front 1 C - Cleaning the least-soiled areas prior to cleaning the most-soiled areas
The least-soiled areas should be cleaned first to prevent moving
more contaminants into the cleaner areas. | back 1 A nurse is assisting a patient with personal hygiene care. Which of
the following actions be the nurse will reduce the risk of infection?
- Washing the patient from
the shoulder down to the fingertips with smooth, short strokes
- Washing eyes from the outer canthus to the inner canthus
- Cleaning the least-soiled areas prior to cleaning the
most-soiled areas
- Massaging reddened areas of the patient's
skin
|
front 2 B - Moisture from excessive diaphoresis can cause skin breakdown.
The greatest risk to the patient is skin breakdown, which can result
from increased contact with the moist sheets causing skin irritation
and promoting bacteria growth. Therefore, the linens should be changed frequently. | back 2 A nurse is caring for a patient who is on long-term bedrest and
requires frequent linen changes due to excessive diaphoresis. Which of
the following is the priority rationale for frequent linen change?
- It provides an
opportunity to turn the patient from side to side to facilitate
clearing potential fluid from the lungs.
- Moisture from
excessive diaphoresis can cause skin breakdown.
- It provides
an opportunity to frequently evaluate the patient's skin on his back
side.
- Moisture on the sheets can cause discomfort to the
patient.
|
front 3 C - Ask the patient in what order she typically performs her morning routine.
The patient’s plan for routine morning care should be tailored to
the uniqueness of the patient’s typical routine. | back 3 When planning morning hygiene care for a postoperative patient, which
of the following actions should the nurse include?
- Inform the patient when
morning hygiene care is provided at the hospital.
- Schedule
to provide care to the patient and her roommate at the same
time.
- Ask the patient in what order she typically performs
her morning routine.
- Plan to provide care before the next
scheduled dose of pain medication.
|
front 4 - Gather all necessary supplies
- Place a rubber mat on
the tub floor
- Assist the patient into the bathroom
- Instruct the patient on using safety bars when getting in and
out of the tub
- Instruct the patient to remain in the tub
for no longer than 20 min.
When assisting the patient with a tub bath, the nurse should first
gather all necessary supplies and then prepare the room by placing a
rubber mat on the tub floor to prevent the patient from slipping and
falling. The nurse should assist the patient into the bathroom and
then give instructions regarding the use of bars to prevent slipping
and falling when entering or exiting the bathtub. Finally, the patient
should be instructed to remain in the tub for no longer than 20 min
due to the possibility of vasodilation from the warm water, which can
in turn cause light-headedness or dizziness. | back 4 A nurse is preparing to assist a patient with a tub bath. Identify
the sequence of steps the nurse should take?
(Move the steps into the box on the right, placing them in the
selected order of performance. All steps must be used.) |
front 5 D - The AP reuses the patient's blanket and spread.
The mattress pad, sheet, blanket, and spread may be reused for the
same patient if they are not wet or soiled. | back 5 A nurse observes an assistive personnel (AP) make a client's bed
while the client is out of the room. Which of the following actions by
the AP is appropriate for this task?
- The AP records the task
when it is completed.
- The AP makes a mitered corner with
the blanket and spread.
- The AP wears sterile gloves while
making the bed.
- The AP reuses the patient's blanket and
spread.
|
front 6 B - I'll swab the patient's mouth with chlorhexidine (Diluted
Hydrogen Peroxide)
Chlorhexidine is the correct solution to use for daily oral care for
the unconscious patient because evidence-based practice indicates it
improves patient outcomes by preventing microbial build-up. | back 6 A nurse is caring for an unconscious patient. Which of the following
statements by the nurse indicates an understanding of providing good
oral hygiene for the patient?
- I'll swab the patient's
lips with a very small amount of mineral oil.
- I'll swab the
patient's mouth with chlorhexidine.
- I'll swab the patient's
mouth with mouthwash.
- I'll swab the patient's mouth with
lemon-glycerin swabs.
|
front 7 C - raise the room temperature.
Raising the temperature of the room will help keep the patient warm
while various parts of the body are exposed and washed. | back 7 While performing a complete bed bath for a patient, the nurse should
- add soap to the water in
the basin before beginning the bath.
- completely remove the
linens.
- raise the room temperature.
- complete the
bathing for one side of the body at a time.
|
front 8 C - Oral care is still important even though you are not eating.
Bacteria are still present in the oral cavity regardless of NPO
status. It is important to perform oral care to help reduce oral
bacteria and keep the oral cavity moist. | back 8 A nurse is caring for an adult patient who is NPO. The patient is
refusing oral care. Which of the following is an appropriate response
by the nurse?
- Since you are not
eating, we can wait and do it before bedtime.
- We will wait
until your family gets here to help.
- Oral care is still
important even though you are not eating.
- I'll give you a
sip of water to swish around in your mouth, and then you can spit it
out.
|
front 9 activities of daily living (ADLs) | back 9 tasks performed routinely during the course of a typical day, such as
walking, eating, bathing, brushing the teeth, and grooming |
| back 10 adjustment to changes in circumstances such as those resulting from
illness or disability |
| |
| back 12 a chronic superficial fungal infection of the skin of the feet,
typically between the toes |
| back 13 pertaining to or directed toward the bucca (cheek), the fleshy
portion of the side of the face that makes up the lateral wall of the
oral cavity |
| back 14 a thickening of or a hard thickened area on skin |
| back 15 the angular junction of the eyelids at either corner of the eye |
| back 16 manifestation of vitamin B complex deficiency characterized by
reddened lips with fissures at the angles of the mouth |
| back 17 a bed prepared in a hospital room with the top sheet, blanket, and
bedspread drawn up to the head of the mattress under the pillows |
| back 18 often painful and inflamed circumscribed lesion of thickened skin,
usually on the toes and caused by pressure or friction from
ill-fitting shoes |
| back 19 the narrow band of epidermis extending from the nail wall onto the
nail surface |
| |
| back 21 a sticky film accumulating on the teeth that is formed by and harbors
bacteria; also called tartar |
| back 22 linen item placed under the patient's torso and used to lift and
reposition the patient |
| back 23 skin abrasion typically resulting from scratching |
| back 24 to expel fluid or secretions from the mouth, throat, or lungs by
coughing and/or spitting |
| back 25 applying the proximal half of a piece of linen in successive layers
lengthwise for the purpose of tucking it under the patient and rolling
the patient over it while stripping or making an occupied bed |
| back 26 a break, slit, or tear in soft tissue, often at the junction of skin
and mucous membrane |
| back 27 fold of skin covering the glans penis (head) of an uncircumcised
penis; also called prepuce |
| back 28 the part of the oral mucosa covering the tooth-bearing border of the
jaw; also called gums (plural: gingivae) |
| back 29 inflammation of the gums characterized by redness, swelling, and
intermittent bleeding |
| |
| back 31 personal maintenance of cleanliness |
| back 32 unlikely to cause an allergic (hypersensitivity) response |
| back 33 involuntary release of urine from the bladder or feces via the anus |
| back 34 painful condition in which the corner or side of a toenail grows into
the soft flesh of that toe |
| back 35 folds of skin on either side of the vaginal orifice |
| back 36 active area of nailbed growth at the base of the fingernails and toenails |
| back 37 softening or dissolution of tissue after lengthy exposure to fluid |
| back 38 the moist inner lining of various tubular structures, including the
mouth, esophagus, stomach, and intestines |
| back 39 any of numerous disturbances or pathologic changes in the peripheral
nervous system, most often affecting sensation |
| back 40 nothing by mouth, derived from the Latin words nil per os |
| back 41 a bed prepared in a hospital room with the top covers folded back to
make it easy for the patient to get into the bed |
| back 42 the roof of the mouth separating the mouth from the nasal cavity,
comprised of the hard palate (in the front of the mouth, separating
cavities of the mouth and the nose) and the soft palate (the fleshy
portion that separates the mouth from the pharynx) |
| |
| back 44 area between the anus and the posterior portion of the external genitalia |
| back 45 surrounding or near a tooth |
| back 46 inflammation or degeneration of the tissues surrounding the teeth |
| back 47 a skin lesion on the sole of the foot typically caused by any of the
human papillomaviruses |
| back 48 oil-secreting organ of the skin |
| back 49 fatty lubricant secreted by the skin's sebaceous glands |
| back 50 position with the head of the bed raised approximately 30 degrees |
| back 51 thick, cheesy secretion that accumulates under the labia minora or
the male foreskin |
| back 52 any inflammatory disorder of the mouth |
| back 53 a sticky film accumulating on the teeth that is formed by and harbors
bacteria; also called dental plaque |
| back 54 a fungal infection in the mouth and/or throat caused by Candida
albicans and manifesting as white patches and ulcers |
| back 55 a narrow tube through which urine passes from the bladder to the
outside of the body |
front 56 - remove sweat, oil, and micro-organism
- stimulates
circulation
- promotes a feeling of self-worth by improving the
patient's appearance
- time for socialization for patient who
are on bedrest
- opportune time for the nurse and
patient
- be able to perform a head-to-toe skin
assessment:
palpation
skin's color
trexture
temperature | |
front 57 - bed bath
- partial bed bath
- therapeutic
bath
- shower
- tub bath.
For patients in critical and long-term care settings who are unable
to bathe themselves, you’ll provide a complete bed bath using either a
commercial bag bath or cleansing pack. | back 57 Types of baths (bathing) techniques |
front 58 - bathing only those parts of the body that cause discomfort if
not bathed. These include the hands, face, axillae, back, and
perineal area. Patients who are dependent and require only a partial
bed bath or self-sufficient patients who must remain in bed but
cannot reach all body parts often receive a partial bed bath.
| |
front 59 - part of the treatment plan for such conditions as skin
disorders, burns, elevated body temperature, and muscular injuries.
Oatmeal, cornstarch, and commercial bath products are sometimes
added to the bath water to relieve skin irritation. For patients who
have had rectal or perineal surgery, a sitz bath is often prescribed
to reduce pain and inflammation. To add this type of bath to a
patient’s plan of care, you must obtain an order from the patient’s
provider.
| |
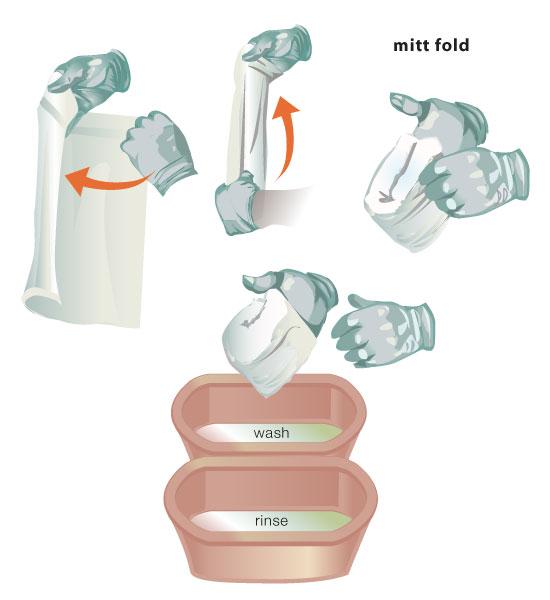
front 60 - When performing a bed bath with soap, water, and a washcloth,
fold the washcloth into a mitt over your hand to keep water from
splashing or dripping onto the bed or the patient. It also helps
keep the edges of the washcloth from brushing against the
patient.
- To fold the washcloth into a mitt, wrap one edge of
the cloth around your palm and fingers. Wrap the other edge of the
washcloth around your hand and hold it in place with your thumb.
Finally, tuck the top edge of the washcloth under the edge that is
in the palm of your hand.
| |
front 61 - You’ll change bed linens after the patient’s bath or while the
patient is in the shower, sitting in a chair, or out of the room for
a test or a procedure. You’ll also straighten the bed linens
throughout the day to remove any wrinkles and, of course, you’ll
change them if you find them wet or soiled. Encourage patients on
bed rest to participate as much as possible, as this can help
maintain their strength, mobility, and a certain amount of
independence with activities of daily living.
- It is ideal
to change the bed linens when the patient is out of the bed.
However, if the patient is too weak to get out of bed or restricted
to bed rest, you’ll have to change the linens while the patient is
in bed. Because this can be tiring for the patient, be sure you are
organized before beginning the process. If the patient is
experiencing any pain, administer a prescribed PRN analgesic about
30 to 60 minutes beforehand to help control the pain and make the
patient as comfortable as possible while you change the linens.
- When changing the linens on the patient’s bed, you might not
have to change all the linens each day. Typically, you’ll change the
bottom sheet, top sheet, and the pillowcase. However, you can leave
the same mattress pad, blanket, and bedspread in place if they are
not wet or soiled.
- Follow standard precautions by wearing
gloves if the linens are soiled and by keeping the linens away from
your scrubs when throwing them in the linen hamper. Also, avoid
shaking the linens since this can spread micro-organisms in the air.
If at anytime during the linen change the clean linens touch the
floor, place them in the linen hamper and use clean ones
instead.
- Observing good body mechanics and patient safety is
also important when changing the linens on the patient’s bed. Be
sure the bed is at a comfortable working height so that you don’t
have to bend or stretch over the mattress to remove the dirty linens
or to put clean ones on the bed. Also, make sure the side rails are
up when changing an occupied bed to keep the patient from rolling
out of bed and to give the patient something to hold onto while
moving from side to side.
- Before beginning the process of
changing the patient’s bed linens, be sure that you have all of the
necessary supplies. Try to plan ahead and bring only the linens you
will actually use. You cannot place any extra linens you bring into
the patient’s room back on the linen cart until after they have been
laundered.
| |
| |
front 63 In addition to an open or closed bed, you’ll prepare unoccupied beds
for patients who will be brought to your unit after surgery. With this
type of bed, you won’t tuck in or mitre the corners. Instead, you’ll
fold them to the bottom third of the bed to make transferring the
patient from the stretcher to the bed easier.
After you have replaced the bed linens, lower the bed to its
original position and make sure the wheels are locked to keep the
patient from falling when getting in and out of bed. In addition,
place the call light, bed controls, patient-controlled analgesia
button, and any other devices the patient needs within the patient’s reach. | |
front 64 - Encourage patients who wear dentures to care for them in the
same manner as they would care for their natural teeth. Keeping
dentures clean can help prevent the gums from becoming irritated and
infected. To keep bacteria from building up underneath the dentures
and to give the gums a rest, dentures should be removed at
night.
- Before removing a patient’s dentures, be sure to break
the seal on the upper denture by gently moving the denture up and
down or by placing your finger on the edge of the denture and
pulling down. Remove the upper denture by grasping the plate between
thumb and index finger wrapped in gauze and pull downward. To remove
lower denture, gently lift it from the jaw and rotate one side
downward. Place dentures in emesis basin or sink.
- For
patients who are unable to care for their own dentures, it is your
responsibility to provide this care for them. Because dentures are
the patient’s personal property and are costly to replace if broken
or damaged, handle them with care when cleaning them. When preparing
to clean dentures over a sink, place a towel or a washcloth in the
bottom of the sink to avoid breakage if you drop them.
- When
rinsing the patient’s dentures, be sure to use cool or tepid water.
Avoid hot water because heat can soften the material that some
dentures are made of, resulting in damage to the dentures.
- If dentures are stained, soak them in a commercial cleaner
following the manufacturer’s directions. If the dentures have any
metal pieces, avoid soaking them overnight as this can cause
corrosion. Be sure to rinse them well before putting them back in
the patient’s mouth.
- When the patient is not wearing the
dentures, store them in a small amount of water in a denture cup or
in a container with a lid. Label the cup with the patient’s name and
room number and store it in a safe place to prevent loss. Discourage
the patient from placing dentures in a napkin or a facial tissue
because they can be easily mistaken as garbage and discarded.
- Because dentures improve the patient’s speech, appearance, and
self-image, it’s important to put back them back in as soon as
possible after oral hygiene or after the patient returns from a
procedure. If the dentures are dry, moisten them with water before
putting them back in the patient’s mouth. After cleaning, ask if the
patient needs help inserting the dentures. Moisten the upper denture
and press firmly to seal it in place. Insert the moistened lower
denture.
| |
front 65 - Caring for the hair and scalp is important for the patient’s
appearance and sense of well-being and is an essential component of
personal hygiene. Hair care needs vary from patient to patient
depending on health status and cultural
preferences.
- Brush or comb the hair daily to
remove tangles, massage the scalp, stimulate circulation to the
scalp, and distribute natural oils along the shaft of the hair. Use
a soft-bristled brush to prevent injury or trauma to the scalp and a
wide-toothed comb or hair pick to comb through tightly curled or
kinky hair.
- Begin combing the hair by dividing it into
three or four sections. Then, brush or comb each section one at a
time starting at the scalp and moving to the ends of the hair to
minimize pulling. For tangled hair, use a wide-toothed comb and comb
the tangles out from the ends of the hair toward the scalp.
- Shampooing cleans the hair and scalp and can also relax the
patient. Start shampooing at the hairline and work toward the neck.
To wash the hair on the back of the patient’s head, gently lift the
head with one hand and shampoo with the other. Before rinsing,
massage the patient’s scalp by applying light pressure with your
fingertips.
- Depending on the patient’s health status, you can
shampoo the hair in any of a variety of ways. If the patient is
ambulatory, use the shower. If the patient is able to sit in a chair
and lean back, shampoo the hair at the sink. For patients on bed
rest, use a plastic shampoo trough. Dry or no-rinse shampoos and
shampoo caps are also options for patients on bed rest.
- Place a folded or rolled towel behind the patient’s neck to pad
the edge of the sink. Before beginning, make sure there are no
contraindications to having the patient’s head and neck manipulated
or extended back over the sink.
- When using a plastic
shampoo trough for a patient on bed rest, place a small basin at the
side of the bed to catch the water that drains from the trough. To
keep the bed linens and the patient’s gown dry, place a waterproof
pad underneath the trough and a towel around the patient’s
shoulders. Also, place a washcloth over the patient’s eyes to
protect them from the water and the shampoo.
- Another option
for shampooing the hair of patients on bed rest is to use a dry
shampoo, a no-rinse shampoo, or a shampoo cap. These shampoos are
activated by heat and must be warmed in a microwave oven before you
massage them into the patient’s hair and scalp. Although these
shampoos are convenient and require minimal movement of the patient,
they can make the hair and scalp dry.
| |
front 66 - Nail, hand, and foot care is performed on a regular basis to
assess for lesions, dryness, and signs of infection. This is
especially essential for patients who have peripheral vascular
disease or diabetes mellitus and for patients with immunosuppression
or who are otherwise at higher risk for developing foot and nail
problems.
- You’ll perform nail, hand, and foot care during
bathing. Soak the patient’s hands and feet in a basin of water for a
short period of time while performing other hygiene procedures and
then wash the hands and feet with soap and water. When drying the
hands and feet, be sure to dry between each finger and each
toe.
- If you trim the patient’s fingernails or toenails, cut
them straight across to prevent injury or trauma to the surrounding
tissue. Before cutting any patient’s nails, check your facility’s
policy, as some settings and patient conditions require provider
orders for foot care. In some cases, a podiatrist is required for
toenail care.
- Be sure to clean underneath the patient’s
nails using an orangewood stick or the end of a plastic applicator
stick to remove debris that can harbor micro-organisms. Shape the
nails and smooth rough edges using a nail file. Apply lotion to the
patient’s hands and feet, focusing on dry or callused areas. If the
patient’s hands or feet are extremely dry and the skin is cracked,
use a deep-penetrating moisturizer.
- Your foot and nail care
will vary from the standard when you care for a patient who has
diabetes mellitus. Do not soak the feet due to the risk of infection
and do not cut the nails. Instead, file them using a nail file. Do
not apply lotion between the fingers or toes since the moisture can
cause skin irritation and breakdown.
| back 66 Nail, hand, and foot care |
front 67 - Maintaining oral hygiene is important for preventing the
development of plaque-related disorders. Regular oral hygiene
includes brushing, flossing, and rinsing. Brushing cleans teeth of
food particles, plaque and bacteria. It also massages gums and
eliminates discomfort of unpleasant odors and tastes. Flossing
removes tartar that collects at the gumline. Rinsing removes
dislodged food particles and excess toothpaste.
- Inadequate
oral care diminishes salivary production, which reduces the ability
to fight effects of pathogens. Oral hygiene includes different
components depending on the patient, the patient’s health status,
and whether the patient has dentures or his natural teeth or both.
When to offer oral care might vary with the facility, but the most
common times are before breakfast, after each meal, and at bedtime.
The frequency of care is also based on condition of oral cavity and
patient’s level of comfort. Most often, though, oral hygiene
includes brushing the teeth several times a day, flossing at least
once a day, and rinsing with an antiseptic mouthwash once or twice a
day. American Dental Association guidelines include brushing teeth
at least twice a day with approved fluoride toothpaste and
antimicrobial mouth rinse.
- A well-balanced diet is very
important for developing healthy oral tissues. Patients may need to
change their dietary habits. Regularly scheduled visits to the
dentist for dental check-ups is advised for clients of all ages.
Educating clients about common gum and tooth disorders and methods
of prevention motivates them to follow good oral hygiene practices.
Poor oral health is linked to risk of impaired nutrition, stroke,
poor blood sugar control in diabetes, and nursing home-acquired
pneumonia.
- When oral hygiene is not performed correctly or
often enough, oral health problems can develop. The most common of
these are plaque and tartar build-up, tooth decay, gingivitis, and
periodontitis. Plaque is a soft, sticky, colorless substance that
forms on the hard, rough surfaces of the teeth. If plaque is not
removed and accumulates on the teeth, the gums can become irritated,
the outer enamel of the teeth can be destroyed, and halitosis can
develop.
- Another common dental problem resulting from the
accumulation of plaque on the patient’s teeth is tooth decay, also
known as dental caries or cavities. It is caused by the acid in the
plaque’s bacteria destroying the outer surfaces of the tooth.
-
Gingivitis is the early stage of periodontal
disease. It involves inflammation of the gums and often times
bleeding when the patient brushes and flosses the teeth. With proper
oral hygiene, which includes both brushing and flossing, gingivitis
can usually be reversed.
- If gingivitis is left untreated,
periodontitis develops. This gum disease destroys the supporting
structures of the teeth, including bone, and is characterized by
red, swollen, bleeding gums.
| |
front 68 - Perineal care is a part of a complete bed bath. Patients who
are at risk for infection are most in need of perineal care. These
are usually uncircumcised male patients, those with indwelling
urinary catheters, or those recovering from rectal or genital
surgery or childbirth, or women who are having a menstrual period.
Patients need to be encouraged to perform their own care.
Embarrassment can be a major deterrent for the nurse for performing
perineal care. A gender-congruent nurse can perform this care
efficiently. It is important to maintain a professional,
straightforward attitude and to protect the patient’s privacy at all
times during this procedure.
- Because your hands will come
into contact with mucous membranes and possibly body fluids when you
provide perineal care, follow standard precautions at all times. Not
only does this protect you, but it also protects the patient.
- Perineal care is often included in bathing and involves cleaning
the perineum, the external genitalia, and the surrounding skin. For
patients who are recovering from rectal or genital surgery or from
childbirth or for those who have an indwelling catheter, you might
have to provide perineal care frequently to prevent skin breakdown,
infection, and odor. Inquire about complaints of burning during
urination or localized soreness, excoriation, or pain in the
perineum. The vaginal and perineal areas can be inspected at this
time, as well as noting any abnormal odors.
- Before
beginning perineal care, position the bed at a comfortable working
height. Position the patient with knees bent and legs slightly
apart, unless contraindicated. This position exposes the areas you
will clean and allows for more thorough bathing.
- While
providing personal hygiene, keep the patient covered as much as
possible to maintain privacy and comfort and to keep the patient
warm. Before beginning perineal care, drape the area with a bath
blanket or a towel. Your technique will vary depending on whether
the patient is male or female.
| |
front 69 - Shaving is often a component of personal hygiene care. For male
patients, shaving is done after the bath or after you’ve shampooed
the hair. Female patients need the hair on the legs and axillae
shaved during bathing. Depending on the patient’s hair growth and
personal preference, daily shaving might be required.
- For
patients taking anticoagulants or high doses of aspirin or for those
with low platelet counts or bleeding disorders, use an electric
razor. Before using it, though, make sure it is in good working
condition and will not harm the patient. Check your facility’s
policy about using the patient’s electric razor or a hospital-issued
electric razor. Check the razor for frayed cords or other electrical
hazards.
- When using a disposable razor, be sure the patient’s
skin is soft before beginning to shave it. To accomplish this, place
a warm washcloth over the patient’s face for a few seconds before
applying shaving cream. Softening the skin first helps prevent
pulling, scraping, or cutting the skin during shaving. When patients
are unable to shave themselves, the nurse will have to shave for
them.
- To avoid causing discomfort and to reduce the risk of
cutting the patient’s skin during shaving, pull the skin taut and
use long, firm strokes to shave the larger areas of the face and
short downward strokes to shave around the chin and lips. Shaving in
the direction of hair growth is also helpful. Clients with tightly
curled or kinky hair may experience ingrown hair, so they need to be
shaved close to the skin.
- If the patient has a beard or
mustache, he might need daily grooming. It is important to keep
these areas clean, since food particles and mucus can collect in the
hair. Comb and trim the patient’s beard and mustache as necessary.
However, it is inappropriate to shave a patient’s beard or mustache
off without the patient’s permission to do so
| |