Instructions for Side by Side Printing
- Print the notecards
- Fold each page in half along the solid vertical line
- Cut out the notecards by cutting along each horizontal dotted line
- Optional: Glue, tape or staple the ends of each notecard together
A&P 2 Chapters 18, 19, 20, 21
front 1 The body contains two kinds of glands, what are they? | back 1 Exocrine and Endocrine |
front 2 Secrete their products through ducts into body cavities or onto body surfaces. (sudoriferous, sebaceous, and digestive) | back 2 Exocrine glands |
front 3 Secrete their products (hormones) into the extracellular spaces around the secretary cells, rather than into ducts. The secretion then diffuses into capillaries and is carried away by the blood. | back 3 Endocrine glands |
front 4 The endocrine system consists of endocrine glands and several organs that contain endocrine tissue. True or False | back 4 True |
front 5 In contrast, the endocrine system releases its messenger molecules, called _________, into the bloodstream | back 5 Hormones |
front 6 The nervous system controls homeostasis through _________ conducted along axons of neurons. | back 6 Nerve impulses (action potentials) |
front 7 Is the following true? Certain parts of the nervous system stimulate or inhibit the release of hormones. Hormones, in turn, may not promote or inhibit the generation of nerve impulses. True or False | back 7 False |
front 8 The nervous system causes muscles to contract and glands to secrete; the endocrine system affects virtually all body tissues, what does this system affect?? | back 8 Altering metabolic activities, Regulating growth and development, and Guiding reproductive processes. |
front 9 Nerve impulses are generally much more what? | back 9 Rapid, but brief when compared to those of the endocrine system. |
front 10 Hormones regulate the what? | back 10 Internal environment, Metabolism, and Energy balance |
front 11 Hormones also helps regulate what? | back 11 Smooth and cardiac muscular contraction, glandular secretion, and certain immune responses. |
front 12 Hormones DO NOT play a role in the integration of growth and development, and in the maintenance of homeostasis despite emergency environmental disruptions, and contribute to the basic processes of reproduction. True or False | back 12 False |
front 13 Hormones only affect specific________ that have _________ to recognize a given hormone. | back 13 Target cells and Receptors |
front 14 Receptors, like other cellular proteins, are constantly synthesized and broken down. True or False | back 14 True |
front 15 When a hormone (or neurotransmitter) is present in excess, the number of receptors may decrease __________, thereby decreasing the responsiveness of target cells to the hormone. | back 15 (Down-regulation) |
front 16 When a hormone (or neurotransmitter) is deficient, the number of receptors may increase __________, making the target tissue more sensitive to the stimulating effect of the hormone. | back 16 (Up-regulation) |
front 17 Hormones that pass into the blood to act on distant target cells are called what? | back 17 Circulating hormones or endocrines |
front 18 Hormones that act on target cells close to their site of release are called what? | back 18 Local hormones (paracrines or autocrines). |
front 19 Chemically, hormones are classified as what? | back 19 Steroids, Biogenic amines, Proteins and Peptides, and Eicosanoids (including prostaglandins and leukotrienes). |
front 20 Water-soluble hormones circulate in free form in the blood; lipid-soluble steroid and thyroid hormones are carried attached to what? | back 20 Transport proteins |
front 21 The response to a hormone depends on what? | back 21 Both the hormone and the target cell; various target cells respond differently to the same hormone. |
front 22 Hormones bind to and activate their specific receptors in two quite different ways. True or False | back 22 True |
front 23 These 2 hormones affect cell function by binding to and activating an intracellular receptor (usually in the nucleus), consequently altering gene expression. What are they? | back 23 Steroid hormones and Thyroid hormones |
front 24 Altered by cell function by activating plasma membrane receptors, which initiate a cascade of events inside the cell. What is this called? | back 24 Water-soluble hormones |
front 25 After a water-soluble hormone is release from an endocrine gland, it circulates in the blood, reaches a target cell, and brings a specific message to that cell; since such a hormone can deliver its message only to the plasma membrane, it is called the what? | back 25 First messenger |
front 26 A _____________ is needed to relay the message inside the cell where hormone-stimulated responses can take place; the best known second messenger is cyclic AMP (cAMP) but other substances are known second messengers. | back 26 Second messenger |
front 27 What is the best known second messenger? | back 27 Cyclic AMP (cAMP) |
front 28 G-proteins are a common feature of most second messenger systems; the symptoms of cholera are a direct result of the cholera toxin on G-proteins in the intestinal lining. True or False | back 28 True |
front 29 Cyclic AMP does not directly produce a particular physiological response, but instead activates one or more enzymes known as what? | back 29 Protein kinases |
front 30 The responsiveness of a target cell to a hormone depends on the hormone’s concentration and the number of receptors. The manner in which hormones interact with other hormones is also important: three hormonal interactions are the? (Hint: Remember the 3 effects) | back 30 Permissive effect, Synergistic effect, and Antagonistic effect. |
front 31 Is the following true?
| back 31 Yes they are all true facts. |
front 32 What is the major integrating link between the nervous and endocrine systems? | back 32 Hypothalamus |
front 33 The hypothalamus and the pituitary gland (hypophysis) do not regulate virtually all aspects of growth, development, metabolism, and homeostasis. True or False | back 33 False |
front 34 Where is the pituitary gland is located??? | back 34 Sell turcica of the sphenoid bone |
front 35 Hormones of the adenohypophysis are controlled by releasing or inhibiting hormones produced by the what? | back 35 Hypothalamus |
front 36 The blood supply to the anterior pituitary is from the superior hypophyseal arteries. It carries releasing and inhibiting hormones to the anterior pituitary. True or False | back 36 True |
front 37 Histologically, the anterior pituitary consists of five principal types of glandular cells. What are they? Hint: Sarah loves to cry to guys. | back 37
|
front 38 Somatotrophs produce what hormone? | back 38 Human Grown Hormone (hGH) |
front 39 hGH is produced by who? | back 39 Somatotrophs |
front 40 Lactotrophs produce what hormone? | back 40 Prolactin (PRL) |
front 41 Prolactin is produced by who? | back 41 Lactotrophs |
front 42 Corticotrophs secrete what hormones? | back 42 Adrenocorticotropic hormone (ACTH) and Melanocyte-stimulating hormone (MSH) |
front 43 Adrenocorticotropic hormone (ACTH) and melanocyte-stimulating hormone (MSH) are secreted by who? | back 43 Corticotrophs |
front 44 Thyrotrophs secrete what hormone? | back 44 Thyroid-stimulating hormone (TSH). |
front 45 Thyroid-stimulating hormone (TSH) are secreted by who? | back 45 Thyrotrophs |
front 46 Gonadotrophs secrete what hormones? | back 46 Follicle-stimulating hormone (FSH) and Luteinizing hormone (LH) |
front 47 Follicle-stimulating hormone (FSH) and Luteinizing hormone (LH) are secreted by who? | back 47 Gonadotrophs |
front 48 Negative feedback systems will decrease the secretory activity of corticotrophs, thyrotrophs, and gonadotrophs if levels of their target gland hormones rise. True or False | back 48 True |
front 49 Human growth hormone (hGH, GH, or somatotropin) does what? | back 49 Stimulates body growth through somatomedins and is controlled by GHIH (growth hormone inhibiting hormone, or somatostatin) and GHRH (growth hormone releasing hormone, or somatocrinin). |
front 50 Disorders associated with improper levels of hGH are what? | back 50 Pituitary dwarfism, Giantism, and Acromegaly. |
front 51 Thyroid-stimulating hormone (TSH or thyrotropin) does what? | back 51 Regulates thyroid gland activities and is controlled by TRH (thyrotropin release hormone). |
front 52 Follicle-stimulating hormone (FSH) does what? | back 52 Regulates the activities of the ovaries and testes and is controlled by GnRH (gonadotropin releasing hormone). |
front 53 Luteinizing hormone (LH) does what? | back 53 Regulates the activities of the ovaries and testes and is controlled by GnRH. |
front 54 Prolactin (PRL or lactogenic hormone) does what? | back 54 Helps initiate milk secretion and is controlled by PIH (prolactin inhibiting hormone) and PRH (prolactin releasing hormone) from the hypothalamus. |
front 55 Melanocyte-stimulating hormone (MSH) does what? | back 55 Increases skin pigmentation and is controlled by MRH (melanocyte-releasing hormone) and MIH (melanocyte-inhibiting hormone). |
front 56 Adrenocorticotropic hormone (ACTH) does what? | back 56 Regulates the activities of the adrenal cortex and is controlled by CRH (corticotropin releasing hormone). |
front 57 hGH stands for? | back 57 Human Growth Hormone |
front 58 What does TSH stand for? | back 58 Thyroid-stimulating hormone |
front 59 What does FSH mean? | back 59 Follicle-stimulating hormone |
front 60 What does LH stand for? | back 60 Luteinizing hormone |
front 61 What does PRL stand for? | back 61 Prolactin |
front 62 What does MSH stand for? | back 62 Melanocyte-stimulating hormone |
front 63 What does ACTH stand for? | back 63 Adrenocorticotropic hormone |
front 64 Hormones made by the hypothalamus and stored in the posterior pituitary, what are they called? | back 64 Oxytocin (OT) and Antidiuretic hormone (ADH). |
front 65 OT stands for? | back 65 Oxytocin |
front 66 What does ADH stand for? | back 66 Antidiuretic hormone |
front 67 Stimulates contraction of the uterus and ejection (let-down) of milk from the breasts; during labor and delivery, OT is released in large quantities. | back 67 Oxytocin (OT) |
front 68 Stimulates water reabsorption by the kidneys and arteriolar constriction. | back 68 Antidiuretic hormone (ADH) |
front 69 OT secretion is not controlled by uterine distention and nursing. True or False | back 69 False |
front 70 Synthetic OT (Pitocin) is often given to induce labor or to increase uterine tone and control hemorrhage just after giving birth. True or False | back 70 True |
front 71 The effect of ADH is to decrease urine volume and conserve body water. True or False | back 71 True |
front 72 ADH is controlled primarily by osmotic pressure of the blood. True or False | back 72 True |
front 73 The thyroid gland is located just below the _________ and has right and left lateral lobes. | back 73 Larynx |
front 74 Histologically, the thyroid consists of thyroid follicles composed of follicular cells, which secrete the thyroid hormones called what? | back 74 thyroxine (T4) and triiodothyronine (T3) and calcitonin (CT) |
front 75 IMPORTANT: Thyroid hormones are synthesized from iodine and tyrosine within a large glycoprotein molecule called thyroglobulin (TGB) and are transported in the blood by plasma proteins, mostly thyroxine-binding globulin (TBG). IMPORTANT: | back 75 (Watch out for confusion here since the order of the letters in these acronyms is easily reversed). |
front 76 Thyroid hormones regulate the what? | back 76 Rate of metabolism, growth and development, and the reactivity of the nervous system. Secretion is controlled by the level of iodine in the thyroid gland and by negative feedback systems involving both the hypothalamus and the anterior pituitary. TRH (thyrotropin releasing hormone) and TSH (thyroid stimulating hormone) are responsible for initiating thyroid activity. |
front 77 Disorders associated with the thyroid gland are what? | back 77 Cretinism, myxedema, Graves’ disease, and goiter |
front 78 Calcitonin (CT) lowers the blood level of calcium. Secretion is controlled by calcium levels in the blood. True or False | back 78 True |
front 79 The parathyroid glands are embedded where? | back 79 Posterior surfaces of the lateral lobes of the thyroid. |
front 80 The parathyroids consist of what? | back 80 principal (chief) and oxyphil cells, which secrete parathyroid hormone (PTH), or parathormone. |
front 81 Parathyroid hormone (PTH), or parathormone, regulates what? | back 81 The homeostasis of calcium and phosphate by increasing blood calcium level and decreasing blood phosphate level. Secretion is controlled by calcium level in the blood. |
front 82 Disorders associated with parathyroid glands, what are they? | back 82 Tetany and Osteitis fibrosa cystica |
front 83 Tetany results from what? | back 83 From a deficiency of calcium caused by hypoparathyroidism. |
front 84 Osteitis fibrosa cystica is characterized by what? | back 84 Emineralized, weakened, and deformed bones, resulting from the condition of hyperparathyroidism. |
front 85 The adrenal glands are located where? | back 85 Superior to the kidneys; they consist of an outer cortex and inner medulla. |
front 86 Histologically, the cortex is divided into 3 zones what are they? | back 86 zona glomerulosa zona fasciculata zona reticularis |
front 87 Increase sodium and water reabsorption and decrease potassium reabsorption, helping to regulate sodium and potassium levels in the body. What is this called? | back 87 Mineralocorticoids (e.g., aldosterone) |
front 88 A dysfunction related to aldosterone hypersecretion is what? | back 88 Aldosteronism |
front 89 Secretion is not controlled by the renin-angiotension pathway and the blood level of potassium. True or False | back 89 False |
front 90 Promote normal organic metabolism, help resist stress, and serve as anti-inflammatory substances. What is this called? | back 90 Glucocorticoids (e.g., cortisol) |
front 91 Secretion is controlled by CRH (corticotropin releasing hormone) and ACTH (adrenocorticotropic hormone) from the anterior pituitary. True or False | back 91 True |
front 92 Disorders associated with glucocorticoid secretion are what? | back 92 Addison’s disease and Cushing’s syndrome |
front 93 Secreted by the adrenal cortex usually have minimal effects. What is this called? | back 93 Gonadocorticoids (sex hormones) (e.g., estrogens and androgens) |
front 94 Excessive production occurs in congenital adrenal hyperplasia (CAH), resulting in virilism (masculinization). True or False | back 94 True |
front 95 Virilism or gynecomastia (excessive growth of male mammary glands) may also result from tumors of the adrenal gland. True or False | back 95 True |
front 96
| back 96 Chromaffin cells |
front 97 Medullary secretions are epinephrine and norepinephrine (NE), which produce effects similar to ___________. They are released under stress by direct innervation from the autonomic nervous system. Like the glucocorticoids of the adrenal cortex, these hormones help the body resist stress. However, unlike the cortical hormones, the medullary hormones are not essential for life. | back 97 Sympathetic responses |
front 98 Tumors of the chromaffin cells, called _______. These cause hypersecretion of epinephrine and norepinephrine. Since these hormones create the same effect as sympathetic nervous stimulation, hypersecretion puts the individual into a prolonged state of fight-or-flight response, ultimately causing generalized fatigue and weakness. | back 98 Pheochromocytomas |
front 99 The pancreas is a flattened organ located where? | back 99 Posterior and slightly inferior to the stomach and can be classified as both an endocrine and an exocrine gland. |
front 100 What organ can be classified as both as a endocrine and an exocrine gland? | back 100 Pancreas |
front 101 Histologically, the pancreas consists of pancreatic islets or islets of Langerhans and clusters of cells (acini) (enzyme-producing exocrine cells). Four types of hormone-secreting cells compose the pancreatic islets. True or False | back 101 True |
front 102 Secrete the hormone glucagon | back 102 Alpha cells |
front 103 Alpha cells secrete what hormone? | back 103 Glucagon |
front 104 Alpha cells secretion is stimulated by what? | back 104 Low blood glucose level. |
front 105 Glucagon increases blood glucose levels. True or False | back 105 True |
front 106 Beta cells secrete what hormone? | back 106 Insulin |
front 107 Insulin is secreted from where? | back 107 Beta Cells |
front 108 Insulin decreases blood glucose levels. True or False | back 108 True |
front 109 Insulin secretion is stimulated by what? | back 109 High blood glucose levels |
front 110 Disorders associated with insulin production are what? | back 110 diabetes mellitus and hyperinsulinism |
front 111 These are located in the pelvic cavity and produce sex hormones (estrogens and progesterone) related to development and maintenance of female sexual characteristics, reproductive cycle, pregnancy, lactation, and normal reproductive functions. These also produce inhibin and relaxin. | back 111 Ovaries |
front 112 Ovaries produce what hormone? | back 112 Estrogen Progesterone Inhibin Relaxin |
front 113 Lies inside the scrotum and produce sex hormones (primarily testosterone) related to the development and maintenance of male sexual characteristics and normal reproductive functions. The testes also produce inhibin. | back 113 Testes |
front 114 Testes produce what hormones? | back 114 Testosterone Inhibin |
front 115 Testes and ovaries both produce this hormone, what is it? | back 115 Inhibin |
front 116 Is attached to the roof of the third ventricle, inside the brain. What is it? | back 116 Pineal gland (epiphysis cerebri) |
front 117 Histologically, pineal gland consists of secretory parenchymal cells called parenchymal cells called pinealocytes, neuroglial cells, and scattered postganglionic sympathetic fibers. True or False | back 117 True |
front 118 The pineal secretes melatonin in a diurnal rhythm linked to the dark-light cycle. That helps you to fall asleep. True or False | back 118 True |
front 119 A type of depression that arises during the winter months when day length is short, is thought to be due, in part, to over-production of melatonin. Bright light therapy, repeated doses of several hours of exposure to artificial light as bright as sunlight, may provide relief for this disorder and for jet lag. | back 119 Seasonal affective disorder (SAD) |
front 120 Secretes several hormones related to immunity, this is called? | back 120 Thymus gland |
front 121 The thymus produces what hormones? | back 121 Thymosin, Thymic humoral factor (THF), Thymic factor (TF), Thymopoietin |
front 122 What do the hormones of the Thymus gland do??? | back 122 Promote the proliferation and maturation of T cells, a type of white blood cell involved in immunity. |
front 123 Prostaglandins (PGs) and leukotrienes (LTs) do not act as paracrines and autocrines in most body tissues by altering the production of second messengers, such as cyclic AMP. True or False | back 123 False |
front 124 Prostaglandins have a wide range of biological activity in normal physiology and pathology. True or False | back 124 True |
front 125 Aspirin and related nonsteroidal anti-inflammatory drugs (NSAIDS), such as ibuprofen and acetaminophen, inhibit a key enzyme in prostaglandin synthesis and are used to treat a wide variety of inflammatory disorders. True or False | back 125 True |
front 126 ___________ are hormones that stimulate cell growth and division. | back 126 Growth factors |
front 127 Examples include epidermal growth factor (EGF), platelet-derived growth factor (PDGF), fibroblast growth factor (FGF), nerve growth factor (NGF), tumor angiogenesis factors (TAFs), insulin-like growth factor (IGF), and cytokines. True or False | back 127 True |
front 128 ____________ is initiated by nerve impulses from the hypothalamus to the sympathetic division of the autonomic nervous system and adrenal medulla. Responses are the immediate and brief fight-or-flight reactions that increase circulation promote catabolism for energy production, and decrease nonessential activities. | back 128 Alarm reaction |
front 129 ____________ is initiated by regulating hormones secreted by the hypothalamus. The regulating hormones are CRH (corticotrophin releasing hormone), GHRH (growth hormone releasing hormone), and TRH (thyrotropin releasing hormone). CRH stimulates the adenohypophysis (anterior pituitary) to increase its secretion of ACTH (adrenocorticotropic hormone), which in turn stimulates the adrenal cortex to secrete hormones. Resistance reactions are long-term and accelerate catabolism to provide energy to counteract stress. Glucocorticoids are produced in high concentrations during stress. They create many distinct physiological effects. | back 129 Resistance reaction |
front 130 ____________ results from dramatic changes during alarm and resistance reactions. Exhaustion is caused mainly by loss of potassium, depletion of adrenal glucocorticoids, and weakened organs. If stress is too great, it may lead to death. | back 130 Stage of exhaustion |
front 131
True or False End of chapter 18 | back 131 True |
front 132 Blood inside blood vessels, interstitial fluid around body cells, and lymph inside lymph vessels constitute one’s what? | back 132 Internal environment. |
front 133 The blood, heart, and blood vessels together make up the cardiovascular system. True or False | back 133 True |
front 134 The lymph, lymphatic vessels that transport lymph, and structures and organs containing lymphatic tissue (large clusters of white blood cells called lymphocytes) make up the what??? | back 134 Lymphatic system. |
front 135 The branch of science concerned with the study of blood, blood-forming tissues, and the disorders associated with them is called? | back 135 Hematology. |
front 136 FUNCTIONS OF THE BLOOD ARE WHAT? | back 136
|
front 137 Physical characteristics of blood include a viscosity greater than that of water; temperature, 38°C (100.4°F); and a pH of 7.35 to 7.45. True or False | back 137 True |
front 138 The pH of blood is what? | back 138 7.35 to 7.45 |
front 139 Blood constitutes about ________ of body weight; volume ranges from 4 to 6 liters. | back 139 8% |
front 140 Blood samples for laboratory testing may be obtained by? | back 140 Venipuncture, Finger-stick, or A rterial stick. |
front 141 Blood consists of 55% plasma and 45% formed elements. | back 141 Blood consists of 55% plasma and 45% formed elements. |
front 142 Plasma consists of 91.5% and 8.5% solutes. | back 142 Plasma consists of 91.5% and 8.5% solutes. |
front 143 Principal solutes include proteins (albumins, globulins, fibrinogen), nutrients, enzymes, hormones, respiratory gases, electrolytes, and waste products. True or False | back 143 True |
front 144
| back 144 Formed elements |
front 145 Formed elements come from where? | back 145 Erythrocytes (red blood cells) Leukocytes (white blood cells) Thrombocytes (platelets). |
front 146 Blood cells are formed from pluripotent hematopoietic stem cells called? | back 146 Hemocytoblasts |
front 147 Hemopoiesis (or hematopoiesis) is stimulated by several hematopoietic growth factors. These hematopoietic growth factors stimulate differentiation and proliferation of the various blood cells. True or False | back 147 True |
front 148 Red bone marrow (myeloid tissue) is responsible for producing red blood cells, granular leukocytes, and platelets; lymphoid tissue and myeloid tissue produce agranular leukocytes. True or False | back 148 True |
front 149 Are biconcave discs without nuclei that contain what? | back 149 Hemoglobin |
front 150 Erythrocytes are known as? | back 150 Red blood cells or RBC"s |
front 151 Hemoglobin molecules are specialized components of the red blood cell plasma membrane which combine with oxygen (as oxyhemoglobin) or with carbon dioxide (as carbaminohemoglobin) in this transport process. True or False | back 151 True |
front 152 A serious disorder called sickle-cell anemia (SCA) is due to what? | back 152 A genetic defect in the structure of hemoglobin in affected individuals. |
front 153 Has been used by some athletes in an attempt to boost the oxygen-carrying capacity of their blood before an athletic event. Although evidence suggests that there may be performance benefits related to the procedure, the potential risks from higher blood viscosity are unknown and the practice is considered dishonest by the International Olympics Committee. What is this called? | back 153 Induced erythrocytemia (blood doping) |
front 154 Red blood cells live for how long? | back 154 90-120 days |
front 155 A healthy male has how many red blood cells? | back 155 5.4 million RBCs/mm3 |
front 156 A healthy female has how many red blood cells? | back 156 4.8 million/mm3 |
front 157 After phagocytosis of worn-out RBCs by macrophages, hemoglobin is ________. The globin portion is split from the heme with the amino acids being reused for protein synthesis. The iron in the heme portion is reclaimed with the rest of the heme molecule; the rest becomes a component of bile in the digestive process. | back 157 Recycled |
front 158 Erythrocyte formation is called what? | back 158 Erythropoiesis |
front 159 Occurs in adult red bone marrow of certain bones. It is stimulated by hypoxia, which stimulates release of ____________ by the kidneys. | back 159 Erythropoietin . |
front 160 A reticulocyte count (average 0.5%-1.5% of all RBCs) is a diagnostic test that indicates the rate of erythropoiesis, useful in diagnosing and treating anemia. True or False | back 160 True |
front 161 Measures the percentage of red blood cells in whole blood. | back 161 Hematocrit (Hct) |
front 162 An average male has a hematocrit range of? | back 162 47% (range of 40-54%) |
front 163 Females have a hematocrit range of? | back 163 42% (range of 38-46%) |
front 164 Leukocytes (white blood cells, or WBCs) are nucleated cells and do not contain hemoglobin. True or False | back 164 True |
front 165 Are nucleated cells and do not contain hemoglobin, what is this called? | back 165 Leukocytes (white blood cells, or WBCs) |
front 166 Neutrophils, Eosinophils, Basophils are what? G ranular or Agranular | back 166 Granular |
front 167 Lymphocytes and Monocytes are what? G ranular or Agranular | back 167 Agranular |
front 168 Leukocytes have surface proteins, as do erythrocytes | back 168 Leukocytes have surface proteins, as do erythrocytes |
front 169 Are unique for each person (except for identical twins), and can be used to identify a tissue. What is this called? | back 169 Major histocompatibility antigens (MHC) |
front 170 Is performed to determine tissue compatibility between a donor and a recipient before any organ transplant. What is this called? | back 170 Tissue typing (histocompatibility testing) |
front 171 The general function of leukocytes is to what? | back 171 To combat inflammation and infection. |
front 172 ___________ and wandering or fixed macrophages (which develop from monocytes) do so through phagocytosis. | back 172 Neutrophils |
front 173 __________ combat the effects of histamine in allergic reactions, phagocytize antigen-antibody complexes, and combat parasitic worms. | back 173 Eosinophils |
front 174 ___________ develop into mast cells that liberate heparin, histamine, and serotonin in allergic reactions that intensify the inflammatory response. | back 174 Basophils |
front 175 ____________ in response to the presence of foreign substances called antigens, differentiate into tissue plasma cells that produce antibodies. -Antibodies attach to the antigens and render them harmless. -This antigen-antibody response combats infection and provides immunity. | back 175 B lymphocytes |
front 176 This destroys foreign invaders directly. | back 176 T lymphocytes |
front 177 Is a diagnostic test in which specific white blood cells are enumerated. Because each type of white cell plays a different role, determining the percentage of each type in the blood assists in diagnosing the condition. What is this called? | back 177 A differential white blood cell count |
front 178 White blood cells usually live for only a few hours or a few days. Normal blood contains 5,000-10,000 leukocytes/mm3. True or False | back 178 True |
front 179 May be used to treat several types of anemia, leukemia, and numerous other blood disorders. What is this called? | back 179 Bone marrow transplants |
front 180 Are disc-shaped structures without nuclei, what is this called?
| back 180 Thrombocytes, or Platelets |
front 181 Is used to determine blood cell counts, hemoglobin, hematocrit, white blood cell count, differential white blood cell count, and platelet count. What is this called? | back 181 Complete blood count (CBC) |
front 182 This refers to the stoppage of bleeding. When blood vessels are damaged or ruptured, the hemostatic response must be quick, localized to the region of damage, and carefully controlled. What is this called? | back 182 Hemostasis |
front 183 Hemostasis involves vascular spasm, platelet plug formation, and blood coagulation (clotting). True or False | back 183 True |
front 184 The smooth muscle of a blood vessel wall contracts to stop bleeding. What is this called? | back 184 Vascular spasm |
front 185 Involves the clumping of platelets around the damage to stop the bleeding. What is this called? | back 185 Platelet plug formation |
front 186
| back 186 Clot |
front 187 The formation of prothrombinase is initiated by the interplay of two mechanisms called the extrinsic and intrinsic pathways of blood clotting. True or False | back 187 True |
front 188 Refers to several different hereditary deficiencies of coagulation in which bleeding may occur spontaneously or after only minor trauma. What is this called? | back 188 Hemophilia |
front 189 The formation of prothrombinase is initiated by the interplay of two mechanisms called? | back 189 Extrinsic Intrinsic |
front 190 Normal coagulation requires vitamin K and also involves? | back 190 Clot retraction (or syneresis, tightening of the clot) and fibrinolysis (dissolution of the clot). |
front 191 Tightening of the clot this called? | back 191 Syneresis |
front 192 Dissolution of the clot is called? | back 192 Fibrinolysis |
front 193 _____________ are chemical substances injected into the body that dissolve blood clots to restore circulation; the most common use is in treatment of clots in coronary arteries of the heart (streptokinase and tissue plasminogen activator, or t-PA). | back 193 Thrombolytic (clot-dissolving) agents |
front 194
| back 194 Anticoagulants |
front 195 Despite the anticoagulating and fibrinolytic mechanisms, blood clots sometimes form within the cardiovascular system. True or False | back 195 True |
front 196 Clotting in an unbroken blood vessel is called what? | back 196 Thrombosis |
front 197 A __________ bubble of air, fat from broken bones, or piece of debris transported by the bloodstream that moves from its site of origin is called an embolus. | back 197 Thrombus (clot) |
front 198 The surfaces of red blood cells contain genetically determined blood group antigens, called agglutinogens or isoantigens, and the plasma of many persons contains genetically determined antibodies, called agglutinins or isoantibodies, against the blood group antigens which they do not have. True or False | back 198 True |
front 199 agglutinogens isoantigens agglutinins isoantibodies All of these are simply known as what? | back 199 Antigens |
front 200 The ABO and Rh blood grouping systems are based on antigen-antibody responses. True or False | back 200 True |
front 201 Individuals whose erythrocytes have Rh agglutinogens are classified as Rh+ and those who lack the antigen are Rh-. True or False | back 201 True |
front 202 A disorder due to Rh incompatibility between mother and fetus is called what? Also This disease is treatable, but also preventable | back 202 Hemolytic disease of the newborn (HDN), or erythroblastosis fetalis |
front 203 Is a condition in which the oxygen-carrying capacity of the blood is reduced; it is a sign, not a diagnosis and is usually characterized by a decreased erythrocyte count or hemoglobin deficiency. What is this called? | back 203 Anemia |
front 204 Kinds of anemia include are what? | back 204 Nutritional, pernicious, hemorrhagic, hemolytic, aplastic, sickle-cell (SCA). |
front 205 Is an abnormal increase in the number of erythrocytes (Hct > 55%). Increased viscosity of the blood causes a rise in blood pressure and contributes to thrombosis and hemorrhage. What is this called? | back 205 Polycythemia |
front 206 Is a contagious disease that primarily affects lymphoid tissue. It is characterized by an elevated white blood cell count, with an abnormally high percentage of lymphocytes. The cause is the Epstein-Barr virus (EBV). What is this called? | back 206 Infectious mononucleosis (IM) |
front 207 ___________ is a malignant disease of blood-forming tissue characterized by the uncontrolled production of white blood cells that interferes with normal clotting and vital body activities. It is classified based on the duration and character of the disease and also according to the identity and site of origins of the predominant cell involved (myelocytic, lymphocytic, or monocytic). | back 207 Leukemia |
front 208 Is characterized by uncontrolled production and accumulation of immature leukocytes. What is this called? | back 208 Acute leukemia |
front 209 In ________, there is an accumulation of mature leukocytes in the bloodstream because they do not die at the end of their normal life span. | back 209 Chronic leukemia |
front 210 End of Chapter 19 | back 210 End of Chapter 19 |
front 211 What organ is the center of the cardiovascular system? | back 211 Heart |
front 212 LOCATION AND SIZE OF THE HEART | back 212
|
front 213 The heart is enclosed by and held in place by? | back 213 Pericardium |
front 214 The pericardium consists of an outer ______________ and an inner ___________. | back 214 fibrous pericardium (out) and serous pericardium (inner) |
front 215 The serous pericardium is not composed of a parietal layer and a visceral layer. True or False | back 215 False |
front 216 Between the parietal and visceral layers of the serous pericardium is the ___________, a potential space filled with pericardial fluid that reduces friction between the two membranes. | back 216 Pericardial cavity |
front 217 Pericardial fluid does what? | back 217 Reduces friction between membranes |
front 218 An inflammation of the pericardium is known as what? | back 218 Pericarditis |
front 219 Associated bleeding into the pericardial cavity compresses the heart (cardiac tamponade) and is potentially lethal. True or False | back 219 True |
front 220 The wall of the heart has three layers: what are they? Hint: Think "eat my egg" | back 220 Epicardium Myocardium Endocardium |
front 221 The epicardium consists of? | back 221 Mesothelium and Connective tissue |
front 222 The myocardium is composed of? | back 222 Cardiac muscle tissue |
front 223 The endocardium consists of? | back 223 Endothelium and Connective tissue. |
front 224 The chambers of the heart include? | back 224 Two upper atria and two lower ventricles. |
front 225 What separates the atria?? | back 225 Interatrial septum |
front 226 What separates the ventricles? | back 226 Interventricular septum |
front 227 What does septum mean? | back 227 A wall |
front 228  Blood flows through the heart from the superior and inferior venae cavae and the coronary sinus to the right atrium, through the tricuspid valve to the right ventricle, through the pulmonary trunk and pulmonary arteries to the lungs, through the pulmonary veins into the left atrium, through the bicuspid valve to the left ventricle, and out through the aorta. | back 228  Blood flows through the heart from the superior and inferior venae cavae and the coronary sinus to the right atrium, through the tricuspid valve to the right ventricle, through the pulmonary trunk and pulmonary arteries to the lungs, through the pulmonary veins into the left atrium, through the bicuspid valve to the left ventricle, and out through the aorta. |
front 229 Divisions of the aorta are the? | back 229 1. Ascending aorta 2. Arch of the aorta 3. Thoracic aorta 4. Abdominal aorta. |
front 230 These are composed of dense connective tissue covered by endothelium, prevent backflow of blood in the heart. What are they? | back 230 Valves |
front 231  Atrioventricular (AV) valves, between the atria and their ventricles, are the tricuspid valve on the right side of the heart and the bicuspid (mitral) valve on the left. True or False | back 231  True |
front 232  The chordinae tendineae and their papillary muscles keep the flaps of the valves pointing in the direction of the blood flow and stop blood from backing into the atria. True or False | back 232  True |
front 233  ____________ prevent blood from flowing back into the heart as it leaves the heart for the lungs (pulmonary semilunar valve) or for the rest of the body (aortic semilunar valve). | back 233  Semilunar valves |
front 234 ____________ is precipitated by infection with group A, β-hemolytic strains of Streptococcus pyogenes The ultimate result is damage to valves of the heart, most commonly the bicuspid and aortic semilunar valves. | back 234 Rheumatic fever |
front 235 The flow of blood through the many vessels that pierce the myocardium of the heart is called the _________ ; it delivers oxygenated blood and nutrients to the myocardium and removes carbon dioxide and wastes from it. | back 235 Coronary (cardiac) circulation |
front 236 The principle arteries, branching from the ascending aorta and carrying oxygenated blood, are the right and left coronary arteries; deoxygenated blood returns to the right atrium primarily via the principal vein, the __________. . | back 236 Coronary sinus. |
front 237 Most heart problems results from faulty coronary circulation due to blood clots, fatty atherosclerotic plaques, or spasm of the smooth muscle in coronary artery walls. Complications of this system include angina pectoris (severe pain that accompanies reduced blood flow, or ischemia, to the myocardium) and myocardial infarction (MI, or heart attack, in which there is death of an area of the myocardium due to an interruption of the blood supply; it may result from a thrombus or embolus). True or False | back 237 True |
front 238 Whenever a disease or injury deprives a tissue of oxygen, reestablishing the blood flow (reperfusion) may damage the tissue further due to the formation of oxygen free radicals; these can destabilize the molecular structure of proteins, neurotransmitters, nucleic acids, and phospholipids of plasma membranes. True or False | back 238 True |
front 239 An ___________ may be used to restore cardiac rhythm due to disruption of some component of the conduction system. | back 239 Artificial pacemaker |
front 240 A recording of the electrical changes that accompany each cardiac cycle (heartbeat) is called an? | back 240 Electrocardiogram (ECG or EKG) |
front 241 Who developed the electrocardiogram? And when? | back 241 Mtoren in 1830 |
front 242 A normal ECG consists of a P wave (atrial depolarization – spread of impulse from SA node over atria), QRS complex (ventricular depolarization – spread of impulse through ventricles), and T wave (ventricular repolarization). True or False | back 242 True |
front 243 A normal ECG consists of a? | back 243 P wave (atrial depolarization – spread of impulse from SA node over atria), QRS complex (ventricular depolarization – spread of impulse through ventricles), and T wave (ventricular repolarization) |
front 244 The __________ represents the conduction time from the beginning of atrial excitation to the beginning of ventricular excitation. Full ventricular depolarization/plateau of the ventricles | back 244 P-Q (PR) interval |
front 245 The _________ represents the time when ventricular contractile fibers are fully depolarized, during the plateau phase of the impulse. | back 245 S-T segment |
front 246 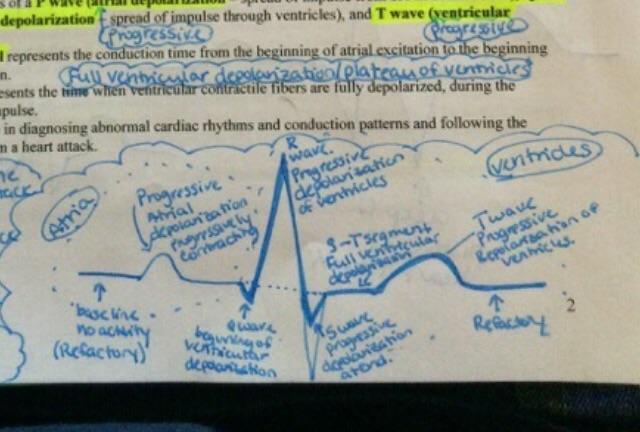 The ECG is invaluable in diagnosing abnormal cardiac rhythms and conduction patterns and following the course of recovery from a heart attack. | back 246 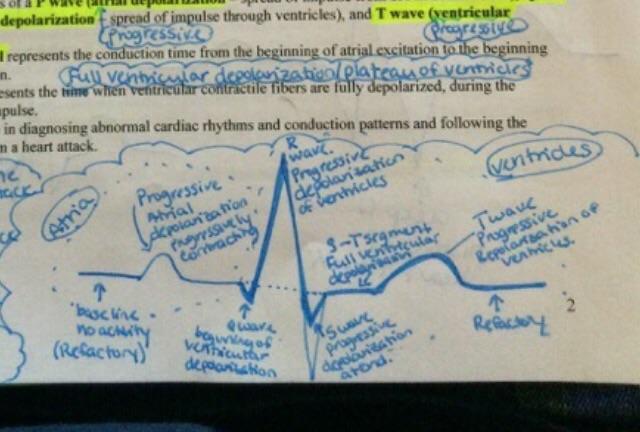 The ECG is invaluable in diagnosing abnormal cardiac rhythms and conduction patterns and following the course of recovery from a heart attack. |
front 247 A __________ consists of the systole (contraction) and diastole (relaxation) of both atria, rapidly followed by the systole and diastole of both ventricles. | back 247 Cardiac cycle |
front 248 The phases of the cardiac cycle are? | back 248 (1) the relaxation (or quiescent) period, (2) ventricular filling, and (3) ventricular systole. |
front 249 With an average heart rate of 75 beats/min, a complete cardiac cycle requires 0.8 sec. True or False | back 249 True |
front 250 A ___________ is an abnormal sound that consists of a flow noise that is heard before, between, or after the lubb-dupp or that may mask the normal sounds entirely. Some murmurs are caused by turbulent blood flow around valves due to abnormal anatomy or increased volume of flow. | back 250 Heart murmur |
front 251 The act of listening to sounds within the body is called? And is usually done with a stethoscope. | back 251 Auscultation |
front 252 The sound of a heartbeat comes primarily from the turbulence in blood flow caused by the closure of the valves, not from the contraction of the heart muscle. True or False
| back 252 True |
front 253
| back 253
|
front 254 ___________ is the amount of blood ejected by the left ventricle (or right ventricle) into the aorta (or pulmonary trunk) per minute. It is calculated as follows: CO = stroke volume x beats per minute | back 254 Cardiac output (CO) |
front 255 Is the amount of blood ejected by a ventricle during each systole. | back 255 Stroke volume (SV) |
front 256 Stroke volume depends on how much blood enters a ventricle during diastole, that is, the stretch on the heart before it contracts (end-diastolic volume, or EDV, also called preload), and how much blood is left in a ventricle following its systole (end-systolic volume, or ESV). EDV averages 120-130 ml and SV is about 70 ml; ESV, then is approximately 50-60 ml. | back 256 Stroke volume depends on how much blood enters a ventricle during diastole, that is, the stretch on the heart before it contracts (end-diastolic volume, or EDV, also called preload), and how much blood is left in a ventricle following its systole (end-systolic volume, or ESV). EDV averages 120-130 ml and SV is about 70 ml; ESV, then is approximately 50-60 ml. |
front 257 Stroke volume also is related to contractility (forcefulness of contraction at any given time) and afterload (pressure that must be exceeded before ventricular ejection can begin); factors that increase the stroke volume or heart rate tend to increase CO and vice versa. | back 257 Stroke volume also is related to contractility (forcefulness of contraction at any given time) and afterload (pressure that must be exceeded before ventricular ejection can begin); factors that increase the stroke volume or heart rate tend to increase CO and vice versa. |
front 258 _________ is the ratio between the maximum cardiac output a person can achieve and the cardiac output at rest. | back 258 Cardiac reserve |
front 259 According to the Frank-Startling law of the heart, a greater preload (stretch) on cardiac muscle fibers just before they contract increases their force of contraction during systole. True or False | back 259 True |
front 260 A greater preload (stretch) on cardiac muscle fibers just before they contract increases their force of contraction during systole. What is this called? | back 260 Frank-Startling law of the heart |
front 261 This results when the heart cannot supply the oxygen demands of the body; it is characterized by diminished blood flow to the various tissues of the body and by accumulation of excess blood in the various organs because the heart is unable to pump out the blood returned to it by the great veins. Causes include chronic hypertension and myocardial infarction (heart attack). What is this called? | back 261 Congestive heart failure (CHF) |
front 262 Cardiac output does not depends on heart rate as well as stroke volume. True or False | back 262 False |
front 263
| back 263
|
front 264
| back 264
|
front 265 Help for Failing Hearts
Researchers are investigating a wide variety of devices and techniques to aid a failing heart, including heart transplants, artificial hearts, and cardiac assist devices | back 265 Help for Failing Hearts
Researchers are investigating a wide variety of devices and techniques to aid a failing heart, including heart transplants, artificial hearts, and cardiac assist devices |
front 266 ___________ in heart disease that can be modified include high blood cholesterol level, high blood pressure cigarette smoking, obesity, and lack of regular exercise. Other factors include diabetes mellitus; genetic predisposition; male gender; high blood levels of fibrinogen, renin, and uric acid; and left ventricular hypertrophy. | back 266 Risk factors |
front 267 An __________ is an abnormality or irregularity in the heart rhythm resulting from a disturbance in the conduction system of the heart; due either to faulty production of electrical impulses or to poor conduction of impulses as they pass through the system. | back 267 arrhythmia |
front 268
| back 268
|
front 269
| back 269
|
front 270 ___________ is a process in which smooth muscle cells proliferate and fatty substances especially cholesterol and triglycerides (neural fats), accumulate in the walls of medium-sized and large arteries in response to certain stimuli, such as endothelial damage. | back 270 Atherosclerosis |
front 271
| back 271
|
front 272 _________ is a condition in which the smooth muscle of a coronary artery undergoes a sudden contraction, resulting in narrowing of a blood vessel. | back 272 Coronary artery spasm |
front 273 A congenital defect is a defect that exists at birth, and usually before birth. True or False | back 273 True |
front 274
| back 274
|
front 275 End of Chapter 20 | back 275 End of Chapter 20 |
front 276 These are vessels that carry away blood from the heart to the tissues, what are these called? | back 276 Arteries |
front 277 As the arterioles enter a tissue, they branch into countless microscopic vessels called what? | back 277 Capillaries |
front 278 These vessals carry blood from the tissues back to the heart, what are these called? | back 278 Veins |
front 279 These are very small, almost microscopic, arteries that deliver blood to capillaries. What are these called? | back 279 Arterioles |
front 280 An alternate blood route from an anastomosis is called what? | back 280 Collateral circulation |
front 281 Arteries that do not anastomose are called? | back 281 End arteries |
front 282 This decreases in the size of the lumen of a blood vessel, what is this called? | back 282 Vasoconstriction |
front 283 This increase in the size of the lumen of a blood vessel, what is this called? | back 283 Vasodilation |
front 284 These are microscopic blood vessels through which materials are exchanged between blood and tissue cells. What are these called? | back 284 Capillaries |
front 285 Capillaries usually connect what with each other? | back 285 Arterioles and Venules |
front 286 Capillary walls are composed of only a single layer of cells (endothelium) and a basement membrane. True or False | back 286 True |
front 287 Capillaries branch to form an extensive capillary network throughout the tissue. This network increases the surface area, allowing a rapid exchange of large quantities of materials. True or False | back 287 True |
front 288 The flow of blood through capillaries is regulated by who?? | back 288 By vessels with smooth muscle in their walls. |
front 289 Rings of smooth muscle fibers (cells) called _________ regulate blood flow through true capillaries. | back 289 Pre-capillary sphincters |
front 290 Some capillaries are continuous, whereas others are fenestrated. True or False | back 290 True |
front 291 Microscopic blood vessels in organs such as the liver, spleen, and bone marrow are called _________ ;they are wider than capillaries, more tortuous, and specialized for the functions of the specific organs. | back 291 Sinusoids |
front 292 These are small vessels that are formed from the union of several capillaries; venules merge to form veins. They drain blood from capillaries into veins. What is this called? | back 292 Venules |
front 293 Thses consist of the same three tunics as arteries but have a thinner tunica interna and media and a thicker tunica externa; they have less elastic tissue and smooth muscle and are therefore thinner-walled than arteries. What are these called? | back 293 Veins -They contain valves to prevent backflow of blood. -Weak valves can lead to varicose veins. |
front 294 Vascular (venous) sinuses are veins with very thin walls with no smooth muscle to alter their diameters. Examples are the brain’s superior sagittal sinus and the coronary sinus of the heart. True or False | back 294 True |
front 295 At rest, the largest portion of the blood volume is in systemic veins and venules, collectively called? -They store blood and, through venous vasoconstriction, can move blood to other parts of the body if the need arises. -In cases of hemorrhage, when blood pressure and volume decrease, vasoconstriction of veins in venous reservoirs helps to compensate for the blood loss. | back 295 Blood reservoirs |
front 296 The principal reservoirs are the veins of the abdominal organs (liver and spleen) and skin. True or False | back 296 True |
front 297
(R): (CO = MABP / R) | back 297
(R): (CO = MABP / R) |
front 298 This is the pressure exerted on the walls of a blood vessel; in clinical use, BP refers to pressure in arteries. What is this called? | back 298 Blood pressure |
front 299 Factors that affect blood pressure include? | back 299 Cardiac output, blood volume, viscosity, resistance, and elasticity of arteries. |
front 300 As blood leaves the aorta and flows through systemic circulation, its pressure progressively falls to 0 mmHg by the time it reaches the right atrium. True or False | back 300 True |
front 301 _________ refers to the opposition to blood flow as a result of friction between blood and the walls of the blood vessels. | back 301 Resistance |
front 302 Resistance depends on what? | back 302 Blood viscosity, blood vessel length, and blood vessel radius. |
front 303 This refers to all of the vascular resistances offered by systemic blood vessels; most resistance is in arterioles, capillaries, and venules due to their small diameters. What is this called? Also known as total peripheral resistance. | back 303 Systemic vascular resistance (SVR) |
front 304 The near equilibrium at the arterial and venous ends of a capillary by which fluids exit and enter is called? | back 304 Startling’s Law of the Capillaries |
front 305 Occasionally, the balance of filtration and reabsorption between interstitial fluid and plasma is disrupted, allowing an abnormal increase in interstitial fluid called? | back 305 Edema |
front 306 These are all factors that come from what
| back 306
|
front 307 A number of factors aid ________ , the volume of blood flowing back to the heart from the systemic veins, by increasing the magnitude of the pressure gradient between the venules and the right atrium. Blood return to the heart is maintained by several factors, including skeletal muscular contractions, valves in veins (especially in the extremities), and pressure changes associated with breathing. | back 307 Venous return |
front 308 Fill in the blank.
| back 308 Cardiovascular (CV) center |
front 309 Output from the CV center flows along sympathetic and parasympathetic fibers. Sympathetic impulses along ____________ increase heart rate and contractility. Parasympathetic impulses from vagus (X) nerves decrease heart rate. | back 309 Cardioaccelerator nerves |
front 310 Parasympathetic impulses from _________ decrease heart rate. | back 310 Vagus (X) nerves |
front 311 The sympathetic division also continually sends impulses to smooth muscle in blood vessel walls via ___________. The result is a moderate state of tonic contraction or vasoconstriction, called __________. | back 311 Vasomotor nerves and V asomotor tone. |
front 312 These are important pressure-sensitive sensory neurons that monitor stretching of the walls of blood vessels and the atria. What is this called? | back 312 Baroreceptors (pressoreceptors) |
front 313
| back 313 Cardiac sinus reflex |
front 314 The cardiac sinus reflex is concerned with maintaining normal blood pressure in the brain and is initiated by baroreceptors in the wall of the carotid sinus. True or False | back 314 True |
front 315 The ___________ is concerned with general systemic blood pressure and is initiated by baroreceptors in the wall of the arch of the aorta or attached to the arch. | back 315 Aortic reflex |
front 316 The aortic reflex is not concerned with general systemic blood pressure and is initiated by baroreceptors in the wall of the arch of the aorta or attached to the arch. True or False | back 316 False |
front 317 If blood pressure falls, the baroreceptor reflexes accelerate heart rate, increase __________, and promote vasoconstriction. | back 317 Force of contraction |
front 318 The right heart (atrial) reflex responds to increases in venous blood pressure and is initiated by baroreceptors in the right atrium and venae cavae. True or False | back 318 True |
front 319 The __________ responds to increases in venous blood pressure and is initiated by baroreceptors in the right atrium and venae cavae. | back 319 Right heart (atrial) reflex |
front 320 Receptors sensitive to chemicals are called? -They monitor blood levels of oxygen, carbon dioxide, and hydrogen ion concentration. | back 320 Chemoreceptors |
front 321 This refers to local, automatic adjustments of blood flow in a given region to match the particular needs of the tissue. What is this called? | back 321 Autoregulation |
front 322 What is the principle element not a direct stimulus for autoregulation? | back 322 Oxygen |
front 323 __________, or faint, refers to a sudden, temporary loss of consciousness followed by spontaneous recovery. It is most commonly due to cerebral ischemia (lack of sufficient blood flow). | back 323 Syncope |
front 324 _________ is an inadequate cardiac output that results in failure of the cardiovascular system to deliver adequate amounts of oxygen and nutrients to meet the metabolic needs of body cells. As a result, cellular membranes dysfunction, cellular metabolism is abnormal, and cellular death may eventually occur without proper treatment.
| back 324 Shock |
front 325 Stages of shock are all characterized by inadequate perfusion of tissues. True or False | back 325 True |
front 326 This refers to decreased blood volume resulting from loss of blood or plasma due to acute hemorrhage or excessive fluid loss (as in excess vomiting, diarrhea, sweating, dehydration, urine production, and burns). What is this called? | back 326 Hypovolemic shock |
front 327 The development of shock occurs in three principal stages, what are they? | back 327 Stage I is compensated (nonprogressive) shock Stage II is decompensated (progressive) shock Stage III is irreversible shock |
front 328 Shock, in which negative feedback systems restore homeostasis. What stage is this called?
| back 328 Stage I is compensated (nonprogressive) shock |
front 329 In which positive feedback cycles intensify the shock and immediate medical intervention is required. What stage is this called?
| back 329 Stage II is decompensated (progressive) shock |
front 330 This is rapid deterioration of the cardiovascular system that cannot be helped by compensatory mechanisms or medical intervention. What stage is this? | back 330 Stage III is irreversible shock |
front 331 ___________ is the alternate expansion and elastic recoil of an artery wall with each heartbeat. It may be felt in any artery that lies near the surface or over a hard tissue, and is strongest in the arteries closest to the heart; the radial artery is most commonly used to feel the pulse. | back 331 Pulse |
front 332 A normal resting pulse (heart) rate is? | back 332 60 to 100 beats |
front 333 Means a rapid resting heart or pulse rate (> 100 beats/min). | back 333 Tachycardia |
front 334 Indicates a slow resting heart or pulse rate (< 60 beats/min). | back 334 Bradycardia |
front 335 Blood pressure is the pressure exerted by blood on the wall of an artery when the left ventricle undergoes systole and then diastole. It is measured by the use of a ____________ usually in one of the brachial arteries. | back 335 Sphygmomanometer |
front 336 __________ is the force of blood recorded during ventricular contraction. | back 336 Systolic blood pressure (SBP) |
front 337 ________ is the force of blood recorded during ventricular relaxation. | back 337 Diastolic blood pressure (DBP) |
front 338 The various sounds that are heard while taking blood pressure are called? | back 338 Korotkoff sounds |
front 339 The normal blood pressure of a young adult male is 120/80 mmHg (8-10 mmHg less in a young adult female). The range of average values varies with many factors. True or False | back 339 True |
front 340 This is the difference between systolic and diastolic pressure. It normally is about 40 mmHg and provides information about the condition of the arteries. What is this called? | back 340 Pulse pressure (PP) |
front 341 The blood vessels are organized into parallel routes that deliver blood throughout the body. True or False | back 341 True |
front 342 The largest circulatory route is the? | back 342 Systemic circulation |
front 343 Two of the several subdivisions of the systemic circulation are coronary (cardiac) circulation, which supplies the myocardium of the heart; the cerebral circulation, which supplies the brain; and the hepatic portal circulation, which extends from the gastrointestinal tract to the liver. | back 343 Two of the several subdivisions of the systemic circulation are coronary (cardiac) circulation, which supplies the myocardium of the heart; the cerebral circulation, which supplies the brain; and the hepatic portal circulation, which extends from the gastrointestinal tract to the liver. |
front 344 Other routes include pulmonary circulation and fetal circulation. | back 344 Other routes include pulmonary circulation and fetal circulation. |
front 345 The ______________ takes oxygenated blood from the left ventricle through the aorta to all parts of the body, including some lung tissue (but does not supply the air sacs of the lungs) and returns the deoxygenated blood to the right atrium.
| back 345 Systemic circulation |
front 346 Blood returns to the heart through the systemic veins. All the veins of the systemic circulation flow into the superior or inferior venae cavae or the coronary sinus, which in turn empty into the right atrium. True or False | back 346 True |
front 347 The ___________ collects blood from the veins of the pancreas, spleen, stomach, intestines, and gallbladder and directs it into the hepatic portal vein of the liver before it returns to the heart. | back 347 Hepatic portal circulation |
front 348 A ____________ carries blood between two capillary networks, in this case from capillaries of the -This circulation enables nutrient utilization and blood detoxification by the liver. | back 348 P ortal system |
front 349 The ___________ takes deoxygenated blood from the right ventricle to the air sacs of the lungs and returns oxygenated blood from the lungs to the left atrium. -It allows blood to be oxygenated for systemic circulation. | back 349 Pulmonary circulation |
front 350 The ___________ involves the exchange of materials between fetus and mother. | back 350 Fetal circulation |
front 351 ___________ or high blood pressure, is the most common disease affecting the heart and blood vessels. It is classified as primary (essential) or secondary. | back 351 Hypertension |
front 352 ________________________ (approximately 90-95% of all hypertension cases) is a persistently elevated blood pressure that cannot be attributed to any particular organic cause. | back 352 Primary (essential) hypertension |
front 353 Only _____________ has causes that are identifiable. Two of these are kidney disease and adrenal hypersecretion. | back 353 Secondary hypertension |
front 354 An __________ is a thin, weakened section on the wall of an artery or a vein that bulges outward, forming a balloon-like sac of the blood vessel. Left untreated, it may burst, causing massive hemorrhage with shock, severe pain, cardiovascular accident (CVA, or stroke), or death. Some may be surgically repaired. | back 354 Aneurysm |
front 355 ______________ is a condition in which the heart muscle receives inadequate oxygen due to blockage of its blood flow. It may be caused by atherosclerosis, coronary artery spasm, and other factors. | back 355 Coronary artery disease (CAD) |
front 356 ______________ is a blood clot (thrombus) in a deep vein, especially in the lower extremities. It has two serious complications: pulmonary embolism and postphlebitic syndrome. | back 356 Deep-venous thrombosis (DVT) |