Instructions for Side by Side Printing
- Print the notecards
- Fold each page in half along the solid vertical line
- Cut out the notecards by cutting along each horizontal dotted line
- Optional: Glue, tape or staple the ends of each notecard together
BMD 420 Module 4 (Chapter 10)
front 1 Blood main functions | back 1 Transport oxygen and nutrients, remove wastes, immune defense, maintain homeostasis |
front 2 Blood components | back 2 Plasma, erythrocytes, leukocytes, thrombocytes |
front 3 Arteries | back 3 Carry blood away from the heart |
front 4 Veins | back 4 Return blood to the heart |
front 5 Capillaries | back 5 Site of gas, nutrient, and waste exchange |
front 6 Blood cells formed in RED bone marrow | back 6 Hemocytoblast (early stem cell), Proerythroblast (RBC), Myeloblast (Granulocytic WBC), Lymphoblast (lymphocytes/agranulocytes), Monoblast (monocytes/agranulocytes), Megakaryoblast (thrombocytes/platelets) |
front 7 Erythrocyte characteristics | back 7 Biconcave flexible discs, no nucleus, glucose is the primary nutrient source, contains hemoglobin. Erythropoietin produced in the kidney stimulates erythrocyte production. Folic acid and Vitamin B12 are essential for RBC maturation. |
front 8 Breakdown of hemoglobin | back 8 1. Hemolysis of erythrocyte->Hemoglobin->Heme and Globin. 2. Heme->Iron that is recycled to bone marrow or stored->Hematopoiesis. 3. Heme->Bilirubin/unconjugated (transported bound to serum albumin)->Blood->Liver (conjugated with glucuronic acid)->Bilirubin/conjugated-> Bile 4. Globin-> Amino acids recycled |
front 9 Hemostasis steps | back 9 Vasoconstriction or vascular spasm after injury, platelet plug, coagulation fibrin mesh formation |
front 10 The Common Pathway of Clot Formation and Anticoagulant Drugs | back 10 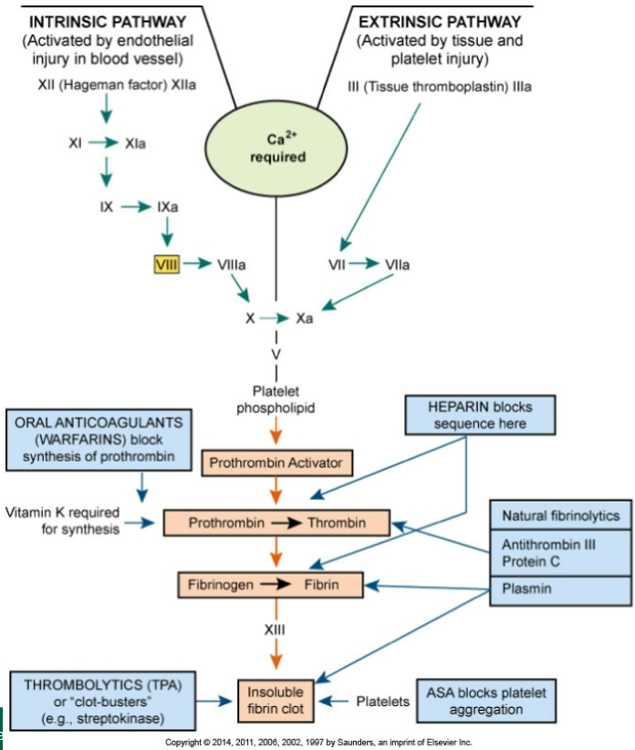 |
front 11 CBC test | back 11 Measures RBC, WBC, platelet counts hemoglobin and hematocrit. |
front 12 Leukocytosis | back 12 Increased WBCs associated with inflammation or infection |
front 13 Leukopenia | back 13 Decreased WBCs associated with some viral infections, radiation, chemotherapy |
front 14 Increased eosinophils | back 14 Common in allergic responses |
front 15 Types of diagnostic tests | back 15 Morphology (shows size, shape, uniformity, maturity of cells), Hematocrit (Percent by volume of cellular elements in blood), Hemoglobin (Amount of hemoglobin per unit volume of blood. Mean corpuscular volume (MCV) indicates the oxygen-carrying capacity of blood). |
front 16 Reticulocyte count | back 16 Indicates bone marrow production of RBCs |
front 17 Chemical analysis | back 17 Determines serum levels of components such as iron, vitamin B12, folic acid, cholesterol, urea, glucose |
front 18 Bleeding time | back 18 Measures platelet function |
front 19 PT and PTT | back 19 Tests measuring blood clotting factor function |
front 20 Whole blood, packed RBCs, packed platelets | back 20 For severe anemia or thrombocytopenia |
front 21 Plasma or colloid volume-expanding solutions | back 21 To maintain blood volume. Crystalloids (intravenous saline; increase intravascular and interstitial volume) and Colloid (contain glucose or hydroxyethyl starch to increase intravascular volume) |
front 22 Artificial blood products | back 22 O2 and CO2 transport. Compatible with all blood types. None of them can perform all the complex functions of normal whole blood |
front 23 Epoetin Alpha | back 23 Artificial form of erythropoietin. Boost RBC production. Before certain surgical procedures, anemia related to cancer, chronic renal failure |
front 24 Bone marrow or stem cell transplantation | back 24 Close tissue matches necessary. Treatment of some cancers, severe immunodeficiency, severe blood cell diseases |
front 25 Drug treatment | back 25 Aids in the clotting process |
front 26 Anemia general definition | back 26 Reduced oxygen transport due to low hemoglobin or RBCs |
front 27 In anemia oxygen deficit leads to what? | back 27 Less energy production, Compensation mechanisms (Tachycardia and vasoconstriction=Increased HR and BP), General signs of anemia (fatigue, pallor, dyspnea/shortness of breath), Decreased regeneration of epithelial cells, Angina and Congestive Heart Failure |
front 28 Iron deficiency anemia cause | back 28 Low iron from blood loss, poor intake, malabsorption, liver disease, which impairs hemoglobin synthesis. |
front 29 Iron deficiency RBC type | back 29 Microcytic (small) hypochromic (reduced hemoglobin content) erythrocytes |
front 30 Iron deficiency manifestations | back 30 Cold intolerance, irritability, fatigue, pallor, stomatitis/glossitis (inflammation of the mouth mucous membranes and tongue), tachycardia, syncope (fainting) |
front 31 Iron deficiency treatment | back 31 Iron replacement and treatment of underlying cause |
front 32 Pernicious anemia cause | back 32 Lack of intrinsic factor prevents vitamin B12 absorption possibly due to genetic factors and often accompanied by chronic gastritis |
front 33 Pernicious anemia RBC type | back 33 Large immature megaloblastic erythrocytes that carry less hemoglobin and have a shorter life span |
front 34 Pernicious anemia manifestations | back 34 Red enlarged sore smooth tongue, Paresthesia (tingling due to nerve damage), digestive discomfort (nausea and diarrhea) |
front 35 Pernicious anemia diagnosis | back 35 Microscopic examination (erythrocytes), Bone marrow examination (hyperactive), Low serum B12, hypochlorhydria/achlorhydria (low levels of stomach acid), gastric atrophy (stomach cells atrophy) |
front 36 Pernicious anemia treatment | back 36 Vitamin B12 replacement injections |
front 37 Aplastic anemia definition | back 37 Bone marrow failure causing pancytopenia (low levels of RBCs, WBCs, and platelets.) Normal appearing RBCs. |
front 38 Aplastic anemia causes | back 38 Often idiopathic but could be due to Myelotoxins (Radiation, chemicals, drugs), Viruses, Genetic disorders (Myelodysplastic syndrome and Fanconi's anemia) |
front 39 Aplastic anemia treatment | back 39 Removal of any bone marrow suppressants and supportive care bone marrow transplant |
front 40 Hemolytic anemia definition | back 40 Excessive destruction of red blood cells |
front 41 Hemolytic anemia causes | back 41 Immune reactions, changes in blood chemistry, infections, toxins, incompatible transfusion, genetic defects |
front 42 Sickle cell anemia cause | back 42 Genetic condition (Autosomal, incomplete dominance, homozygous recessive) Inherited abnormal hemoglobin HbS (Amino acid, Valine, is replacing glutamic acid on the Beta chain) |
front 43 Sickle cell crisis trigger | back 43 Low oxygen causes RBC sickling and vessel obstruction because they are too large to pass through microcirculation. |
front 44 Sickle cell complications | back 44 Infarctions (obstruction of blood flow), Hyperbilirubinemia, jaundice, gallstones (high rate of hemolysis) |
front 45 Sickle cell manifestations | back 45 Vascular occlusion/infarctions (lungs: acute chest syndrome and smaller blood vessels: Hand-foot syndrome), necrosis, ischemia, severe pain, Hyperbilirubinemia (Jaundice), splenomegaly (enlarged spleen), Congestive heart failure |
front 46 Sickle cell diagnosis | back 46 Hemoglobin electrophoresis, Blood test (abnormal RBC morphology), Prenatal DNA analysis |
front 47 Sickle cell treatment | back 47 Hydroxyurea, folic acid, immunizations, bone marrow transplant |
front 48 Thalassemia cause | back 48 Genetic defect (Autosomal dominant inheritance) reducing alpha or beta globin chains. Abnormal globin damages RBCs causing hemolysis (lower RBC numbers) and anemia |
front 49 Thalassemia manifestations | back 49 Pallor, tachycardia, vasoconstriction, increased hemolysis, impaired growth, hyperactivity in the bone marrow, and heart failure. |
front 50 Thalassemia diagnosis | back 50 Microcytic (small) hypochromic (reduced hemoglobin content) RBCs, increased erythropoietin, iron overload |
front 51 Thalassemia treatment | back 51 Blood transfusions, iron chelation (removes excess iron), bone marrow transplant |
front 52 Primary polycythemia | back 52 Neoplastic bone marrow disorder causing excessive RBC production with low erythropoietin |
front 53 Secondary polycythemia | back 53 Increased RBC production from chronic hypoxia with high erythropoietin |
front 54 Polycythemia manifestations | back 54 Thick sluggish blood, increased BP, thrombosis, hypertrophied heart, headaches, dyspnea (shortness of breath), splenomegaly, hepatomegaly, visual disturbances |
front 55 Polycythemia diagnostic tests | back 55 Tests to determine increased cell counts, increased hemoglobin and hematocrit, hypercellular bone marrow, hyperuricemia (elevated uric acid levels) |
front 56 Polycythemia treatment | back 56 Identify specific cause (Primary: low erythropoietin levels or secondary: elevated erythropoietin levels). Drugs or radiation, suppressions of bone marrow activity, periodic phlebotomy (bloodletting) |
front 57 Indications of blood clotting disorders | back 57 Bleeding from gums, epistaxis (nosebleed), hemarthrosis (joints), hematuria (feces), Hemoptysis (cough), and Hematemesis (vomit). Petechiae, purpura, anemia, low BP and rapid pulse. |
front 58 Hemophilia A cause | back 58 Inherited x-linked recessive trait (manifested in men and carried in woman) where there is a factor VIII deficiency. |
front 59 Hemophilia A manifestations | back 59 Prolonged bleeding, hemarthrosis (bleeding into joints), hematuria (blood in feces) |
front 60 Hemophilia A diagnostic tests | back 60 Normal PT and bleeding time, prolonged PTT, low serum levels of factor VIII |
front 61 Hemophilia A treatment | back 61 Factor VIII replacement, desmopressin |
front 62 Petechiae | back 62 Small pinpoint hemorrhages under skin |
front 63 Purpura | back 63 Medium sized bleeding spots in skin |
front 64 Ecchymosis | back 64 Large bruising from bleeding into tissue |
front 65 Von Willebrand's Disease cause | back 65 Most common hereditary clotting disorder. Type 1: most common (85% of cases), mildest form, low levels of VWF and factor VIII. Type 2: normal amounts of VWF, but non-functional; 4 subtypes (A: wrong size, B: attaches at the wrong time, M: doesn't attach to platelets, N: cannot attach to factor VIII) |
front 66 Von Willebrand's Disease manifestations | back 66 Skin rashes, frequent nosebleeds, easy bruising, bleeding of gums, abnormal menstrual bleeding, longer than normal bleeding |
front 67 Von Willebrand's Disease Treatment | back 67 Desmopressin Acetate (mild forms/type 1) and Factor replacement therapy (more serious forms/type 2&3) |
front 68 Disseminated intravascular coagulation definition | back 68 Excessive bleeding and clotting and consume clotting factors causing both thrombosis and severe bleeding |
front 69 DIC causes | back 69 Septicemia, childbirth complications, severe burns, trauma |
front 70 DIC manifestations | back 70 Ischemia, infarctions, excessive bleeding and hemorrhage, organ failure |
front 71 DIC treatment | back 71 Treat underlying cause replace clotting factors supportive care |
front 72 Thrombophilia | back 72 Group of inherited or acquired disorders. Risk of abnormal clots in veins or arteries. Blood testing for clotting factor levels and abnormal antibody levels. Causative condition should be treated. |
front 73 Leukemia definition | back 73 Malignant proliferation of abnormal white blood cells in bone marrow |
front 74 Leukemia pathophysiology | back 74 Immature nonfunctional leukocytes crowd out normal blood cell production |
front 75 Acute leukemia characteristics | back 75 Rapid onset many immature blast cells severe symptoms common in children |
front 76 Chronic leukemia characteristics | back 76 Slow onset more mature cells milder symptoms common in older adults |
front 77 Leukemia manifestations | back 77 Frequent infections, anemia, bleeding, bone pain, enlarged spleen liver lymph nodes |
front 78 Leukemia complications | back 78 Opportunistic infections, sepsis, congestive heart failure, hemorrhage, liver and renal failure, CNS depression and coma |
front 79 Leukemia diagnosis | back 79 Blood smear abnormal leukocytes bone marrow biopsy confirmation |
front 80 Leukemia treatment | back 80 Chemotherapy, biological therapy, stem cell transplant |
front 81 Arteriosclerosis | back 81 General term for arterial thickening loss of elasticity, lumen narrowing, and increased BP |
front 82 Atherosclerosis | back 82 Plaque formation of lipids calcium and clots in large arteries. Related to diet, exercise, and stress |
front 83 LDL role in atherosclerosis | back 83 Transports cholesterol to tissues promotes plaque formation |
front 84 HDL role in atherosclerosis | back 84 Removes cholesterol from tissues and carries it to liver where it is catabolized and excreted |
front 85 Nonmodifiable atherosclerosis risks | back 85 Age, sex, genetic factors |
front 86 Modifiable atherosclerosis risks | back 86 Smoking, obesity, sedentary lifestyle, diabetes, hypertension |
front 87 Atherosclerosis treatment (no cure) | back 87 Weight loss, exercise, diet, reduce Na+ intake, control hypertension, stop smoking, antilipidemic drugs (lowers LDL levels), surgical intervention |
front 88 Peripheral arterial disease definition | back 88 Atherosclerosis in arteries outside the heart causing reduced blood flow |
front 89 Peripheral arterial disease symptom | back 89 Intermittent claudication (leg pain) during exercise due to ischemia |
front 90 Peripheral arterial disease signs | back 90 Weak pulses, numbness, pale, or cyanotic skin, dry, hairless skin |
front 91 Peripheral arterial disease treatment | back 91 Smoking cessation, exercise, control diabetes, reduce cholesterol, anticoagulants |
front 92 Aneurysm definition | back 92 Localized dilation and weakening of arterial wall |
front 93 Aneurysm types | back 93 Saccular (bulging wall on the side), fusiform (Circumferential dilation along a section of artery), and dissecting (develops when there is a tear in the intima of the wall and blood continues to dissect or separate tissues) |
front 94 Aneurysm cause | back 94 Atherosclerosis, trauma, syphilis, congenital (present from birth) defects |
front 95 Aneurysm manifestations | back 95 Murmurs may be heard on auscultation, pulse felt on palpation of abdomen, frequently asymptomatic until it ruptures |
front 96 Aneurysm diagnosis | back 96 Ultrasound, CT, MRI, radiography |
front 97 Aneurysm treatment | back 97 Blood pressure control, surgical repair, avoid strain |
front 98 Varicose veins | back 98 Dilated tortuous superficial veins from valve weakness and venous pressure |
front 99 Varicose vein treatment | back 99 Elevation compression stockings avoid prolonged standing |
front 100 Thrombophlebitis | back 100 Thrombus formation in inflamed vein (IV site) |
front 101 Phlebothrombosis | back 101 Thrombus formation without prior inflammation loosely attached |
front 102 Venous thrombosis manifestations | back 102 Often unnoticed, Aching, burning, tenderness, fever, malaise, leukocytosis (high WBC count) |
front 103 Major complication venous thrombosis | back 103 Pulmonary embolism |
front 104 Venous thrombosis treatment | back 104 Anticoagulants, exercise, leg elevation, surgery if needed |