Instructions for Side by Side Printing
- Print the notecards
- Fold each page in half along the solid vertical line
- Cut out the notecards by cutting along each horizontal dotted line
- Optional: Glue, tape or staple the ends of each notecard together
BMD 330 Chapter 21 - Infectious Diseases Manifesting in the Cardiovascular and Lymphatic Systems
front 1 The circulatory system is a ____ system which carries ____ to the tissues and ____ away. | back 1 The circulatory system is a closed system which carries oxygen to the tissues and carbon dioxide away.
|
front 2 Arteries | back 2
|
front 3 Veins | back 3
|
front 4 Capillaries | back 4
|
front 5 True or False: Deoxygenated blood moves away from the heart. | back 5 False; Deoxygenated blood comes toward the heart to get oxygenated. |
front 6 What system is the main source of immune cells and fluids? | back 6 Lymphatic System |
front 7 The lymphatic systems consists of: | back 7
|
front 8 Lymphatic systems collects what? | back 8
|
front 9 What is the main concern/problem of the cardiovascular system? | back 9 The cardiovascular system has access to the entire body, including the most sterilized environments like the brain --> So we need surveillance constantly and those are usually via WBCs |
front 10 Defenses in the bloodstream? | back 10
|
front 11 White blood cells can be divided into: | back 11
|
front 12 Non-Granular consists of (or can be further broken down into two categories): | back 12
|
front 13 Granular cells consists of | back 13
|
front 14 The suffice -emia means... | back 14 in the blood or the condition involves the blood |
front 15 Viremia | back 15 Viruses that cause meningitis |
front 16 Fungemia | back 16 Fungi in the blood |
front 17 Bacteremia | back 17 Presence of bacteria in the blood |
front 18 Septicemia | back 18
|
front 19 What is the normal biota of the cardiovascular system? | back 19 None; because it is a closed system |
front 20 COVID-19 is caused by severe ____ _____ syndrome coronavirus starting a pandemic in December ____. | back 20 COVID-19 is caused by severe acute respiratory syndrome coronavirus starting a pandemic in December 2019. |
front 21 SARS-CoV-2 stands for... | back 21 Severe Acute Respiratory Syndrome Coronavirus #2 |
front 22 COVID-19 can access the ____________ system which causes it to.... | back 22 COVID-19 can access the cardiovascular system and can spread throughout the body. |
front 23 True or False: All coronaviruses infected humans. | back 23 False;
|
front 24 How did the pandemic begin? | back 24
|
front 25 SARS-CoV-2 is one of the ____ members of the ___________ family that infects humans. | back 25 SARS-CoV-2 is one of the seven members of the Coronaviridae family that infects humans. |
front 26 What is the purpose of the spike (S) protein on SARS-CoV-2? | back 26 The S protein of the virus attaches to the ACE-2 host cell protein and uses it to initiate its entry into the cell |
front 27 Where are the ACE-2 proteins found? | back 27
|
front 28 The viral particles of SARS-CoV-2 are transmitted via... | back 28 The viral particles of SARS-CoV-2 are transmitted via respiratory droplets |
front 29 What type of virus is SARS-CoV-2? Enveloped or Non-Enveloped, RNA or DNA? | back 29
|
front 30 What causes much of the inflammation and damage in SARS-CoV-2? | back 30
|
front 31 There are three variants of SARS-CoV-2 due to mutations... | back 31
|
front 32 Symptoms and Signs of COVID-19 | back 32
|
front 33 What does neurotrophic mean? | back 33
|
front 34 What are some COVID-19 prevention and treatment? | back 34
|
front 35 What were the 3 original vaccines approved by FDA for COVID-19? | back 35
|
front 36 What is endocarditis? | back 36 Inflammation of the inner lining of the heart (endocardium) |
front 37 There are two types of endocarditis: | back 37
|
front 38 What predisposes patients to endocarditis? | back 38
|
front 39 Signs and symptoms of acute endocarditis: | back 39
|
front 40 Signs and symptoms of subacute endocarditis | back 40
|
front 41 The causative agent of acute endocarditis is | back 41 The causative agent of acute endocarditis is Staphylococcus aureus, Streptococcus pyogenes, S. pneumoniae, and others. |
front 42 The causative agent of subacute endocarditis is | back 42 The causative agent of subacute endocarditis is alpha-hemolytic streptococci |
front 43 What is the most common mode of transmission for acute endocarditis? | back 43 Parental |
front 44 What is the most common mode of transmission for subacute endocarditis? | back 44 Endogenous transfer of normal biota to bloodstream |
front 45 Sepsis is also known as... | back 45 Sepsis is also known as septicemia which occurs when organisms are actively multiplying in the blood.
|
front 46 What are signs and symptoms of sepsis? | back 46
|
front 47 Endotoxic show is a result of gram-______ bacteria multiplying in the bloodstream and releasing ____. | back 47 Endotoxic show is a result of gram-negative bacteria multiplying in the bloodstream and releasing endotoxin (usually the LPS). |
front 48 What occurs as a result of endotoxic shock? | back 48
|
front 49 What is the virulence factor of sepsis? | back 49 Cell wall or membrane components |
front 50 There are three manifestations of plague (PBS)... | back 50
|
front 51 The causative organism of plague is... | back 51 Yersinia pestis |
front 52 How it Yersinia pestis transmitted? | back 52 Via fleas; usually found on animals like rats |
front 53 Pneumonic | back 53
|
front 54 Bubonic | back 54
|
front 55 Septicemic | back 55
|
front 56 The number of bacteria require to initiate infection in bubonic (septicemic) cases is ______. | back 56 Only 3 to 50 cells |
front 57 "Rabbit Fever" | back 57 Tularemia |
front 58 What is Tularemia? | back 58 A zoonotic disease endemic throughout Northern Hemisphere |
front 59 What are symptoms of Tularemia? | back 59
|
front 60 What are signs of Tularemia? | back 60
|
front 61 What is the mortality rate of Tularemia for those without proper treatment? | back 61 30% |
front 62 The causative agent of Tularemia is... | back 62 Francisella tularensis |
front 63 Francisella tularensis is gram-________ and the infectious dose is _____. | back 63 Francisella tularensis is gram-negative and the infectious dose is 10 to 50. |
front 64 Francisella tularensis is a faculative ________ bacterium. | back 64 Intracellular |
front 65 Chief reservoirs of Francisella tularensis are: | back 65
|
front 66 Lyme disease is a ____ acting, progressive syndrome in which ____ is an early symptom. | back 66 Lyme disease is a slow-acting, progressive syndrome in which bull's eye rash is an early symptom |
front 67 What are some other signs and symptoms of Lyme Disease? | back 67
|
front 68 The causative agent of Lyme Disease is ______ which has a ____ morphology. | back 68 The causative agent of Lyme Disease is Borrelia burgdoferi which has a spirochete morphology. |
front 69 What is special about the virulence of Borrelia burgoferi? | back 69 It has the ability to adapt so it evades the immune system by changing antigens. It also has multiple proteins for attachment to host cells |
front 70 Cycle of Lyme Disease | back 70 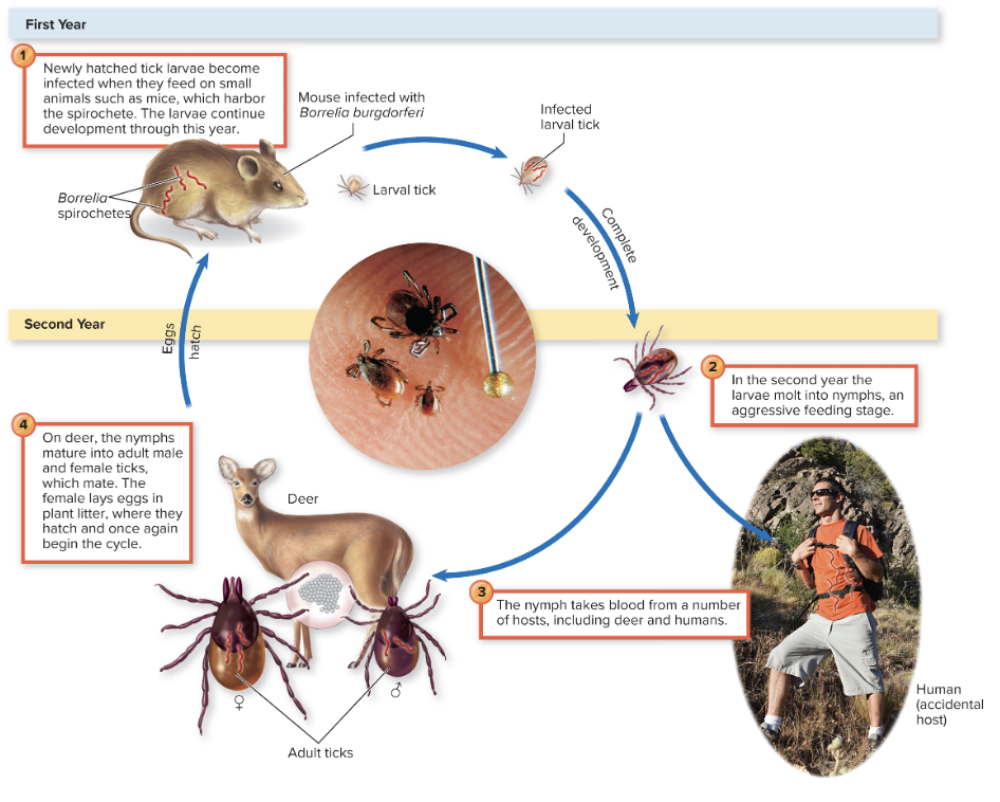
|
front 71 What is the common mode of transmission of Borrelia burdgdorferi? | back 71
|
front 72 The ________ virus causes mono or infectious mononucleosis. | back 72 The Epstein-Barr virus causes mono or infectious mononucleosis. |
front 73 The EBV is a ____-_____-4. | back 73 Herpes Simplex 4 |
front 74 Epstein-Barr Virus contains ____ form of DNA/RNA that is spliced into host _____. | back 74 Epstein-Barr Virus contains circular form of DNA that is spliced into host cell DNA |
front 75 What allows EBV to evade the host immune respone? | back 75 Its latency and ability to splice into host cell DNA allows it to evade the host immune response. |
front 76 Is EBV common? | back 76 Yes
|
front 77 The most common symptom of mono is... | back 77
|
front 78 Anthrax | back 78
|
front 79 Anthrax is usually found in the ____ and affects primarily _________. | back 79 Anthrax is usually found in the soil and affects primarily sheep and cattle. |
front 80 What is the causative agent of anthrax? | back 80 Bacillus anthracis |
front 81 Morphology of Bacillus anthracis? | back 81
|
front 82 What is the virulence factor of Bacillus anthracis? | back 82 Has a unique triple protein exotoxin (tripartite toxin) that causes a:
|
front 83 Anthrax is aerobic or anaerobic? | back 83 Aerobic
|
front 84 What are hemorrhagic fever diseases? | back 84
|
front 85 What are the five Hemorrhagic Fevers? What do they all have in common? | back 85 They are all carried by Aedes mosquitoes
|
front 86 Yellow Fever | back 86
|
front 87 Dengue Fever | back 87
|
front 88 Chikungunya | back 88
|
front 89 Ebola and Marburg Fevers | back 89 Cannot be transmitted by mosquitoes, but rather via respiratory droplets from infected animals and bodily fluids Bats are thought to natural reservoir of Ebola Capillary fragility is extreme and patients can bleed from their orifices and mucous membranes
Marburg fever begins with the high fever, severe headache, and severe malise. After 5 days of the disease, patients may develop hemorrhagic manifestations, and usually death is from bleeding out |
front 90 Lassa Fever | back 90
|
front 91 How are nonhemorrhagic fevers characterized? | back 91
|
front 92 Nonhemorrhagic fevers are caused by bacteria: (list them) | back 92
|
front 93 Brucella is a gram-______. | back 93
|
front 94 Where does Brucella live? | back 94
|
front 95 The causative agent of Q Fever is.... | back 95 Coxiella burnetti |
front 96 Q in Q fever stands for... | back 96 Q in Q fever stands for query, due to the frustration in discovering the cause of the disease |
front 97 Coxiella burnetti is a _____, pleomorphic, gram-______ bacteria. | back 97 Coxiella burnetti is a small, pleomorphic, gram-negative bacteria.
|
front 98 How is Q Fever (Coxiella burnetti) transmitted? | back 98
|
front 99 Cat-scratch disease is caused by... | back 99 Cat-scratch disease is caused by Bartonella henselae |
front 100 Morphology of Bartonella henselae? | back 100
|
front 101 How is cat-scratch disease transmitted? | back 101 Infection connected with being clawed or bitten by a cat
|
front 102 When infected by Bartonella henselae, symptoms start ____ and include ___. | back 102 When infected by Bartonella henselae, symptoms start 1 to 2 weeks afters and include:
|
front 103 Trench fever is caused by... | back 103 Trench fever is caused by Bartonella quintana |
front 104 How is Trench fever transmitted? | back 104 Carried by lice, spread when louse feces enter a bite wound |
front 105 What are symptoms of Trench fever? | back 105
|
front 106 What is the causative agent of spotted fever rickettsioses (SFR)? | back 106 Rickettsia rickettsii |
front 107 How is rickettsia rickettsii transmitted? | back 107 Hard Ticks |
front 108 Signs and Symptoms of Spotted Rever Rickettsioses | back 108
|
front 109 ______ is spread via mosquitoes, but not person to person. | back 109 Malaria |
front 110 Signs and symptoms of malaria occur within ______ hour intervals | back 110 48 or 72 |
front 111 Signs and symptoms of malaria include | back 111
|
front 112 There are two types of malaria: | back 112
|
front 113 What is the causative agent of malaria? | back 113 Plasmodium |
front 114 There are two phases of plasmodium: | back 114
|
front 115 ______________ live in animal hosts and lack locomoter appendages in the mature states | back 115 Apicomplexans |
front 116 Malaria pathogenesis and virulence factors include | back 116
|
front 117 Malaria Prevention | back 117 Long-term mosquito abatement
Human chemoprophylaxis
|
front 118 Human immunodeficiency virus is a _____. | back 118 Retrovirus |
front 119 True or False: HIV causes AIDs (immune deficiency syndrome) | back 119 True |
front 120 Symptoms of HIV | back 120
|
front 121 Signs and symptoms of HIV are tied to the level of virus in the blood and the level of ____ cells in the blood | back 121 Signs and symptoms of HIV are tied to the level of virus in the blood and the level of T cells in the blood |
front 122 To be diagnosed with AIDs, T cell count has be to ____________. | back 122 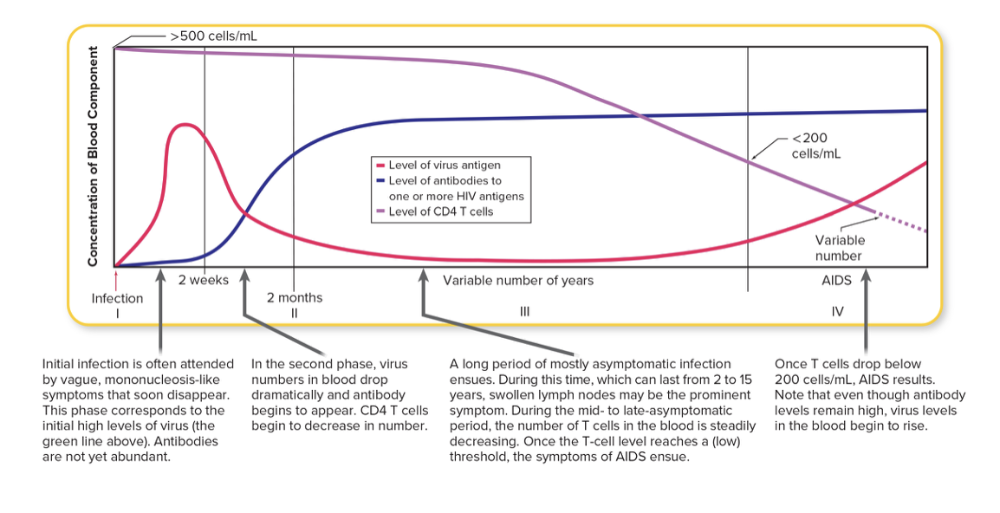 To be diagnosed with AIDs, T cell count has be to less than 200. |
front 123 What are the initial symptoms of HIV infection and AIDs? | back 123
|
front 124 Other signs and symptoms of HIV infection and AIDs | back 124
|
front 125 What is the causative agent of HIV Infection and AIDs? | back 125 Retrovirus in the genus Lentivirus
|
front 126 Two types of HIV | back 126
|
front 127 Most dominant form of HIV in the word; most related to simian immunodeficiency viruses in chimpanzees | back 127 HIV-1 |
front 128 General Multiplication Cycle of HIV | back 128 1. Virus is absorbed and endocytosed, and the twin RNAs are uncoated. Reverse transcriptase catalyzes the synthesis of a single complementary strand of DNA (ssDNA). This single strand serves as a template for synthesis of a double stranded DNA. In latency, dsDNA is inserted into the host chromosome as provirus 2. After latent period, various immune activators stimulate the infected cell, causing reactivation of provirus genes and production of viral mRNA 3. HIV mRNA is translated by the cell's synthetic machinery into virus components (capsid, reverse transcriptase, spikes), and the viruses are assembled. Budding of mature viruses lyses the infected cell |
front 129 How is HIV transmitted? | back 129 Any form of intimate contact involving transfer of blood can be potential source of infection
Urine, tears, sweat, and saliva are not considered sources of infection |
front 130 HIV Epidemiology | back 130
Global estimate:
|
front 131 How is HIV cultured and diagnosed? | back 131 A person is diagnosed as having HIV infection if they have tested positive for exposure to the human immunodeficiency virus
Viral testing is based on detection of antibodies specific to the virus in serum or other fluids
|
front 132 What are two criteria to diagnosis AIDs? | back 132 Diagnosis with Stage 3 HIV infection requires both:
|
front 133 How is HIV prevented? | back 133
|
front 134 When should treatment of HIV infection and AIDs occur? | back 134
|
front 135 What are treatments of HIV infection and AIDs? | back 135
|
front 136 What are the mechanisms of anti-HIV drugs? | back 136
|
front 137 Bacillus anthracis | back 137
|
front 138 Staphylococcus aureus | back 138
|
front 139 Streptococcus pneumoniae | back 139
|
front 140 Yersinia pestis | back 140
|
front 141 Borrelia burgdorferi | back 141
|
front 142 Bartonella henselae | back 142
|
front 143 Rickettsia species | back 143
|
front 144 Epstein–Barr virus | back 144
|
front 145 SARS-CoV-2 | back 145
|
front 146 Yellow Fever Virus | back 146
|
front 147 HIV | back 147
|