| back 1 - Transports essential oxygen to tissues along with nutrients
required for cellular metabolism
- provides for the necessary
removal of many cell wastes
- plays a critical role in the
body's defenses/immune system
- serves in maintaining body
homeostasis
- Provides a mechanism for controlling body
temperature by distributing Core heat throughout the peripheral
tissues
|
front 2 Two Separate Circulations | back 2 - The pulmonary circulation
- The systemic
circulation
|
front 3 The Pulmonary Circulation | back 3 - allows The exchange of oxygen and carbon dioxide in the
lungs
|
| back 4 - Provides for the exchange of nutrients and wastes between the
blood and the cells throughout the body
|
| back 5 - Transports Blood
away from the heart
|
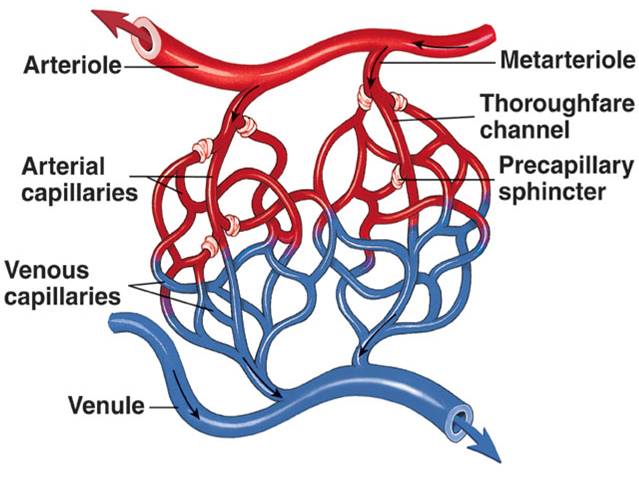
| back 6 - The smaller branches of arteries
- Controls the amount
of blood flowing into the capillaries in specific areas through the
degree of contraction of smooth muscle in the vessel wall
|
| back 7 - Very small vessels
- Forms the microcirculation
- Blood flow very slowly through capillaries
-
precapillary sphincters
- Single
endothelial layer
- Facilitates the exchange of fluid,
oxygen, carbon dioxide, electrolytes glucose, and other
nutrients and waste between the blood and interstitial
fluid
|
| back 8 - Determines the amount of blood flowing from the arterioles into
the individual capillaries
- depends on the metabolic needs
of the tissues
|
| back 9 - conduct blood from the capillary beds toward the heart
|
| back 10 - returns blood back to the heart
- Have thinner walls
than arteries and less smooth muscles
|
| back 11 - the blood vessels that hold the major portion of
theintravascular blood volume
- veins
|
front 12 Walls of arteries and veins | back 12 -
Tunica Intima
- the inner layer
- endothelium (simple squamous)
- flat so fluid can be
exchanged back-and-forth
-
Tunica Media
- The middle layer
- Layer of smooth muscle
- Controls the diameter and
lumen size
-
Tunica Adventitia
- outer connective
tissue layer
- Contains elastic and collagen fibers
|
| back 13 - A reflex adjustment in a small area of a tissue
- varies
depending on the needs of the cells in the area
|
front 14 Causes of local vasodilation | back 14 - decrease in pH
- increase in carbon dioxide
- decrease in oxygen
|
| back 15 - Water and its dissolve solutes (plasma) = 55% of the whole
blood volume
- remaining 45% is composed of the cells or
formed elements erythrocytes, leukocytes, and thrombocytes
|
| back 16 - Refers to The proportion of cells in blood
- Indicates
the viscosity of the blood
|
| back 17 - The clear yellowish fluid remaining after the cells
have been removed
-
contains:
- water 92%
- plasma
proteins 7%
- other solutes 1%
- Amino acids
- Carbohydrates
- Lipids
- Vitamins
- Hormones
- Enzymes
- Electrolytes
- Wastes
|
| back 18 - Refers to the fluid and solutes remaining after the cells and
fibrinogen has been removed
|
front 19 Examples of plasma proteins | back 19 - Albumin
- Globulins/Anti-bodies
- fibrinogen
|
| back 20 - Maintains osmotic pressure in the blood
|
| back 21 - essential for the formation of blood clots
|
| back 22 - Origination of all blood cells
- found in the flat and
irregular bones, ribs, vertebrae, sternum, and pelvis
|
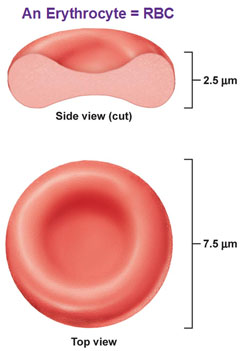
front 23 Erythrocytes or red blood cells | back 23 - Biconcave flexible discs
- non-nucleated when mature
state
- Contain hemoglobin
- Size and structure are
essential for easy passage to small capillaries
- life span =
120 days b/c no nucleus
|
| back 24 - Originates in the kidney
- Hormone that stimulates
erythrocyte production in the red bone marrow
|
| back 25 -
Consists of:
- the globlin portion
- two pairs of amino acid chains
- four
heme groups
- each containing a ferrous iron atom, to
which oxygen molecule can attach
|
| back 26 - A bright red color that distinguishes arterial blood from
venous blood
|
| back 27 - Dark bluish red in color and font and venous blood
|
| back 28 - Production of white blood cells
- Stimulated by colony
stimulating factors that are produced by cells such as macrophages
and T lymphocytes
|
| back 29 - Makes up only about 1% of blood volume
- Subdivided into
two categories:
- Granulocytes
- Agranulocytes
- All types develop in differentiate from the original
stem cell in bone marrow
- There are five types of leukocytes
- Lymphocytes
- Neutrophils
- Basophils
- Eosinophils
- Monocytes
|
| back 30 - Makes up 30 to 40% of the white blood cells
|
| back 31 - The most common leukocyte
- Makes up 50
to 60% of White blood cells
- Survive only four days
- The first to respond to any tissue damage And
phagocytosis
- Increase in numbers by bacterial
affection
|
| back 32 - Can release histamine and heparin
- Maybe fixed in
tissues or wandering
|
| back 33 - Combat the effects of histamine
- Increase by
allergic rea ctions and parasitic
infections
|
| back 34 - can enter the tissue to become macrophages
|
| back 35 - Indicates the proportion the specific types of white blood
cells in the blood
- Assist in making a diagnosis
|
| back 36 - Essential part of the blood clotting process
- Not
cells
- Non-nucleated
|
| back 37 - An immediate response of a blood vessel to injury is
vasoconstriction of vascular spasm
- Form a platelet plug in
the vessel
- Coagulation mechanism
|
| back 38 - an anticoagulant
- Released from basophils or mast cells
in the tissues
- Blocks thrombin
- Does not dissolve
clots but prevents further growth of the thrombus
|
| back 39 - Determined by the presence of specific antigens on the cell
membranes of erythrocytes
|
| back 40 - An inherited characteristic
- Depends on the presence of
type A or B antigens
|
| back 41 - Lack A and B antigens
- are considered universal
donors
|
| |
| back 43 - May cause blood and incompatibility if the mother is Rh
negative and the fetus is Rh positive
-
Antigen D in plasma membrane = RH positive
-
Absence of antigen D = RH negative
|
front 44 Complete blood count (CBC)
diagnostic test for blood | back 44 - Includes total red blood cells, white blood cells, platelet
count, and morphology (size and shape), a differential count for
white blood cells, hemoglobin, and hematocrit values
|
| back 45 - An increase in white blood cells
- Often associated with
inflammation or infection
|
| back 46 - Decrease in leukocytes
- Occurs with some viral
infections as well as with radiation and chemo therapy
|
| back 47 - Common with allergic responses and parasitic infections
|
| back 48 - Observe with blood sMears
- Shows size, shape,
uniformity, and maturity of cells
- Helps to distinguish
different types of anemia
|
front 49 Hemoglobin (diagnostic test) | back 49 - Amount of hemoglobin per unit volume of blood
- Mean
corpuscular volume
- Indicates the oxygen-carrying capacity
of blood
- Mean corpuscular hemoglobin
|
| back 50 - Assessment of bone marrow function
|
front 51 Chemical analysis of the blood | back 51 - Determine serum levels of components such as iron, vitamin B12,
folic acid, cholesterol, urea, and glucose
|
front 52 Bleeding time (diagnostic test) | back 52 - Measures platelet function
|
front 53 prothrombin time (PT) and partial thromboplastin time (PTT) | back 53 - Measures function of various factors in coagulation
process
- interNational normalized ratio is a standardized
version
|
front 54 partial thromboplastin time | back 54 - Measures the intrinsic pathway
-
PTT... the 2 t's are in(trinsic) a relationship
|
| back 55 - measures the extrinsic pathway
|
| back 56 - A reduction in oxygen transport in the blood due to a decrease
in hemoglobin content
- May result from the declining
production of the protein, a decrease in the number of erythrocytes,
or a combination of these factors
- May be classified by
typical cell morphology
-
oxygen deficiency leads to:
- Less energy production and all cells
- Cell
metabolism and reproduction diminished
- Compensation mechanism to improve the oxygen supply
- ex:
- Tachycardia
- peripheral vasoconstriction
- General signs of anemia
- Fatigue, Pallor,
dyspnea, and tachycardia
- Decrease
regeneration of epithelial cells
|
| back 57 - Insufficient iron impairs hemoglobin synthesis
- Which
reduces the amount of oxygen transported in the blood
- Red blood cells are microcytic
and hypochromic
- Very
common
- Ranges from mild to severe
- Occurs in all
age groups
- One in five women is affected
- Proportion increases for pregnant women
- Frequently a sign of an underlying problem
|
front 58 Etiology of iron deficiency anemia | back 58 - Dietary intake of iron may be below the minimum
requirement
- Chronic blood loss
- duodenal absorption
of iron may be impaired
- Severe liver disease may affect
both iron absorption and iron storage
|
front 59 Manifestations of iron deficiency anemia | back 59 - pallor of the skin and mucous membranes
- Due to
vasoconstriction
- Fatigue,lethargy, and cold intolerance
- b/c cell
metabolism decreased
- Irritability
- A
central nervous system response to hypoxia
- Degenerative changes
- such as brittle hair, spoon shaped
and rigid nails
- Inflammation of oral mucosa
and tongue
- Menstrual irregularities
- Delayed
healing
- Tachycardia, heart palpitations, dyspnea,
syncope
* People who have iron deficiency anemia may have unusual craving
for nonfood items such as ice, paint, or starch. This craving is
called pica |
front 60 Diagnostic tests for Iron deficiency anemia | back 60 - Laboratory test demonstrate low values of hemoglobin,
hematocrit, mean corpuscular volume and mean corpuscular hemoglobin,
serum ferritin and serum iron, and transferrin saturation
|
front 61 Treatment for iron deficiency anemia | back 61 - Identified underlying cause and resolves if possible
- Consume Iron rich foods or iron supplements
|
front 62 pernicious anemia: vitamin B12 deficiency (megaloblastic anemia) | back 62 - The common form of megaloblastic anemia
- Caused by the
malabsorption of the vitamin B12
- Iron deficiency
may be present as well
- Red blood cells are very large and
contain nuclei
- Dietary and sufficiency is a very rare
cause
- May be an outcome of surgeries in which the parietal
cells are removed or resection of the ileum which is a sight of
absorption
|
front 63 Vitamin B12 and nerve cells | back 63 - Vitamin B12 is needed for the function and
maintenance of neurons
- Deficiency can result in
neuropsychiatric symptoms
|
front 64 Manifestations of pernicious anemia | back 64 - Tongue is typically in large, red, sore, and shiny
- Decrease in gastric acid leads to digestive discomfort such as
nausea and diarrhea
- Tingling or burning sensations in the
extremities or loss of coordination and ataxia
|
front 65 Diagnostic tests for pernicious anemia | back 65 - Microscopic examination (erythrocytes)
- Bone marrow
examination (hyperactive)
- Vitamin B12 serum
levels below normal
|
front 66 Treatment for Pernicious Anemia | back 66 - Oral supplements are recommended
- Vitamin
B12 is administered by injection
|
| back 67 - Results from impairment or failure of bone marrow leading to
loss of stem cells and pancytopenia
- may be temporary or
permanent
- often idiopathic
|
| back 68 - decreased numbers of erythrocytes, leukocytes, and thrombocytes
in the blood.
|
| back 69 - results from excessive destruction of RBCs
- leads to a
low erythrocyte count and low hemoglobin
-
causes:
- genetic defects
- immune
reactions
- Changes in blood chemistry
- Presence of
toxins in the blood
- Infections such as malaria
- Antigen-antibody reaction
- Incompatible blood
transfusion
|
front 70 What term is used to describe a deficit of all types of blood cells?
- Leucopenia
- Neutropenia
- Pancytopenia
- Erythrocytosis
| |
front 71 Capillary walls consist of:
- multiple endothelial layers.
- a thick layer of smooth
muscle.
- two or three epithelial layers.
- a single
endothelial layer
| back 71 - a single endothelial layer
|
front 72 Individuals with type O blood are considered to be universal donors
because their blood:
- contains A and B antibodies.
- contains A and B
antigens.
- lacks A and B antibodies.
- lacks A and B
antigens.
| |
front 73 What causes numbness and tingling in the fingers of individuals with
untreated pernicious anemia?
- Persistent hyperbilirubinemia
- Increasing acidosis
affecting metabolism
- Vitamin B12 deficit causing
peripheral nerve demyelination
- Multiple small vascular
occlusions affecting peripheral nerves
| back 73 - Vitamin B12 deficit causing peripheral nerve
demyelination
|
front 74 What is the cause of oral ulcerations and delayed healing occurring
with any severe anemia?
- Lack of folic acid for DNA synthesis
- Frequent
microinfarcts in the tissues
- Deficit of oxygen for
epithelial cell mitosis and metabolism
- Elevated bilirubin
levels in blood and body fluids
| back 74 - Deficit of oxygen for epithelial cell mitosis and
metabolism
|
front 75 Why is pernicious anemia treated with injections of vitamin B12?
- An immune reaction in the stomach would destroy the
vitamin.
- Digestive enzymes would destroy the vitamin.
- The vitamin irritates the gastric mucosa.
- The ingested
vitamin would not be absorbed into the blood.
| back 75 - The ingested vitamin would not be absorbed into the blood.
|
front 76 Why do vascular occlusions and infarcts occur frequently with sickle
cell anemia?
- The red blood cells are abnormally large.
- Increased
hemolysis of erythrocytes occurs.
- Erythrocytes change to
sickle shape when hypoxia occurs
- HbS is unable to transport
oxygen
| back 76 - Erythrocytes change to sickle shape when hypoxia occurs
|
front 77 In cases of polycythemia vera, blood pressure is elevated as a result of:
- increased blood volume.
- frequent infarcts in the
coronary circulation.
- congested spleen and bone
marrow.
- increased renin and aldosterone secretions.
| |
front 78 In individuals with pernicious anemia, antibodies form to:
- vitamin B12 .
- intrinsic factor or parietal
cells.
- mucus-producing glands.
- hydrochloric
acid.
| back 78 - intrinsic factor or parietal cells.
|
front 79 Petechiae and purpura are common signs of:
- excessive hemolysis.
- leucopenia.
- increased
bleeding.
- hemoglobin deficit.
| |
front 80 Which of the following substances acts as an anticoagulant?
- Prothrombin
- Heparin
- Fibrinogen
- Vitamin K
| |
front 81 Why is excessive bleeding a common occurrence with acute leukemia?
- Deficit of calcium ions
- Impaired production of
prothrombin and fibrinogen
- Decreased platelets
- Dysfunctional thrombocytes
| |
front 82 Multiple myeloma is a malignant tumor involving:
- plasma cells.
- granulocytes
- bone cells.
- lymph nodes.
| |
front 83 The Reed-Sternberg cell is diagnostic for:
- chronic myeloblastic leukemia.
- Hodgkin’s
lymphoma.
- multiple myeloma.
- non-Hodgkin’s
lymphoma.
| |
front 84 Which of the following applies to the leukemias?
- Chronic leukemias are more common in older people.
- AML is the most common childhood leukemia.
- Exposure to
chemicals is not considered a predisposing factor.
- Lymphoid
tissue produces abnormal leukocytes.
| back 84 - Chronic leukemias are more common in older people.
|
front 85 A high percentage of blast cells in the leukocyte population
indicates a poor prognosis for an individual with:
- thalassemia
- acute myelogenous leukemia (AML).
- myelodysplastic syndrome.
- multiple myeloma.
| back 85 - acute myelogenous leukemia (AML).
|
front 86 Which of the following applies to erythropoietin?
- It is produced by the liver.
- It increases iron
absorption for heme production.
- It stimulates production of
red blood cells.
- Hypoxia stimulates the red bone marrow to
produce erythropoietin.
| back 86 - It stimulates production of red blood cells.
|
front 87 Microcytic and hypochromic erythrocytes are commonly found as a
result of:
- iron deficiency anemia.
- polycythemia
- disseminated intravascular coagulation.
- hemophilia
A
| |