- Lethal Factor: can combine with with edema and become a more lethal toxin; causes inflammation to the alveolar epithelium
- Protective Factor: Commonly use for targeting.
Anthrax is aerobic or anaerobic?
Aerobic
- Also catalase positive
What are hemorrhagic fever diseases?
- Agents that infect the blood and lymphatics
- Extreme fevers accompanied by internal hemorrhaging (internal bleeding from damaged blood vessels)
- Mainly caused by RNA viruses
- Distribution related to the distribution of Aedes genus of mosquito
- Prevalence fluctuates due to global warming patterns
What are the five Hemorrhagic Fevers? What do they all have in common?
They are all carried by Aedes mosquitoes
- Yellow Fever
- Dengue Fever
- Chikungunya
- Ebola and Marburg Fevers
- Lassa Fever
Yellow Fever
- Symptoms include fever, chills, severe headaches, and may transition to high fever, eventually yellowing of the skin and eyes.
- Jaundice and internal bleeding
- Currently, there is no treatment, but there are vaccines available
- More frequent in rainy climates
- Endemic in Africa and South America
Dengue Fever
- Usually asymptomatic or mild, but can cause high fever, headache, swollen glands, muscle aches, and if affected again, may have more severe symptoms, including persistent vomiting, bleeding gums or nose, as well as bloody stool and weakness, which may last long after clearing of other symptoms
- Endemic in Southeast Asia and Africa; epidemics have occurred in South and Central America and the Caribbean
Chikungunya
- Marked by fever, severe joint pulling (especially in the hands, feet, knees, and ankles), headache, muscle pain, nausea, and sometimes rash
- No current treatments
- Vaccination is recommended, especially for those who are traveling to endemic areas
- Endemic in Africa; arrived in Central America in 2013 and in the United States and Europe in 2014
Ebola and Marburg Fevers
Cannot be transmitted by mosquitoes, but rather via respiratory droplets from infected animals and bodily fluids
Bats are thought to natural reservoir of Ebola
Capillary fragility is extreme and patients can bleed from their orifices and mucous membranes
- Ebola: Two phases: Dry that then turns into wet, where:
- Dry – Starts with fever, aches, pains, and fatigue
- Wet – Diarrhea, vomiting, and unexplained bleeding
Marburg fever begins with the high fever, severe headache, and severe malise. After 5 days of the disease, patients may develop hemorrhagic manifestations, and usually death is from bleeding out
Lassa Fever
- Cannot be transmitted by mosquitoes, but rather via respiratory droplets from infected animals and bodily fluids
- Similar to Marburg where symptoms become serious, like bleeding, face swelling, and shock.
- And if you eventually get over Lassa, long-term complications can include things like deafness
- Reservoir of virus is multimammate rat
How are nonhemorrhagic fevers characterized?
- Characterized by a high fever but without fragility leading to hemorrhagic symtpoms
- Mostly caused by multiple bacterial species and one protozoan (Babesia) species
Nonhemorrhagic fevers are caused by bacteria: (list them)
- Brucellosis
- Q Fever
- Cat-Scratch Disease
- Trench Fever
- Ehrilichiosis
- Anaplasmosis
- Spotted fever rickettsiosis
Brucella is a gram-______.
- Gram-Negative
- Coccobacilli
Where does Brucella live?
- Lives in the phagocytic cells that carry bacteria into the bloodstream causing focal lesions in the liver, spleen, bone marrow, and kidney
- Most prominent manifestation of human brucellosis is fluctuating pattern of fever, which is the origin of the common name undulant fever
The causative agent of Q Fever is....
Coxiella burnetti
Q in Q fever stands for...
Q in Q fever stands for query, due to the frustration in discovering the cause of the disease
Coxiella burnetti is a _____, pleomorphic, gram-______ bacteria.
Coxiella burnetti is a small, pleomorphic, gram-negative bacteria.
- It is a intraceullar parasite and forms and endospore-like structure
How is Q Fever (Coxiella burnetti) transmitted?
- Ticks play an essential role in transmission between wild and domestic animals, but not transmit the disease to humans.
- Transmitted by contact with infected animals.
- It is a natural species found in animals and can be found in much of their bodily fluid, especially animal products of birth and sometimes raw milk.
- Usually, people are unaffected or asymptomatic, but some will develop flu-like symptoms
- A very small percentage can develop chronic Q fever once infected which can eventually lead to endocarditis.
Cat-scratch disease is caused by...
Cat-scratch disease is caused by Bartonella henselae
Morphology of Bartonella henselae?
- Gram-Negative
- Rod
- Fastidious, will grow on blood agar
How is cat-scratch disease transmitted?
Infection connected with being clawed or bitten by a cat
- Present in over 40% of cats
When infected by Bartonella henselae, symptoms start ____ and include ___.
When infected by Bartonella henselae, symptoms start 1 to 2 weeks afters and include:
- Cluster of small papules at the inoculation site
- Lymph nodes swell and become pus filled
- One-third of patients experience a high fever
Trench fever is caused by...
Trench fever is caused by Bartonella quintana
How is Trench fever transmitted?
Carried by lice, spread when louse feces enter a bite wound
What are symptoms of Trench fever?
- 5 to 6 days fever, leg pains, headache, chills, muscle aches, macular rash
- Endocarditis can develop
What is the causative agent of spotted fever rickettsioses (SFR)?
Rickettsia rickettsii
How is rickettsia rickettsii transmitted?
Hard Ticks
Signs and Symptoms of Spotted Rever Rickettsioses
- Chills, fever, headache, muscular pain
- Distinctive spotted rash occurs 2 to 4 days after the prodome (initial stage)
- If untreated, lesions merge and become necrotic
- Cardiovascular disruption: hypotension, thrombosis, hemorrhage
- Treatment usually has to be done immediately and if untreated, it can cause serious cardiovascular complications
______ is spread via mosquitoes, but not person to person.
Malaria
Signs and symptoms of malaria occur within ______ hour intervals
48 or 72
Signs and symptoms of malaria include
- Malaise, fatigue, aches, nausea with or without diarrhea
- Chills, fever, and sweating
There are two types of malaria:
- Falciparum malaria: persistent fever, cough, and weakness for weeks without relief
- Cerebral malaria: small blood vessels in the brain become obstructed, leading to coma and death
What is the causative agent of malaria?
Plasmodium
There are two phases of plasmodium:
- Asexual phase: carried out in the human
- Sexual phase: carried out in the mosquito
______________ live in animal hosts and lack locomoter appendages in the mature states
Apicomplexans
Malaria pathogenesis and virulence factors include
- Invasion of merozoites into RBCs causes the release of fever-inducing chemicals into the bloodstream
- Plasmodium metabolizes glucose at a high rate
- Damage to RBCs causes anemia
- Accumulation of malarial products in the liver and immune stimulation in the spleen can lead to enlargement of these organs
- RBC adhesion to blood vessels in the brain adds to its virulence
- Parasite undergoes antigenic variation
Malaria Prevention
Long-term mosquito abatement
- Elimination of standing water
- Spraying of insecticides
- Introducing sterile male mosquitoes into populations
- Mosquito nets, screens, repellants
Human chemoprophylaxis
- Prophylactic treatment for travelers
- A vaccine shows promise and is recommended for children in endemic areas
Human immunodeficiency virus is a _____.
Retrovirus
True or False: HIV causes AIDs (immune deficiency syndrome)
True
Symptoms of HIV
- Pneumonia caused by Pneumocystitis jiroveci
- Kaposi’s sarcoma
- Sudden weight loss
- Swollen lymph nodes
- General loss of immune function
Signs and symptoms of HIV are tied to the level of virus in the blood and the level of ____ cells in the blood
Signs and symptoms of HIV are tied to the level of virus in the blood and the level of T cells in the blood
To be diagnosed with AIDs, T cell count has be to ____________.
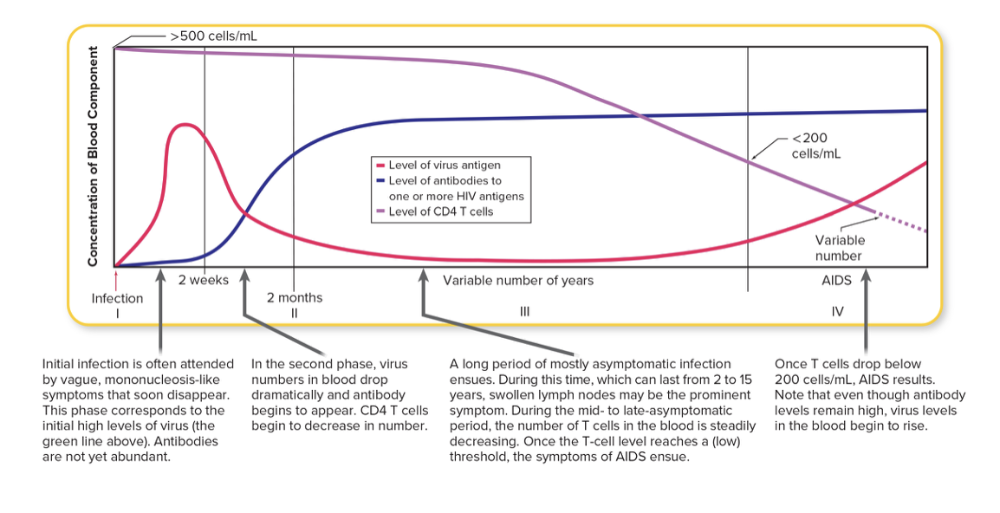
To be diagnosed with AIDs, T cell count has be to less than 200.
What are the initial symptoms of HIV infection and AIDs?
- Fatigue
- Diarrhea
- Weight loss
- Neurological Changes
Other signs and symptoms of HIV infection and AIDs
- Opportunistic infections and neoplasms
- Severe immune deregulation, hormone imbalances, and metabolic disturbances
- Weight loss, diarrhea, and poor nutrient absorption
- Protracted fever, fatigue, sore throat, and night sweats
- Lesions on the brain, meninges, spinal column, and peripheral nerves
What is the causative agent of HIV Infection and AIDs?
Retrovirus in the genus Lentivirus
- Contains reverse transcriptase that catalyzes the replication of double-stranded DNA from single-stranded RNA
- Viral genes become permanently integrated into the host genome
Two types of HIV
- HIV-1
- HIV-2
Most dominant form of HIV in the word; most related to simian immunodeficiency viruses in chimpanzees
HIV-1
General Multiplication Cycle of HIV
1. Virus is absorbed and endocytosed, and the twin RNAs are uncoated. Reverse transcriptase catalyzes the synthesis of a single complementary strand of DNA (ssDNA). This single strand serves as a template for synthesis of a double stranded DNA. In latency, dsDNA is inserted into the host chromosome as provirus
2. After latent period, various immune activators stimulate the infected cell, causing reactivation of provirus genes and production of viral mRNA
3. HIV mRNA is translated by the cell's synthetic machinery into virus components (capsid, reverse transcriptase, spikes), and the viruses are assembled. Budding of mature viruses lyses the infected cell
How is HIV transmitted?
Any form of intimate contact involving transfer of blood can be potential source of infection
- Trauma and needle sharing
- Sexual transmission
- Breast milk
Urine, tears, sweat, and saliva are not considered sources of infection
HIV Epidemiology
- Since the beginning of the epidemic in the 1980s, 60 million have become infected and more than 30 million have died of HIV-related causes worldwide
Global estimate:
- 38 million infected worldwide
- 1.2 million infections currently in the United States
- In the United States, 15% of those infected with HIV are unaware
How is HIV cultured and diagnosed?
A person is diagnosed as having HIV infection if they have tested positive for exposure to the human immunodeficiency virus
- This diagnosis is not the same as having AIDS
Viral testing is based on detection of antibodies specific to the virus in serum or other fluids
- ELISA
- Latex agglutination
- Rapid antibody tests
What are two criteria to diagnosis AIDs?
Diagnosis with Stage 3 HIV infection requires both:
- Test positive for the virus
- CD4 count of fewer than 200 cells per microliter of blood
How is HIV prevented?
- Avoidance of unprotected sexual contact with infected persons
- Barrier protection should be used when having sex with anyone whose HIV status is unknown
- Not sharing needles or by cleaning needles with bleach and then rinsing before another use
- HIV-positive individuals with uninfected partners should begin a regimen of antiretroviral drugs
- Clinical trials of various vaccines are ongoing
When should treatment of HIV infection and AIDs occur?
- Treatment should begin immediately after HIV diagnosis
What are treatments of HIV infection and AIDs?
- Antiviral chemotherapy and a variety of drugs to prevent or treat opportunistic infections and other complications such as wasting disease
- Three-drug cocktail containing two nucleoside analog reverse transcriptase inhibitors and one nonnucleoside reverse transcriptase inhibitor
What are the mechanisms of anti-HIV drugs?
- Nucleoside analogs that inhibit reverse transcriptase - Inserted in place of the natural nucleotide by reverse transcriptase but block further action of the enzyme and synthesis of viral DNA. Non-nucleotide RT inhibitors are also in use.
- Protease inhibitors - Plug into active sites on HIV protease. This enzyme is necessary to cut elongated HIV protein strands and produce functioning smaller protein units. Because the enzyme is blocked, the proteins remain uncut, and abnormal defective viruses form.
- Integrase inhibitors - Attach to the enzyme required to splice the dsDNA from HIV into host genome. This will prevent formation of the provirus and block future virus multiplication in that cell
Bacillus anthracis
- Gram-Positive Endospore-Forming Bacteria
- Causes Anthrax
Staphylococcus aureus
- Gram-Positive Bacteria
- Causes Acute Endocarditis
Streptococcus pneumoniae
- Gram-Positive Bacteria
- Causes Acute Endocarditis
Yersinia pestis
- Gram-Negative Bacteria
- Causes Plague
Borrelia burgdorferi
- Gram-Negative Bacteria
- Causes Lyme Disease
Bartonella henselae
- Gram-Negative Bacteria
- Causes Cat-Scratch Disease
Rickettsia species
- Gram-Negative Bacteria
- Causes Spotted Fever Rickettsiosis
Epstein–Barr virus
- DNA Virus
- Causes Infectious Mononucleosis
SARS-CoV-2
- RNA Virus
- Causes COVID-19
Yellow Fever Virus
- RNA Virus
- Causes Hemorrhagic Fever
HIV
- Retroviruses
- Causes HIV infection and AIDs