Instructions for Side by Side Printing
- Print the notecards
- Fold each page in half along the solid vertical line
- Cut out the notecards by cutting along each horizontal dotted line
- Optional: Glue, tape or staple the ends of each notecard together
SWM Module 15: Assessing the Wound — Lower Extremity Ulcers
front 1 What Is a Lower Extremity Ulcer? | back 1 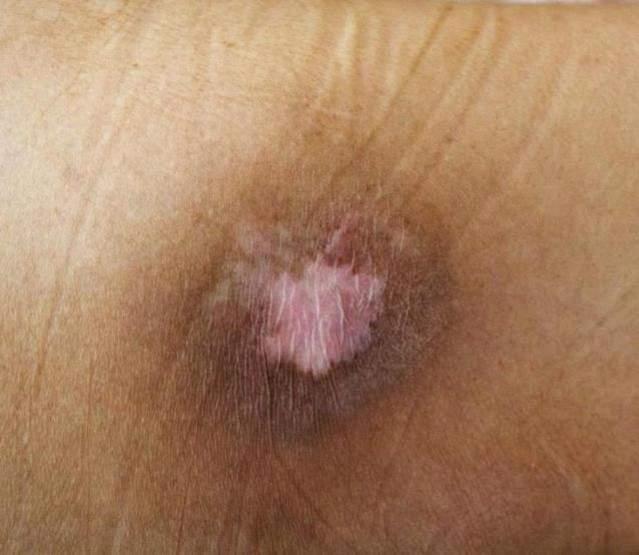 Lower extremity ulcers are open sores or ulcers occurring on the lower legs, typically below the knee (DynaMed, 2022). |
front 2 Frequently encountered types of lower extremity ulcers include: | back 2
|
front 3 Lower extremity ulcers: Primary causes include | back 3
|
front 4 Lower extremity ulcers result from- | back 4 underlying conditions impairing blood flow tissue oxygenation and skin integrity |
front 5 Other causes of lower extremity wounds can include: | back 5 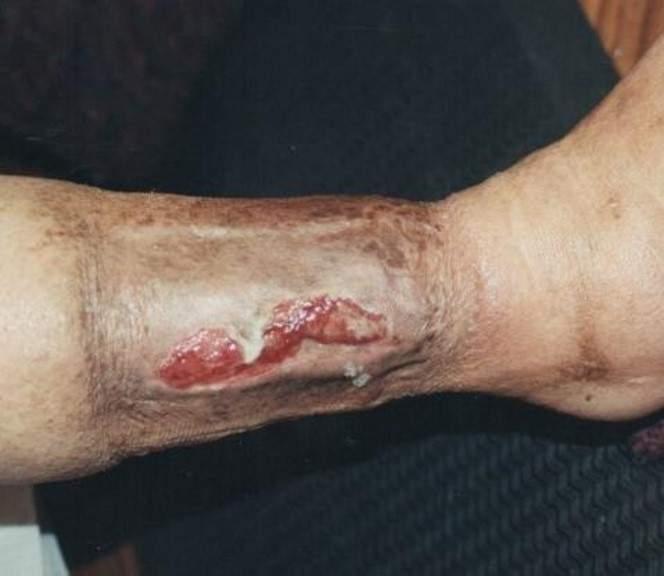
|
front 6 Identifying Lower Extremity Ulcers: Identify the Cause | back 6 Accurate diagnosis allows for tailored treatment, addressing issues like poor circulation, arterial disease, or diabetes to promote healing and avoid missteps like inappropriate treatment. |
front 7 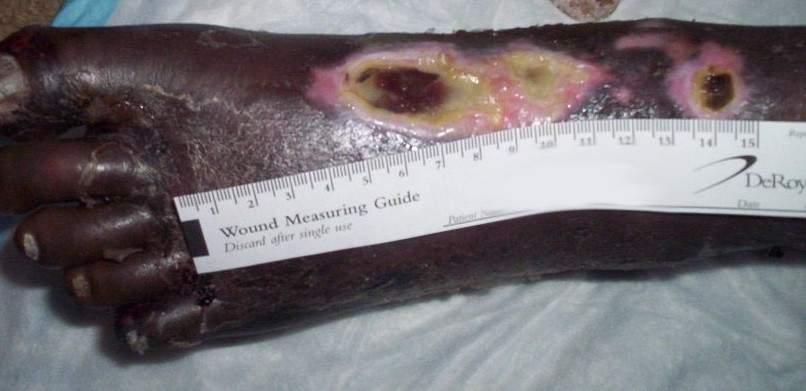 What type of ulcer is this? | back 7 Arterial ulcer |
front 8 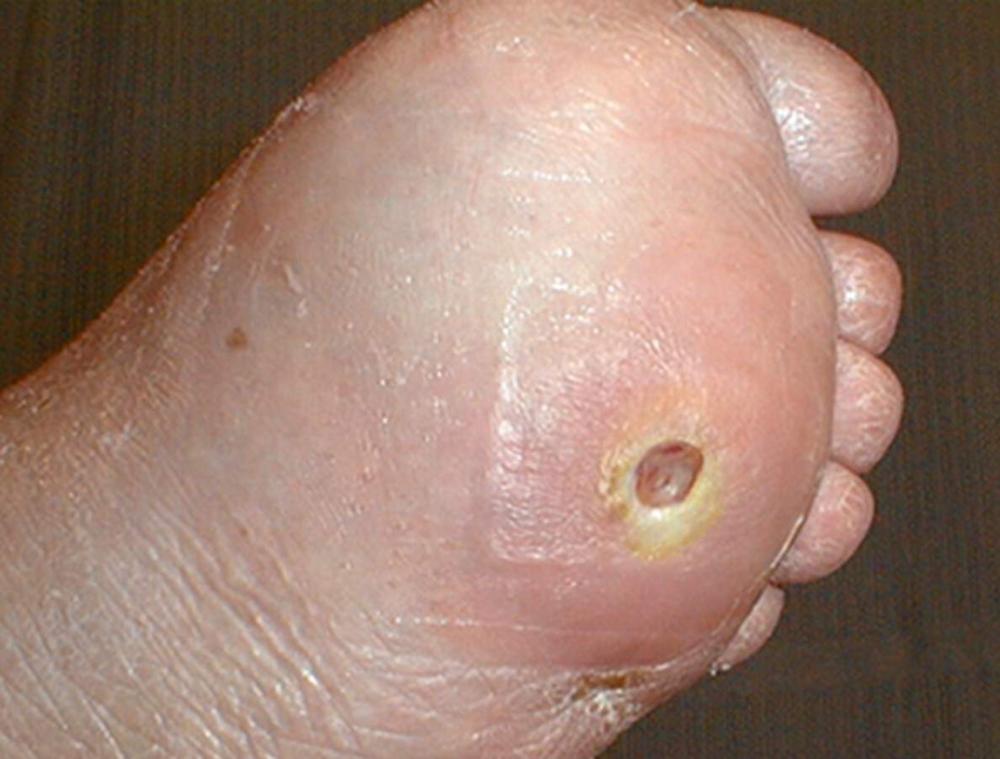 What type of ulcer is this? | back 8 Diabetic foot ulcer |
front 9 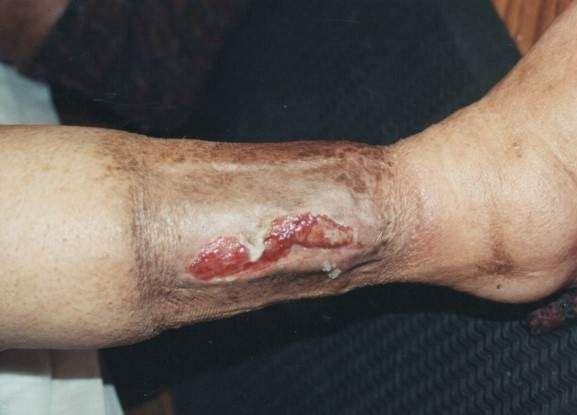 What type of ulcer is this? | back 9 Venous leg ulcer |
front 10 Review of Past Ulcers Rate of Recurrence Many occurrences might indicate chronic issues (e.g., ____ _____). | back 10 venous insufficiency |
front 11 Previous Medical History: Kidney Disease: Renal failure | back 11 is often linked with poor wound healing and increased risk of ulcers. |
front 12 Review of Past Ulcers: Autoimmune Disorders: Autoimmune diseases | back 12 like rheumatoid arthritis or lupus can impact skin integrity and healing. These patients are often on anti-inflammatory/steroid medications which can impair the inflammatory phase of wound healing. |
front 13 Lifestyle Factors Certain modifiable lifestyle factors that increase the risk for ulcers and poor healing should be assessed to see if the patient needs to be coached in these areas (McNichol et al., 2021): | back 13
|
front 14 Diabetes Poorly controlled diabetes can lead to neuropathy and impaired healing. Thus, it is important to assess for (Baranoski & Ayello, 2020; McNichol et al., 2021): | back 14
|
front 15
| back 15 Hyperglycemia negatively impacts healing by prolonging the inflammatory phase and decreasing the immune system's efficiency. |
front 16
| back 16 Loss of sensation, tingling, or numbness in the extremities increases the risk of unseen injuries and subsequent ulcers. |
front 17 Hypertension | back 17 Poorly controlled blood pressure (BP) can contribute to poor circulation and delayed healing (WOCN, 2024). |
front 18 Peripheral Vascular Disease Assess for the following in patients suspected of having peripheral vascular disease (PVD) (McNichol et al., 2021): | back 18
|
front 19 Pain, cramping, or complaints of fatigue in the legs during physical activity that is relieved within 10 minutes of rest can indicate PVD. Intermittent claudication is considered the most typical symptom of LEAD, but most patients are asymptomatic. | back 19
|
front 20 Occurs in the absence of activity. Sleep is affected by throbbing pain with leg elevation that is relieved by dangling affected leg(s) in a dependent position. | back 20
|
front 21 Cardiff Wound Impact Schedule _____ was designed and validated to specifically assess the HRQoL of subjects with chronic wounds (Granado-Casas, et al., 2021). It helps healthcare providers understand how wounds affect various aspects of a patient’s daily life. | back 21 The Cardiff Wound Impact Schedule (CWIS)
|
front 22 The ____-__quickly evaluates the impacts of various chronic wounds on a person’s HRQoL. Its brevity, ease of use, and availability in multiple languages make it highly suitable for clinical practice. (Janke et al., 2024). | back 22 The Wound-QoL |
front 23 The Wound-QoL quickly evaluates the impacts of various chronic wounds on a person’s HRQoL. Its brevity, ease of use, and availability in multiple languages make it highly suitable for clinical practice. (Janke et al., 2024). It is comprised of 17 questions covering three domains including- | back 23
|
front 24 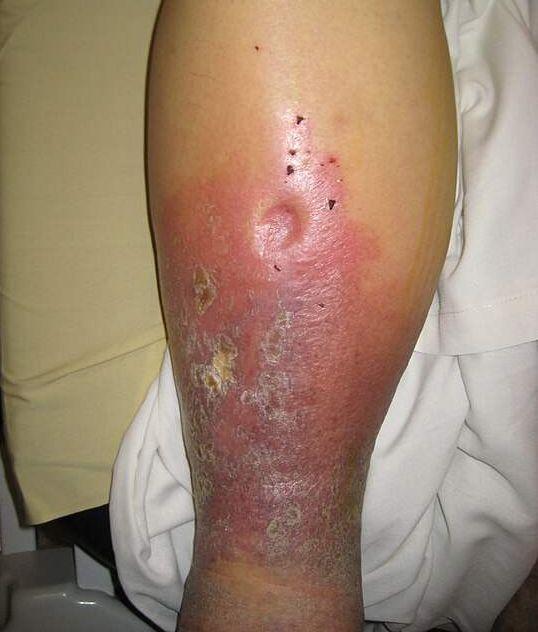 Edema: | back 24 Assessing whether the edema is in one or both LEs can help determine if the cause is a systemic disease affecting the entire body (e.g., heart failure) or related to a condition that affects part of the body (e.g., venous insufficiency) (DynaMed, 2023). |
front 25 Edema presents in the lower extremities as non-pitting or pitting. | back 25
|
front 26 Often caused by conditions like lymphedema or thyroid disorders | back 26 Non-Pitting Edema |
front 27 Often associated with venous insufficiency, congestive heart failure, or kidney disease | back 27 Pitting Edema |
front 28 Pitting Edema: Grade 1 | back 28 Indicates mild pitting edema with a slight indentation that is barely noticeable and about 2 mm deep, disappearing almost immediately. |
front 29 Pitting Edema: Grade 2 | back 29 Is moderate pitting edema with a deeper indentation, about 3 to 4 mm, disappearing within 15 seconds. |
front 30 Pitting Edema: Grade 3 | back 30 Is moderately severe pitting edema with a noticeably deep indentation, about 5 to 6 mm, remaining for more than 15 seconds but less than 1 minute. |
front 31 Pitting Edema: Grade 4 | back 31 Grade 4 Grade 4 indicates severe pitting edema with a very deep indentation, about 8 mm or more, remaining for 2 minutes or longer. |
front 32 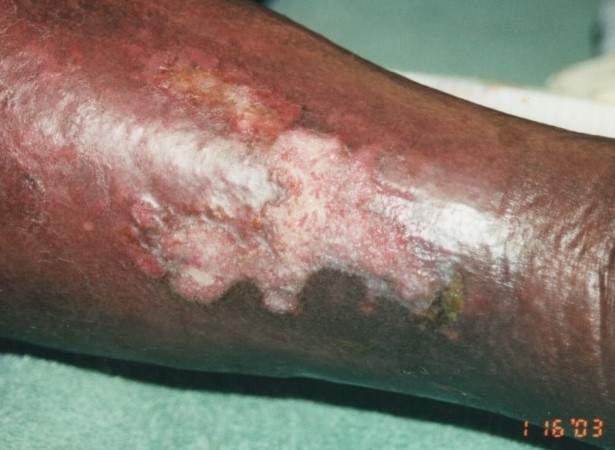 Periwound assessment: | back 32  Hyperpigmentation, shiny taught skin, no hair growth, thickend, evidence of scaling, and ulceration present |
front 33 Sensory Testing- purpose | back 33 Sensory testing is important to determine if patients can detect pain, pressure, and temperature changes, especially for those with diabetes (McNichol et al., 2021). Tests include: |
front 34 Semmes-Weinstein Monofilament Test | back 34 This checks for protective sensation in the feet using a 10G monofilament (McNichol et al., 2021). The monofilament is pressed against the bottom of the foot until it bends. Ask the patient to close their eyes while you perform the test and have them say “yes” each time they feel the pressure from the monofilament. |
front 35 Tuning Fork Test and Temperature Assessment | back 35 The following is the procedure for performing the assessment:
|
front 36 Tuning Fork Test and Temperature Assessment | back 36 A 128 Hz tuning fork is used to test for vibratory sensation loss, which indicates large fiber nerve damage (McNichol et al., 2021). |
front 37 Achilles Tendon Reflex Test the Achilles tendon reflex by gently tapping the Achilles tendon with a reflex hammer while the patient’s foot is dorsiflexed (WOCN, 2024). The procedure is:
A diminished or absent Achilles reflex may suggest peripheral neuropathy. While this reflex is typically present in healthy individuals, it often decreases with age. Bilateral absence in older adults may not be clinically significant. | back 37 Test the Achilles tendon reflex by gently tapping the Achilles tendon with a reflex hammer while the patient’s foot is dorsiflexed (WOCN, 2024). |
front 38 Achilles Tendon Reflex The procedure is: | back 38
A diminished or absent Achilles reflex may suggest peripheral neuropathy. While this reflex is typically present in healthy individuals, it often decreases with age. Bilateral absence in older adults may not be clinically significant. |
front 39 Pulse Check: Dorsalis pedis: | back 39 Located on the top of the foot, between the first and second metatarsal bones. |
front 40 Pulse Check: Posterior tibial: | back 40 Located behind the medial malleolus. |
front 41 PULSE INTESITY RECORD 0 1 2 3 | back 41 0 = ABSENT 1 = DECREASED 2 = NORMAL 3 = BOUNDING * A strong pulse indicates good blood flow |
front 42 Normal capillary refill should be less than _____. | back 42 2 seconds. |
front 43 A delayed refill time of over ___ may indicate poor perfusion (WOCN, 2024). | back 43 3 seconds |
front 44 TRUE / FALSE Capillary refill can be affected by temperature and should not be used exclusively to determine blood flow to the LEs. | back 44 True |
front 45 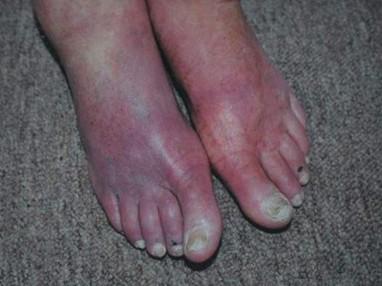 What does this image display | back 45 Dependent Rubor |
front 46 Patients with ___ or ____ _____ will exhibit pallor and dependent rubor after returning to an upright position with their legs dangling. | back 46  PAD ; limb ischemia |
front 47 If there is critical limb ischemia (CLI), the limb will become pale at or before __ elevation | back 47 20° |
front 48 Elevation Phase: With the patient lying supine, raise their legs to about ___. If pallor is noticeable within 30 seconds, it indicates relevant ischemia | back 48 45-60° |
front 49 What is reactive hyperemia? | back 49 After assessing pallor, have the patient sit up with their legs in a dependent position. If their legs slowly revert to their normal color, followed immediately by an intensely red coloration when dependent, this is known as reactive hyperemia, and the leg will eventually return to its normal color after a few minutes |
front 50 The development of dependent rubor indicates that there is some ___ present that requires further diagnostic testing. | back 50 ischemia * Vascular referral may be necessary |
front 51 Common noninvasive diagnostic tests for the lower extremities include (Bryant & Nix, 2024): | back 51
|
front 52 What is TCPO2? | back 52 Assesses blood flow by measuring the partial pressure of oxygen at the periwound skin surface using special sensors |
front 53 TCP02 Range > 40 mmHg = Normal 30 to < 40 mmHg = Borderline ischemia < 30 mmHg = Critical limb ischemia | back 53 Memory : ___ Normal ___ Borderline ischemia ___ Critical limb ischemia |
front 54 TCP02 Interpretation Parameters for Normal? | back 54 > 40 mmHg |
front 55 TCP02 Interpretation Parameters for Borderline ischemia? | back 55 30 to < 40 mmHg |
front 56 TCP02 Interpretation Critical Limb Ischemia? | back 56 < 30 mmHg |
front 57 This test is often done with an oxygen challenge to determine if the patient may benefit from hyperbaric oxygen therapy. Echo Pedal Pulse TCPO2 SPP | back 57 no data |
front 58 Abbreviations: TCPO2 is | back 58 Transcutaneous Oxygen Measurement |
front 59 Abbreviations: SPP | back 59 Skin Perfusion Pressure |
front 60 Abbreviations: NIR | back 60 Near Infrared Light |
front 61 Abbreviations: ABI | back 61 Ankle-Brachial Index |
front 62 Abbreviations: PVR | back 62 Pulse Volume Recording |
front 63 Abbreviations: TBPI | back 63 Toe-Brachial Pressure Index |
front 64 Skin Perfusion Pressure: It can be used on ____ __ and is helpful for predicting ulcer healing or planning amputation level to maintain maximal functioning and mobility | back 64 noncompressible arteries |
front 65 The ____ uses a cuff with a laser Doppler sensor to identify the point at which blood flow resumes when the cuff is deflated. | back 65 The skin perfusion pressure (SPP) |
front 66 SPP Range are: 1. 2. 3. | back 66 1. > 50 mmHg 2. 30 to < 50 mmHg 3. < 30 mmHg |
front 67 SPP Ranges: Interpretations > 50 mmHg = 30 to < 50 mmHg = < 30 mmHg = | back 67 Normal , PAD , Severe PAD |
front 68 SPP Range A pressure exceeding __ mmHg is required for healing | back 68 30 mmHg |
front 69 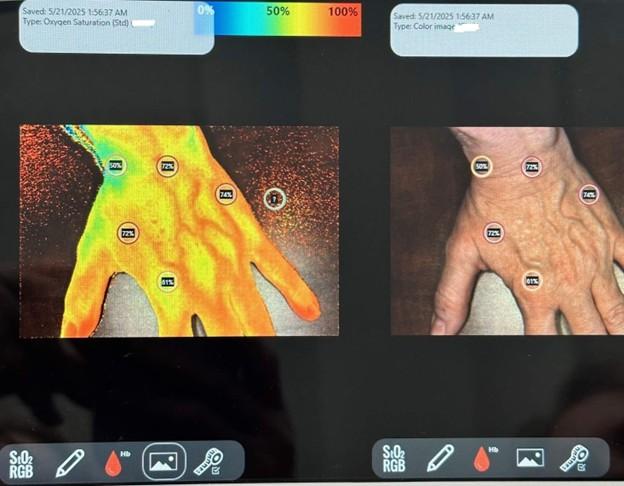 Near-Infrared Light, or NIR | back 69 It is a noninvasive method that quantifies microcirculation and healing potential, photographs the wound, and measures the wound surface area. |
front 70 Technology incorporating ______ assists with detecting oxygenated and deoxygenated blood, conveying a comprehensive picture of the health of the tissues and healing capacities. | back 70 NIR |
front 71 What is Ankle-Brachial Index (ABI)? | back 71 It is standard of care to check the perfusion of a leg before applying any compression. |
front 72 How is ABI calculated? | back 72 It is calculated by dividing the ankle's systolic blood pressure (SBP) measurement by the arm's SBP measurement (Stanford Medicine 25, n.d.). |
front 73 ABI Procedure: Noninvasive | back 73 Testing requires a blood pressure cuff and handheld Doppler. It takes about 10 minutes to complete. |
front 74 Before starting the ABI test make sure | back 74 Patient is comfortable in a supine position and allow them to rest for 10 minutes. Socks and shoes must be removed for the test. |
front 75 ABI procedure: Measuring the Brachial Pressure Systolic brachial pressures will be taken on both arms unless contraindicated (e.g., dialysis shunt). To obtain the brachial SBP: | back 75
|
front 76 ABI procedure: Measuring the Ankle Pressure The ankle SBP will be obtained from both the dorsalis pedis (DP) and posterior tibialis (PT) on both limbs. | back 76
|
front 77 Calculating ABI TRUE / FALSO To calculate the ABI, the higher pressure of the two ankle arteries is divided by the highest arm (brachial) pressure. | back 77 TRUE |
front 78 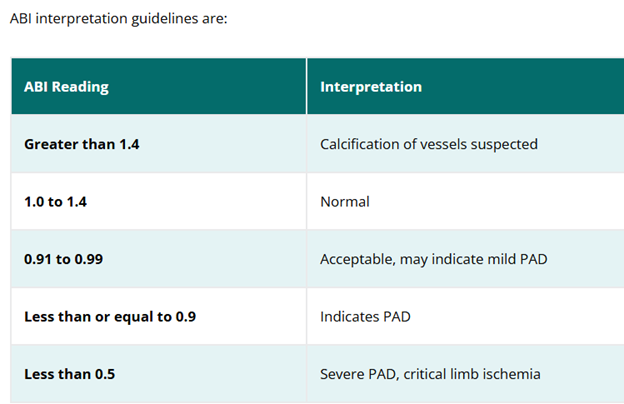 ABI interpretation guidelines are:
| back 78
|
front 79 ABI interpretation reading of >1.4 is | back 79 Calcification of vessels suspected |
front 80 ABI interpretation reading of 0.91 to 0.99 | back 80 Acceptable, may indicate mild PAD |
front 81 ABI interpretation reading of <0.5 | back 81 Severe PAD, critical limb ischemia |
front 82 An ABI of less than 0.5 indicates severe arterial disease, meaning.... | back 82 there may not be sufficient blood flow to heal a chronic wound. This can be limb-threatening, and these patients will need prompt referral to a vascular specialist for further workup and potential interventions to improve blood flow necessary for healing. |
front 83 Remember an ABI of LESS THAN 0.5 indicates ____ ___ ___, meaning ________ | back 83 severe arterial disease ; there may not be sufficient blood flow to heal a chronic wound. This can be limb-threatening, |
front 84 Toe-Brachial Pressure Index | back 84 It is calculated the same way as an ABI, with the SBP of the great toe (hallux) divided by the highest brachial SBP |
front 85 Toe-Brachial Pressure Index | back 85 A toe-brachial pressure index (TBPI) is useful to determine the presence or lack of perfusion in the toes. |
front 86 A result greater than 0.7 is normal, while less than 0.64 indicates PAD for what pressure index? | back 86 Toe-Brachial Pressure Index (TBI) |
front 87 Dopper Waveform Analysis | back 87 Uses a Doppler probe to assess the shape and quality of arterial waveforms. It helps evaluate blood flow and detect defects in arterial supply |
front 88 What test is this? It is often the first step in assessing arterial blood flow in patients with suspected PAD. It helps discern between normal, monophasic, biphasic, and triphasic waveforms, which indicate varying degrees of arterial health. | back 88 Doppler Waveform Analysis |
front 89 Normal arterial flow is triphasic and has three distinct phases; what are they? | back 89
|
front 90 ___ or _____ waveforms suggest reduced vascular resistance or flow restriction. | back 90 Biphasic ; monophasic |
front 91 Biphasic waveforms have two phases, what are they? | back 91
|
front 92 Monophasic waveforms have a single phase, typically ___ ____ ____. | back 92 continuous forward flow |
front 93 A transition from triphasic to monophasic helps ___ the level of the ____ | back 93 localize ; disease |
front 94 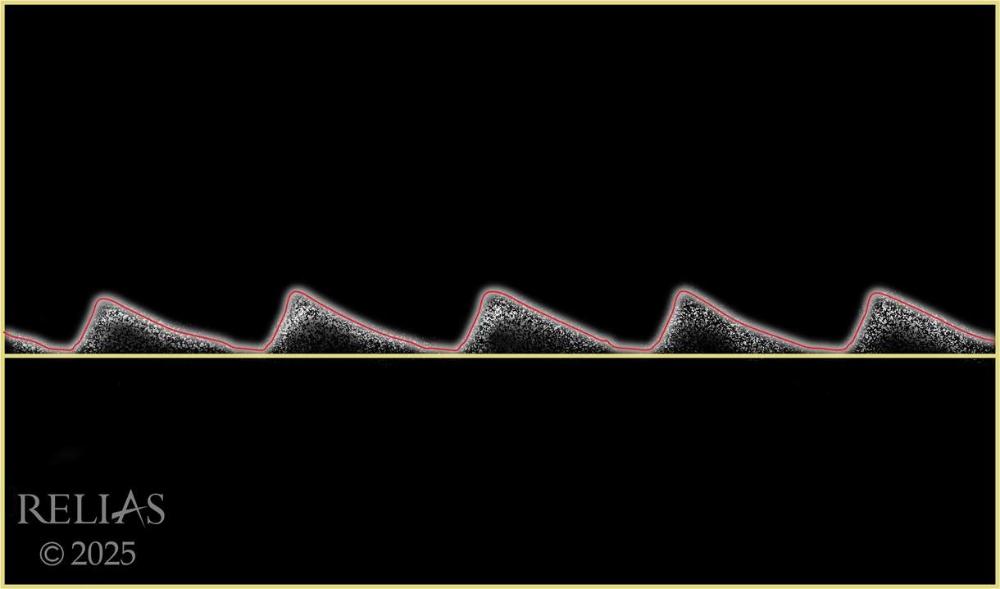 Name the waveform | back 94 Monophasic |
front 95 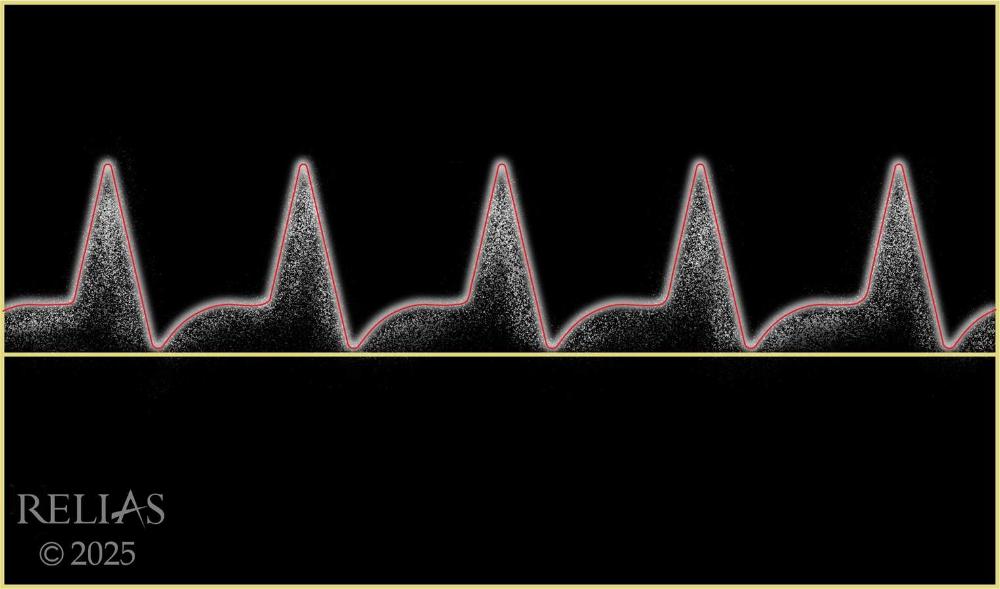 Name the waveform | back 95 Biphasic |
front 96 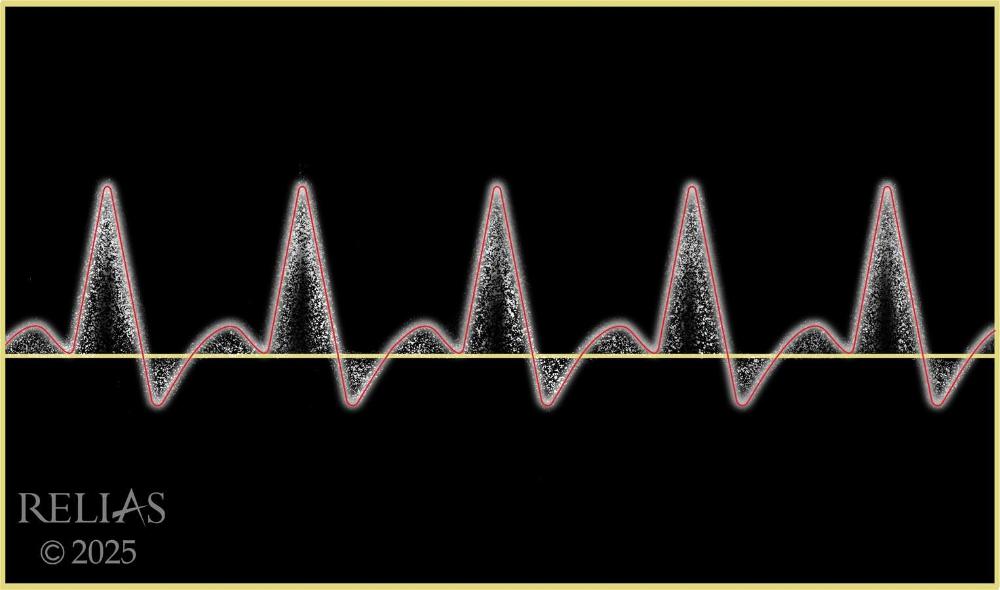 Name the waveform | back 96 Triphasic |
front 97 Pulse Volume Recording | back 97 The pulse volume recording (PVR) graphs limb volume changes with blood flow. |
front 98 Pulse Volume Recording process | back 98 Special cuffs that incorporate pneumoplethysmography (detects volume changes in the arteries) capability are placed around the limb at multiple points along the limb and inflated to standard pressure |
front 99 Pulse Volume Recording (PVR) uses | back 99 PVR is useful for locating areas of blockage in limb segments, especially in patients with non-compressible vessels. |
front 100 PVR A ____ ___ shows a quick rise and sharp peak, with a noticeable dip (dicrotic notch) followed by a rounded curve. | back 100 normal PVR |
front 101 PVR An abnormal PVR, which might have ____ ___ or miss this dip, can signal blocked or reduced blood flow. | back 101 flattened peaks |
front 102 PVR Sudden changes in the ___ or ___ of the wave between different areas suggest a blockage in the blood vessels | back 102 size or shape |
front 103 Using BP cuffs and a Doppler device, the segmental limb pressure test measures BP at multiple points along the limb. The purpose is | back 103 It helps identify a general location of arterial blockages or stenoses but is not exact. |
front 104 Segmental Limb Pressure: process | back 104 This test is performed on both legs to compare the arterial flow from the left and right limbs. A difference of 30 mm Hg at the same level between the left and right legs could suggest an occlusion or blockage in blood flow |
front 105 Segmental Limb Pressure Additionally, if there is a ______ ___ __ from one segment to the other on the same limb, it signals occlusive disease and can help pinpoint its general location (McNichol et al., 2021; Sibley et al., 2017). For example, a decrease in pressure at the thigh level may indicate an aortoiliac or femoral artery issue, whereas pressure drops closer to the ankle suggest distal disease | back 105 significant pressure drop (e.g., greater than 20 mmHg) |
front 106 Venous Duplex | back 106 Ultrasound checks blood flow in the veins, looking for signs of reflux lasting more than 0.5 seconds after muscle contraction or applying pressure (Baranoski & Ayello, 2020). |
front 107 Color Duplex Ultrasound | back 107 This advanced ultrasound technique combines traditional ultrasound imaging with Doppler flow studies. It provides detailed images of blood vessels and flow properties in color. It is ideal for a comprehensive evaluation of both arterial and venous systems. It helps detect precise locations of stenosis, occlusions, aneurysms in arteries. |
front 108 What test helps detect precise locations of stenosis, occlusions, aneurysms in arteries | back 108 Color Duplex Ultrasound |
front 109 What two invasive tests are used to diagnose vessel disease and sometimes involve a procedure (e.g., balloon angioplasty) to fix diseased vessels or serve as an initial step before a complex operation to repair blood vessels | back 109 Angiography and Arteriography. |
front 110 Angiography and Arteriography. | back 110 What Invasive LE Diagnositc tests are usually completed with a vascular specialist in an interventional radiology suite. |
front 111 This uses contrast dye to assess blood flow and check for blockages or narrowing in the arteries. It can precisely identify and measure disease in the arteries, allowing for a clear diagnosis. | back 111 Contrast Angiogram (Arteriogram) |
front 112 The ____ must be checked before the application of compression therapy. The ___ is a noninvasive test that assesses arterial disease by measuring the ratio of BP in the ankle to that in the arm to assess for arterial blockages | back 112 ABI / ABI |
front 113 An ABI over 1.4 suggests ___ ___, common with diabetes, making the ABI unreliable. The next step is referring to a vascular specialist for additional tests. | back 113 calcification of vessels * No compression, it's not recommend until we know there is adequate blood flow present in the limb. |
front 114 The ____ ___ is a network of veins that fight gravity to return deoxygenated blood to the heart and lungs for reoxygenation. | back 114 venous system |
front 115 There are three types of lower extremity veins, including: | back 115 1. Superficial 2. Deep 3. Perforator |
front 116 Superficial Veins: | back 116
|
front 117 Deep Veins | back 117
|
front 118 Perforator Vein | back 118
|
front 119 Steps of normal venous flow include: | back 119
|
front 120 ___ ___ __ originates from the dysfunction of the venous valves. Valve dysfunction occurs when the one-way valves become damaged or weakened. This valve failure leads to blood pooling in the lower extremities, which increases venous pressure, a condition known as venous hypertension. | back 120 Chronic venous insufficiency (CVI) |
front 121 Persistent venous hypertension and pooling lead to various skin changes, including _____ and _____, as well as the ___ ___ ___ __, predisposing the skin to ulcerations | back 121 hyperpigmentation ; thickening ; breakdown of tissue integrity |
front 122 What conditions are the below factors a risk for?
| back 122 Risk factors for CVI and VLUs include |
front 123 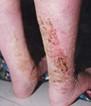 What condition is this image of? | back 123 Venous Dermatitis: Also known as “stasis dermatitis,” this dermatitis is a chronic, non-contagious skin inflammation in patients with CVI. It is often confused with cellulitis but is uniquely different, as it is not infectious. |
front 124 Management of Venous Dermatitis | back 124 Prompt detection and early intervention
|
front 125 If the patient has dermatitis/eczema, evidenced by increased pruritus, erythema and scaling | back 125
|
front 126 Cellulitis | back 126
|