Instructions for Side by Side Printing
- Print the notecards
- Fold each page in half along the solid vertical line
- Cut out the notecards by cutting along each horizontal dotted line
- Optional: Glue, tape or staple the ends of each notecard together
Unit 7: Proteins and other Nitrogen-Containing Compounds
front 1 What is the full medical breakdown for: 40-year-old Female with a history of valvular heart disease presents for a physical. She has been feeling tired recently and can't exercise. Her prosthetic valve is beginning to malfunction | back 1 Test: Serum BUN/Creatinine Sample: Plasma or Serum (preferably transported separated from the erythrocytes) Method: Quantitative Spectrophotometry
Result: BUN 84 mg/dL Creatinine 1.8 mg/dL Reference
Range Disease or Condition: Valvular Regurgitation (Prerenal Azotemia) |
front 2 What is the full medical breakdown for:72-year-old Male
who | back 2 Test: Serum BUN/Creatinine Sample: Plasma or Serum (preferably transported separated from the erythrocytes) Method: Quantitative Spectrophotometry
Result: BUN 57 mg/dL Creatinine 5.8 mg/dL Reference
Range Disease or Condition: Transitional Cell Carcinoma of the Bladder (Postrenal Azotemia) |
front 3 What is the full medical breakdown for: 28-year-old Female with
a | back 3 Test: Serum Protein Electrophoresis Sample: Serum Method: Quantitative Capillary Electrophoresis Result: Elevated a1 and a2 bands Disease or Condition: Acute Phase Reaction |
front 4 What is the full medical breakdown for: 47-year-old Male with
a | back 4 Test: Serum Albumin Sample: Serum Method: Quantitative Spectrophotometry Result: 2.8 g/dL Reference Range (3.5-5.0 g/dL) Disease or Condition: Cirrhosis after a Fasciola hepatica infection |
front 5 What is the full medical breakdown for: 53-year-old Male
presents | back 5 Test: Synovial Fluid Uric Acid Sample: Synovial Fluid from a joint aspirate Method: Quantitative Spectrophotometry Result: 7.2 mg/dL Reference Range (No Reference Range in Synovial fluid) Disease or Condition: Gout |
front 6 What is the full medical breakdown for: 6-year-old girl is
being | back 6 Test: Serum Uric Acid Sample: Serum Method: Quantitative Spectrophotometry Result: 9.3 mg/dL Reference Range (2.5-6.1 mg/dL) Disease or Condition: Tumor Lysis Syndrome |
front 7 A 3-day old baby boy is brought in by his parents for his newborn screening. The physician takes a whiff and says that this child smells “mousy”. What disease does this child likely have based on the smell? | back 7 If you see the phrase “mousy odor” on the registry exam, they
are |
front 8 What is the cure for PKU? | back 8 A phenylalanine-restricted diet, rich in grains, fruits, and vegetables, and low in meats, eggs, cheese, and milk. |
front 9 What enzyme is deficient in tyrosinemia type I? | back 9 Fumarylacetoacetate hydrolase |
front 10 What is the tell-tale sign that a patient has alkaptonuria? | back 10 Dark brown or black urine |
front 11 What are the three branched chain amino acids? | back 11 Leucine, Isoleucine, and Valine |
front 12 If your cousin from Qatar, has a downward dislocation of the lens in his eye, what disease do you think that he could have? | back 12 Homocystinuria |
front 13 What is the deficient enzyme found in cystinuria? | back 13 None. Remember, it is caused by a deficient transporter protein which allows for cystine reabsorption by the kidney. |
front 14 An 11-year-old female presents to her pediatrician with the CBS
mutation, and she was properly screened with the Guthrie test. She is
being adequately treated with vitamin B6 . She comes in complaining
that she can’t see well out of one eye. This started suddenly this
morning. What is the most likely clinical effect? | back 14 The correct answer is A) This fact is the most likely to be tested
clinical nuance that will give the answer away every time. It’s just
screaming at you that this patient has homocystinuria. The most common
mutation is the CBS gene, screened with the Guthrie test using
L-methionine sulfoximine to inhibit bacterial growth, but the
increased level of methionine in the sample will still allow for the
bugs to grow. If you have growth on a Guthrie test, that is positive!
The treatment of vitamin B6 |
front 15 A pregnant mother is admitted to the hospital to deliver her first baby. Upon delivery, the doctors take a few samples for newborn testing for rare diseases that are easily treatable. This baby has an increased level of branched chain amino acids in her blood. What is the name of this rare metabolic deficiency? A. Alkaptonuria | back 15 The correct answer is C) The hallmark of this disease is that there is an elevated level of branched chain amino acids, which are leucine, isoleucine, and valine. The deficient enzyme is BCKD. Treatment is a BCAA-restricted diet. |
front 16 A 35-year-old male immigrant from Ghana is found mumbling to himself
on the streets of San Francisco. It is discovered that he is married
to a Ghanaian woman with two kids, and he lives in Boston. He doesn’t
know how he got to San Francisco. He has no health records here in
America, but after talking to his wife on the phone, the physician
discovers that they moved here 1 year ago because her husband was able
to land a job here. Before they moved, they were A. Alkaptonuria | back 16 The correct answer is D) This man was likely never screened in Ghana, but was inadvertently adhering to a phenylalanine-restricted diet by eating only vegetarian food. This all changed once he and his family were introduced to the wonders of American table trash and had the means to procure it. PKU is the most common inherited aminoacidopathy in America, occuring about 1 in 15,000 births (He is an immigrant, so this statistic wouldn’t apply to him). The deficient enzyme is phenylalanine hydroxylase and the gene is PAH. Screening for PKU now occurs across the country equally. Screening is performed by a Guthrie test using |
front 17 A 49-year-old female has nonalcoholic steatohepatitis and a very reduced capacity to synthesize proteins. What clinical issues would you expect? | back 17 Ascites and edema. This is a case where the synthetic capacity of
the |
front 18 What structures of a protein will be affected by Alanine Aminotransferase (ALT), with the addition of an alanine? | back 18 Short answer is it depends. The longer answer is that it depends on where the alanine is added. If it is added to the end of the polypeptide chain, then it would change the primary structure, which would likely affect the secondary, tertiary, and quaternary structures. If the alanine is added to an amino acid side chain, then it will likely affect tertiary and quaternary structures |
front 19 What is the protein assay method principle and use for: Kjeldahl | back 19 Principle: Protein digestion assay, measures released Nitrogen Use: Reference method |
front 20 What is the protein assay method principle and use for: Biuret | back 20 Principle: Cu 2+ and peptide bonds create a purple color Use: Routine method; performed in an alkaline medium |
front 21 What is the protein assay method principle and use for: Dye Binding | back 21 Principle: Dye binds to the protein which causes a shift in the absorbance of the dye Use: Used for research |
front 22 What are the two classifications of testing that are performed to assess protein in a serum sample? | back 22 BUN and Serum Total Protein |
front 23 A 35-year-old patient is found to have a diet deficient in Tyrosine. What metabolic deficits will likely present? | back 23 None! It is considered a nonessential amino acid and can be synthesized from phenylalanine. Of note, It is an amino acid which is richly used in adrenal medullary hormones (e.g. epinephrine, norepinephrine, dopamine) and thyroid hormone. All of hormones that stimulate activity in the body. |
front 24 A 21-year-old nonalcoholic female presents to their physician with vague abdominal pain and difficulty breathing. She is diagnosed with cirrhosis and emphysema. What is the likely enzyme deficiency that she is suffering from? | back 24 α1-antitrypsin |
front 25 A 35-year-old female presents to her physician after a long,
strenuous hike through the mountains. She has low blood pressure and
is diagnosed with mild dehydration. Protein concentration would be
increased. What is the routine method for protein identification and A. Kjeldahl method | back 25 The correct answer is B) Remember, this method is the routine one that it is used in everyday laboratory testing. This uses Cu 2+ , which binds to peptide bonds and creates a purple color. The color change is measured at 540 nm. |
front 26 A 19-year-old male cocaine abuser has just injected himself with a
double hit of cocaine. His heart starts to race and he is sweating
while sitting still. He begins breathing quickly and feels great! His
friends, who were against him shooting up in the first place, notice
that he has become too agitated and hyperthermic so they take him to
the hospital where initial laboratory tests show a significant
metabolic acidosis and pH of 7.2. What level of protein structure
would A. Primary structure | back 26 The correct answer is A) This is the only structure that would likely NOT be denatured. B) is formed by weak bonds and would likely be the first to disintegrate. One could argue that C) would also likely NOT be denatured because they are covalently-bonded side chains. What I wanted to get you to understand is that the Primary structure is the hardest one to break down. D) would likely be different because if the secondary structure is changed, then the proteins would likely NOT fit as well as they are supposed to. |
front 27 A 48-year-old male presents to the ED complaining of vague abdominal
pain and he can’t stop the bleeding from minor cuts. He has also been
feeling numbness and tingling in his arms B.α 2 C. β D.γ | back 27 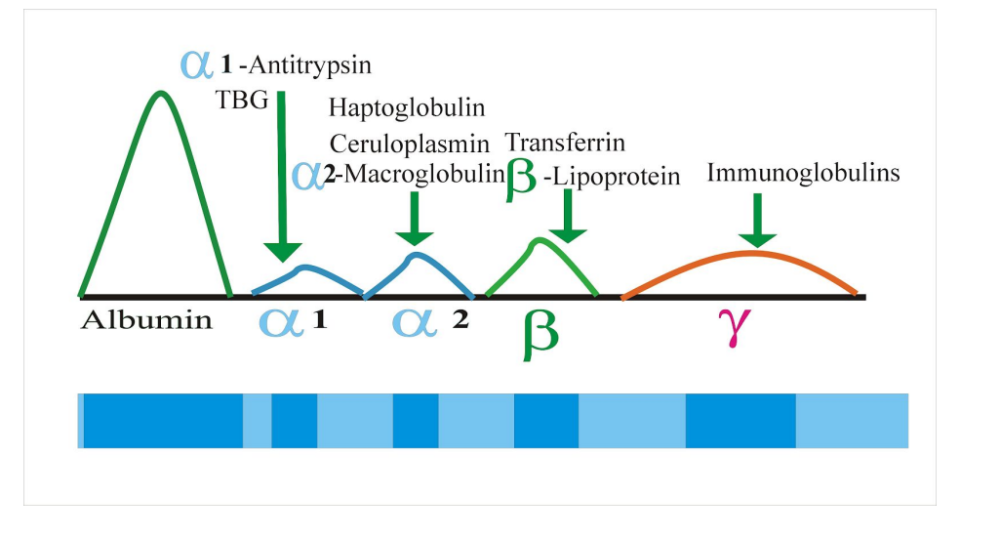 The correct answer is A) It would be increased because of the presence of Ceruloplasmin, the copper transport protein. This patient likely has Wilson’s disease, a genetic defect in the body’s ability to metabolize copper, causing it to be deposited everywhere. This results in cirrhosis and occasionally neurologic effects as we |
front 28 What is uric acid created from? | back 28 DNA degradation, adenine and guanine |
front 29 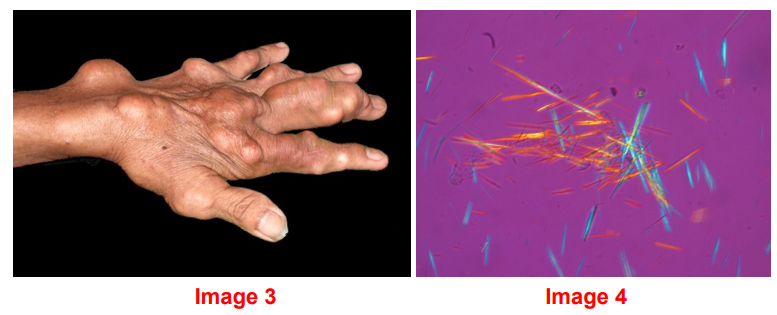 A 54-year-old male presents with severe flank pain and a tophus on his right foot (see image 3). What stereotypical finding would you see under the microscope? | back 29 Negatively birefringent crystals. This means that if you’re looking
with |
front 30 A patient with Acute Lymphoblastic Leukemia is being treated with the chemotherapeutic agent 6-mercaptopurine which stops purine synthesis. What effect will this have on the patient’s plasma uric acid level? | back 30 The patient will likely have hypouricemia 0.6 - 1.1 mg/dL |
front 31 What sample should be received if the ordering physician desires ammonia testing on his patient? | back 31 An EDTA or Heparin tube on ice. The plasma should be immediately separated from the red cells and assayed or stored |
front 32 What is the substance that causes neuronal destruction in hepatic | back 32 Ammonia (NH3) |
front 33 A 47-year-old female gardener, has had to stop wearing gloves because
her hands don’t fit or move around comfortably in them. She has
noticed that when she lies in bed at night, sometimes the weight of
just the bedsheet is unbearable on her great toe. Physical
examination, reveals a red, swollen right metatarsophalangeal joint
and tophaceous deposits on her ears. What non-protein nitrogen would
you expect to see elevated in this case? | back 33 the correct answer is D) This patient has gout and the podagra described (gouty tophi over the metatarsophalangeal joint), is typical of gouty arthritis. Even the weight of a bedsheet, can send these patients off the edge. |
front 34 A 53-year-old male presents to the ED after eating a delicious meal at a steakhouse and downing 4 beers. He has exquisite joint pain and can’t seem to move. His left foot hurts the worst. When the doctor asks him to rate his pain out of 10, he immediately yells 14! The patient also said that his left elbow and right wrist are both at 11. His physician is worried about diet-induced gout and decides to order a plasma uric acid level. What tube is NOT acceptable if we are using the uricase method to evaluate the uric acid concentration? A. EDTA | back 34 The correct answer is A) It binds to Ca2+ and chelates it, making it unavailable for assaying, but also unavailable for protein function. Ca 2+ is used as a cofactor for a bunch of enzymes that are involved in protein and uric acid degradation. Different labs require different samples. Some just say that they need plasma or serum from any tube. |
front 35 A 32-year-old male presents to his primary care physician because his
previously drawn ammonia level came back very elevated. He just got
over having a severe gastroenteritis where he had many bacteria
proliferating in his intestines. These bacteria broke down his
body’s | back 35 The correct answer is B) The point of this question is to help
you |
front 36 When preparing the Jaffe reagent, what must you be cautious of? | back 36 Picric acid is explosive, even crust that forms on the cap can
ignite |
front 37 What is the approximate reference range for creatinine in most labs across the country? | back 37 0.6 - 1.1 mg/dL |
front 38 How do you calculate the amount of creatinine that a patient has effectively eliminated from their blood in 24 hours? | back 38
We have a few
equations to be able to do this: The next one to know would be the equation for estimated GFR or the Cockroft-Gault Formula GFR = [(140-Age) x weight (kg)] / [72 x SCr] |
front 39 What is the creatinine clearance if 72-year-old 60 kg male had a serum creatinine of 5.3 mg/dL? | back 39 10.7 mL/min. This man is in severe renal failure and is probably in line for his weekly dialysis appointment, or at least he should be. The next one to know would be the equation for estimated GFR or the Cockroft-Gault Formula GFR = [(140-Age) x weight (kg)] / [72 x SCr] |
front 40 How do we calculate the BUN concentration from a urea concentration? | back 40 Divide the urea concentration by 2.14. This is easy to remember which one is bigger because urea is the large molecule, and BUN stands for Blood Urea Nitrogen, so it’s obviously just looking for nitrogen. If you want to calculate the urea concentration, then you multiply BUN by 2.14. |
front 41 What is the likely etiology of a patient’s renal failure with a BUN of 70 mg/dL, and Creatinine of 1.5 | back 41 BUN:Cr ratio = 46. This is indicative of a prerenal etiology. The most common being something to cause a decreased amount of blood to flow through the kidneys. This would include dehydration, shock, congestive heart failure, or anything else the leads to a decrease in circulating blood volume |
front 42 A 72-year-old male has a heart attack and is recovering slowly in the hospital. Two hours after the embolus is removed from his left anterior descending coronary artery, he has flank pain and the physicians are worried about renal damage from hypoperfusion of the kidney. What values would you expect to see if the patient had a prerenal azotemia? A. BUN >80 mg/dL | back 42 The correct answer is C). This would be a definitive laboratory finding of prerenal azotemia. If the ratio is >20, then that’s just suggestive, but over 40 is definitive. The reason why this happens is because Creatinine is much more dependent on the glomerular filtration rate, rather than kidney function. As long as the kidneys are being perfused at 50% capacity, the creatinine value doesn’t increase. Prerenalazotemia can be caused by renal hypoperfusion; which can be caused by dehydration, renal vasoconstriction, or a myocardial infarction. This causes activation of the renin-angiotensin-aldosterone system, antidiuretic hormone, and sympathetic nerve signals to increase reabsorption of water, salt, BUN, and creatinine so that the kidney can be adequately perfused. BUN is reabsorbed at a MUCH greater rate than creatinine, thereby causing the drastic increase in BUN. A) Bun >80 mg/dL can occur in this clinical situation, but the big point is that the creatinine would be normal or slightly elevated, making answer A. the most correct. B) Cr >8.2 mg/dL would show up in chronic, renal failure. These patients are possibly dialysis dependent. D) Cystatin C is an analyte which is completely filtered by the glomeruli and is constantly produced by all nucleated cells. It is NOT secreted in the PCT, but it does have some clinical situations which confound analysis … just like creatinine |
front 43 A 53-year-old male triathlete is complaining of always having a full bladder. He can’t quite seem to urinate very easily. It takes him approximately 2-3 minutes before he can get a stream of urine. He is diagnosed with benign prostatic hypertrophy by a digital rectal exam. A Kidney-Ureter-Bladder radiograph is ordered. The resulting scan shows hydronephrosis. What would be this patient’s likely BUN and Creatinine findings? A. BUN 41 mg/dL Cr 1.2 mg/dL PSA 19 ng/mL (0-3.5
ng/mL) | back 43 The correct answer is A) The reason for this is because with
postrenal azotemia, your patients have a fairly normal BUN/Cr. This
normal ratio will remain until the backup of urine flows retrograde up
the ureters and into the kidneys, causing renal failure. The normal
BUN and |
front 44 12-year-old female presents to her physician after she was diagnosed
and treated for streptococcal pharyngitis. She had recovered with the
antibiotics, but two weeks later, she developed generalized edema, a
puffy face, and has frothy urine. Her urinalysis studies reveal
massive proteinuria, increased polymorphonucleocytes, and renal
epithelial cells. What would you expect her BUN and Creatinine to
be? | back 44 The correct answer is B) which shows that she is NOT in renal
failure, because her values are close to normal. She has a nephrotic
picture with urine positive for protein, PMNs, and renal epithelial
cells. We would expect her BUN and Creatinine values to be fairly
normal, because she presented to the physician right when these
symptoms started. So she likely doesn’t have any renal failure yet,
but we can look for other symptoms to give the answer away, then we
know A) BUN 10 mg/dL Creatinine 18.1 mg/dL is physiologically improbable. C. BUN 87 mg/dL Creatinine 4.3 mg/dL is a sign of renal failure, but is strange because the creatinine is elevated significantly higher than the BUN should be. This is likely caused by an increased production of creatinine, either via rhabdomyolysis (skeletal muscle destruction) or an increased intake of cooked meat D. BUN 117 mg/dL Creatinine 3.2 mg/dL is a sign of probable prerenal failure with the ratio at 36 |
front 45 What are the usual diagnostic findings in nephrotic syndrome ? | back 45 1. Proteinuria greater than 3-3.5 g/24 hour 2. No increased serum albumin <25 g/l 3. Clinical evidence of peripheral edema 4. Severe hyperlipidaemia (total cholesterol >380 mg/dL) is often present |
front 46 Where are most proteins are synthesized? | back 46 produced in the liver |
front 47 Where are Immunoglobulins synthesized? | back 47 produced by plasma cells |
front 48 Where are Hemoglobin synthesized? | back 48 produced in the RBC |
front 49 What protein has the smallest size to charge ratio? | back 49 Albumin note: Largest peak and migrates the fastest on electrophoresis |
front 50 What protein goes the opposite way and why? | back 50 Gammas are cations so they go the other way |
front 51 What is the reference range for total serum protein? | back 51 6.0 - 8.3 g/dL (may vary from lab to lab) |
front 52 What is the main function of albumin? | back 52 maintains oncotic pressure (colloidal osmotic pressure) |
front 53 What is the clinical significance of Albumin? | back 53 Increased catabolism - Physical injury Decreased synthesis - Primary (liver disease), Secondary (malabsorption, malnutrition) Increased loss - Renal protein loss |
front 54 What does deficiency of α antitrypsin cause? | back 54 emphysema and cirrhosis Note it is called antitrypsin because it destroys titrypsin and titrypsin destroyed proteins. |
front 55 What is the most common alpha protein? | back 55 AAT makes up 90%, most common, of the |
front 56 What is α1Acid Glycoprotein | back 56
|
front 57 What is Alpha-Fetoprotein? | back 57
|
front 58 What is α1 Antichymotrypsin | back 58 Serum protease inhibitor. Found between the A1 and A2 zones. |
front 59 What is Haptoglobin? | back 59 Acute Phase Reactant, binds hemoglobin, and is removed in the spleen. Haptoglobin prevents hemoglobin from being removed in the glomeruli. Increased in inflammation, intravascular hemolysis, and smoking positively associated with hemolytic anemia. M ore hemaglobin means for haptoglobin needs to be there to bind it. |
front 60 What is Ceruloplasmin? | back 60 Copper containing protein, oxidizes iron, Decreased in Wilson’s Disease, causing excessive Cu to accumulate in liver and brain causing cirrhosis. Binds to copper. |
front 61 What is α2 Macroglobulin | back 61 Protease inhibitor (inhibits complement, coagulation, and fibrinolytics). Largely increased in nephrotic syndrome. Decreased in pancreatitis, RA, and multiple myeloma. N ote similar to to α1Antitrypsin and α1Antichymotrypsin it breaks down proteins. |
front 62 What is Transferrin? | back 62 Transports Ferric (Fe3+) cations to storage sites (marrow, liver, spleen) Acute Phase Protein, transports iron, and increased in hemochromatosis |
front 63 What is Hemopexin? | back 63 Plasma glycoprotein that removes heme from circulation. Increased in Diabetes, inflammation, and pregnancy. Decreased in hemolytic diseases |
front 64 What are β lipoproteins? | back 64 Carry lipids in the plasma, classified as LDL-C |
front 65 What is β2 Microglobulin | back 65 Found on nucleated cell membranes, especially on lymphocytes Elevated in multiple myeloma, leukemias, hepatitis, Rheumatoid Arthritis, Systemic Lupus Erythematosus, and AIDS They work with gamma globulins. |
front 66 What is CRP(C-Reactive Protein)? | back 66 Acute phase reactant and an indicator of tissue injury or inflammation |
front 67 What is Fibrinogen? | back 67 Acute phase reactant and a coagulation factor. Increased in pregnancy and women on OCPs. Decreased in consumptive coagulopathies |
front 68 What is Complement? | back 68 Over 30 glycoproteins with many effects on the body, think of cell lysis |
front 69 What are C3and C4? | back 69 Acute phase proteins, Decreased in Disseminated Intravascular Coagulopathy (DIC), Paroxysmal Nocturnal Hemoglobinuria (PNH), infections with meningococci, or malnutrition |
front 70 What are γ globulins | back 70 Gamma globulins are thought of as antibodies Gamma globulins that have been mistakenly created against our own cells are called autoimmune diseases, meaning that we are attacking ourselves |
front 71 What is the formula and range for the Albumin/Globulin Ratio (A/G ratio)? | back 71 A/G ratio = albumin / globulin (Total Protein - Albumin = Globulin) Normal range is 1.1-1.5 |
front 72 What does a low (A/G ratio) indicate? | back 72 <1.1 1.multiple myeloma (immunoglobulin hyperproduction) 2.cirrhosis (lack of albumin synthesis) 3.nephrotic syndrome (loss of protein in the urine) |
front 73 What does a high (A/G ratio) indicate? | back 73 High A/G ratios (>1.5) 1.leukemias (lack of immunoglobulin production) 2.genetic immunoglobulin deficiencies (Common Variable Immunodeficiency [CVID], selective Ig deficiencies) |
front 74 What is the function Prealbumin / Transthyretin? | back 74 Serves as a transport protein or shuttle |
front 75 What is the clinical significance of realbumin / Transthyretin? | back 75
|
front 76 What does a normal Serum Protein Electrophoresis graph look like? | back 76  |
front 77 What does a nephrotic syndrome Protein Electrophoresis graph look like? | back 77 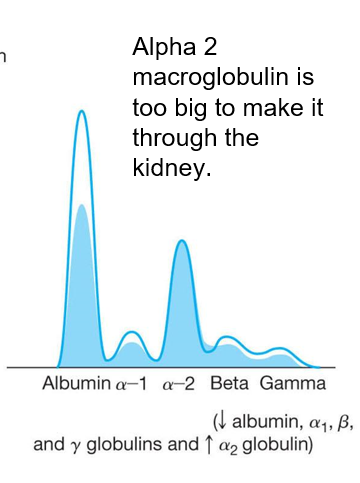 |
front 78 What does a acute phase reactants Protein Electrophoresis graph look like? | back 78 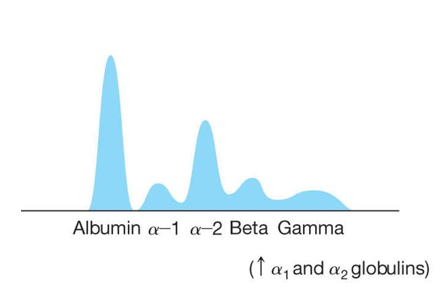 |
front 79 What does a multiple myeloma Protein Electrophoresis graph look like? | back 79 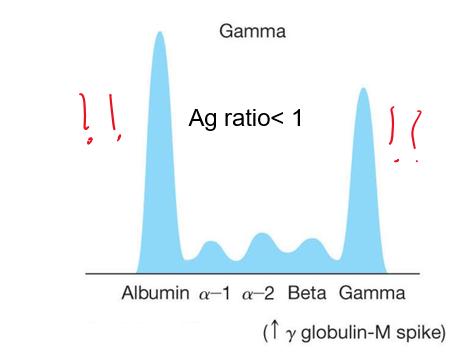 |
front 80 What is Multiple Myeloma | back 80 is cancer of the plasma cells, resulting in uncontrolled hyperproduction of immunoglobulin Leads to pathologic fractures and hypercalcemia Patients generally have bone pain and hypercalcemia along with proteinuria Low α1 macroglobulin high β2 micro globulin |
front 81 What can cause Hypoproteinemia? | back 81 can caused by hemodilution, decreased production, increased loss of protein inadequate nutrition, water intoxication, nephrotic syndrome, or liver failure note: Clinical giveaway is Ascites, which is an excess amount of water in the peritoneal cavity. |
front 82 What happens in most forms of hepatitis? | back 82 a decreased synthetic capacity of the liver, which includes a low A/G ratio with decreased plasma albumin levels, coagulopathies Almost all serum protien are produced by liver. C an cause bleeding and Ascites |
front 83 What is the Biuret method? | back 83 Cupric ions (Cu2+) in an alkaline medium form a purple color (540 nm) as they interact with peptide bonds |
front 84 What does the biuret reagent contain? | back 84 1) NaOH for alkalinity, 2) NaK tartrate, 3) Potassium Iodide (KI), 4) CuSo4 |
front 85 What is Refractometry used for? | back 85 rapid, approximate range of total protein concentration. This method measures the refractive index. |
front 86 What is the Dye-Binding Method? | back 86 Coomassie blue in acidic solution. When the dye binds the protein, the absorbance increases at 595 nm. |
front 87 What should not be done when testing for urinary proteins? | back 87 Do NOT dilute urine for proteins. You dilute for creatinine. Only smaller proteins can pass through the glomeruli, but they are VERY likely to be reabsorbed |
front 88 The major problem with urinary dipstick is? | back 88 There can be a lot of false positive results Notes: They use tetrabromphenol blue at pH of 3, Turbidimetric methods precipitate (denature) proteins with sulfasalicylic acid (SSA), trichloroacetic acid, or benthonium chloride. SSA is known to precipitate many substances and cause false positive results |
front 89 What to know about Homogentistic acid (HGA) oxidase? | back 89 it is the deficient enzyme Leads to a build up of HGA in body tissues Autosomal recessive |
front 90 What is Ochronosis? | back 90 darkening of body tissues due to HGA Diapers stain black because of HGA in the urine of babies |
front 91 what is Cystinuria? | back 91 Defect in Amino Acid transport system, NOT a metabolic deficiency Kidneys are unable to reabsorb the divalent amino acids (cystine, lysine, arginine, ornithine) Cystine can result in kidney stones, which can cause flank pain and hematuria |
front 92 There is a certain smell with PKU. What is that smell? | back 92 “Mousy” or “Musty” urine odor, eczema, fair complexion note: Causes mental retardation if not corrected early in life Can be controlled with PKU-free diet Brain damage occurs with cessation of a PKU-free diet |
front 93 what is a break down for Non-Protein Nitrogens (NPN)? | back 93 Urea nitrogen - ~45% of NPN in the blood Uric acid - ~20% of NPN in the blood Creatinine - ~5% of NPN in the blood Ammonia will be covered later - ~0.2% of NPN in the blood |
front 94 What formula do you need to know for BUN? | back 94 BUN (mg/dL) x 2.14 = Urea (mg/dL) |
front 95 How are bun and glomerular related? | back 95 BUN is inversely correlated with glomerular filtration rate and renal plasma flow |
front 96 What is the cause of Prerenal Azotemia ? | back 96 usually caused by dehydration, but can be due to any reason for impaired blood flow to the kidneys or increased protein catabolism |
front 97 What is the cause of Renal Azotemia? | back 97 Acute renal failure |
front 98 What is the cause of Postrenal Azotemia? | back 98 Obstructive Renal Disease |
front 99 What is the formula for the Urease method ? | back 99 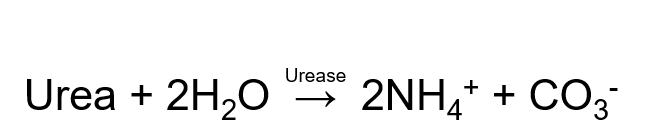 |
front 100 What are the BUN reference ranges and other important clinical information to know? | back 100 BUN Reference Range 7-18 mg/dL 24 hour urine 12-20 grams/24 hours BUN is stable at RT for 4 hours Several days at 4˚C Several months at -20˚C Males are slightly higher, but it is not clinically significant |
front 101 What is the formula for the Diacetyl or “Fearon” Reaction at 540 nm? | back 101 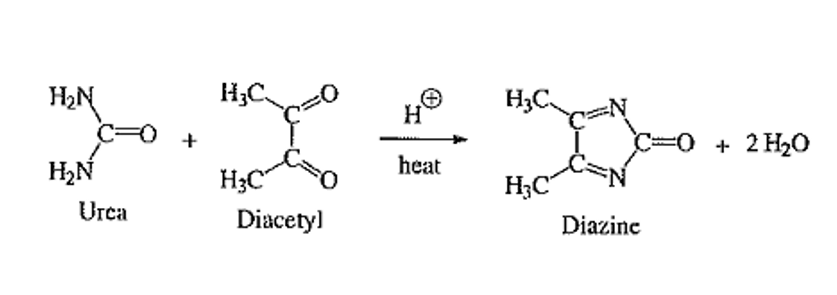 |
front 102 What does a higher BUN:Cr Ratio indicate? | back 102 ratio is indicative of prerenal azotemia: dehydration, heart failure |
front 103 What does a lower BUN:Cr Ratio indicate? | back 103 ratio can be seen in intrarenal azotemia, dialysis, SIADH, low protein diet, diarrhea |
front 104 What can a normal BUN:Cr Ratio indicate? | back 104 postrenal azotemia (causes of decreased GFR, like congestive heart failure, obstructive renal cell carcinoma, dehydration, etc.) note:BUN is usually 15 times that of creatinine don’t use on normal patients. |
front 105 BUN: 56 mg/dL Cr: 1.5 mg/dL BUN:Cr ratio: Prerenal, Renal, or Postrenal? | back 105  37.3= prerenal note: Remember a BUN/Cr 10-20 is usually a renal etiology, BUN/Cr >30 is usually prerenal renal failure unless proven otherwise, BUN/Cr >40 is definitely prerenal |
front 106 BUN: 43 mg/dL Cr: 2.9 mg/dL BUN:Cr ratio: Prerenal, Renal, or Postrenal? | back 106  15= postrenal note: Remember a BUN/Cr 10-20 is usually a renal etiology, BUN/Cr >30 is usually prerenal renal failure unless proven otherwise, BUN/Cr >40 is definitely prerenal |
front 107 What throws off the estimation of glomerular filtration? | back 107 creatinine is secreted ever-so-slightly in the distal convoluted tubule (DCT) In renal disease, creatinine excretion is decreased |
front 108 What method is used for testing creatinine? | back 108 Jaffe Reaction - Creatinine and Picric Acid in alkaline solution Beware! Picric acid is explosive! Interferences with protein, glucose, uric acid, ascorbic acid, acetone, ketoacids, cephalosporins Enzymatic methods are also available which all start with creatininase |
front 109 What reference ranges for creatinine? | back 109 0.9-1.2 mg/dL men 0.6-1.1 mg/dL for women |
front 110 What causes Gout? | back 110 usually increased production of Uric Acid |
front 111 What causes Lesch-Nyhan Syndrome? | back 111 HGPRT deficiency which results in elevated levels of Uric Acid. Symptoms include mental retardation, muscle fasciculations, Self-mutilation |
front 112 What causes Cytotoxic Chemotherapy? | back 112 Tumor-Lysis Syndrome, the rapid killing of cells results in DNA damage, and the production of lots of Uric Acid |
front 113 What causes Malignancies? | back 113 Cancer can lead to rapid formation of cells, but they often die off quickly, resulting in DNA damage and release of Uric Acid into the serum |
front 114 What is uremia? | back 114 Urea and Creatinine Results from Renal failure Neurotoxic Elevated levels of Uric Acid in the blood, can cause Uremic Frost on a patient’s skin |
front 115 57-year-old male - congestive heart failure, Creatinine of 2.1 mg/dL, BUN of 75 mg/dL. what is the BUN/Cr ratio and Prerenal, Renal, or Postrenal? | back 115 Prerenal azotemia Ratio of 35.7 not full diagnositic need over 40 |
front 116 12-year-old female - polycystic kidney disease, Creatinine of 4.5 mg/dL, BUN of 81 mg/dL what is the BUN/Cr ratio and Prerenal, Renal, or Postrenal? | back 116 Renal azotemia Ratio of 18: in ratio |
front 117 75-year-old male - benign prostatic hypertrophy, Creatinine of 3.2 mg/dL, BUN of 57 mg/dL what is the BUN/Cr ratio and Prerenal, Renal, or Postrenal? | back 117 Postrenal azotemia Ratio of 17.8 why this is post is because of the prostate vs the kidney |
front 118 How do we test for ammonia? | back 118 the glutamate dehydrogenase method It measures the diminishing concentration of NADP at 340 This sample must be tested immediately, no waiting. The sample should be venous blood, collected in EDTA or Heparin, and placed on ice |
front 119 What is the process for hepatic encephalopathy? | back 119 Liver failure → ↑NH3 → neuronal destruction → hepatic encephalopathy |
front 120 What is Reye’s syndrome? | back 120 The result is fulminant liver failure and many patients don’t survive the ordeal. Blood ammonia levels are the preferred lab test in this scenario, because they are most closely associated with prognosis and survival Note: The connection that I want you to make with this is that whenever you hear of a child taking aspirin for a viral illness |
front 121 What is a lesser known cause of hyperammonemia? | back 121 urea cycle enzyme disorders |
front 122 Define the following: Primary protein. | back 122 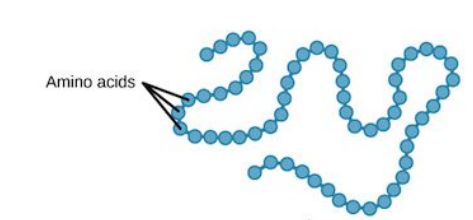 A sequence of amino acid chains. |
front 123 Define the following: Secondary protein structure | back 123 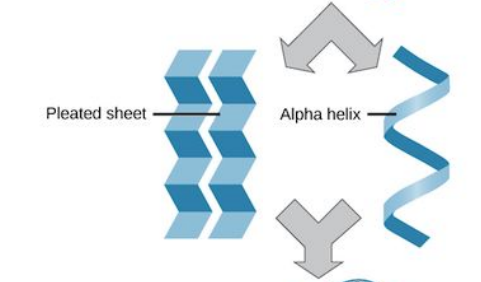 Hydrogen bonding of the peptide back bone cause the amino acids to fold into a repeating pattern. |
front 124 Define the following: tertiary protein structure | back 124 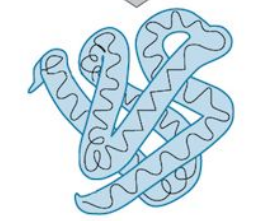 three-dimensional folding patter of a protein due to side chain reactions |
front 125 Define the following: quaternary protein structure | back 125  Protein consisting of more than one amino acid chain. |