Instructions for Side by Side Printing
- Print the notecards
- Fold each page in half along the solid vertical line
- Cut out the notecards by cutting along each horizontal dotted line
- Optional: Glue, tape or staple the ends of each notecard together
Unit 10 TDM and Toxicology
front 1 Define ED50 | back 1 The dose of a medication which will have the intended effect for 50% of the population |
front 2 Define TD50 | back 2 The dose which will cause toxic symptoms in 50% of the population |
front 3 Define LD50 | back 3 The dose which is lethal in 50% of the population |
front 4 What is used to metabolize toxicants that our bodies can't get rid of? | back 4 Cytochrome P450 Oxidase enzymes (CYP450) |
front 5 How do CYP450 enzymes work? | back 5 Phase I - Oxidizing or reducing a compound |
front 6 Define Vd | back 6 Volume of distribution, tells how widely the substance is spread throughout your body |
front 7 Define elimination constant | back 7 How much of a substance you get rid of in a specific amount of time |
front 8 Define Half-life | back 8 How long it takes for the plasma concentration to decrease by half |
front 9 Define qualitative testing | back 9 The test gives you a result which is positive or negative |
front 10 Define quantitative testing | back 10 The test gives you a numerical value as a result |
front 11 Why does CO cause shortness of breath and death? | back 11 Because it displaces oxygen on our hemoglobin and holds on tightly so that we can no longer transport oxygen in our blood |
front 12 What is the treatment for CO poisoning? | back 12 100% oxygen |
front 13 What are common symptoms of carbon monoxide poisoning? | back 13 Red face, headache, shortness of breath |
front 14 Where does cyanide have it's primary pathologic effect on the body? | back 14 The heart and the brain |
front 15 What life-sustaining process does cyanide interrupt? | back 15 Oxidative phosphorylation (i.e. the ability for oxygen to accept electrons in the electron transport chain). Results in tissue death, seizures, and coma. |
front 16 What source can provide arsenic and cyanide exposure? | back 16 Open flames in an enclosed space |
front 17 What factors will affect drug absorption? | back 17 So many. Primarily gastrointestinal motility, acidity of the drug, gastric acidity, |
front 18 Describe peak drug assessment | back 18 This is when a drug is measured after 1-4 hours and is considered to be completely absorbed, reaching it's peak concentration |
front 19 Describe trough drug assessment | back 19 this is when a drug is measured immediately prior to the next dose, at theoretically the lowest concentration |
front 20 Define First order elimination | back 20 A constant percentage of substance is eliminated over time |
front 21 Define zero order elimination | back 21 A constant amount of substance is eliminated over time |
front 22 Name a commonly-abused substance with zero-order elimination | back 22 alcohol |
front 23 How many doses of a drug does it take to reach a stable steady state concentration? | back 23 5 |
front 24 What is a steady state? | back 24 When the drug intake equals drug excretion |
front 25 Define pharmacodynamics | back 25 What the drug does to the body |
front 26 Define pharmacokinetics | back 26 What the body does to the drug |
front 27 What are the common side effects for excess Digoxin levels? | back 27 Nausea, vomiting, cardiac arrhythmias note: is a cardiac glycoside used to improve cardiac contraction in patients with congestive heart failure. Side effects of increased concentrations (>3 ng/mL) include nausea, vomiting, premature ventricular contractions (PVCs), and atrioventricular node blockade. |
front 28 What are the common side effects for excess Quinidine levels? | back 28 Nausea, vomiting, tinnitus, thrombocytopenia, and cardiac arrhythmias note :is a drug used to treat cardiac arrhythmias. It is generally administered as a slowly-absorbed oral pill. Trough levels are assessed. Toxicity begins at twice the upper limit of the therapeutic range. Side effects include nausea, vomiting, tinnitus, thrombocytopenia, and PVCs. |
front 29 What are the two commonly assessed cardiac drugs for TDM? | back 29 Digoxin and Quinidine |
front 30 What are the two commonly assessed antibiotic drugs for TDM? | back 30 Aminoglycosides and Vancomycin |
front 31 What are the common side effects for excess Aminoglycoside levels? | back 31 Nephrotoxicity and Ototoxicity note:are a group of antibiotics used to treat
gram-negative bacterial infections. |
front 32 What are the common side effects for excess Vancomycin levels? | back 32 Nephrotoxicity, otoxicity, and Red Man Syndrome note: is at the pinnacle of antibiotics and one of the kingpins that we use to treat the “untreatable” infections. It is administered intravenously and can cause “red man syndrome” (erythema or the whole body), Nephrotoxicity, and Ototoxicity. Same as the aminoglycosides, but just add that it causes the cool red man syndrome thing and you’re good. |
front 33 What are the common side effects for excess Phenytoin levels? | back 33 Hirsuitism, gingival hyperplasia, vitamin D deficiency, folate deficiency note: is an anti-seizure, Anti-Epileptics, drug and used in brain injury to prevent further loss of functional tissue. Seizures can occur in sub-therapeutic or supratherapeutic doses. Other side effects include hirsutism (become a hairy man beast like bigfoot), gingival hyperplasia, vitamin D deficiency, and folate deficiency. |
front 34 What are the common side effects for excess Carbamazepine levels? | back 34 Rashes, nausea, vertigo, and a deadly leukopenia note: is an effective anti-seizure drug, but is only used in refractory cases that do not respond to other antiepileptic drugs. Side effects can include rashes, nausea, vertigo, and the most serious is the deadly leukopenia. |
front 35 What are the common side effects for excess Ethosuximide levels? | back 35 Used for absence seizures Causes nausea, vomiting, anorexia, dizziness, lethargy note: is used for controlling petit mal seizures.
These are the seizures that don’t |
front 36 What are the three anti-epileptic drugs commonly assessed for TDM? | back 36 Phenytoin, Carbamaepine, and Ethosuximide |
front 37 What are the three antidepressant drugs commonly assessed for TDM? | back 37 Lithium, Tricyclic antidepressants, and clozapine |
front 38 What are the common side effects for excess Lithium levels? | back 38 Anemia, renal impairment, apathy, lethargy, hypothyroidism, seizures note: is a common mood-altering medication used for bipolar disorder. Lithium has a half-life of 10-35 hours and has a narrow therapeutic index, meaning that side effects present just above the effective concentration. These include apathy, lethargy, renal impairment, hypothyroidism, and seizures. |
front 39 What are the common side effects for excess Tricyclic antidepressant (TCAs) levels? | back 39 Seizures, arrhythmias, and loss of consciousness note: are used to treat depression, and the most pertinent ones are imipramine, amitriptyline, and doxepin. TCAs hang out in the body a VERY long time; half-life of 17-40 hours. Side effects include seizures, arrhythmias, and loss of consciousness. |
front 40 What are the common side effects for excess Clozapine levels? | back 40 Seizures note: is a drug used in refractory schizophrenia as an antipsychotic. Excess dosing can result in seizures. |
front 41 What are the common side effects for excess Cyclosporine and tacrolimus levels? | back 41 renal dysfunction note:is an immunosuppressive agent used to prevent host-versus-graft
rejection. note: is another oral immunosuppressive agent but it is 100 times more potent . Although it is still effective at lower concentrations, It's toxicity still results in renal dysfunction |
front 42 What are the common side effects for excess methotrexate (MTX) levels? | back 42 inhibits DNA synthesis in all cells note: This works well for cancer, because those cells are rapidly dividing and they will take more MTX and suffer more. The peak concentrations are measured 1 hour after the dose is given orally. Side effects will include a cytotoxic effect to most cells in the body. We have a procedure to halt the MTX effect on our cells called leucovorin rescue, where we basically infuse the patient with folic acid which effectively stops the deadly action of MTX on our cells. |
front 43 What is the procedure to halt methotrexate's effect on our healthy cells when we give it to patients with cancer? | back 43 leukovorin rescue |
front 44 What are the three Immunosuppressant drugs commonly assessed for TDM? | back 44 Cyclosporine, tacrolimus, methotrexate |
front 45 What is a bronchodilator that is commonly assessed for TDM? | back 45 Theophylline |
front 46 What are the symptoms of Theophylline toxicity? | back 46 Seizures note: is an older drug, but shows up with high frequency on standardized exams. It is used to dilate the bronchial passages to alleviate respiratory problems, but can cause seizures. Since the advent of inhaled glucocorticoids, It is rarely used anymore. |
front 47 Two 60 kg patients are given 1 gram of different drugs and after 1 hour, the serum concentration of Drug A is 10 mg/dL and Drug B is 20 ug/mL. What drug has a greater volume of distribution? | back 47 Drug B is the correct answer. This problem actually has two
challenges to be overcome, the first is units, the second is Vd .
Let’s get everything to the same units first.10 mg/dL = 0.1 g/L 20
ug/mL = 0.02 g/L The Vd for Drug A is 1 g (administered drug) / 0.1
g/L (plasma concentration) = 10 L The Vd |
front 48 A 45-year-old female is status-post left hemicolectomy (excision of her colon from the splenic flexure to the cecum). She is given morphine for the pain, which will further decrease her gastrointestinal motility, how will her GI motility affect the absorption of drugs into her body? | back 48 The decrease in GI motility will increase the absorption of morphine into her bloodstream. |
front 49 How many doses of a drug does it take to reach a stable steady-state | back 49 5, isn’t this interesting that it takes 5 half-lives for a drug to effectively be eliminated from the body and it takes 5 dosages to reach a stable steady-state concentration. This is assuming that the patient took all 5 doses at the proper times though, which may or may not happen. |
front 50 Grandpa’s cough medicine was too strong for grandpa, but mom socked back a few glasses to cure her cough. It didn’t really cure her cough, but she had a blood alcohol content of 0.15%, above the legal limit in Utah. How would the liquor be eliminated from mom’s body? | back 50 Zero order elimination. It would be eliminated at a constant rate of 0.01 g ETOH / 100 mL blood / 1 hour in a person who has not chronically abused alcohol and developed a tolerance to it. In patients who develop an alcohol tolerance, this rate can increase to as fast as 0.06 g ETOH / 100 mL blood/ 1 hour ... that’s a 6-fold increase! Holy Batman! |
front 51 A 68-year-old male with chronic renal failure has a GFR of 12 mL/min.
How will | back 51 The decrease in GFR will lead to a decrease in the elimination of the drug. His serum Digoxin levels should stay between 0.8 - 2 ng/mL in the serum. Higher levels will predispose him to some fairly daunting cardiac problems, including premature ventricular contractions and AV node blockages. |
front 52 What two drugs will cause nephrotoxicity and ototoxicity? | back 52 Aminoglycosides and Vancomycin |
front 53 Laura, an 18-year-old female who is a non-drinker was tricked at a party and told that she was being given a “virgin” daiquiri. While everyone else is laughing and snickering, Laura asks for another one and ends up passing out. Why was she so affected by the alcohol when others at the party had way more than two drinks? | back 53 The answer comes from the metabolism of alcohol. She only had the action of alcohol dehydrogenase to metabolize the liquor. The CYP450 enzymes in the liver can be induced, which were likely present in higher quantities in her friends who probably drink often. She will likely have a hangover in the morning as well, and will probably choose new friends after the glorious experience of repeatedly puking after she wakes up. |
front 54 What do steroid hormones do to affect cellular function? | back 54 Steroids bind to intranuclear receptors and cause transcription of DNA into RNA. This allows for proteins to be made from the RNA via translation. Because steroids start a cellular process inside the nucleus, they do NOT have immediate activity |
front 55 What metabolite of cocaine do you screen for with an immunoassay? | back 55 Benzoylecgonine |
front 56 An immunoassay is positive codeine for an 18-year-old young man. He says that he had been taking oxycodone prescribed by his physician. Is this possible? | back 56 Theoretically, yes because oxycodone and codeine do cross react in the screening immunoassay, just at very low rates. The likelihood of this scenario being true is NOT high. He most likely just found, bought, or somehow procured codeine pills, but it probably was NOT oxycodone that caused a positive immunoassay for codeine. |
front 57 Acetaminophen (Tylenol) doesn’t kill you immediately, it depletes what substance in your liver that scavenges for reactive oxygen species? | back 57 Glutathione, this substance generally takes care of all free
radicals |
front 58 What is the toxic substance produced by Tylenol metabolism in the liver? | back 58 N-acetyl-p-benzoquinoneimine |
front 59 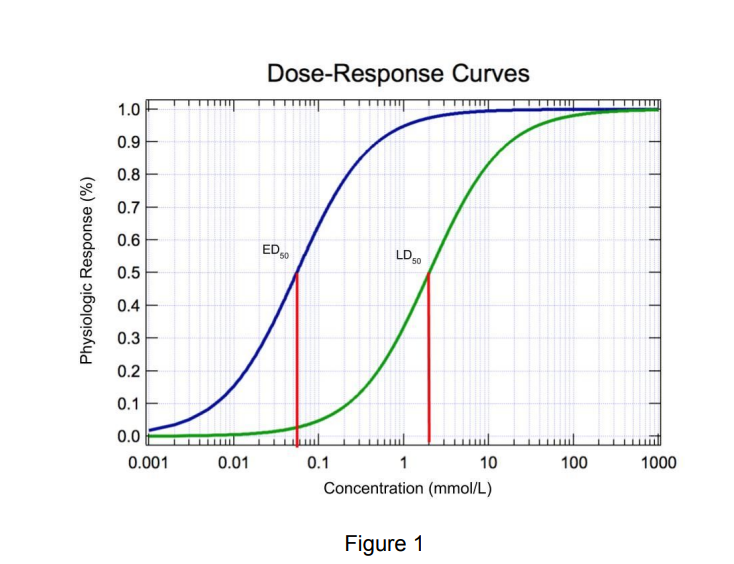 Where does the Toxic dose fit into the dose response curves? | back 59 The toxic dose curve fits between the effective dose curve and the lethal dose curve which makes sense because you would expect to feel sick from a substance before you die from your exposure to it. That’s not always the case,nbut a good rule of thumb. |
front 60 A lipophilic drug like Theophylline has a very high Vd . What would a CYP450 enzyme do to improve excretion? | back 60 CYP450 enzymes would likely conjugate the drug to an ion to make it water soluble and readily excreted in the urine. |
front 61 Your cousin Ed is driving drunk, and the cop pulls him over and gives him a breathalyzer test. Is this a quantitative or qualitative test? | back 61 Quantitative, because it gives you a number! 0.08% is drunk driving in Utah! An easy way to tell if the test is a quantitative test is that you’ll get a number whereas you will get either a (+) or a (-) on a qualitative test. Think breathalyzer for quantitative and pregnancy test for qualitative. |
front 62 You have a 48-year-old white male who lives alone in the Rocky
Mountains presents to the ER after the largest snowstorm that the
region has seen in over 30 years. His face is very red, and many
people think that he looks like Santa with his rosy cheeks. He has
been complaining of a very bad headache for the past few days. Upon
questioning, he reveals that in order to keep warm, he is | back 62 CO poisoning is the most likely cause of this patient’s headache and red complexion. This is commonly seen in patients with old propane heaters in poorly-ventilated areas of their home. Some people also get CO poisoning by running their car engine in their garage with the garage door closed. If there is a flame source with inadequate ventilation, CO could be the cause. |
front 63 How does carbon monoxide displace oxygen from hemoglobin? | back 63 CO binds hemoglobin 200 times stronger than oxygen does. The
CO |
front 64 A 34-year-old female presents to the ER with generalized weakness, headache, and abdominal pain. Without asking for her history, big mistake, the physician just goes ahead and orders a blood cyanide level. What are the possible sources of exposure for this poison? | back 64 The cause of this patient’s symptoms would likely become clear upon
collecting a quick history from the patient. Intentional poisoning for
suicide is occasionally seen, however smoke inhalation is by far the
most common cause for harmful cyanide exposure. Workers in the metal
trades (especially electroplating), mining, jewelry making,
photography, and agriculture can have significant
industrial |